ABSTRACT
BACKGROUND
Prior studies evaluating racial/ethnic differences in responses to antiretroviral therapy (ART) among HIV-infected patients have not adequately accounted for many potential confounders, and few have included Hispanic patients.
OBJECTIVE
To identify racial/ethnic differences in ART adherence, and risk of AIDS and death after ART initiation for HIV patients with similar access to care.
DESIGN
Retrospective cohort study.
PARTICIPANTS
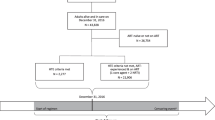
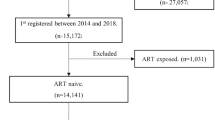
4,686 HIV-infected patients (66% White, 20% Black, and 14% Hispanic) initiating ART and who were enrolled in an integrated healthcare system.
MEASUREMENTS
Main outcomes evaluated were ART adherence, new AIDS clinical events, and all-cause mortality. The potential confounding effects of demographics, socioeconomic status, ART parameters, HIV disease stage, and other clinical parameters were considered in multivariable models.
RESULTS
Adjusted mean adherence levels were higher among White (70.1%; ref) compared with Black (64.2%; P < 0.001) and Hispanic patients (65.2%; P < 0.001). Adjusted hazard ratios (HR) for the risk of new AIDS events (White patients as reference) were 1.3 (P = 0.09) for Black and 0.9 (P = 0.64) for Hispanic patients. The adjusted HR for AIDS comparing Hispanic to Black patients was 0.7 (P = 0.11). Hispanic patients had fewer deaths compared with other racial/ethnic groups, particularly cancer and cardiovascular-related. However, adjusted HRs for death were 1.2 (P = 0.37) and 0.9 (P = 0.62) for Black and Hispanic patients, respectively, compared with White patients and 0.9 (P = 0.63) for Hispanic compared with Black patients. Adjustment for adherence did not change inferences for AIDS or death.
CONCLUSIONS
In the setting of similar access to care, we did not observe a disparity for the risk of clinical events for racial/ethnic minorities, despite lower ART adherence.



Similar content being viewed by others
References
CDC. Racial/ethnic disparities in diagnoses of HIV/AIDS–33 states, 2001–2005. MMWR Morb Mortal Wkly Rep. 2007;56:189–93.
CDC. HIV/AIDS Surveillance Report, 2005. 2007;17:1–54.
Heron MP, Smith BL. Deaths: leading causes for 2003. Hyattsville, MD: National vital statistics reports; 2007;15:1–92.
Anastos K, Schneider MF, Gange SJ, et al. The association of race, sociodemographic, and behavioral characteristics with response to highly active antiretroviral therapy in women. J Acquir Immune Defic Syndr. 2005;39:537–44.
Giordano TP, Morgan RO, Kramer JR, et al. Is there a race-based disparity in the survival of veterans with HIV? J Gen Intern Med. 2006;21:613–7.
Jensen-Fangel S, Pedersen L, Pedersen C, et al. The effect of race/ethnicity on the outcome of highly active antiretroviral therapy for human immunodeficiency virus type 1-infected patients. Clin Infect Dis. 2002;35:1541–48.
Poundstone KE, Chaisson RE, Moore RD. Differences in HIV disease progression by injection drug use and by sex in the era of highly active antiretroviral therapy. AIDS. 2001;15:1115–23.
Silverberg MJ, Wegner SA, Milazzo MJ, et al. Effectiveness of highly-active antiretroviral therapy by race/ethnicity. AIDS. 2006;20:1531–8.
Smith PR, Sarner L, Murphy M, et al. Ethnicity and discordance in plasma HIV-1 RNA viral load and CD4+ lymphocyte count in a cohort of HIV-1-infected individuals. J Clin Virol. 2003;26:101–7.
Tedaldi EM, Absalon J, Thomas AJ, Shlay JC, van den Berg-Wolf M. Ethnicity, race, and gender. Differences in serious adverse events among participants in an antiretroviral initiation trial: results of CPCRA 058 (FIRST Study). J Acquir Immune Defic Syndr. 2008;47:441–8.
McGinnis KA, Fine MJ, Sharma RK, et al. Understanding racial disparities in HIV using data from the veterans aging cohort 3-site study and VA administrative data. Am J Public Health. 2003;93:1728–33.
Merriman NA, Porter SB, Brensinger CM, Reddy KR, Chang KM. Racial difference in mortality among U.S. veterans with HCV/HIV coinfection. Am J Gastroenterol. 2006;101:760–7.
Messeri P, Lee G, Abramson DM, Aidala A, Chiasson MA, Jessop DJ. Antiretroviral therapy and declining AIDS mortality in New York City. Med Care. 2003;41:512–21.
Gordon NP. How does the adult kaiser permanente membership in Northern California compare with the larger community? Oakland: KP Division of Research; 2009. Available at: http://www-dor.kaiser.org/dor/mhsnet/public/kpnc_community.htm. Accessed June 4, 2009.
US Department of Health and Human Services. Guidelines for the use of antiretroviral agents in HIV-1-Infected adults and adolescents. Available at: http://aidsinfo.nih.gov/contentfiles/AdultandAdolescentGL.pdf. Accessed June 4, 2009.
Horberg MA, Hurley LB, Silverberg MJ, Kinsman CJ, Quesenberry CP. Effect of clinical pharmacists on utilization of and clinical response to antiretroviral therapy. J Acquir Immune Defic Syndr. 2007;44:531–9.
Silverberg MJ, Leyden W, Horberg MA, DeLorenze GN, Klein D, Quesenberry CP Jr. Older age and the response to and tolerability of antiretroviral therapy. Arch Intern Med. 2007;167:684–91.
Steiner JF, Prochazka AV. The assessment of refill compliance using pharmacy records: methods, validity, and applications. J Clin Epidemiol. 1997;50:105–16.
Centers for Disease Control and Prevention. 1993 revised classification system for HIV infection and expanded surveillance case definition for AIDS among adolescents and adults. MMWR. 1992;41:1–19.
Bendel RB, Afifi AA. Comparison of stopping rules in forward "stepwise" regression. J Am Stat Assoc. 1977;72:46–53.
Hosmer DW, Lemeshow S. Applied logistic regression, second edition. Hoboken, NJ: John Wiley & Sons, Inc.; 2000.
Cox DR, Oates D. Analysis of survival data. London and New York: Chapman and Hall; 1984.
Diggle PJ, Liang KY, Zeger SL. Analysis of longitudinal data. New York, NY: Oxford University Press; 1995.
Epidemiology of HIV/AIDS–United States, 1981–2005. MMWR Morb Mortal Wkly Rep. Jun 2 2006;55:589–92.
Hayes-Bautista DE, Baezconde-Garbanati L, Schink WO, Hayes-Bautista M. Latino health in California, 1985–1990: implications for family practice. Fam Med. 1994;26:556–62.
Markides KS, Coreil J. The health of Hispanics in the southwestern United States: an epidemiologic paradox. Public Health Rep. 1986;101:253–65.
Krieger N. Overcoming the absence of socioeconomic data in medical records: validation and application of a census-based methodology. Am J Public Health. 1992;82:703–10.
Kleeberger CA, Phair JP, Strathdee SA, Detels R, Kingsley L, Jacobson LP. Determinants of heterogeneous adherence to HIV-antiretroviral therapies in the Multicenter AIDS Cohort Study. J Acquir Immune Defic Syndr. 2001;26:82–92.
Kleeberger CA, Buechner J, Palella F, et al. Changes in adherence to highly active antiretroviral therapy medications in the Multicenter AIDS Cohort Study. AIDS. 2004;18:683–88.
Li X, Margolick JB, Conover CS, et al. Interruption and discontinuation of highly active antiretroviral therapy in the multicenter AIDS cohort study. J Acquir Immune Defic Syndr. 2005;38:320–28.
Golin CE, Liu H, Hays RD, et al. A prospective study of predictors of adherence to combination antiretroviral medication. J Gen Intern Med. 2002;17:756–65.
Gifford AL, Bormann JE, Shively MJ, Wright BC, Richman DD, Bozzette SA. Predictors of self-reported adherence and plasma HIV concentrations in patients on multidrug antiretroviral regimens. J Acquir Immune Defic Syndr. 2000;23:386–95.
Smith CJ, Sabin CA, Youle MS, et al. Factors influencing increases in CD4 cell counts of HIV-positive persons receiving long-term highly active antiretroviral therapy. J Infect Dis. 2004;190:1860–8.
Hartzell JD, Spooner K, Howard R, Wegner S, Wortmann G. Race and mental health diagnosis are risk factors for highly active antiretroviral therapy failure in a military cohort despite equal access to care. J Acquir Immune Defic Syndr. 2007;44:411–6.
Schackman BR, Ribaudo HJ, Krambrink A, Hughes V, Kuritzkes DR, Gulick RM. Racial differences in virologic failure associated with adherence and quality of life on efavirenz-containing regimens for initial HIV therapy: results of ACTG A5095. J Acquir Immune Defic Syndr. 2007;46:547–54.
Kumar PN, Rodriguez-French A, Thompson MA, et al. A prospective, 96-week study of the impact of Trizivir, Combivir/nelfinavir, and lamivudine/stavudine/nelfinavir on lipids, metabolic parameters and efficacy in antiretroviral-naive patients: effect of sex and ethnicity. HIV Med. 2006;7:85–98.
Giordano TP, Wright JA, Hasan MQ, White AC Jr., Graviss EA, Visnegarwala F. Do sex and race/ethnicity influence CD4 cell response in patients who achieve virologic suppression during antiretroviral therapy? Clin Infect Dis. 2003;37:433–37.
Lucas GM, Chaisson RE, Moore RD. Highly active antiretroviral therapy in a large urban clinic: risk factors for virologic failure and adverse drug reactions. Ann Intern Med. 1999;131:81–7.
ACKNOWLEDGMENTS
This material was presented at the 4th International AIDS Society Conference on HIV Pathogenesis, Treatment, and Prevention, Sydney, Australia, July 22–25, 2007 (#WEPEB107). This research was supported by a Community Benefit grant from Kaiser Permanente Northern California. Dr. Silverberg’s contribution was also supported in part by grant number K01AI071725 from the NIAID. We would like to thank Leo Hurley for assistance with data analysis and helpful discussions during manuscript preparation.
Conflict of Interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Silverberg, M.J., Leyden, W., Quesenberry, C.P. et al. Race/Ethnicity and Risk of AIDS and Death Among HIV-infected Patients with Access to Care. J GEN INTERN MED 24, 1065–1072 (2009). https://doi.org/10.1007/s11606-009-1049-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-009-1049-y