Abstract
Purpose
Pituitary dysfunction is reported to be a common complication following aneurysmal subarachnoid hemorrhage (aSAH). The aim of this meta-analysis is to analyze the literature on clinical prevalence, risk factors and outcome impact of pituitary dysfunction after aSAH, and to assess the possible need for pituitary screening in aSAH patients.
Methods
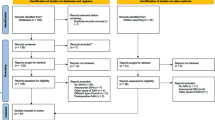
We performed a systematic review with meta-analysis based on a comprehensive search of four databases (PubMed/MEDLINE, ISI/Web of Science, Scopus and Google Scholar).
Results
A total of 20 papers met criteria for inclusion. The prevalence of pituitary dysfunction in the acute phase (within the first 6 months after aSAH) was 49.30 % (95 % CI 41.6–56.9), decreasing in the chronic phase (after 6 months from aSAH) to 25.6 % (95 % CI 18.0–35.1). Abnormalities in basal hormonal levels were more frequent when compared to induction tests, and the prevalence of a single pituitary hormone dysregulation was more frequent than multiple pituitary hormone dysregulation. Increasing age was associated with a lower prevalence of endocrine dysfunction in the acute phase, and surgical treatment of the aneurysm (clipping) was related to a higher prevalence of single hormone dysfunction. The prevalence of pituitary dysfunction did not correlate with the outcome of the patient.
Conclusions
Neuroendocrine dysfunction is common after aSAH, but these abnormalities have not been shown to consistently impact outcome in the data available. There is a need for well-designed prospective studies to more precisely assess the incidence, clinical course, and outcome impact of pituitary dysfunction after aSAH.
Similar content being viewed by others
References
van Gijn J, Kerr RS, Rinkel GJ (2007) Subarachnoid haemorrhage. Lancet 369(9558):306–318
Bederson JB, Connolly ES Jr, Batjer HH, Dacey RG, Dion JE, Diringer MN et al (2009) Guidelines for the management of aneurysmal subarachnoid hemorrhage: a statement for healthcare professionals from a special writing group of the Stroke Council, American Heart Association. Stroke 40(3):994–1025
Guha D, Ibrahim GM, Kertzer JD, Macdonald RL (2014) National socioeconomic indicators are associated with outcomes after aneurysmal subarachnoid hemorrhage: a hierarchical mixed-effects analysis. J Neurosurg 121(5):1039–1047
Boerboom W, Heijenbrok-Kal MH, Khajeh L, van Kooten F, Ribbers GM (2015) Long-term functioning of patients with aneurysmal subarachnoid hemorrhage: a 4-yr follow-up study. Am J Phys Med Rehabil 95(10):e10. doi:10.1016/j.apmr.2014.07.387
von Vogelsang AC, Forsberg C, Svensson M, Wengstrom Y (2015) Patients experience high levels of anxiety 2 years following aneurysmal subarachnoid hemorrhage. World Neurosurg 83(6):1090–1097
Springer MV, Schmidt JM, Wartenberg KE, Frontera JA, Badjatia N, Mayer SA (2009) Predictors of global cognitive impairment 1 year after subarachnoid hemorrhage. Neurosurgery 65(6):1043–1050 (discussion 50–51)
Visser-Meily JM, Rinkel GJ, Vergouwen MD, Passier PE, van Zandvoort MJ, Post MW (2013) Post-traumatic stress disorder in patients 3 years after aneurysmal subarachnoid haemorrhage. Cerebrovasc Dis 36(2):126–130
Suarez JI, Tarr RW, Selman WR (2006) Aneurysmal subarachnoid hemorrhage. N Engl J Med 354(4):387–396
Tanriverdi F, Dagli AT, Karaca Z, Unluhizarci K, Selcuklu A, Casanueva FF et al (2007) High risk of pituitary dysfunction due to aneurysmal subarachnoid haemorrhage: a prospective investigation of anterior pituitary function in the acute phase and 12 months after the event. Clin Endocrinol 67(6):931–937
Bendel S, Koivisto T, Ruokonen E, Rinne J, Romppanen J, Vauhkonen I et al (2008) Pituitary–adrenal function in patients with acute subarachnoid haemorrhage: a prospective cohort study. Crit Care 12(5):R126
Klose M, Brennum J, Poulsgaard L, Kosteljanetz M, Wagner A, Feldt-Rasmussen U (2010) Hypopituitarism is uncommon after aneurysmal subarachnoid haemorrhage. Clin Endocrinol 73(1):95–101
Dimopoulou I, Kouyialis AT, Tzanella M, Armaganidis A, Thalassinos N, Sakas DE et al (2004) High incidence of neuroendocrine dysfunction in long-term survivors of aneurysmal subarachnoid hemorrhage. Stroke 35(12):2884–2889
Lanterna LA, Spreafico V, Gritti P, Prodam F, Signorelli A, Biroli F et al (2013) Hypocortisolism in noncomatose patients during the acute phase of subarachnoid hemorrhage. J Stroke Cerebrovasc Dis 22(7):e189–e196
Jovanovic V, Pekic S, Stojanovic M, Tasic G, Djurovic B, Soldatovic I et al (2010) Neuroendocrine dysfunction in patients recovering from subarachnoid hemorrhage. Hormones 9(3):235–244
Pereira JL, Albuquerque LA, Dellaretti M, Carvalho GT, Vieira G Jr, Brochado VM et al (2013) Pituitary deficiency after aneurysmal subarachnoid hemorrhage. Clinics 68(6):745–749
Aimaretti G, Ambrosio MR, Di Somma C, Gasperi M, Cannavo S, Scaroni C et al (2005) Residual pituitary function after brain injury-induced hypopituitarism: a prospective 12-month study. J Clin Endocrinol Metab 90(11):6085–6092
Kopczak A, Kilimann I, von Rosen F, Krewer C, Schneider HJ, Stalla GK et al (2014) Screening for hypopituitarism in 509 patients with traumatic brain injury or subarachnoid hemorrhage. J Neurotrauma 31(1):99–107
Kronvall E, Valdemarsson S, Saveland H, Nilsson OG (2015) High prevalence of pituitary dysfunction after aneurysmal subarachnoid hemorrhage: a long-term prospective study using dynamic endocrine testing. World Neurosurg 83(4):574–582
Lammert A, Bode H, Hammes HP, Birck R, Fatar M, Zohsel K et al (2011) Neuro-endocrine and neuropsychological outcome after aneurysmal subarachnoid hemorrhage (aSAH): a prospective cohort study. Exp Clin Endocrinol Diabetes 119(2):111–116
Hannon MJ, Behan LA, O’Brien MM, Tormey W, Javadpour M, Sherlock M et al (2015) Chronic hypopituitarism is uncommon in survivors of aneurysmal subarachnoid haemorrhage. Clin Endocrinol 82(1):115–121
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Begg CB, Mazumdar M (1994) Operating characteristics of a rank correlation test for publication bias. Biometrics 50(4):1088–1101
Lammert A, Bode H, Hammes HP, Birck R, Fatar M, Zohsel K et al (2012) Aneurysmal subarachnoid hemorrhage (aSAH) results in low prevalence of neuro-endocrine dysfunction and NOT deficiency. Pituitary 15(4):505–512
Karaca Z, Tanriverdi F, Dagli AT, Selcuklu A, Casanueva FF, Unluhizarci K et al (2013) Three years prospective investigation of pituitary functions following subarachnoid haemorrhage. Pituitary 16(1):76–82
Blijdorp K, Khajeh L, Ribbers GM, Sneekes EM, Heijenbrok-Kal MH, van den Berg-Emons HJ et al (2013) Diagnostic value of a ghrelin test for the diagnosis of GH deficiency after subarachnoid hemorrhage. Eur J Endocrinol 169(4):497–502
Schneider HJ, Schneider M, Kreitschmann-Andermahr I, Tuschy U, Wallaschofski H, Fleck S et al (2011) Structured assessment of hypopituitarism after traumatic brain injury and aneurysmal subarachnoid hemorrhage in 1242 patients: the German interdisciplinary database. J Neurotrauma 28(9):1693–1698
Poll EM, Bostrom A, Burgel U, Reinges MH, Hans FJ, Gilsbach JM et al (2010) Cortisol dynamics in the acute phase of aneurysmal subarachnoid hemorrhage: associations with disease severity and outcome. J Neurotrauma 27(1):189–195
Kassell NF, Torner JC, Haley EC Jr, Jane JA, Adams HP, Kongable GL (1990) The international cooperative study on the timing of aneurysm surgery. Part 1: overall management results. J Neurosurg 73(1):18–36
Hijdra A, van Gijn J, Nagelkerke NJ, Vermeulen M, van Crevel H (1988) Prediction of delayed cerebral ischemia, rebleeding, and outcome after aneurysmal subarachnoid hemorrhage. Stroke 19(10):1250–1256
Hutter BO, Gilsbach JM, Kreitschmann I (1995) Quality of life and cognitive deficits after subarachnoid haemorrhage. Br J Neurosurg 9(4):465–475
Hutter BO, Kreitschmann-Andermahr I, Gilsbach JM (1998) Cognitive deficits in the acute stage after subarachnoid hemorrhage. Neurosurgery 43(5):1054–1065
Powell J, Kitchen N, Heslin J, Greenwood R (2004) Psychosocial outcomes at 18 months after good neurological recovery from aneurysmal subarachnoid haemorrhage. J Neurol Neurosurg Psychiatry 75(8):1119–1124
Ljunggren B, Sonesson B, Saveland H, Brandt L (1985) Cognitive impairment and adjustment in patients without neurological deficits after aneurysmal SAH and early operation. J Neurosurg 62(5):673–679
Powell J, Kitchen N, Heslin J, Greenwood R (2002) Psychosocial outcomes at three and nine months after good neurological recovery from aneurysmal subarachnoid haemorrhage: predictors and prognosis. J Neurol Neurosurg Psychiatry 72(6):772–781
Crompton MR (1963) Hypothalamic lesions following the rupture of cerebral berry aneurysms. Brain 86:301–314
Schneider HJ, Kreitschmann-Andermahr I, Ghigo E, Stalla GK, Agha A (2007) Hypothalamopituitary dysfunction following traumatic brain injury and aneurysmal subarachnoid hemorrhage: a systematic review. JAMA 298(12):1429–1438
Charles MS, Ostrowski RP, Manaenko A, Duris K, Zhang JH, Tang J (2012) Role of the pituitary–adrenal axis in granulocyte-colony stimulating factor-induced neuroprotection against hypoxia–ischemia in neonatal rats. Neurobiol Dis 47(1):29–37
Aimaretti G, Ambrosio MR, Di Somma C, Fusco A, Cannavo S, Gasperi M et al (2004) Traumatic brain injury and subarachnoid haemorrhage are conditions at high risk for hypopituitarism: screening study at 3 months after the brain injury. Clin Endocrinol 61(3):320–326
Rybnikova E, Mironova V, Pivina S, Tulkova E, Ordyan N, Nalivaeva N et al (2007) Involvement of the hypothalamic–pituitary–adrenal axis in the antidepressant-like effects of mild hypoxic preconditioning in rats. Psychoneuroendocrinology 32(7):813–823
Schilling T, Strang CM, Wilhelm L, Moritz KU, Siegmund W, Grundling M et al (2001) Endocrine effects of dopexamine vs. dopamine in high-risk surgical patients. Intensive Care Med 27(12):1908–1915
Lu X, Yu RM, Murphy MB, Lau K, Wu RS (2014) Hypoxia disrupts gene modulation along the brain–pituitary–gonad (BPG)-liver axis. Ecotoxicol Environ Saf 102:70–78
Can A, Gross BA, Smith TR, Dammers R, Dirven C, Woodmansee WW, et al (2015) Pituitary dysfunction after aneurysmal subarachnoid hemorrhage: a systematic review and meta-analysis. Neurosurgery
Khursheed N, Ramzan A, Shoaib Y, Bashir I, Wani A, Shafiq A (2013) Is hypothyroidism and hypogonadism an issue after aneurysmal subarachnoid hemorrhage—an institutional experience? Int J Endocrinol Metab 11(3):179–183
Kreitschmann-Andermahr I, Hartmann Y, Poll E, Schneider HJ, Buchfelder M, Stalla GK (2011) The German database on hypopituitarism after traumatic brain injury and aneurysmal subarachnoid hemorrhage—description, objectives and design. Exp Clin Endocrinol Diabetes 119(1):15–20
Tölli A, Borg J, Bellander B-M, Höybye C (2015) Pituitary function in the acute phase of traumatic brain injury and subarachnoid hemorrhage. Int J Clin Med 6:411–422
Brandt L, Saveland H, Valdemarsson S, Sjoholm H, Reinstrup P (2004) Fatigue after aneurysmal subarachnoid hemorrhage evaluated by pituitary function and 3D-CBF. Acta Neurol Scand 109(2):91–96
Tanriverdi F, Ulutabanca H, Unluhizarci K, Selcuklu A, Casanueva FF, Kelestimur F (2008) Three years prospective investigation of anterior pituitary function after traumatic brain injury: a pilot study. Clin Endocrinol 68(4):573–579
Kreitschmann-Andermahr I, Hoff C, Saller B, Niggemeier S, Pruemper S, Hutter BO et al (2004) Prevalence of pituitary deficiency in patients after aneurysmal subarachnoid hemorrhage. J Clin Endocrinol Metab 89(10):4986–4992
Khajeh L, Blijdorp K, Heijenbrok-Kal MH, Sneekes EM, van den Berg-Emons HJ, van der Lely AJ et al (2015) Pituitary dysfunction after aneurysmal subarachnoid haemorrhage: course and clinical predictors—the HIPS study. J Neurol Neurosurg Psychiatry 86(8):905–910
Khajeh L, Blijdorp K, Neggers SJ, Ribbers GM, Dippel DW, van Kooten F (2014) Hypopituitarism after subarachnoid haemorrhage, do we know enough? BMC Neurol 14:205
Osterman PO (1975) Hypothalamo–pituitary–adrenal function following subarachnoid hemorrhage. Acta Neurol Scand 52(1):56–62
Jenkins JS, Buckell M, Carter AB, Westlake S (1969) Hypothalamic–pituitary–adrenal function after subarachnoid haemorrhage. Br Med J 4(5685):707–709
Kelly DF, Gonzalo IT, Cohan P, Berman N, Swerdloff R, Wang C (2000) Hypopituitarism following traumatic brain injury and aneurysmal subarachnoid hemorrhage: a preliminary report. J Neurosurg 93(5):743–752
Savaridas T, Andrews PJ, Harris B (2004) Cortisol dynamics following acute severe brain injury. Intensive Care Med 30(7):1479–1483
Srinivasan L, Roberts B, Bushnik T, Englander J, Spain DA, Steinberg GK et al (2009) The impact of hypopituitarism on function and performance in subjects with recent history of traumatic brain injury and aneurysmal subarachnoid haemorrhage. Brain Injury 23(7):639–648
Weant KA, Sasaki-Adams D, Dziedzic K, Ewend M (2008) Acute relative adrenal insufficiency after aneurysmal subarachnoid hemorrhage. Neurosurgery 63(4):645–649 (discussion 9–50)
Fleck SK, Wallaschofski H, Rosenstengel C, Matthes M, Kohlmann T, Nauck M et al (2013) Prevalence of hypopituitarism after intracranial operations not directly associated with the pituitary gland. BMC Endocr Disorders 13:51
Zetterling M, Engstrom BE, Arnardottir S, Ronne-Engstrom E (2013) Somatotropic and thyroid hormones in the acute phase of subarachnoid haemorrhage. Acta Neurochir (Wien) 155(11):2053–2062
Parenti G, Cecchi PC, Ragghianti B, Schwarz A, Ammannati F, Mennonna P et al (2011) Evaluation of the anterior pituitary function in the acute phase after spontaneous subarachnoid hemorrhage. J Endocrinol Invest 34(5):361–365
Dutta P, Mukherjee KK, Chaudhary PK, Masoodi SR, Anand S, Pathak A et al (2012) Pituitary dysfunction in survivors of spontaneous subarachnoid hemorrhage of anterior communicating artery and middle cerebral artery aneurysms: a comparative study. Neurol India 60(4):390–394
Acknowledgments
The authors would like to thank Dr. Fabio Gallo from the University of Genoa, Italy for the fundamental help in the meta-analysis.
Author contributions
Dr. Robba contributed to the concept and design of the manuscript, to data acquisition and interpretation of data and writing of the manuscript. Dr. Bacigaluppi contributed to concept and design of the manuscript, data acquisition and interpretation, and critical revision of the paper. Dr. Bragazzi contributed to the concept and design of the manuscript, data revision and analysis and critical revision of the paper. Dr Lavinio and Dr Bilotta revised the article critically for important intellectual content. Dr David Menon and Mark Gurnell contributed to the concept and design and writing of the manuscript and supervised the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Susanna Bacigaluppi and Nicola Bragazzi have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Robba, C., Bacigaluppi, S., Bragazzi, N. et al. Clinical prevalence and outcome impact of pituitary dysfunction after aneurysmal subarachnoid hemorrhage: a systematic review with meta-analysis. Pituitary 19, 522–535 (2016). https://doi.org/10.1007/s11102-016-0733-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-016-0733-2