Abstract
OBJECTIVES
Systematic review of preventive pharmacologic treatments for community-dwelling adults with episodic migraine.
DATA SOURCES
Electronic databases through May 20, 2012.
ELIGIBILITY CRITERIA
English-language randomized controlled trials (RCTs) of preventive drugs compared to placebo or active treatments examining rates of ≥50 % reduction in monthly migraine frequency or improvement in quality of life.
STUDY APPRAISAL AND SYNTHESIS METHODS
We assessed risk of bias and strength of evidence and conducted random effects meta-analyses of absolute risk differences and Bayesian network meta-analysis.
RESULTS
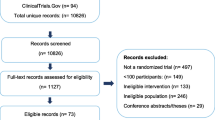
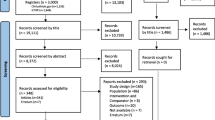
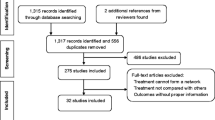
Of 5,244 retrieved references, 215 publications of RCTs provided mostly low-strength evidence because of the risk of bias and imprecision. RCTs examined 59 drugs from 14 drug classes. All approved drugs, including topiramate (9 RCTs), divalproex (3 RCTs), timolol (3 RCTs), and propranolol (4 RCTs); off-label beta blockers metoprolol (4 RCTs), atenolol (1 RCT), nadolol (1 RCT), and acebutolol (1 RCT); angiotensin-converting enzyme inhibitors captopril (1 RCT) and lisinopril (1 RCT); and angiotensin II receptor blocker candesartan (1 RCT), outperformed placebo in reducing monthly migraine frequency by ≥50 % in 200–400 patients per 1,000 treated. Adverse effects leading to treatment discontinuation (68 RCTs) were greater with topiramate, off-label antiepileptics, and antidepressants than with placebo. Limited direct evidence as well as frequentist and exploratory network Bayesian meta-analysis showed no statistically significant differences in benefits between approved drugs. Off-label angiotensin-inhibiting drugs and beta-blockers were most effective and tolerable for episodic migraine prevention.
LIMITATIONS
We did not quantify reporting bias or contact principal investigators regarding unpublished trials.
CONCLUSIONS
Approved drugs prevented episodic migraine frequency by ≥50 % with no statistically significant difference between them. Exploratory network meta-analysis suggested that off-label angiotensin-inhibiting drugs and beta-blockers had favorable benefit-to-harm ratios. Evidence is lacking for long-term effects of drug treatments (i.e., trials of more than 3 months duration), especially for quality of life.



Similar content being viewed by others
REFERENCES
Goadsby PJ, Raskin NH. Chapter 15. Headache. In: Fauci AS, Braunwald E, Kasper DL, et al., eds. Harrison’s principles of internal medicine. 17th ed. New York: The McGraw-Hill Companies; 2008.
Silberstein SD. Preventive migraine treatment. Neurol Clin. 2009;27:429–43.
Solomon GD, Santanello N. Impact of migraine and migraine therapy on productivity and quality of life. Neurology. 2000;55:S29–35.
Diamond S, Bigal ME, Silberstein S, Loder E, Reed M, Lipton RB. Patterns of diagnosis and acute and preventive treatment for migraine in the United States: results from the American Migraine Prevalence and Prevention study. Headache. 2007;47:355–63.
Lipton RB, Scher AI, Kolodner K, Liberman J, Steiner TJ, Stewart WF. Migraine in the United States: epidemiology and patterns of health care use. Neurology. 2002;58:885–94.
Bigal ME, Lipton RB, Winner P, et al. Migraine in adolescents: association with socioeconomic status and family history. Neurology. 2007;69:16–25.
Hernandez-Latorre MA, Roig M. Natural history of migraine in childhood. Cephalalgia. 2000;20:573–9.
Headache Classification Subcommittee of the International Headache Society. The International Classification of Headache Disorders: 2nd edition. Cephalalgia. 2004;24(Suppl 1):9–160.
Olesen J, Bousser MG, Diener HC, et al. New appendix criteria open for a broader concept of chronic migraine. Cephalalgia. 2006;26:742–6.
Solomon S. New appendix criteria open for a broader concept of chronic migraine (Comment on: Cephalagia 2006 Jun:26(6):742–6). Cephalalgia. 2007;27:469. author reply −70.
Stewart WF, Ricci JA, Chee E, Morganstein D. Lost productive work time costs from health conditions in the United States: results from the American Productivity Audit. J Occup Environ Med. 2003;45:1234–46.
Hu XH, Markson LE, Lipton RB, Stewart WF, Berger ML. Burden of migraine in the United States: disability and economic costs. Arch Intern Med. 1999;159:813–8.
Burton WN, Landy SH, Downs KE, Runken MC. The impact of migraine and the effect of migraine treatment on workplace productivity in the United States and suggestions for future research. Mayo Clin Proc. 2009;84:436–45.
Lipton RB, Scher AI, Steiner TJ, et al. Patterns of health care utilization for migraine in England and in the United States. Neurology. 2003;60:441–8.
Lipton RB, Stewart WF. The epidemiology of migraine. Eur Neurol. 1994;34(Suppl 2):6–11.
Rapoport AM. Acute and prophylactic treatments for migraine: present and future. Neurol Sci. 2008;29(Suppl 1):S110–22.
Stafford RS. Regulating off-label drug use–rethinking the role of the FDA. N Engl J Med. 2008;358:1427–9.
Silberstein S, Tfelt-Hansen P, Dodick DW, et al. Guidelines for controlled trials of prophylactic treatment of chronic migraine in adults. Cephalalgia. 2008;28:484–95.
Schroeder BM. AAFP/ACP-ASIM release guidelines on the management and prevention of migraines. Am Fam Physician. 2003;67(1392):5–7.
Morey SS. Guidelines on migraine: part 4. General principles of preventive therapy. Am Fam Physician. 2000;62:2359–60.
Lainez MJ, Freitag FG, Pfeil J, Ascher S, Olson WH, Schwalen S. Time course of adverse events most commonly associated with topiramate for migraine prevention. Eur J Neurol. 2007;14:900–6.
Luykx J, Mason M, Ferrari MD, Carpay J. Are migraineurs at increased risk of adverse drug responses? A meta-analytic comparison of topiramate-related adverse drug reactions in epilepsy and migraine. Clin Pharmacol Ther. 2009;85:283–8.
Geraud G, Lanteri-Minet M, Lucas C, Valade D. French guidelines for the diagnosis and management of migraine in adults and children. Clin Ther. 2004;26:1305–18.
Evers S, Afra J, Frese A, et al. EFNS guideline on the drug treatment of migraine–revised report of an EFNS task force. Eur J Neurol. 2009;16:968–81.
Dowson AJ, Lipscombe S, Sender J, Rees T, Watson D. New guidelines for the management of migraine in primary care. Curr Med Res Opin. 2002;18:414–39.
Epstein RM, Alper BS, Quill TE. Communicating evidence for participatory decision making. JAMA. 2004;291:2359–66.
Amanzio M, Corazzini LL, Vase L, Benedetti F. A systematic review of adverse events in placebo groups of anti-migraine clinical trials. Pain. 2009;146:261–9.
Whyte CA, Tepper SJ. Adverse effects of medications commonly used in the treatment of migraine. Expert Rev Neurother. 2009;9:1379–91.
Sung NS, Crowley WF Jr, Genel M, et al. Central challenges facing the national clinical research enterprise. JAMA. 2003;289:1278–87.
Institute of Medicine (US). Finding what works in health care: Standards for systematic reviews. Heidelberg: National Academies Press; 2011.
Institute of Medicine (US). Committee on Ethical and Scientific Issues in Studying the Safety of Approved Drugs. Ethical and scientific issues in studying the safety of approved drugs. Washington: National Academies Press; 2012.
Slutsky J, Atkins D, Chang S, Collins Sharp BA. Comparing medical interventions: AHRQ and the Effective Health Care Program. Methods Guide for Effectiveness and Comparative Effectiveness Reviews AHRQ Publication No 10(11)-EHC063-EF. 2011/03/25 ed. Rockville, MD: Agency for Healthcare Research and Quality; 2008:1–4. Available at http://effectivehealthcare.ahrq.gov/ehc/products/118/324/MethodsGuide_Slutsky_Comparing%20Medical%20Interventions.pdf; accessed on February 19, 2013.
Helfand M, Balshem H. Principles in Developing and Applying Guidance. 2008.
Whitlock EP, Lopez SA, Chang S, Helfand M, Eder M, Floyd N. AHRQ series paper 3: identifying, selecting, and refining topics for comparative effectiveness systematic reviews: AHRQ and the effective health-care program. J Clin Epidemiol. 2010;63:491–501.
Rothner AD. Complicated migraine and migraine variants. Curr Pain Headache Rep. 2002;6:233–9.
Hansen JM, Thomsen LL, Olesen J, Ashina M. Calcitonin gene-related peptide does not cause the familial hemiplegic migraine phenotype. Neurology. 2008;71:841–7.
Norris S, Atkins D, Bruening W, et al. Chapter 4. Selecting observational studies for comparing medical interventions. Methods Guide for Effectiveness and Comparative Reviews AHRQ Publication No 10(11)-EHC063-EF. Rockville, MD: Agency for Healthcare Research and Quality. March 2011:56–68. Available at: http://effectivehealthcare.ahrq.gov/ehc/products/196/454/MethodsGuideNorris_06042010.pdf; accessed on February 19, 2013.
Chou R, Aronson N, Atkins D, et al. AHRQ series paper 4: assessing harms when comparing medical interventions: AHRQ and the Effective Health-Care Program. J Clin Epidemiol. 2008;63:502–12.
Higgins J, Green S, eds. Cochrane handbook for systematic reviews of interventions. Version 5.1.0. London: The Cochrane Collaboration; 2011.
Higgins JP, Altman DG, Gotzsche PC, et al. The Cochrane Collaboration's tool for assessing risk of bias in randomised trials. BMJ. 2011;343:d5928.
van der Velde G, van Tulder M, Cote P, et al. The sensitivity of review results to methods used to appraise and incorporate trial quality into data synthesis. Spine. 2007;32:796–806. Phila Pa 1976.
Herbison P, Hay-Smith J, Gillespie WJ. Adjustment of meta-analyses on the basis of quality scores should be abandoned. J Clin Epidemiol. 2006;59:1249–56.
Wallace BC, Schmid CH, Lau J, Trikalinos TA. Meta-Analyst: software for meta-analysis of binary, continuous and diagnostic data. BMC Med Res Methodol. 2009;9:80.
Egger M, Smith GD, Altman DG. Systematic reviews in health care: meta-analysis in context. 2nd ed. London: BMJ Books; 2001.
Treadwell JR, Uhl S, Tipton K, et al. Assessing equivalence and noninferiority. J Clin Epidemiol. 2012;65:1144–9.
Lievre M, Cucherat M, Leizorovicz A. Pooling, meta-analysis, and the evaluation of drug safety. Current controlled trials in cardiovascular medicine. 2002;3:6.
Fu R, Gartlehner G, Grant M, et al. Chapter 9. Conducting quantitative synthesis when comparing medical interventions. Methods Guide for Effectiveness and Comparative Effectiveness Reviews AHRQ Publication No 10(11)-EHC063-EF. Rockville, MD: Agency for Healthcare Research and Quality. March 2011:104–19. Available at: http://effectivehealthcare.ahrq.gov/ehc/products/243/554/MethodsGuide--ConductingQuantitativeSynthesis.pdf; accessed on February 20, 2013.
Rucker G, Schwarzer G, Carpenter J, Olkin I. Why add anything to nothing? The arcsine difference as a measure of treatment effect in meta-analysis with zero cells. Stat Med. 2009;28:721–38.
Bradburn MJ, Deeks JJ, Berlin JA, Russell LA. Much ado about nothing: a comparison of the performance of meta-analytical methods with rare events. Stat Med. 2007;26:53–77.
Sweeting MJ, Sutton AJ, Lambert PC. What to add to nothing? Use and avoidance of continuity corrections in meta-analysis of sparse data. Stat Med. 2004;23:1351–75.
Stijnen T, Hamza TH, Ozdemir P. Random effects meta-analysis of event outcome in the framework of the generalized linear mixed model with applications in sparse data. Stat Med. 2010;29:3046–67.
White IR. Multivariate random-effects meta-regression: Updates to mvmeta. The Stata Journal 2011;11.
Owens DK, Lohr KN, Atkins D, et al. AHRQ series paper 5: grading the strength of a body of evidence when comparing medical interventions-Agency for Healthcare Research and Quality and the Effective Health-Care Program. J Clin Epidemiol. 2010;63:513–23.
Viechtbauer W. Confidence intervals for the amount of heterogeneity in meta-analysis. Stat Med. 2007;26:37–52.
Knapp G, Biggerstaff BJ, Hartung J. Assessing the amount of heterogeneity in random-effects meta-analysis. Biom J. 2006;48:271–85.
DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7:177–88.
Ad Hoc Committee on Classification of Headache. Classification of headache. JAMA. 1962;179:717–8.
Ebrahim S. The use of numbers needed to treat derived from systematic reviews and meta-analysis. Caveats and pitfalls. Eval Health Prof. 2001;24:152–64.
Altman DG. Confidence intervals for the number needed to treat. BMJ. 1998;317:1309–12.
Coory M, Jordan S. Frequency of treatment-effect modification affecting indirect comparisons: a systematic review. Pharmcoeconomics. 2010;28:723–32.
Wells G, Sultan S, Chen L, Khan M, Coyle D. Indirect evidence: Indirect treatment comparisons in meta-analysis. Ottawa: Canadian Agency for Drugs and Technologies in Health; 2009.
Glenny AM, Altman DG, Song F, et al. Indirect comparisons of competing interventions. Health Technol Assess. 2005;9:1–134. iii-iv.
Song F, Loke YK, Walsh T, Glenny AM, Eastwood AJ, Altman DG. Methodological problems in the use of indirect comparisons for evaluating healthcare interventions: survey of published systematic reviews. BMJ. 2009;338:b1147.
Donegan S, Williamson P, Gamble C, Tudur-Smith C. Indirect comparisons: a review of reporting and methodological quality. PLoS One. 2010;5:e11054.
Carlin BP, Louis TA. Bayesian methods for data analysis. Boca Raton: Chapman & Hall/CRC; 2009.
Higgins JPT, Jackson D, Barrett JK, Lu G, Ades AE, White IR. Consistency and inconsistency in network meta-analysis: concepts and models for multi-arm studies. Research Synthesis Methods. 2012;3:98–110.
Aschengrau A, Seage GR. Essentials of epidemiology in public health. Sudbury: Jones and Bartlett; 2003.
Lunn D, Thomas A, Best N, Spiegelhalter D. WinBUGS- a Bayesian modelling framework: concepts, structure, and extensibility. Statistics and Computing. 2000;10:325–37.
Berkman ND, Lohr KN, Morgan LC, et al. Reliability Testing of the AHRQ EPC Approach to Grading the Strength of Evidence in Comparative Effectiveness Reviews. Rockville (MD) 2012.
Guyatt G, Oxman AD, Kunz R, et al. GRADE guidelines 6. Rating the quality of evidence-imprecision. J Clin Epidemiol 2011.
Sterne JA, Sutton AJ, Ioannidis JP, et al. Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ. 2011;343:d4002.
Silberstein S. Efficacy and safety of topiramate in migraine prevention: a dose-ranging, placebo-controlled, double-blind, multicenter study. Advanced Studies in Medicine. 2003;3:S565–8.
Brandes JL, Saper JR, Diamond M, et al. Topiramate for migraine prevention: a randomized controlled trial. JAMA. 2004;291:965–73.
Silberstein SD, Neto W, Schmitt J, Jacobs D. Topiramate in migraine prevention: results of a large controlled trial. Arch Neurol. 2004;61:490–5.
Diener HC, Agosti R, Allais G, et al. Cessation versus continuation of 6-month migraine preventive therapy with topiramate (PROMPT): a randomised, double-blind, placebo-controlled trial. Lancet Neurol. 2007;6:1054–62.
Brandes JL, Kudrow DB, Rothrock JF, Rupnow MF, Fairclough DL, Greenberg SJ. Assessing the ability of topiramate to improve the daily activities of patients with migraine. Mayo Clin Proc. 2006;81:1311–9.
Diener HC, Bussone G, Van Oene JC, Lahaye M, Schwalen S, Goadsby PJ. Topiramate reduces headache days in chronic migraine: a randomized, double-blind, placebo-controlled study. Cephalalgia. 2007;27:814–23.
Dahlof C, Loder E, Diamond M, Rupnow M, Papadopoulos G, Mao L. The impact of migraine prevention on daily activities: a longitudinal and responder analysis from three topiramate placebo-controlled clinical trials. Health Qual Life Outcomes. 2007;5:56.
Klapper J. Divalproex sodium in migraine prophylaxis: a dose-controlled study. Cephalalgia. 1997;17:103–8.
Mei D, Ferraro D, Zelano G, et al. Topiramate and triptans revert chronic migraine with medication overuse to episodic migraine. Clin Neuropharmacol. 2006;29:269–75.
Lipton RB, Silberstein S, Dodick D, et al. Topiramate intervention to prevent transformation of episodic migraine: the topiramate INTREPID study. Cephalalgia. 2011;31:18–30.
Bussone G, Diener HC, Pfeil J, Schwalen S. Topiramate 100 mg/day in migraine prevention: a pooled analysis of double-blind randomised controlled trials. Int J Clin Pract. 2005;59:961–8.
Forssman B, Henriksson KG, Johannsson V, et al. Propranolol for migraine prophylaxis. Headache. 1976;16(5):238–45.
Schoonman GG, Wiendels NJ, Ferrari MD. Gabapentin in migraine prophylaxis: is it effective and well tolerated? Headache. 2002;42:235.
Nanda RN, Johnson RH, Gray J, Keogh HJ, Melville ID. A double blind trial of acebutolol for migraine prophylaxis. Headache. 1978;18(1):20–2.
Forssman B, Lindblad CJ, Zbornikova V. Atenolol for migraine prophylaxis. Headache. 1983;23(4):188–90.
Freitag FG, Diamond S. Nadolol and placebo comparison study in the prophylactic treatment of migraine. The Journal of the American Osteopathic Association. 1984;84(4):343–7.
Minervini MG, Pinto K. Captopril relieves pain and improves mood depression in depressed patients with classical migraine. Cephalalgia. 1987;7(Suppl 6):485–6.
Schrader H, Stovner LJ, Helde G, Sand T, Bovim G. Prophylactic treatment of migraine with angiotensin converting enzyme inhibitor (lisinopril): randomised, placebo controlled, crossover study. BMJ. 2001;322:19–22.
Tronvik E, Stovner LJ, Helde G, Sand T, Bovim G. Prophylactic treatment of migraine with an angiotensin II receptor blocker: a randomized controlled trial. JAMA. 2003;289:65–9.
Diener HC, Gendolla A, Feuersenger A, et al. Telmisartan in migraine prophylaxis: a randomized, placebo-controlled trial. Cephalalgia. 2009;29:921–7.
Adelman J, Freitag FG, Lainez M, et al. Analysis of safety and tolerability data obtained from over 1,500 patients receiving topiramate for migraine prevention in controlled trials. Pain Med. 2008;9:175–85.
Couch JR, Hassanein RS. Amitriptyline in migraine prophylaxis. Arch Neurol. 1979;36:695–9.
Lampl C, Huber G, Adl J, et al. Two different doses of amitriptyline ER in the prophylaxis of migraine: long-term results and predictive factors. Eur J Neurol. 2009;16:943–8.
Silberstein SD, Hulihan J, Karim MR, et al. Efficacy and tolerability of topiramate 200 mg/d in the prevention of migraine with/without aura in adults: a randomized, placebo-controlled, double-blind, 12-week pilot study. Clin Ther. 2006;28:1002–11.
Reuter U, Del Rio MS, Diener HC, et al. Migraines with and without aura and their response to preventive therapy with topiramate. Cephalalgia: an International Journal of Headache. 2010;30(5):543–51.
Barden J, Derry S, McQuay HJ, Moore RA. Bias from industry trial funding? A framework, a suggested approach, and a negative result. Pain. 2006;121:207–18.
Fox AW. Disease modification in migraine: study design and sample size implications. Headache. 2008;48:1169–75.
Hazard E, Munakata J, Bigal ME, Rupnow MFT, Lipton RB. The burden of migraine in the United States: current and emerging perspectives on disease management and economic analysis. Value in Health. 2009;12:55–64.
Russell MB, Hilden J, Sorensen SA, Olesen J. Familial occurrence of migraine without aura and migraine with aura. Neurology. 1993;43:1369–73.
Arends LR, Hoes AW, Lubsen J, Grobbee DE, Stijnen T. Baseline risk as predictor of treatment benefit: three clinical = meta-re-analyses. Stat Med. 2000;19:3497–518.
Gentile G, Missori S, Borro M, Sebastianelli A, Simmaco M, Martelletti P. Frequencies of genetic polymorphisms related to triptans metabolism in chronic migraine. Journal of Headache & Pain. 2010;11:151–6.
Schurks M, Zee RY, Buring JE, Kurth T. ACE D/I polymorphism, migraine, and cardiovascular disease in women. Neurology. 2009;72:650–6.
Feldman HL. Pushing drugs: genomics and genetics, the pharmaceutical industry, and the law of negligence. Washburn Law J. 2003;42:575–99.
Tomson T, Battino D. Teratogenic effects of antiepileptic drugs. Lancet Neurol. 2012;11:803–13.
Coebergh JA, Waldinger MD. Reversible anorgasmia with topiramate for migraine prophylaxis. The Journal of Neuropsychiatry and Clinical Neurosciences. 2012;24:E30–1.
Huang CY, Keller JJ, Sheu JJ, Lin HC. Migraine and erectile dysfunction: evidence from a population-based case–control study. Cephalalgia. 2012;32:366–72.
Bingham MF, Johnson FR, Miller D. Modeling choice behavior for new pharmaceutical products. Value in Health. 2001;4:32–44.
Silberstein SD, Holland S, Freitag F, Dodick DW, Argoff C, Ashman E. Evidence-based guideline update: pharmacologic treatment for episodic migraine prevention in adults: report of the Quality Standards Subcommittee of the American Academy of Neurology and the American Headache Society. Neurology. 2012;78:1337–45.
Brouwers MC, Kho ME, Browman GP, et al. AGREE II: advancing guideline development, reporting and evaluation in health care. J Clin Epidemiol. 2010;63:1308–11.
Mullan RJ, Flynn DN, Carlberg B, et al. Systematic reviewers commonly contact study authors but do so with limited rigor. J Clin Epidemiol. 2009;62:138–42.
Finding Evidence and Assessing for Reporting Biases when Comparing Medical Interventions: AHRQ and the Effective Health Care Program. In press 2012. The draft is available at: http://effectivehealthcare.ahrq.gov/ehc/products/486/1305/Reporting-Bias_DraftReport_20121023.pdf; accessed on February 19, 2013
Edwards IR. Off-label pharmacovigilance. Drug Saf. 2011;34:795–7.
Layton D, Hazell L, Shakir SA. Modified prescription-event monitoring studies: a tool for pharmacovigilance and risk management. Drug Saf. 2011;34:e1–9.
Mathew NT, Saper JR, Silberstein SD, et al. Migraine prophylaxis with divalproex. Arch Neurol. 1995;52:281–6.
Freitag FG, Collins SD, Carlson HA, et al. A randomized trial of divalproex sodium extended-release tablets in migraine prophylaxis. Neurology. 2002;58:1652–9.
Storey JR, Calder CS, Hart DE, Potter DL. Topiramate in migraine prevention: a double-blind, placebo-controlled study. Headache. 2001;41:968–75.
Mei D, Capuano A, Vollono C, et al. Topiramate in migraine prophylaxis: a randomised double-blind versus placebo study. Neurol Sci. 2004;25:245–50.
Silvestrini M, Bartolini M, Coccia M, Baruffaldi R, Taffi R, Provinciali L. Topiramate in the treatment of chronic migraine. Cephalalgia. 2003;23:820–4.
Gupta P, Singh S, Goyal V, Shukla G, Behari M. Low-dose topiramate versus lamotrigine in migraine prophylaxis (the Lotolamp study). Headache. 2007;47:402–12.
Silberstein S, Lipton R, Dodick D, et al. Topiramate treatment of chronic migraine: a randomized, placebo-controlled trial of quality of life and other efficacy measures. Headache. 2009;49:1153–62.
Tfelt-Hansen P, Standnes B, Kangasneimi P, Hakkarainen H, Olesen J. Timolol vs propranolol vs placebo in common migraine prophylaxis: a double-blind multicenter trial. Acta Neurol Scand. 1984;69:1–8.
Diener HC, Tfelt-Hansen P, Dahlof C, et al. Topiramate in migraine prophylaxis–results from a placebo-controlled trial with propranolol as an active control. J Neurol. 2004;251:943–50.
Diamond S, Medina JL. Double blind study of propranolol for migraine prophylaxis. Headache. 1976;16:24–7.
Standnes B. The prophylactic effect of timolol versus propranolol and placebo in common migraine: beta-blockers in migraine. Cephalalgia. 1982;2:165–70.
Stellar S, Ahrens SP, Meibohm AR, Reines SA. Migraine prevention with timolol. A double-blind crossover study. JAMA. 1984;252:2576–80.
Wessely P, Baumgartner C, Klingler D, et al. Preliminary results of a double-blind study with the new migraine prophylactic drug Gabapentin. Cephalalgia. 1987;7:477–8.
Mathew NT, Rapoport A, Saper J, et al. Efficacy of gabapentin in migraine prophylaxis. Headache. 2001;41:119–28.
NCT00742209. Prevention study in adult patients suffering from migraine headaches. 2010.
Havanka-Kanniainen H, Hokkanen E, Myllylä VV. Efficacy of nimodipine in the prophylaxis of migraine. Cephalalgia: an International Journal of Headache. 1985;5(1):39–43.
Gelmers HJ. Nimodipine, a new calcium antagonist, in the prophylactic treatment of migraine. Headache. 1983;23(3):106–9.
Kangasniemi P, Andersen AR, Andersson PG, et al. Classic migraine: effective prophylaxis with metoprolol. Cephalalgia. 1987;7:231–8.
Andersson PG, Dahl S, Hansen JH, et al. Prophylactic treatment of classical and non-classical migraine with metoprolol–a comparison with placebo. Cephalalgia. 1983;3:207–12.
Peikert A, Wilimzig C, Kohne-Volland R. Prophylaxis of migraine with oral magnesium: results from a prospective, multi-center, placebo-controlled and double-blind randomized study. Cephalalgia. 1996;16:257–63.
Pfaffenrath V, Wessely P, Meyer C, et al. Magnesium in the prophylaxis of migraine–a double-blind placebo-controlled study. Cephalalgia. 1996;16:436–40.
Silberstein SD, Lipton RB, Dodick DW, et al. Efficacy and safety of topiramate for the treatment of chronic migraine: a randomized, double-blind, placebo-controlled trial. Headache. 2007;47:170–80.
Edwards KR, Potter DL, Wu SC, Kamin M, Hulihan J. Topiramate in the preventive treatment of episodic migraine: a combined analysis from pilot, double-blind, placebo-controlled trials. CNS Spectr. 2003;8:428–32.
Pradalier A, Serratrice G, Collard M, et al. Long-acting propranolol in migraine prophylaxis: results of a double-blind, placebo-controlled study. Cephalalgia. 1989;9:247–53.
Boisen E, Deth S, Hübbe P, Jansen J, Klee A, Leunbach G. Clonidine in the prophylaxis of migraine. Acta Neurologica Scandinavica. 1978;58(5):288–95.
Adam EI, Gore SM, Price WH. Double blind trial of clonidine in the treatment of migraine in a general practice. J R Coll Gen Pract. 1978;28:587–90.
Couch JR. Amitriptyline in the prophylactic treatment of migraine and chronic daily headache. Headache. 2011;51:33–51.
Orholm M, Honore PF, Zeeberg I. A randomized general practice group-comparative study of femoxetine and placebo in the prophylaxis of migraine. Acta Neurol Scand. 1986;74:235–9.
Orholm M, Le Fevre P. Prophylactic treatment of migraine with femoxetine—a randomized comparison with placebo. Cephalalgia 1985:516–7.
Steiner TJ, Findley LJ, Yuen AW. Lamotrigine versus placebo in the prophylaxis of migraine with and without aura. Cephalalgia. 1997;17:109–12.
Hering R, Kuritzky A. Sodium valproate in the prophylactic treatment of migraine: a double-blind study versus placebo. Cephalalgia. 1992;12:81–4.
Jensen R, Brinck T, Olesen J. Sodium valproate has a prophylactic effect in migraine without aura: a triple-blind, placebo-controlled crossover study. Neurology. 1994;44:647–51.
Welch KMA, Ellis DJ, Keenan PA. Successful migraine prohpylaxis with naproxen sodium. Neurology1985.
Ziegler DK, Ellis DJ. Naproxen in prophylaxis of migraine. Archives of neurology. 1985;42(6):582–4.
(MINES) M-NESG. European multicenter trial of nimodipine in the prophylaxis of classic migraine (migraine with aura). Headache. 1989;29:639–42.
Dodick DW, Freitag F, Banks J, et al. Topiramate versus amitriptyline in migraine prevention: a 26-week, multicenter, randomized, double-blind, double-dummy, parallel-group noninferiority trial in adult migraineurs. Clin Ther. 2009;31:542–59.
Keskinbora K, Aydinli I. A double-blind randomized controlled trial of topiramate and amitriptyline either alone or in combination for the prevention of migraine. Clin Neurol Neurosurg. 2008;110:979–84.
Acknowledgments
Contributors
We would like to thank the librarians, Judy Stanke, MA, and Delbert Reed, PhD, for their contributions to the literature search; Jeannine Ouellette for her help in writing the report; Marilyn Eells for editing and formatting the report; and Christa Prodzinski, RN, and Kirsten Johnson, BS, for assistance with data entry, quality control, and formatting tables. We would like to thank Hwanhee Hong, PhD candidate, for her help in conducting Bayesian network meta-analyses.
Funders
Prepared by the University of Minnesota Evidence-based Practice Center under contract no. 290-2007-10064 I with the AHRQ
Conflict of Interest
The authors declare that they do not have a conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Systematic review registration no.: CRD42012001918
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 1534 kb)
Rights and permissions
About this article
Cite this article
Shamliyan, T.A., Choi, JY., Ramakrishnan, R. et al. Preventive Pharmacologic Treatments for Episodic Migraine in Adults. J GEN INTERN MED 28, 1225–1237 (2013). https://doi.org/10.1007/s11606-013-2433-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-013-2433-1