Abstract
Objectives
Cerebral microembolization, one of the most frequent complications of carotid artery stenting, is associated with an increased risk of peri- and post-procedural stroke and transient ischemic attack and a mid-term risk of neurocognitive decline. A valuable tool to evaluate carotid plaque instability and risk of embolization is contrast-enhanced ultrasound. With this prospective study we sought to determine the correlation between contrast enhancement of the plaque and cerebral microembolization after carotid stent deployment and to evaluate the clinical impact of the neurological injury.
Materials and methods
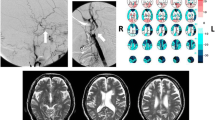
Thirty-five consecutive patients with carotid artery stenosis and indications for endovascular stenting were enrolled. Before the procedure, patients were evaluated with contrast-enhanced ultrasound to define plaque enhancement (signal intensity). All endovascular procedures were performed under cerebral filter protection. Diffusion-weighted magnetic resonance imaging scans to detect microemboli were obtained before and 48 h after the stent deployment. The Ray auditory verbal learning test to assess neurocognitive function was administered before and 1 month after the procedure.
Results
Nineteen patients (54 %) developed new cerebral ischemic lesions after carotid artery stenting. Contrast enhancement of the plaque was greater in the patients with post-procedural microembolization than in those without it [maximum signal intensity 26 ± 7.7 vs. 21 ± 5.2, respectively, (p = 0.039), mean signal intensity, 20.7 ± 6.1 vs. 16.5 ± 5.3, respectively (p = 0.048)]. No correlation was found between neurocognitive test scores and microembolization or plaque enhancement.
Conclusion
Contrast enhancement of the carotid plaque is strongly associated with post-procedural microembolization and for this reason it can be considered a reliable tool for an accurate selection of patients undergoing this endovascular treatment. However, the neurocognitive test scores performed in this study are not enough sensible to appreciate the impact of the neurological injury on the day life activities.

Similar content being viewed by others
References
Maggio P, Altamusa C, Landi D, Migliore S, Lupoi D, Moffa F et al (2013) Diffusion weighted lesions after carotid artery stenting are associated with cognitive impairment. J Neurol Sci 328:58–63
Yamada R, Anderson MB, Guimaraes M, Schönholz C (2013) Carotid stenting in asymptomatic patients: how to identify patients without symptoms and at high risk for neurologic events. J Cardiovasc Surg 54:55–59
Capoccia L, Speziale F, Gazzetti M, Mariani P, Rizzo A, Mansour W et al (2010) Comparative study on carotid revascularization (endoarterectomy vs stenting) using markers of cellular brain injury, neuropsychometric tests, and diffusion-weighted magnetic resonance imaging. J Vasc Surg 51:584–592
Zhou W, Hitchner E, Gillis K, Sun L, Floyd R, Lane B et al (2012) Prospective neurocognitive evaluation of patients undergoing carotid interventions. J Vasc Surg 56(6):1571–1578
Varetto G, Gibello L, Bergamasco L, Sapino A, Castellano I, Garneri P et al (2012) Contrast enhanced ultrasound in atherosclerotic carotid artery disease. Int Angiol 31(6):565–571
Ten Kate GL, van den Oord SC, Sijbrands EJ, van der Lugt A, de Jong N, Bosch JG et al (2013) Current status and future developments of contrast-enhanced ultrasound of carotid atherosclerosis. J Vasc Surg 57(2):539–546
Clevert DA, Paprottka P, Sommer WH, Helck A, Reiser MF, Zengel P (2013) The role of contrast-enhanced ultrasound in imaging carotid arterial diseases. Semin Ultrasound CT MR 34:204–212
Ritter MA, Theismann K, Schmiedel M, Ringelstein BE, Dittrich R (2013) Vascularization of carotid plaque in recently symptomatic patients is associated with the occurrence of transcranial microembolic signals. Eur J Neurol 20:1218–1221
Bijuklic K, Wandler A, Varnakov Y, Tuebler T, Schofer J (2013) Risk factors for cerebral embolization after carotid artery stenting with embolic protection: a diffusion-weighted magnetic resonance imaging study in 837 consecutive patients. Circ Cardiovasc Interv 6(3):311–316
Antignani PL, Benedetti-Valentini F, Aluigi L, Baroncelli TA, Camporese G, Failla G et al (2012) Diagnosis of vascular diseases. Ultrasound investigations—guidelines. Int Angiol 31:1–77
Mauri G, Porazzi E, Cova L, Restelli U, Tondolo T, Bonfanti M et al (2014) Intraprocedural contrast-enhanced ultrasound (CEUS) in liver percutaneous radiofrequency ablation: clinical impact and health technology assessment. Insights Imaging 5(2):209–216
Liu ZJ, Fu WG, Guo ZY, Shen LG, Shi ZY, Li HJ (2012) Updated systematic review and meta-analysis of randomized clinical trials comparing carotid artery stenting and carotid endarterectomy in the treatment of carotid stenosis. Ann Vasc Surg 26(4):576–590
Brewster LP, Beaulieu R, Corriere MA, Veeraswamy R, Niazi KA, Robertson G et al (2011) Carotid revascularization outcome comparing distal filters, flow reversal, and endoarterectomy. J Vasc Surg 54:1000–1004
Zhu L, Wintermark M, Saloner D, Fandel M, Pan XM, Rapp JH (2011) The distribution and size of ischemic lesions after carotid artery angioplasty and stenting: evidence for microembolization to terminal arteries. J Vasc Surg 53:971–976
Schreiber S, Serdaroglu M, Schreiber F, Skalij M, Heinze HJ, Goertler M (2009) Simultaneous occurrence and interaction of hypoperfusion and embolism in a patient with severe middle cerebral artery stenosis. Stroke 40:478–480
Conflict of interest
None.
Ethical standards
This article does not contain any studies with human participants or animals performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Varetto, G., Gibello, L., Faletti, R. et al. Contrast-enhanced ultrasound to predict the risk of microembolization during carotid artery stenting. Radiol med 120, 1050–1055 (2015). https://doi.org/10.1007/s11547-015-0530-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-015-0530-4