Abstract
Purpose
Primary non-refluxing megaureter (pMU) is a multifaceted and challenging congenital pathology of the urinary tract. We report our 23-year experience with this anomaly in terms of presentation, diagnostic work-up and management.
Materials and methods
We retrospectively reviewed the medical records of 212 children diagnosed with pMU between 1986 and 2009 at our institution. Mean follow-up was 45.17 (0–192) months.
Results
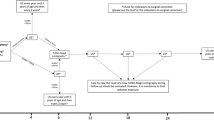
Of the total, 168 (79 %) children presented with upper urinary tract dilation on perinatal ultrasound screening. In 44 (21 %) patients, the diagnosis was made following diagnostic work-up of a urinary tract infection (UTI, 18 %) or flank pain (3 %). In total, 203 of 254 pMUs (79.9 %) were successfully treated conservatively during the 23-year observation period. Forty-eight children (23 %) underwent ureteric reimplantation. UTIs occurred in 91 of 212 children (43 %). Of these, 41 (45 %) occurred despite antibacterial infection prophylaxis. Within the past three decades, there has been a marked shift from surgical toward conservative therapy at our institution.
Conclusion
Neonatal renal ultrasound is the method of choice to timely identify children with pMU and, alongside dynamic renography, to monitor the clinical course. Nowadays, only a minor subset of children with asymptomatic course requires surgical correction. Antibacterial prophylaxis has the potential to reduce the risk of febrile UTIs. Prospective randomized studies are warranted to provide evidence of the beneficial effect of antibacterial prophylaxis.




Similar content being viewed by others
References
Stein R, Rubenwolf P, Ziesel C, Kamal MM, Thüroff JW (2013) Psoas hitch and Boari flap ureteroneocystostomy. BJU Int 112(1):137–155
Stolz G, Schumacher R, Wiesel A, Schlaefer K, Queisser-Luft A (2002) Pre- and postnatal kidney screening compared: an analysis of 34,450 newborn infants of the Mainz model birth register. Radiologe 42(8):630–636
Hanna MK, Jeffs RD (1975) Primary obstructive megaureter in children. Urology 6(4):419–427
Keating MA, Escala J, Snyder HM, Heyman S, Duckett JW (1989). Changing concepts in management of primary obstructive megaureter. J Urol 142(2 Pt 2):636–640; discussion 67-8
Liu HY, Dhillon HK, Yeung CK, Diamond DA, Duffy PG, Ransley PG (1994) Clinical outcome and management of prenatally diagnosed primary megaureters. J Urol 152(2 Pt 2):614–617
Kelalis PP, Kramer SA (1983) Complications of megaureter surgery. Urol Clin North Am 10(3):417–422
Oliveira EA, Diniz JS, Rabelo EA, Silva JM, Pereira AK, Filgueiras MT et al (2000) Primary megaureter detected by prenatal ultrasonography: conservative management and prolonged follow-up. Int Urol Nephrol 32(1):13–18
Pfister RC, Hendren WH (1978) Primary megaureter in children and adults. Clinical and pathophysiologic features of 150 ureters. Urology 12(2):160–176
Shukla AR, Cooper J, Patel RP, Carr MC, Canning DA, Zderic SA et al (2005) Prenatally detected primary megaureter: a role for extended followup. J Urol 173(4):1353–1356
Arena F, Baldari S, Proietto F, Centorrino A, Scalfari G, Romeo G (1998) Conservative treatment in primary neonatal megaureter. Eur J Pediatr Surg 8(6):347–351
Arena S, Magno C, Montalto AS, Russo T, Mami C, Baldari S et al (2012) Long-term follow-up of neonatally diagnosed primary megaureter: rate and predictors of spontaneous resolution. Scand J Urol Nephrol 46(3):201–207
Calisti A, Oriolo L, Perrotta ML, Spagnol L, Fabbri R (2008) The fate of prenatally diagnosed primary nonrefluxing megaureter: do we have reliable predictors for spontaneous resolution? Urology 72(2):309–312
Cozzi F, Madonna L, Maggi E, Piacenti S, Bonanni M, Roggini M et al (1993) Management of primary megaureter in infancy. J Pediatr Surg 28(8):1031–1033
Gimpel C, Masioniene L, Djakovic N, Schenk JP, Haberkorn U, Tönshoff B et al (2010) Complications and long-term outcome of primary obstructive megaureter in childhood. Pediatr Nephrol 25(9):1679–1686
Stehr M, Metzger R, Schuster T, Porn U, Dietz HG (2002) Management of the primary obstructed megaureter (POM) and indication for operative treatment. Eur J Pediatr Surg 12(1):32–37
DiRenzo D, Persico A, DiNicola M, Silvaroli S, Martino G, LelliChiesa P (2015) Conservative management of primary non-refluxing megaureter during the first year of life: a longitudinal observational study. J Pediatr Urol 11(4):226.e1–226.e6
Braga LH, D’Cruz J, Rickard M, Jegatheeswaran K, Lorenzo AJ (2016) The fate of primary nonrefluxing megaureter: a prospective outcome analysis of the rate of urinary tract infections, surgical indications and time to resolution. J Urol 195(4 Pt 2):1300–1305
McLellan DL, Retik AB, Bauer SB, Diamond DA, Atala A, Mandell J et al (2002) Rate and predictors of spontaneous resolution of prenatally diagnosed primary nonrefluxing megaureter. J Urol 168(5):2177–2180; discussion 80
Merlini E, Rotundi F, Seymandi P, Santini L (2002) Primary megaureter detected during the first year of life. Review of case reports in the last 10 years and analysis of prognostic factors. Pediatr Med Chir 24(3):220–222
Tröbs RB, Heinecke K, Elouahidi T, Nounla J, Kluge R (2006) Renal function and urine drainage after conservative or operative treatment of primary (obstructive) megaureter in infants and children. Int Urol Nephrol 38(1):141–147
Chertin B, Pollack A, Koulikov D, Rabinowitz R, Shen O, Hain D et al (2008) Long-term follow up of antenatally diagnosed megaureters. J Pediatr Urol 4(3):188–191
Walsh TJ, Hsieh S, Grady R, Mueller BA (2007) Antenatal hydronephrosis and the risk of pyelonephritis hospitalization during the first year of life. Urology 69(5):970–974
Lee JH, Choi HS, Kim JK, Won HS, Kim KS, Moon DH et al (2008) Nonrefluxing neonatal hydronephrosis and the risk of urinary tract infection. J Urol 179(4):1524–1528
Braga LH, Mijovic H, Farrokhyar F, Pemberton J, DeMaria J, Lorenzo AJ (2013) Antibiotic prophylaxis for urinary tract infections in antenatal hydronephrosis. Pediatrics 131(1):e251–e261
Eskild-Jensen A, Gordon I, Piepsz A, Frøkiaer J (2004) Interpretation of the renogram: problems and pitfalls in hydronephrosis in children. BJU Int 94(6):887–892
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Author A (PR) declares that he has no conflict of interest. Author B (JHN) declares that she has no conflict of interest. Author C (RS) declares that he has no conflict of interest. Author C (RB) declares that he has no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Rubenwolf, P., Herrmann-Nuber, J., Schreckenberger, M. et al. Primary non-refluxive megaureter in children: single-center experience and follow-up of 212 patients. Int Urol Nephrol 48, 1743–1749 (2016). https://doi.org/10.1007/s11255-016-1384-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-016-1384-y