Abstract
Purpose
Pancreaticoduodenectomy (PD) is the most frequently performed resectional procedure in chronic pancreatitis. Only a few studies have evaluated quality of life (QOL) after PD for chronic pancreatitis. This retrospective study examined long-term quality of life and relief of symptoms in a homogenous consecutive cohort of 67 patients undergoing PD for chronic pancreatitis.
Methods
A standard QOL questionnaire was sent to 168 patients after PD who had undergone PD for chronic pancreatitis at the University Hospital Dresden between 1994 and 2008. QOL and long-term sequelae were evaluated by the EORTC quality of life questionnaire supplemented with complementary questions. Results were compared to general population data based on large random samples.
Results
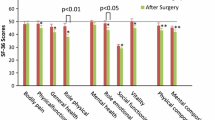
Median follow-up was 69.1 months. Complete response was obtained from 67 (48.5%) patients. Long-term survival of our patients was lower than expected rates based on the Federal Republic of Germany life table analysis (p < 0.001). There was an improved pain control and an increase in weight gain. Overall, QOL scores were slightly inferior to those of the control group. A common problem after PD was onset of diabetes mellitus; however, exocrine function of the pancreas was stable.
Conclusions
This is the largest single-institution experience assessing QOL after PD for chronic pancreatitis. Most patients have QOL scores comparable to those of the control patients and can function independently in daily activities.



Similar content being viewed by others
References
Sohn TA, Campbell KA, Pitt HA, Sauter PK, Coleman JA, Lillemo KD, Yeo CJ, Cameron JL. Quality of life and long-term survival after surgery for chronic pancreatitis. J Gastrointest Surg 2000; 4: 355–364; discussion 364–355.
Ammann RW, Akovbiantz A, Largiader F, Schueler G. Course and outcome of chronic pancreatitis. Longitudinal study of a mixed medical-surgical series of 245 patients. Gastroenterology 1984; 86: 820–828.
Sakorafas GH, Sarr MG. Changing trends in operations for chronic pancreatitis: a 22-year experience. Eur J Surg 2000; 166: 633–637.
Balcom JH, Rattner DW, Warshaw AL, Chang Y, Fernandez-del Castillo C. Ten-year experience with 733 pancreatic resections: changing indications, older patients, and decreasing length of hospitalization. Arch Surg. 2001; 136:391–398.
Trede M, Schwall G, Saeger HD. Survival after pancreatoduodenectomy. 118 consecutive resections without an operative mortality. Ann Surg 1990; 211: 447–458.
Huang JJ, Yeo CJ, Sohn TA, Lillemoe KD, Sauter PK, Coleman J, Hruban RH, Cameron JL. Quality of life and outcomes after pancreaticoduodenectomy. Ann Surg 2000; 231: 890–898.
Sakorafas GH, Farnell MB, Farley DR, Rowland CM, Sarr MG. Long-term results after surgery for chronic pancreatitis. Int J Pancreatol 2000; 27: 131–142.
Rumstadt B, Forssmann K, Singer MV, Trede M. The Whipple partial duodenopancreatectomy for the treatment of chronic pancreatitis. Hepatogastroenterology 1997; 44: 1554–1559.
Aaronson NK, Ahmedzai S, Bergman B, Bullinger M, Cull A, Duez NJ, Filiberti A, Flechtner H, Fleishman SB, de Haes JC, et al. The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 1993; 85: 365–376.
Hjermstad MJ, Fayers PM, Bjordal K, Kaasa S. Health-related quality of life in the general Norwegian population assessed by the European Organization for Research and Treatment of Cancer Core Quality-of-Life Questionnaire: the QLQ = C30 (+ 3). J Clin Oncol 1998; 16: 1188–1196.
Michelson H, Bolund C, Brandberg Y. Multiple chronic health problems are negatively associated with health related quality of life (HRQoL) irrespective of age. Qual Life Res 2000; 9: 1093–1104.
Mannell A, Adson MA, McIlrath DC, Ilstrup DM. Surgical management of chronic pancreatitis: long-term results in 141 patients. Br J Surg 1988; 75: 467–472.
Izbicki JR, Bloechle C, Broering DC, Knoefel WT, Kuechler T, Broelsch CE. Extended drainage versus resection in surgery for chronic pancreatitis: a prospective randomized trial comparing the longitudinal pancreaticojejunostomy combined with local pancreatic head excision with the pylorus-preserving pancreatoduodenectomy. Ann Surg 1998; 228: 771–779.
Lankisch PG. Natural course of chronic pancreatitis. Pancreatology 2001; 1: 3–14.
Traverso LW, Kozarek RA. The Whipple procedure for severe complications of chronic pancreatitis. Arch Surg 1993; 128: 1047–1050; discussion 1051–1043.
Shah NS, Makin AJ, Sheen AJ, Siriwardena AK. Quality of life assessment in patients with chronic pancreatitis receiving antioxidant therapy. World J Gastroenterol 2010; 16: 4066–4071.
Howard JM, Zhang Z. Pancreaticoduodenectomy (Whipple resection) in the treatment of chronic pancreatitis. World J Surg 1990; 14: 77–82.
Evans JD, Wilson PG, Carver C, Bramhall SR, Buckels JA, Mayer AD, McMaster P, Neoptolemos JP. Outcome of surgery for chronic pancreatitis. Br J Surg 1997; 84: 624–629.
Traverso LW, Kozarek RA. Pancreatoduodenectomy for chronic pancreatitis: anatomic selection criteria and subsequent long-term outcome analysis. Ann Surg 1997; 226: 429–435; discussion 435–428.
Stone WM, Sarr MG, Nagorney DM, McIlrath DC. Chronic pancreatitis. Results of Whipple's resection and total pancreatectomy. Arch Surg 1988; 123: 815–819.
Melvin WS, Buekers KS, Muscarella P, Johnson JA, Schirmer WJ, Ellison EC. Outcome analysis of long-term survivors following pancreaticoduodenectomy. J Gastrointest Surg 1998; 2: 72–78.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rückert, F., Distler, M., Hoffmann, S. et al. Quality of Life in Patients After Pancreaticoduodenectomy for Chronic Pancreatitis. J Gastrointest Surg 15, 1143–1150 (2011). https://doi.org/10.1007/s11605-011-1539-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-011-1539-1