Abstract
Introduction
The objective was to evaluate the feasibility of sonographic evaluation of functional tongue motion as a tool to evaluate postoperative outcomes in human subjects using breathing-synchronized stimulation of the hypoglossal nerve—a novel therapy option for patients with obstructive sleep apnea (OSA).
Material and methods
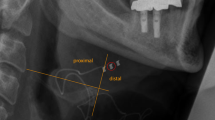
Sixteen patients with OSA (n = 16, age 60.4 ± 10.2, BMI 28.7 ± 2.4, AHI 35.0 ± 11.8) underwent sonographic evaluation of tongue motion after initiation of therapy with the Inspire II Upper Airway Stimulation system. Sonographic examination was performed in four different planes (A = floor of the mouth frontal, B = base of the tongue horizontal, C = floor of the mouth parallel to mandible, and D = floor of the mouth median sagittal) in an attempt to visualize tongue surface, tongue and hyoid motion, and the distance of protrusion.
Results
Identification of the tongue surface was achieved in all cases in planes B, C, and D and 81 % of patients in plane A. Tongue motion was evident on the right (implant) side in 63 % in plane A and 75 % in plane B. Distance of protrusion was measured in plane B at 1.04 cm (±0.51), in plane C at 1.08 cm (±0.47), and in plane D at 0.96 cm (±0.45). Hyoid protrusion was measured in plane C or D and was 0.57 cm (±0.39). Significant correlations among the three planes were observed, but there was no correlation to the reduction of apnea-hypopnea index.
Conclusion
The results indicate feasibility of sonography to identify tongue and hyoid motions during upper airway stimulation. Useful sonographic planes and landmarks, which allow visualization of dynamic effects of upper airway stimulation, could be established. The evaluation of the tongue in a horizontal (B) and in a sagittal plane (D) appears to be superior to the other investigated planes. The approximate tongue protrusion needed to generate a significant reduction of AHI and ODI was 1 cm.





Similar content being viewed by others
References
Pengo MF, Steier J (2015) Emerging technology: electrical stimulation in obstructive sleep apnoea. J Thorac Dis 7:1286–1297
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328:1230–1235
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177:1006–1014
Steier J, Martin A, Harris J, Jarrold I, Pugh D, Williams A (2014) Predicted relative prevalence estimates for obstructive sleep apnoea and the associated healthcare provision across the UK. Thorax 69:390–392
Strollo PJ, Rogers RM (1996) Obstructive sleep apnea. N Engl J Med 334:99–104
Strollo PJ, Soose RJ, Maurer JT, de Vries N, Cornelius J, et al. (2014) Upper-airway stimulation for obstructive sleep apnea. N Engl J Med 370:139–149
Narkiewicz K, Somers VK (1999) Obstructive sleep apnea as a cause of neurogenic hypertension. Curr Hypertens Rep 1:268–273
Martinez D, Klein C, Rahmeier L, da Silva RP, Fiori CZ, et al. (2012) Sleep apnea is a stronger predictor for coronary heart disease than traditional risk factors. Sleep Breath 16:695–701
Palomäki H, Partinen M, Juvela S, Kaste M (1989) Snoring as a risk factor for sleep-related brain infarction. Stroke 20:1311–1315
Bradley TD, Rutherford R, Grossman RF, Lue F, Zamel N, et al. (1985) Role of daytime hypoxemia in the pathogenesis of right heart failure in the obstructive sleep apnea syndrome. Am Rev Respir Dis 131:835–839
Lévy P, Bonsignore MR, Eckel J (2009) Sleep, sleep-disordered breathing and metabolic consequences. Eur Respir J 34:243–260
Punjabi NM, Sorkin JD, Katzel LI, Goldberg AP, Schwartz AR, Smith PL (2002) Sleep-disordered breathing and insulin resistance in middle-aged and overweight men. Am J Respir Crit Care Med 165:677–682
Young T, Palta M, Dempsey J, Peppard PE, Nieto FJ, Hla KM (2009) Burden of sleep apnea: rationale, design, and major findings of the Wisconsin Sleep Cohort study. WMJ 108:246–249
Gottlieb DJ, Yenokyan G, Newman AB, O’Connor GT, Punjabi NM, et al. (2010) Prospective study of obstructive sleep apnea and incident coronary heart disease and heart failure: the sleep heart health study. Circulation 122:352–360
Tregear S, Reston J, Schoelles K, Phillips B (2009) Obstructive sleep apnea and risk of motor vehicle crash: systematic review and meta-analysis. J Clin Sleep Med 5:573–581
Sawyer AM, Gooneratne NS, Marcus CL, Ofer D, Richards KC, Weaver TE (2011) A systematic review of CPAP adherence across age groups: clinical and empiric insights for developing CPAP adherence interventions. Sleep Med Rev 15:343–356
McArdle N, Devereux G, Heidarnejad H, Engleman HM, Mackay TW, Douglas NJ (1999) Long-term use of CPAP therapy for sleep apnea/hypopnea syndrome. Am J Respir Crit Care Med 159:1108–1114
Stuck BA, Leitzbach S, Maurer JT (2012) Effects of continuous positive airway pressure on apnea-hypopnea index in obstructive sleep apnea based on long-term compliance. Sleep Breath 16:467–471
Woodson BT, Gillespie MB, Soose RJ, Maurer JT, de Vries N, et al. (2014) Randomized controlled withdrawal study of upper airway stimulation on OSA: short- and long-term effect. Otolaryngol Head Neck Surg 151:880–887
Caples SM, Rowley JA, Prinsell JR, Pallanch JF, Elamin MB, et al. (2010) Surgical modifications of the upper airway for obstructive sleep apnea in adults: a systematic review and meta-analysis. Sleep 33:1396–1407
Schwartz AR, Bennett ML, Smith PL, De Backer W, Hedner J, et al. (2001) Therapeutic electrical stimulation of the hypoglossal nerve in obstructive sleep apnea. Arch Otolaryngol Head Neck Surg 127:1216–1223
Heiser C, Maurer JT, Steffen A (2015) Functional outcome of tongue motions with selective hypoglossal nerve stimulation in patients with obstructive sleep apnea. Sleep Breath 20:553–560
Van de Heyning PH, Badr MS, Baskin JZ, Cramer Bornemann MA, De Backer WA, et al. (2012) Implanted upper airway stimulation device for obstructive sleep apnea. Laryngoscope 122:1626–1633
Steffen A, Frenzel H, Wollenberg B, König IR (2015) Patient selection for upper airway stimulation: is concentric collapse in sleep endoscopy predictable. Sleep Breath 19:1373–1376
Dotan Y, Golibroda T, Oliven R, Netzer A, Gaitini L, et al. (2011) Parameters affecting pharyngeal response to genioglossus stimulation in sleep apnoea. Eur Respir J 38:338–347
Vanderveken OM, Maurer JT, Hohenhorst W, Hamans E, Lin HS, et al. (2013) Evaluation of drug-induced sleep endoscopy as a patient selection tool for implanted upper airway stimulation for obstructive sleep apnea. J Clin Sleep Med 9:433–438
Kezirian EJ, Hohenhorst W, de Vries N (2011) Drug-induced sleep endoscopy: the VOTE classification. Eur Arch Otorhinolaryngol 268:1233–1236
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14:540–545
Maurer JT, Van de Heyning P, Lin HS, Baskin JZ, Anders C, et al. (2012) Operative technique of upper airway stimulation: an implantable treatment of obstructive sleep apnea. Oper Tech Otolaryngol Head Neck Surg 23:227–233
Goding GS, Tesfayesus W, Kezirian EJ (2012) Hypoglossal nerve stimulation and airway changes under fluoroscopy. Otolaryngol Head Neck Surg 146:1017–1022
Stone M (2005) A guide to analysing tongue motion from ultrasound images. Clin Linguist Phon 19:455–501
Bassiri Gharb B, Tadisina KK, Rampazzo A, Hashem AM, Elbey H, et al. (2015) Microsurgical anatomy of the terminal hypoglossal nerve relevant for neurostimulation in obstructive sleep apnea. Neuromodulation 18:721–728
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of interest
Benedikt Hofauer, Andreas Knopf, Muras Bas, Markus Wirth, and Konrad Stock certify that they have no affiliations with or involvement in any organization or entity with any financial interest, or non-financial interest in the subject matter or materials discussed in this manuscript. Kingman Strohl is the Site Principal Investigator at Case Medical Center for the Star Phase III FDA trial and for the Post-Approval Study for upper airway stimulation (Inspire Medical Systems); no other conflicts to declare. Clemens Heiser is study investigator and consultant of Inspire Medical Systems and received personal fees from Neuwirth Medical Products, Heinen & Loewenstein, Sutter Medizintechnik, outside the submitted work; no other conflicts to declare.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments of comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Hofauer, B., Strohl, K., Knopf, A. et al. Sonographic evaluation of tongue motions during upper airway stimulation for obstructive sleep apnea—a pilot study. Sleep Breath 21, 101–107 (2017). https://doi.org/10.1007/s11325-016-1383-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-016-1383-3