Abstract
Objectives
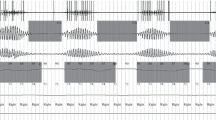
This randomized, controlled trial aimed to investigate whether acute improvement of pulmonary congestion would reduce the severity of Cheyne-Stokes respiration (CSR) in patients with chronic heart failure (CHF).
Methods
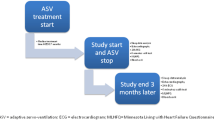
Twenty-one consecutive patients with CHF and CSR (apnea-hypopnea index [AHI] ≥15/h) underwent right heart catheterization with titration of intravenous (IV) glyceryltrinitrate (GTN) to a maximum tolerable dosage and inhalation of iloprost 10 μg/mL after a washout phase. Maximum tolerable dosages of GTN and iloprost were randomly applied during full cardiorespiratory polysomnography within two split-night procedures and compared with IV or inhaled sodium chloride (NaCl) 0.9 %, respectively.
Results
GTN (6.2 ± 1.5 mg/h) and iloprost significantly lowered \mean pulmonary artery pressure (20.1 ± 9.0 to 11.6 ± 4.2 mmHg, p < 0.001 and 16.9 ± 7.9 to 14.2 ± 6.4 mmHg, p < 0.01, respectively). Pulmonary capillary wedge pressure was only reduced by GTN (14.0 ± 5.6 to 7.2 ± 3.9 mmHg, p < 0.001), and there was no significant change in the cardiac index. Sleep studies revealed no significant improvement in markers of CSR severity, including AHI, central apnea index, and CSR cycle length following GTN or iloprost treatment. Significant decreases in blood pressure, mean oxygen saturation, and S3 sleep were documented during GTN infusion.
Conclusions
Acute improvement of pulmonary congestion by GTN had no immediate impact on CSR severity. Future investigations must therefore include longer treatment periods and treatment regimens that have positive, rather than negative, additional effects on peripheral and central chemoreceptors and sleep structure.
Trial registration
German Clinical Trial Registry-ID:DRKS00000467 (www.germanctr.de)


Similar content being viewed by others
References
Oldenburg O (2012) Cheyne-Stokes respiration in chronic heart failure. Circ J 76:2305–2317
Javaheri S (1999) A mechanism of central sleep apnoea in patients with heart failure. N Engl J Med 341:949–954
Solin P, Bergin P, Richardson M et al (1999) Influence of pulmonary capillary wedge pressure on central apnea in heart failure. Circulation 99:1574–1579. doi:10.1161/01.CIR.99.12.1574
Yumino D, Redolfi S, Ruttanaumpawan P et al (2010) Nocturnal rostral fluid shift: a unifying concept for the pathogenesis of obstructive and central sleep apnea in men with heart failure. Circulation 13:1598–1605. doi:10.1161/CIRCULATIONAHA.109.902452
McMurray JJ, Adamopopoulos S, Anker SD et al (2012) ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2012. Eur Heart J 33:1787–1847. doi:10.1093/eurheartj/ehs104
Publication Committeee for the VMAC Investigators, Trial ARC (2002) Intravenous nesiritide vs nitroglycerin for treatment of decompensated. JAMA 287:1531–1540
Braun S, Schrötter H, Schmeisser A, Strasser R (2007) Evaluation of pulmonary vascular response to inhaled iloprost in heart transplant candidates with pulmonary venous hypertension. Int J Cardiol 115:67–72
Olschewski H, Olschewski A, Rose F, Al E (2001) Physiologic basis for the treatment of pulmonary hypertension. J Lab Clin Med 138:287–297
Bradley T, Logan A, Kimoff R et al (2005) Continuous positive airway pressure for central sleep apnea and heart failure. N Engl J Med 353:2025–2033. doi:10.1056/NEJMoa051001
Arzt M, Floras J, Logan A et al (2007) Suppression of central sleep apnea by continuous positive airway pressure and transplant-free survival in heart failure: a post hoc analysis of the Canadian Continuous Positive Airway Pressure for Patients with Central Sleep Apnea and Heart Failure Trial. Circulation 115:3173–3180
Costanzo M, Augostini R, Goldberg L et al (2015) Design of the remedē® system pivotal trial: a prospective, randomized study in the use of respiratory rhythm management to treat central sleep apnea. J Card Fail. doi:10.1016/j.cardfail.2015.08.344
Summerhill EM, Baram M (2005) Principles of pulmonary artery catheterization in the critically ill. Lung 183:209–219. doi:10.1007/s00408-004-2537-9
Berry RB, Budhiraja R, Gottlieb DJ et al (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. J Clin Sleep Med 8:597–619. doi:10.5664/jcsm.2172
Davis JT (1972) The influence of intrathoracic pressure on fluid and electrolyte balance. Chest 62:118S–125S
Lorenzi-Filho G, Azevedo ERE, Parker JJDJ et al (2002) Relationship of PaCO2 to pulmonary wedge pressure in heart failure. Eur Respir J 19:37–40. doi:10.1183/09031936.02.00214502
Oldenburg O, Bitter T, Wiemer M et al (2009) Pulmonary capillary wedge pressure and pulmonary arterial pressure in heart failure patients with sleep-disordered breathing. Sleep Med 10:726–730. doi:10.1016/j.sleep.2008.08.004
Churchill E, Cope O (1929) The rapid shallow breathing resulting from pulmonary congestion and edema. J Exp Med 49:531–537
Pryor W (1951) Cheyne-Stokes respiration in patients with cardiac enlargement and prolonged circulation time. Circulation 14:233–238
Fanfulla F, Mortara A, Maestri R et al (1998) The development of hyperventilation in patients with chronic heart failure and Cheyne-Stokes respiration*—a possible role of chronic hypoxia. Chest 114:1083–1090. doi:10.1378/chest.114.4.1083
Xie A, Skatrud JB, Puleo DS et al (2002) Apnea-hypopnea threshold for CO2 in patients with congestive heart failure. Am J Respir Crit Care Med 165:1245–1250. doi:10.1164/rccm.200110-022OC
Hoeper MM, Pletz MW, Golpon H, Welte T (2007) Prognostic value of blood gas analyses in patients with idiopathic pulmonary arterial hypertension. Eur Respir J 29:944–950. doi:10.1183/09031936.00134506
Schulz R, Baseler G, Ghofrani HA et al (2002) Nocturnal periodic breathing in primary pulmonary hypertension. Eur Respir J 19:658–663. doi:10.1183/09031936.02.00225102
Ulrich S, Fischler M, Speich R, Bloch KE (2008) Sleep-related breathing disorders in patients with pulmonary hypertension. Chest 133:1375–1380. doi:10.1378/chest.07-3035
Dumitrascu R, Tiede H, Eckermann J et al (2013) Sleep apnea in precapillary pulmonary hypertension. Sleep Med 14:247–251. doi:10.1016/j.sleep.2012.11.013
Andreas S, Clemens C, Sandholzer H et al (1996) Improvement of exercise capacity with treatment of Cheyne-Stokes respiration in patients with congestive heart failure. J Am Coll Cardiol 27:1486–1490
Shigemitsu M, Nishio K, Kusuyama T et al (2007) Nocturnal oxygen therapy prevents progress of congestive heart failure with central sleep apnea. Int J Cardiol 115:354–360. doi:10.1016/j.ijcard.2006.03.018
Toyama T, Seki R, Kasama S et al (2009) Effectiveness of nocturnal home oxygen therapy to improve exercise capacity, cardiac function and cardiac sympathetic nerve activity in patients with chronic heart failure and central sleep apnea. Circ J 73:2148–2153
Kee K, Naughton MT (2010) Heart failure and the lung. Circ J 74:2507–2516. doi:10.1253/circj.CJ-10-0869
Tkacova R, Niroumand M, Lorenzi-filho G et al (2001) Overnight shift from obstructive to central apneas in patients with heart failure: role of PCO2 and circulatory delay. Circulation 103:238–243. doi:10.1161/01.CIR.103.2.238
Padeletti M, Green P, Mooney AM et al (2009) Sleep disordered breathing in patients with acutely decompensated heart failure. Sleep Med 10:353–360. doi:10.1016/j.sleep.2008.03.010
Padeletti M, Henriquez A, Mancini DM, Basner RC (2007) Persistence of Cheyne-Stokes breathing after left ventricular assist device implantation in patients with acutely decompensated end-stage heart failure. J Heart Lung Transplant 26:742–744. doi:10.1016/j.healun.2007.04.009
Mansfield D (2003) Raised sympathetic nerve activity in heart failure and central sleep apnea is due to heart failure severity. Circulation 107:1396–1400. doi:10.1161/01.CIR.0000056520.17353.4F
Oldenburg O, Faber L, Vogt J et al (2007) Influence of cardiac resynchronisation therapy on different types of sleep disordered breathing. Eur J Heart Fail 9:820–826
Schäfer T, Schläfke ME (2011) Regulation der Atmung im Schlaf. Somnologie 15:84–91. doi:10.1007/s11818-011-0515-z
Trinder J, Whitworth F, Kay A, Wilkin P (1992) Respiratory instability during sleep onset. J Appl Physiol 73:2462–2469
Horner RL, Rivera MP, Kozar LF, Phillipson EA (2001) The ventilatory response to arousal from sleep is not fully explained by differences in CO2 levels between sleep and wakefulness. J Physiol 534(3):881–890
Pinna GD, Robbi E, Pizza F et al (2014) Sleep-wake fluctuations and respiratory events during Cheyne-Stokes respiration in patients with heart failure. J Sleep Res 23:349–359
Donovan LM, Liu Y, Weiss JW (2014) Effect of endothelin antagonism on apnea frequency following chronic intermittent hypoxia. Respir Physiol Neurobiol 194:6–8. doi:10.1016/j.resp.2014.01.015
Peng Y-J, Nanduri J, Zhang X et al (2012) Endothelin-1 mediates attenuated carotid baroreceptor activity by intermittent hypoxia. J Appl Physiol 112:187–196. doi:10.1152/japplphysiol.00529.2011
Mehta J, Pepine CJ, Conti CR (1978) Haemodynamic effects of hydrallazine and of hydrallazine plus glyceryl trinitrate paste in heart failure. Br Heart J 40:845–850. doi:10.1136/hrt.40.8.845
Acknowledgments
The authors would like to thank Markus Möllenberg, Jelena Dohrmann, Thomas Fischbach, Maryam Afsah, and all the nurses from our sleep laboratory for their enormous efforts spent on the success of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Funding
Bayer Healthcare GmbH and the Ruhr University Bochum provided financial support for the conduction of the study. The sponsor had no role in the design or conduct of this research.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Bitter, T., Fox, H., Schmalgemeier, H. et al. Acute improvement of pulmonary hemodynamics does not alleviate Cheyne-Stokes respiration in chronic heart failure—a randomized, controlled, double-blind, crossover trial. Sleep Breath 20, 795–804 (2016). https://doi.org/10.1007/s11325-015-1300-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-015-1300-1