Abstract
Purpose
Bevacizumab has been shown to increase progression free and overall survival in patients with metastatic colorectal cancer. Neoadjuvant bevacizumab is commonly used in patients undergoing liver resection. Our purpose was to evaluate whether bevacizumab is associated with increased rate of perioperative complications in patients undergoing hepatic resection for colorectal liver metastases (CRLM).
Methods
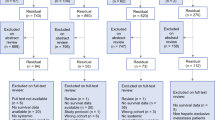
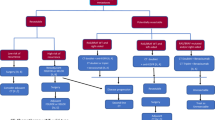
Retrospective analysis of patients undergoing hepatic resection for CRLM who received chemotherapy and bevacizumab (group 1, n = 134), or chemotherapy alone (group 2, n = 57). We compared demographics, surgical characteristics, and perioperative course.
Results
Perioperative complications developed in 35 % of patients in group 1, and 47 % in group 2 (p = 0.11). Of those complications, 15 (11.2 %) in group 1, and 5 (8.8 %) in group 2 were considered major (p = 0.617). Four patients, all of whom received preoperative bevacizumab, developed enteric leaks following combined liver and bowel resection. The rate of anastomotic leak in group 1 was 10 %, compared with 0 in group 2, p = 0.56.
Conclusion
Neoadjuvant chemotherapy along with bevacizumab was not associated with an increased risk of postoperative complications after hepatic resection. Possible association of increased morbidity with simultaneous bowel and liver resections following bevacizumab administration was found and we recommend avoiding such treatment combination.
Similar content being viewed by others
References
Jemal A, Siegel R, Xu J et al. Cancer statistics. Cancer J Clin 2010 60(5):277–300.
Scheele J, Stangl R, Altendorf-Hofmann A. Hepatic metastases from colorectal carcinoma: impact of surgical resection on natural history. Br J Surg 1990;77(11):1241–6.
Labianca R, Beretta GD, Kildani B et al. Colon cancer. Crit Rev Oncol Hematol 2010;74(2):106–33.
Zelek L, Bugat R, Cherqui D et al. Multimodal therapy with intravenous biweekly leucovorin, 5-fluorouracil and irinotecan combined with hepatic arterial infusion pirarubicin in non-resectable hepatic metastases from colorectal cancer (a European Association for Research Oncology trial). Ann Oncol 2003;14(10):1537–42.
Bismuh H, Adam R, Levi F et al. Resection of nonresectable liver metastases from colorectal cancer after neoadjuvant chemotherapy. Ann Surg 1996;224(4):509–20.
Adam R, Delvart V, Pascal G et al. Rescue surgery for unresectable colorectal liver metastases downstaged by chemotherapy: a model to predict long-term survival. Ann Surg 2004;240(4):644–57.
Saif MW. Secondary hepatic resection as a therapeutic goal in advanced colorectal cancer. World J Gastroenterol 2009 12;15(31):3855–64.
Popescu I, Alexandrescu S, Croitoru A et al. Strategies to convert to resectability the initially unresectable colorectal liver metastases. Hepatogastroenterology 2009 56(91–92):739–44.
Bertolini F, Malavasi N, Scarabelli L et al. FOLFOX6 and bevacizumab in non-optimally resectable liver metastases from colorectal cancer. Br J Can 2011 29;104(7):1079–84.
Hurwitz H, Fehrenbacher L, Novotny W et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Eng J Med 2004 3;350(23):2335–42.
Scappaticci FA, Skillings JR, Holden SN et al. Arterial thromboembolic events in patients with metastatic carcinoma treated with chemotherapy and bevacizumab. J Natl Can Inst 2007 15;99(16):1232–9.
Wu S, Kim C, Baer L et al. Bevacizumab increases risk for sever proteinuria in cancer patients. J Am Soc Nephrol 2010;21(8):1381–9.
Elice F, Rodegheiro F. Bleeding complications of antiangiogenic therapy: pathogenetic mechanism and clinical impact. Thromb Res 2010;125 Suppl 2;S55–S57
Chaundhury P, Hassanain M, Bouganim N et al. Perioperative chemotherapy with bevacizumab and liver resection for colorectal liver metastases. HPB(Oxford).2010;12:37–42
Kemeny N. Presurgical chemotherapy in patients being considered for liver resection. The Oncologist 2007;12:825–39.
Folprecht G, Grothey A, Alberts S et al. Neoadjuvant treatment of unresectable colorectal liver metastases: correlation between tumour response and resection rates. Ann Oncol 2005;16:1311–9.
Pozzo C, Basso M, Cassano A et al. Neoadjuvant treatment of unresectable liver disease with irinotecan and 5-fluorouracil plus folinic acid in colorectal cancer patients. Ann Oncol 2004;15:933–9.
Small RM, Lubezky N, Shmueli E et al. Response to chemotherapy predicts survival following resection of hepatic colorectal metastases in patients treated with neoadjuvant therapy. J Surg Oncol 2009 1;99(2):93–8.
Vauthey JN, Pawlick TM, Ribero D et al. Chemotherapy regimen predicts steatohepatitis and an increase in 90-day mortality after surgery for hepatic metastases. J Clin Oncol 2006;24:2065–2072.
Rubbia-Brandt L, Audard V, Satoretti P et al. Severe hepaic sinusoidal obstruction associated with oxaliplatin-based chemotherapy in patients with metastatic colorectal cancer. Ann Oncol 2004;15:460–6
Aloia T, Sebagh M, Plasse M et al. Liver histology and surgical outcomes after preoperative chemotherapy with fluorouracil plus oxaliplatin in colorectal cancer liver metastases. J Clin Oncol 24:4983–90, 2006.
Tamandl D, Gruenberger B, Klinger M et al. Liver resection remains a safe procedure after neoadjuvant chemotherapy sincluding bevacizumab. A case-controlled study. Ann Surg 2010;252:124–130.
Scappaticci FA, Fehrenbacher L et al. Phase 2, randomized trial comparing bevacizumab plus fluorouracil (FU)/leucovorin (LV) with FU/LV alone in patients with metastatic colorectal cancer. J Surg Oncol. 91:173–180, 2005.
Reddy SK, Morse MA, Hurwitz HI, et al. Addition of bevacizumab to irinotecan- and oxaliplatin- based preoperative chemotherapy regimens does not increase morbidity after resection of colorectal liver metastases. J Am Coll Surg 2008;206:96–106.
D’Angelica M, Kornprat P, Mithat G, et al. Lack of evidence for increased operative morbidity after hepatectomy with perioperative use of bevacizumab: a matched case–control study. Ann Surg Oncol 2007;14(2):759–65.
Kesmodel SB, Ellis LM, Lin E, et al. Preoperative bevacizumab does not significantly increase postoperative complication rates in patients undergoing hepatic surgery for colorectal cancer liver metastases. J Clin Oncol 2007;26:5254–60.
Mahfud M, Breitenstein S, El-Badry AM, et al. Impact of preoperative bevacizumab on complications after resection of colorectal liver metastases: case-matched control study. World J Surg (2010) 34:92–100.
Ribero D, Wang H, Donadon M, et al. Bevacizumab improves pathologic response and protects against hepatic injury in patients treated with oxaliplatin-based chemotherapy for colorectal liver metastases. Cancer (2007) 110:2761–2767.
Financial Support
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lubezky, N., Winograd, E., Papoulas, M. et al. Perioperative Complications After Neoadjuvant Chemotherapy With and Without Bevacizumab for Colorectal Liver Metastases. J Gastrointest Surg 17, 527–532 (2013). https://doi.org/10.1007/s11605-012-2108-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-012-2108-y