ABSTRACT
Background
Electronic medical records (EMR) are commonly believed to improve quality of care. Primary care patients with multiple chronic conditions have potentially greater opportunity to benefit from receiving care at practices with EMRs if these systems help coordinate complex care.
Objective
To examine how chronic conditions impact the odds that depressed patients receive depression treatment in primary care practices with EMRs compared to practices without EMRs.
Design
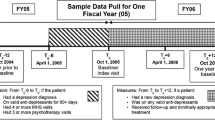
The study uses logistic regression to analyze cross-sectional data of primary care physician office visits in freestanding, office-based practices from the 2006–2008 National Ambulatory Medical Care Surveys.
Patients
All visits to primary care providers made by patients ages 18 and older with physician-identified depression (N = 3,467).
Main Measures
Outcomes include depression treatment which is defined as receipt or ordering of antidepressant medication and/or mental health counseling.
Key Results
EMRs were associated with significantly lowered odds that depressed patients received depression treatment (OR = 0.75, p = 0.009, 95% CI: 0.61-0.93); however when stratified by the number of chronic conditions, this association was observed only in patients with three or more chronic conditions (OR = 0.50, p > 0.001, 95% CI: 0.36-0.70). EMRs did not have a significant association with depression treatment for patients with two or fewer chronic conditions.
Conclusions
EMRs appear to have an unintended negative association with depression care provided during visits made by primary care patients with multiple chronic conditions.
Similar content being viewed by others
REFERENCES
Kessler RC, Berglund P, Demler O, et al. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289(23):3095–3105.
U.S. Department of Health and Human Services. Mental Health : A Report of the Surgeon General. Rockville, MD: U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration, Center for Mental Health Services, National Institutes of Health, National Institutes of Mental Health.;1999.
Kessler RC, Berglund P, Demler O, et al. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289(23):3095–3105.
Wang PS, Lane M, Olfson M, Pincus HA, Wells KB, Kessler RC. Twelve-month use of mental health services in the United States: Results from the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62:629–640.
Marcus SC, Olfson M. National Trends in the Treatment for Depression From 1998 to 2007. Arch Gen Psychiatry. 2010;67(12):1265–1273.
Wang PS, Demler O, Olfson M, Pincus HA, Wells KB, Kessler RC. Changing profiles of service sectors used for mental health care in the United States. Am J Psychiatry. 2006;163(7):1187–1198.
Pincus HA, Tanielian TL, Marcus SC, et al. Prescribing trends in psychotropic medications: primary care, psychiatry, and other medical specialities. JAMA. 1998;279(7):526–531.
Pincus HA, Zarin DA, Tanielian TL, et al. Psychiatric patients and treatments in 1997. Findings from the American psychiatric practice research network. Arch Gen Psychiatry. 1999;56:441–449.
Olfson M, Marcus SC, Druss B, Elinson L, Tanielian T, Pincus HA. National trends in the outpatient treatment of depression. JAMA. 2002;287(2):203–209.
Blumenthal D, Tavenner M. The Meaningful Use Regulation for Electronic Health Records. N Engl J Med. 2010;363(6):501–504.
DesRoches CM, Campbell EG, Rao SR, et al. Electronic health records in ambulatory care: a national survey of physicians. N Engl J Med. 2008;359(1):50–60.
Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Washington D.C.: National Academy Press; 2001a.
Garg AX, Adhikari NKJ, McDonald H, et al. Effects of Computerized Clinical Decision Support Systems on Practitioner Performance and Patient Outcomes. JAMA. 2005;293(10):1223–1238.
Chaudhry B, Wang J, Wu S, et al. Systematic review: impact of health information technology on quality, efficiency, and costs of medical care. Ann Intern Med. 2006;144(10):742–752.
Linder JA, Ma J, Bates DW, Middleton B, Stafford RS. Electronic health record use and the quality of ambulatory care in the United States. Arch Intern Med. 2007;167(13):1400–1405.
Romano MJ, Stafford RS. Electronic Health Records and Clinical Decision Support Systems: Impact on National Ambulatory Care Quality. Arch Intern Med. Forthcoming:archinternmed.2010.2527.
Ash JS, Berg M, Coiera E. Some unintended consequences of information technology in health care: the nature of patient care information system-related errors. J Am Med Inform Assoc. 2004;11(2):104–112.
Campbell EM, Sittig DF, Ash JS, Guappone KP, Dykstra RH. Types of unintended consequences related to computerized provider order entry. J Am Med Inform Assoc. 2006;13(5):547–556.
Harrison MI, Koppel R, Bar-Lev S. Unintended consequences of information technologies in health care–an interactive sociotechnical analysis. J Am Med Inform Assoc. 2007;14(5):542–549.
Cherry DK, Woodwell DA, Rechsteiner EA. National ambulatory Medicaid care survey: 2005 summary. Adv Data. 2007;387:1–39.
Bryant E, Shimizu I. Sample design, sampling variance, and estimation procedures for the National Ambulatory Medical Care Survey. Vital and health statistics Series 2, Data evaluation and methods research 1988 Sep(108): 1-39.
StataCorp. Stata Statistical Software: Release 10.0 Special Edition. College Station, TX: Stata Corporation; 2007.
Hsu J, Huang J, Fung V, Robertson N, Jimison H, Frankel R. Health information technology and physician-patient interactions: impact of computers on communication during outpatient primary care visits. Journal of the American Medical Informatics Association:. 2005;12(4):474–80.
Makoul G, Curry RH, Tang PC. The use of electronic medical records: communication patterns in outpatient encounters. Journal of the American Medical Informatics Association. 2001;8(6):610–5.
Margalit RS, Roter D, Dunevant MA, Larson S, Reis S. Electronic medical record use and physician-patient communication: an observational study of Israeli primary care encounters. Patient Educ Couns. 2006;61(1):134–41.
Arar NH, Wen L, McGrath J, Steinbach R, Pugh JA. Communicating about medications during primary care outpatient visits: the role of electronic medical records. Inform Prim Care. 2005;13(1):13–22.
Kuo GM, Mullen PD, McQueen A, Swank PR, Rogers JC. Cross-sectional comparison of electronic and paper medical records on medication counseling in primary care clinics: a Southern Primary-Care Urban Research Network (SPUR-Net) study. J Am Board Fam Med. 2007;20(2):164–73.
Booth N, Robinson P, Kohannejad J. Identification of high-quality consultation practice in primary care: the effects of computer use on doctor-patient rapport. Inform Prim Care. 2004;12(2):75–83.
Ventres W, Kooienga S, Vuckovic N, Marlin R, Nygren P, Stewart V. Physicians, patients, and the electronic health record: an ethnographic analysis. Ann Fam Med. 2006;4(2):124–31.
Ash JS, Sittig DF, Dykstra RH, Guappone K, Carpenter JD, Seshadri V. Categorizing the unintended sociotechnical consequences of computerized provider order entry. Int. J. Med. Inf. 2007;76:S21–S27.
Koppel R, Metlay JP, Cohen A, et al. Role of computerized physician order entry systems in facilitating medication errors. JAMA. 2005;293(10):1197–203.
Holden R. Cognitive performance-altering effects of electronic medical records: an application of the human factors paradigm for patient safety. Cognition, Technology & Work. 2011;13(1):11–29.
ACKNOWLEDGEMENTS
There were no funding sources for this research. This research was presented at the AcademyHealth Annual Research Meeting, Seattle, WA, June 12, 2011.
Conflict of Interest
The authors declare that they do not have any conflicts of interest to report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Harman, J.S., Rost, K.M., Harle, C.A. et al. Electronic Medical Record Availability and Primary Care Depression Treatment. J GEN INTERN MED 27, 962–967 (2012). https://doi.org/10.1007/s11606-012-2001-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-012-2001-0