Abstract
Purpose
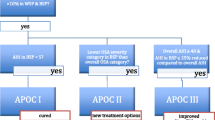
This study examined the effect of hypopnoea criteria on the prevalence of positional obstructive sleep apnoea (pOSA) identified under the Amsterdam Positional OSA Classification (APOC) system.
Methods
Three hundred three consecutive patients undertaking polysomnography (PSG) for the suspicion of OSA were included in this retrospective investigation. PSGs were scored using both the 2007 American Academy of Sleep Medicine (AASM) recommended hypopnoea criteria (AASM2007Rec) and the 2012 AASM recommended hypopnoea criteria (AASM2012Rec). For each hypopnoea criteria, OSA patients were grouped according to the APOC categories (I, II or II) or else deemed non-APOC if they did not meet the APOC criteria. Outcome measures, such as Functional Outcomes of Sleep Questionnaire (FOSQ), MOS 36-item short-form health survey (SF-36) and psychomotor vigilance task (PVT), were also compared between the groups.
Results
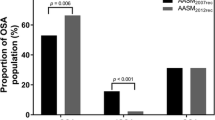
The AASM2012Rec increased the prevalence of OSA compared to AASM2007Rec. The AASM2012Rec trebled the number of APOC I patients compared to AASM2007Rec (297% increase) as well as increased the proportion of females in the APOC I group. AASM2012Rec did not change the number of APOC II and APOC III patients. In fact, the same patients were present in these categories irrespective of hypopnoea criteria. The proportion of non-APOC patients proportionally decreased with the AASM2012Rec criteria. There were no differences in outcome measures between the AASM2012Rec and AASM2007Rec groups.
Conclusions
This study demonstrates that, compared to AASM2007Rec, AASM2012Rec increases the prevalence of who could be successfully treated with positional therapy. The proportion of females with pOSA also increases as a consequence of AASM2012Rec.

Similar content being viewed by others
References
Gottlieb DJ, Whitney CW, Bonekat WH et al (1999) Relation of sleepiness to respiratory disturbance index: the sleep heart health study. Am J Respir Crit Care Med 159:502–507. doi:10.1164/ajrccm.159.2.9804051
Lopes C, Esteves AM, Bittencourt LRA et al (2008) Relationship between the quality of life and the severity of obstructive sleep apnea syndrome. Brazilian J Med Biol Res 41:908–913
Olaithe M, Bucks RS (2013) Executive dysfunction in OSA before and after treatment: a meta-analysis. Sleep 36:1297–1305. doi:10.5665/sleep.2950
Young T, Peppard PE, Gottlieb DJ (2002) Epidemiology of obstructive sleep apnea. Am J Respir Crit Care Med 165:1217–1239. doi:10.1164/rccm.2109080
Cartwright RD (1984) Effect of sleep position on sleep apnea severity. Sleep 7:110–114. doi:10.1378/chest.90.3.424
Ong JSL, Touyz G, Tanner S et al (2011) Variability of human upper airway collapsibility during sleep and the influence of body posture and sleep stage. J Sleep Res 20:533–537. doi:10.1111/j.1365-2869.2011.00925.x
Joosten SA, O’Driscoll DM, Berger PJ, Hamilton GS (2014) Supine position related obstructive sleep apnea in adults: pathogenesis and treatment. Sleep Med Rev 18:7–17. doi:10.1016/j.smrv.2013.01.005
Duce B, Kulkas A, Langton C, et al (2016) The AASM 2012 recommended hypopnea criteria increases the incidence of obstructive sleep apnea but not the proportion of positional obstructive sleep apnea. Sleep Med. doi:10.10.16/j.sleep.2016.07.013
Bignold JJ, Mercer JD, Antic NA et al (2011) Accurate position monitoring and improved supine-dependent obstructive sleep apnea with a new position recording and supine avoidance device. J Clin Sleep Med 7:376–383. doi:10.5664/JCSM.1194
de Vries GE, Hoekema A, Doff MH et al (2015) Usage of positional therapy in adults with obstructive sleep apnea. J Clin Sleep Med 11:131–137. doi:10.5664/jcsm.4458
Frank MH, Ravesloot MJL, van Maanen JP et al (2014) Positional OSA part 1: towards a clinical classification system for position-dependent obstructive sleep apnoea. Sleep Breath. doi:10.1007/s11325-014-1022-9
Ravesloot MJL, Frank MH, van Maanen JP et al (2015) Positional OSA part 2: retrospective cohort analysis with a new classification system (APOC). Sleep Breath. doi:10.1007/s11325-015-1206-y
Duce B, Milosavljevic J, Hukins C (2015) The 2012 AASM respiratory event criteria increase the incidence of hypopneas in an adult sleep center population. J Clin Sleep Med 11:1425–1431. doi:10.5664/jcsm.5280
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14:540–545. doi:10.1016/j.sleep.2007.08.004
Weaver TE, Laizner AM, Evans LK et al (1997) An instrument to measure functional status outcomes for disorders of excessive sleepiness. Sleep 20:835–843
Ware JEJ, Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 30:473–483
Mueller ST, Piper BJ (2014) The psychology experiment building language (PEBL) and PEBL test battery. J Neurosci Methods 222:250–259. doi:10.1016/j.jneumeth.2013.10.024
Wilkinson RT, Houghton D (1982) Field test of arousal: a portable reaction timer with data storage. Hum Factors 24:487–493
Urbaniak GC, Plous S (2011) Research Randomizer (Version 3.0). http://www.randomizer.org. Accessed 14 Jan 2016
American Academy of Sleep Medicine (2014) International classification of sleep disorders, 3rd edn. American Academy of Sleep Medicine, Darien
D’Agostino R, Pearson ES (1973) Tests for departure from normality. Empirical results for the distributions of b 2 and √b 1. Biometrika 60:613. doi:10.2307/2335012
Shepertycky MR, Banno K, Kryger MH (2005) Differences between men and women in the clinical presentation of patients diagnosed with obstructive sleep apnea syndrome. Sleep 28:309–314
Ware JC, McBrayer RH, Scott J a (2000) Influence of sex and age on duration and frequency of sleep apnea events. Sleep 23:165–170
Mohsenin V (2001) Gender differences in the expression of sleep-disordered breathing. Chest 120:1442–1447
Turnbull CD, Bratton DJ, Craig SE et al (2016) In patients with minimally symptomatic OSA can baseline characteristics and early patterns of CPAP usage predict those who are likely to be longer-term users of CPAP. J Thorac Dis 8:276–281. doi:10.3978/j.issn.2072-1439.2016.01.54
Smith S (1995) Is the SF 36 sensitive to sleep disruption? A study in subjects with sleep apnoea. J Sleep Res 4:183–188
Bennett LS, Langford BA, Stradling JR, Davies RJ (1998) Sleep fragmentation indices as predictors of daytime sleepiness and nCPAP response in obstructive sleep apnea. Am J Respir Crit Care Med 158:778–786. doi:10.1164/ajrccm.158.3.9711033
Antic NA, Catcheside P, Buchan C et al (2011) The effect of CPAP in normalizing daytime sleepiness, quality of life, and neurocognitive function in patients with moderate to severe OSA. Sleep 34:111–119. doi:10.1016/j.yneu.2011.05.056
Guilleminault C, Hagen CC, Huynh NT (2009) Comparison of hypopnea definitions in lean patients with known obstructive sleep apnea hypopnea syndrome ( OSAHS ). Sleep Breath 13:341–347. doi:10.1007/s11325-009-0253-7
van Kesteren ER, van Maanen JP, Hilgevoord A a J et al (2011) Quantitative effects of trunk and head position on the apnea hypopnea index in obstructive sleep apnea. Sleep 34:1075–1081. doi:10.5665/SLEEP.1164
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Financial support
Antti Kulkas is supported by the Emil Aaltonen and Tampere Tuberculosis Foundations. The sponsors had no role in the design or conduct of this research.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organisation or entity with any financial interest in the subject matter or materials discussed in this manuscript.
Ethical approval
The Institutional Human Research Ethics Committee of the Princess Alexandra Hospital approved this study (HREC/16/QPAH/021). All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study formal consent by the patients was not required.
Rights and permissions
About this article
Cite this article
Duce, B., Kulkas, A., Langton, C. et al. Amsterdam positional OSA classification: the AASM 2012 recommended hypopnoea criteria increases the number of positional therapy candidates. Sleep Breath 21, 411–417 (2017). https://doi.org/10.1007/s11325-016-1432-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-016-1432-y