Abstract
Objective
The purpose of this study was to investigate the effects of water exercise at a day service facility and the effects of water exercise frequency on health-related quality of life (HRQL).
Methods
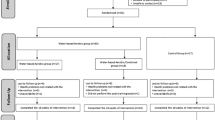
Participants (n = 30) were randomly separated into three groups: two indicating exercise frequency, at once-weekly or twice-weekly, and a control group. One-hour exercise intervention sessions were carried out once or twice a week, accordingly, for 24 weeks. The water exercise session comprised a warm-up on land, activities of daily living (ADL) exercises, stretching, strength training, and relaxation in water. HRQL was evaluated using the Medical Outcomes Survey Short-Form 36 (SF-36) questionnaire, and ADL disability was assessed using the Functional Independence Measure.
Results
Significant differences were found between pre- and 6 months in both the once- and twice-weekly groups in HRQL (p < 0.05). No significant difference was found among pre-, 3 months, and 6 months. The effect size between the once and twice groups was moderate in both the physical component summary (0.72) and mental component summary (0.75) at 3 months. ADL disability shows significant correlation with HRQL.
Conclusion
Water exercise intervention at a day service facility improved participants’ HRQL for 6 months by improving exercise habits and ADL disability. Furthermore, the HRQL change differed according to exercise frequency: twice-weekly exercise showed more rapid improvement than once-weekly.

Similar content being viewed by others
Abbreviations
- HRQL:
-
Health-related quality of life
- ADL:
-
Activities of daily living
- PNCIS:
-
The public nursing-care insurance system
- SF-36:
-
The Medical Outcomes Survey Short form-36
- FIM:
-
Functional Independence Measure
- COPD:
-
Chronic obstructive pulmonary disease
- FM:
-
Fibromyalgia
- PF:
-
Physical functioning
- RP:
-
Role limitations due to physical health
- BP:
-
Bodily pain
- GH:
-
General health
- PCS:
-
Physical component summary
- VT:
-
Vitality
- SF:
-
Social functioning
- RE:
-
Role limitations due to emotional health
- MH:
-
Mental health
- MCS:
-
Mental component summary
- BMI:
-
Body mass index
- RPE:
-
Rating of perceived exertion scale
- SD:
-
Standard deviation
- ES:
-
Effect size
References
Spector, W. D., Katz, S., & Murphy, J. B. (1987). The hierarchical relationship between activities of daily living and instrumental activities of daily living. Journal of Chronic Diseases, 40, 481–489.
Katz, S., Branch, L. G., & Branson, M. H. (1983). Active life expectancy. The New England Journal of Medicine, 309, 1218.
Sato, S., Demura, S., Kobayashi, H., & Nagasawa, Y. (2002). The relationship and its change with aging between ADL and daily life satisfaction characteristics in independent Japanese elderly living at home. Journal of Physiological Anthropology and Applied Human Science, 21(4), 195–204.
Luulinen, H., Lehtola, S., Jokelainen, J., Vaananen-Sainio R., Lotvonen S., & Koistinen P. (2006). Prevention of disability by exercise among the elderly: A population-based, randomized, controlled trial. Scandinavian Journal of Primary Health Care, 24, 199–205.
Health, Labour and Welfare Ministry, http://www.mhlw.go.jp/.
Satake, K., Knazawa, N., Takemura, S., Fujita, K., Yamase, T., & Nishijima, T. (2004). The effect of resistance training in the elderly with nursing care. Hokkaido Journal of Public Health, 18, 34–42.
Ishihara, K., Nishimoto, K., Mimura, T., Tanaka, S., Kurihara, N., & Fujimoto, S. (2001). Effects of a balance training program on balance function in geriatric health services facility residents (vol 16, pp. 18–25). Tokyo: Research Aid Report, Physical Fitness Research Institute: Meiji Yasuda Life Foundation of Health and Welfare.
Gregg, E. W., Pereira, M. A., & Caspersen, C. J. (2000). Physical activity, falls, and fractures among older adults: A review of the epidemiologic evidence. Journal of the American Geriatrics Society, 48, 883–893.
Tinetti, M. E., Speechley, M., & Ginter, S. F. (1988). Risk factors for falls among the elderly. The New England Journal of Medicine, 319, 1800–1806.
Hauer, K., Specht, N., Schuler, M., Bartsch P., & Oster P. (2002). Intensive physical training in geriatric patients after severe falls and hip surgery. Age Ageing, 31, 49–57.
Skelton, D., & Dinan, S. M. (1999). Exercise for falls management: Rationale for an exercise programme aimed at reducing postural instability. Physiotherapy Theory and Practice, 15, 105–120.
Forwood, M. R., & Larsen, J. A. (2000). Exercise recommendations for osteoporosis. A position statement of the Australian and New Zealand Bone Mineral Society. Australian Family Physician, 29, 761–764.
Devereux, K., Robertson, D., & Briffa, N. K. (2005). Effects of a water-based program on women 65 years and over: A randomised controlled trial. Australian Journal of Physiotherapy, 51, 102–108.
Wadell, K., Sundelin, G., Larsen, H. K., & Lundgren, R. (2004). High-intensity physical group training in water-an effective training modality for patients with COPD. Respiratory Medicine, 98, 428–438.
Mannerkorpi, K., Ahimen, M., & Ekdahl, C. (2002). Six- and 24-month follow-up pool exercise therapy and education for patients with fibromyalgia. Scandinavian Journal of Rheumatology, 31, 306–310.
Demura, S., Kobayashi, H., & Kitabayashi, T. (2005). QOL models constructed for the community-dwelling elderly with ikigai (purpose in life) as a composition factor, and the effect of habitual exercise. Journal of Physiological Anthropology and Applied Human Science, 24(5), 525–533.
Acree, L. S., Longfors, J., Fjeldstad, A. S., Fjeldstad, C., Schank, B., Nickel, J. K., et al. (2006). Physical activity is related to quality of life in older adults. Health and Quality of Life Outcomes, 4, 37.
Sato, D., Kaneda, K., Wakabayashi, H., & Nomura, T. (2007). Some effects of water exercise frequency on functional mobility in nursing care elderly. Japanese Journal of Physical Fitness and Sports Medicine, 56, 141–148.
Matsushita, T., & Matsushima, E. (2004). The relationship between QOL and lifestyle in the elderly. Quality of Life Journal, 5(1), 19–28.
Granger, C. V., Hamilton, B. B., & Keith, R. A. (1986). Advance in functional assessment for medical rehabilitation. Topics in Geriatric Rehabilitation, 1, 59–74.
Borg, G. (1970). Perceived exertion as an indicator of somatic stress. Scandinavian Journal of Rehabilitation Medicine, 2, 92–98.
Fukuhara, S., Ikegami, N., Torrance, G. W., Nishimura, S., Drummond, M., & Schubert, F. (2002). The development and use of quality of life measures to evaluate health outcomes in Japan. PharmacoEconomics, 20(2), 17–23.
Fukuhara, S., Bito, S., Hsiao, A., Green, J., & Kurokawa, K. (1998). Translation, adaptation, and validation of the SF-36 Health Survey for use in Japan. Journal of Clinical Epidemiology, 51(11), 1037–1044.
Fukuhara, S., Ware, J. E., Kosinski, M., Wada, S., & Gandek, B. (1998). Psychometric and clinical tests of validity of the Japanese SF-36 Health Survey. Journal of Clinical Epidemiology, 51(11), 1045–1053.
Jenkinson, C., Wright, L., & Coulter, A. (1994). Criterion validity and reliability of the SF-36 in a population sample. Quality of Life Research, 3, 7–12.
Pollak, N., Rheault, W., & Stoecker, L. (1996). Reliability and validity of the FIM for person aged 80 years and above from a multilevel continuing care retirement community. Archives of Physical Medicine and Rehabilitation, 77, 1056–1061.
Stineman, M. G., Jette, A., & Tassoni, C. J. (1996). The Functional Independence Measure: Test of scaling assumptions, structure, and reliability across 20 diverse impairment categories. Archives of Physical Medicine and Rehabilitation, 77, 1101–1108.
Onodera, K., & Miyashita, M. (1976). A study on Japanese scale for rating of perceived exertion in endurance exercise. Japanese Journal of Physical Education, 21(4), 191–203.
Mihevic, P. M. (1981). Sensory cues for perceived exertion: A review. Medicine and Science in Sports and Exercise, 13, 150–163.
Cohen, J. (1988). Statistical power analysis for the behavioral science (2nd ed.). Mahwah: Lawrence Erlbaum.
Suomi, R., & Collier, D. (2003). Effects of arthritis exercise programs on functional fitness and perceived activities of daily living measures in older adults with arthritis. Archives of Physical Medicine and Rehabilitation, 84, 1589–1594.
Foley, A., Halbert, J., Hewitt, T., & Crotty, M. (2003). Does hydrotherapy improve strength and physical function in patients with osteoarthritis—A randomized controlled trial comparing a gym based and a hydrotherapy based strengthening programme. Annals of the Rheumatic Diseases, 62, 1162–1167.
Littbrand, H., Rosendahl, E., & Lindelof, N. (2006). A high-intensity weight-bearing exercise program for older people dependent in activities of daily living and living in residential care facilities: Evaluation of the applicability with focus on cognitive function. Physical Therapy, 86(4), 489–498.
Chin, A., Poppel, M., Twisk, J., & Mechelan, W. (2006). Once a week not sufficient, twice a week not feasible? A randomized controlled exercise trial in long-term care facilities [ISRCTN87177281]. Patient Education and Counseling, 63, 205–214.
Alexander, B., Gross, M., Medell, L., & Hofmeyer, R. M. (2001). Effects of functional ability and training on chair-rise biomechanics in older adults. The Journals of Gerontology. Series A, Biological Sciences and Medical Sciences, 56(9), 538–547.
Ide, H., Hirao, T., & Hashimoto, M. (2001). Health-related quality of life in human community. Journal of Health and Welfare Statistics, 48, 6–11.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sato, D., Kaneda, K., Wakabayashi, H. et al. The water exercise improves health-related quality of life of frail elderly people at day service facility. Qual Life Res 16, 1577–1585 (2007). https://doi.org/10.1007/s11136-007-9269-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-007-9269-2