Abstract
Background
Morbidity after pancreas resection is still high with postoperative pancreatic fistulas (POPF) being the most frequent complication. However, exocrine insufficiency seems to protect from POPF. In clinical practice, patients showing increased postoperative systemic amylase concentrations appear to frequently develop POPF. We therefore retrospectively examined the occurrence of systemic amylase increase after pancreas resections and its association with the clinical course.
Patients and Methods
Perioperative data from 739 consecutive pancreas resections were assessed in a prospectively maintained SPSS database. Serum and drain amylase concentrations were determined by routine clinical chemistry. POPFs were graded into A–C according to ISGPF definitions.
Results
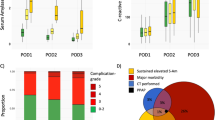
In patients with reduced serum amylase (n = 89) on day 1 after pancreatoduodenectomy, clinically relevant POPFs were not observed. In patients with normal serum amylase concentrations, clinically relevant POPFs occurred in 9 %, while in 39 % of the patients with more than three times elevated amylase concentrations, a clinically relevant postoperative fistula was observed (p < 0.001). Systemic hyperamylasemia detected on postoperative day 1 after pancreatoduodenectomy was further a good predictor for clinically relevant POPFs (AUROC = 0.797, p < 0.001).
Conclusion
Patients with a high risk for developing clinically relevant POPFs can be identified on the first postoperative day by determining serum amylase.





Similar content being viewed by others
References
Wittel, U. A. et al. Retrospective analyses of trends in pancreatic surgery: indications, operative techniques, and postoperative outcome of 1,120 pancreatic resections. World J. Surg. Oncol. 13, 102 (2015).
Fahy, B. N., Frey, C. F., Ho, H. S., Beckett, L. & Bold, R. J. Morbidity, mortality, and technical factors of distal pancreatectomy. Am. J. Surg. 183, 237–241 (2002).
Katsourakis, A. et al. Does Prophylactic Administration of Somatostatin Decrease the Rates of Complications After Pancreatic Resection?: A Clinical and Electron Microscopy Study. Pancreas 42, 37–41 (2013).
Bassi, C. et al. Postoperative pancreatic fistula: An international study group (ISGPF) definition. Surgery 138, 8–13 (2005).
Hassenpflug, M. et al. Decrease in clinically relevant pancreatic fistula by coverage of the pancreatic remnant after distal pancreatectomy. Surgery 152, S164–S171 (2012).
Diener, M. K. et al. Efficacy of stapler versus hand-sewn closure after distal pancreatectomy (DISPACT): a randomised, controlled multicentre trial. The Lancet 377, 1514–1522 (2011).
Wellner, U. F. et al. Randomized controlled single-center trial comparing pancreatogastrostomy versus pancreaticojejunostomy after partial pancreatoduodenectomy. J. Gastrointest. Surg. Off. J. Soc. Surg. Aliment. Tract 16, 1686–1695 (2012).
Crippa, S. et al. Pancreaticojejunostomy is comparable to pancreaticogastrostomy after pancreaticoduodenectomy: an updated meta-analysis of randomized controlled trials. Langenbecks Arch. Surg. 401, 427–437 (2016).
Callery, M. P., Pratt, W. B., Kent, T. S., Chaikof, E. L. & Vollmer, C. M. A prospectively validated clinical risk score accurately predicts pancreatic fistula after pancreatoduodenectomy. J. Am. Coll. Surg. 216, 1–14 (2013).
McMillan, M. T. et al. Drain Management after Pancreatoduodenectomy: Reappraisal of a Prospective Randomized Trial Using Risk Stratification. J. Am. Coll. Surg. 221, 798–809 (2015).
Palani Velu, L. K. et al. Serum amylase and C-reactive protein in risk stratification of pancreas-specific complications after pancreaticoduodenectomy. Br. J. Surg. 103, 553–563 (2016).
Cloyd, J. M., Kastenberg, Z. J., Visser, B. C., Poultsides, G. A. & Norton, J. A. Postoperative serum amylase predicts pancreatic fistula formation following pancreaticoduodenectomy. J. Gastrointest. Surg. Off. J. Soc. Surg. Aliment. Tract 18, 348–353 (2014).
Liu, Q.-Y. et al. Analysis of risk factors for postoperative pancreatic fistula following pancreaticoduodenectomy. World J. Gastroenterol. 20, 17491–17497 (2014).
Uomo, G. et al. The incidence of main pancreatic duct disruption in severe biliary pancreatitis. Am. J. Surg. 176, 49–52 (1998).
Lau, S. T., Simchuk, E. J., Kozarek, R. A. & Traverso, L. W. A pancreatic ductal leak should be sought to direct treatment in patients with acute pancreatitis. Am. J. Surg. 181, 411–415 (2001).
Fujiwara, Y. et al. A novel postoperative inflammatory score predicts postoperative pancreatic fistula after pancreatic resection. Anticancer Res. 33, 5005–5010 (2013).
Ridolfi, C. et al. Morphohistological features of pancreatic stump are the main determinant of pancreatic fistula after pancreatoduodenectomy. BioMed Res. Int. 2014, 641239 (2014).
Okabayashi, T. et al. Postoperative pancreatic fistula following distal pancreatectomy for pancreatic neoplasm; can pancreatic fistula be prevented? Hepatogastroenterology. 51, 1838–1841 (2004).
Palani Velu, L. K. et al. Serum amylase on the night of surgery predicts clinically significant pancreatic fistula after pancreaticoduodenectomy. HPB 16, 610–619 (2014).
Lermite, E. et al. Risk Factors of Pancreatic Fistula and Delayed Gastric Emptying after Pancreaticoduodenectomy with Pancreaticogastrostomy. J. Am. Coll. Surg. 204, 588–596 (2007).
Bassi, C. et al. Reconstruction by pancreaticojejunostomy versus pancreaticogastrostomy following pancreatectomy: results of a comparative study. Ann. Surg. 242, 767–773 (2005)
Wente, M. N. et al. Pancreaticojejunostomy versus pancreaticogastrostomy: systematic review and meta-analysis. Am. J. Surg. 193, 171–183 (2007).
Koch, M. et al. Bile leakage after hepatobiliary and pancreatic surgery: A definition and grading of severity by the International Study Group of Liver Surgery. Surgery 149, 680–688 (2011).
Acknowledgments
Author Contributions
U.W. and C.K. designed the study; N.S. acquired the data; N.S. analyzed the data; C.K., O.S., and F.M. interpreted the data and performed statistical analysis. C.K. and U.W. wrote the manuscript. F.M. and U.H. helped revise the manuscript. All authors discussed the data and the analysis methods and contributed to the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this study.
Conflict of Interest
The authors declare that they have no conflicts of interest.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 36 kb)
Rights and permissions
About this article
Cite this article
Kühlbrey, C.M., Samiei, N., Sick, O. et al. Pancreatitis After Pancreatoduodenectomy Predicts Clinically Relevant Postoperative Pancreatic Fistula. J Gastrointest Surg 21, 330–338 (2017). https://doi.org/10.1007/s11605-016-3305-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-016-3305-x