Abstract
Purpose
The aim of this study was to analyze the prevalence and association between sleep quality with gender and age and to examine the relation between age and the components of the PSQI in institutionalized adolescents.
Methods
High school internal students of both genders, aged between 14 and 19 years old, were analyzed. After a full clinical evaluation, the Pittsburg Sleep Quality Index Score was obtained from all participants.
Results
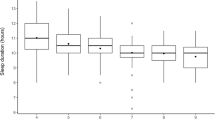
We studied 210 participants [male: 15. 7 ± 1.2 years; BMI: 21.7 ± 2.6 kg/m2; female: 15.7 ± 1. 2 years; BMI: 21.9 ± 4.5 kg/m2]. Poor sleep quality was present in 137 (65.3%) participants and was predominant among girls than boys (PSQI = 76.3 vs 55.8%; p < 0.001), respectively. There were positive correlations between PSQI components with age in boys (sleep latency: R = 0.23; p = 0.02; sleep duration: R = 0.28; p < 0.01 and overall sleep quality: R = 0.21; p = 0.03), but not among girls.
Conclusion
Institutionalized girls have worse sleep quality than boys and positive correlations between sleep quality components with age were only present among boys.

Similar content being viewed by others
References
Van Dongen HP, Dinges DF (2003) Investigating the interaction between the homeostatic and circadian processes of sleep-wake regulation for the prediction of waking neurobehavioural performance. J Sleep Res 12(3):181–187
Perkinson-Gloor N, Lemola S, Grob A (2013) Sleep duration, positive attitude toward life, and academic achievement: the role of daytime tiredness, behavioral persistence, and school start times. J Adolesc 36(2):311–318
Colrain IM, Baker FC (2011) Changes in sleep as a function of adolescent development. Neuropsychol Rev 21(1):5–21
Short MA, Gradisar M, Lack LC, Wright HR, Chatburn A (2013) Estimating adolescent sleep patterns: parent reports versus adolescent self-report surveys, sleep diaries, and actigraphy. Nat Sci Sleep 5:23–26. doi:10.2147/NSS.S38369
Carskadon MA, Acebo C, Jenni OG (2004) Regulation of adolescent sleep: implications for behavior. Ann N Y Acad Sci 1021(1):276–291
Myllymaki T, Kyrolainen H, Savolainen K, Hokka L, Jakonen R, Juuti T, Martinmaki K, Kaartinen J, Kinnunen ML, Rusko H (2011) Effects of vigorous late-night exercise on sleep quality and cardiac autonomic activity. J Sleep Res 20(1 Pt 2):146–153. doi:10.1111/j.1365-2869.2010.00874.x
Bertolazi AN, Fagondes SC, Hoff LS, Dartora EG, da Silva Miozzo IC, de Barba MEF, Barreto SSM (2011) Validation of the Brazilian Portuguese version of the Pittsburgh sleep quality index. Sleep Med 12(1):70–75
Mondal P, Gjevre JA, Taylor-Gjevre RM, Lim HJ (2013) Relationship between the Pittsburgh Sleep Quality Index and the Epworth Sleepiness Scale in a sleep laboratory referral population. Nat Sci Sleep 5:15–21
Roberts RE, Roberts CR, Chen IG (2000) Ethnocultural differences in sleep complaints among adolescents. J Nerv Ment Dis 188(4):222–229
Schleider K, Güntert M (2009) Characteristics and conditions of the student’s learning and work disruptions-an inventory. Beiträge zur Hochschulforschung, German
Matos MG, Gaspar T, Tome G, Paiva T (2015) Sleep variability and fatigue in adolescents: associations with school-related features. Int J Psychol. doi:10.1002/ijop.12167
Lohman TG, Going SB (2006) Body composition assessment for development of an international growth standard for preadolescent and adolescent children. Food Nutr Bull 27(4 Suppl Growth Standard):S314–S325
Buysse DJ, Reynolds CF III, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh sleep quality index: a new instrument for psychiatric practice and research. Psychiatry Res 28(2):193–213
Bertolazi AN (2008) Tradução, adaptação cultural e validação de dois instrumentos de avaliação do sono: Escala de sonolência de Epworth e Índice de qualidade de sono de Pittsburgh
Van Reen E, Sharkey KM, Roane BM, Barker D, Seifer R, Raffray T, Bond TL, Carskadon MA (2013) Sex of college students moderates associations among bedtime, time in bed, and circadian phase angle. J Biol Rhythm 28(6):425–431. doi:10.1177/0748730413511771
Zhang B, Wing YK (2006) Sex differences in insomnia: a meta-analysis. Sleep 29(1):85–93
Hyde JS, Mezulis AH, Abramson LY (2008) The ABCs of depression: integrating affective, biological, and cognitive models to explain the emergence of the gender difference in depression. Psychol Rev 115(2):291–313. doi:10.1037/0033-295X.115.2.291
Dewald JF, Meijer AM, Oort FJ, Kerkhof GA, Bogels SM (2010) The influence of sleep quality, sleep duration and sleepiness on school performance in children and adolescents: a meta-analytic review. Sleep Med Rev 14(3):179–189. doi:10.1016/j.smrv.2009.10.004
Matricciani L, Olds T, Petkov J (2012) In search of lost sleep: secular trends in the sleep time of school-aged children and adolescents. Sleep Med Rev 16(3):203–211
Hysing M, Pallesen S, Stormark KM, Jakobsen R, Lundervold AJ, Sivertsen B (2015) Sleep and use of electronic devices in adolescence: results from a large population-based study. BMJ Open 5(1):e006748
Guo L, Deng J, He Y, Deng X, Huang J, Huang G, Gao X, Lu C (2014) Prevalence and correlates of sleep disturbance and depressive symptoms among Chinese adolescents: a cross-sectional survey study. BMJ Open 4(7):e005517
Orff HJ, Meliska C, Martinez L, Parry B (2014) The influence of sex and gonadal hormones on sleep disorders. ChronoPhysiol Ther 4:15–25
Baker FC, Driver HS (2007) Circadian rhythms, sleep, and the menstrual cycle. Sleep Med 8(6):613–622
Sack R, Auckley D, Auger R, Carsakadon M, Wright K, Vitiello M (2007) Circadian rhythm sleep disorders: part 11, advanced sleep phase disorder, free-running disorder, and irregular sleep-wake rhythm. Sleep 30:1484–1501
Crowley SJ, Acebo C, Carskadon MA (2007) Sleep, circadian rhythms, and delayed phase in adolescence. Sleep Med 8(6):602–612. doi:10.1016/j.sleep.2006.12.002
Raudenbush SW, Bryk AS, Cheong YF, Congdon RT, du Toit M (2011) Hierarchical linear and nonlinear modeling. SSI International, Lincolnwood
Lund HG, Reider BD, Whiting AB, Prichard JR (2010) Sleep patterns and predictors of disturbed sleep in a large population of college students. J Adolesc Health 46(2):124–132. doi:10.1016/j.jadohealth.2009.06.016
Kalak N, Brand S, Beck J, Holsboer-Trachsler E, Wollmer MA (2015) Association between subjective actual sleep duration, subjective sleep need, age, body mass index, and gender in a large sample of young adults. Neuropsychiatr Dis Treat 11:107–113. doi:10.2147/NDT.S74829
Pascotto ACS, Martins BR (2013) Avaliação da qualidade do sono em estudantes de ciências da saúde. J Health Sci Inst 31(3):306–310
Benitez A, Gunstad J (2012) Poor sleep quality diminishes cognitive functioning independent of depression and anxiety in healthy young adults. Clin Neuropsychol 26(2):214–223
Acknowledgements
This study was supported by the National Council for Scientific and Technological Development (CNPq), Coordination for the Improvement of Higher Level (or Education) Personnel (CAPES). We thank all adolescents and their families for participating in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
No funding was received for this research.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
da Cunha Silva Santiago, L., Batista, R.M.F., Lyra, M.J. et al. The role played by gender and age on poor sleep quality among institutionalized adolescents. Sleep Breath 21, 197–202 (2017). https://doi.org/10.1007/s11325-017-1463-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-017-1463-z