Abstract
Purpose
Adjuvants are required to ensure the efficacy of subunit vaccines. Incorporating molecular immunopotentiators within particles could overcome drawbacks of molecular adjuvants (such as solubility and toxicity), and improve adjuvanticity of particles, achieving stronger adjuvant activity. Aim of this study is to evaluate the adjuvanticity of immunopotentiator-loaded polymeric particles for subunit vaccine.
Methods
PLGA microparticles (PMPs) and imiquimod (TLR-7 ligand)-loaded PLGA microparticles (IPMPs) were prepared by SPG premix membrane emulsification. In vitro and in vivo studies were performed to their adjuvant activity, using ovalbumin and H5N1 influenza split vaccine as antigens.
Results
Incorporating imiquimod into microparticles significantly improved the efficacy of PLGA microparticles in activating BMDCs and pMΦs, and antigen uptake by pMΦs was also promoted. IPMPs showed stronger adjuvanticity to augment OVA-specific immune responses than PMPs. IgG subclass profiles and cytokine secretion levels by splenocytes indicated that IPMPs elicited more Th1-polarized immune response, compared to PMPs. In vivo study using H5N1 influenza split vaccine as antigen also confirmed the effects of IPMPs on antigen-specific cellular immunity.
Conclusions
Considering adjuvanticity and safety profiles (PLGA and IMQ, both approved by FDA), we conclude that IMQ-loaded PLGA microparticles are promising robust adjuvant for subunit vaccines.
Similar content being viewed by others
Introduction
Vaccination, one of the most significant achievements in medicine, is considered as the most effective and cost-efficient strategy in preventing and controlling infectious diseases [1–3]. However, several problems exist in vaccine development. Exploration of ideal vaccines always suffers from safety concerns and/or inadequate immunogenicity. Traditional whole-pathogen vaccines based on attenuated or inactivated pathogens, the majority of vaccines used nowdays, usually induce potent immune responses and provide sufficient protection against infections, owing to endogenous adjuvants in pathogens. Nevertheless, the side effects and safety concerns limit the extent to which whole-pathogen vaccines can be used [4–6]. Subunit vaccines based on subunit of pathogens, recombinant proteins, peptides, and polysaccharides, are usually better tolerated and regarded as safer alternatives to traditional whole-pathogen vaccines [7]. The drawback of subunit vaccines is poorly immunogenicity. When used alone, subunit vaccines usually fail to elicit sufficient protective immune responses. Therefore, exogenous adjuvants are required to augment the efficacy of subunit vaccines [6, 8].
Adjuvants can be classified into two major categories: particle-based antigen delivery systems (e.g. polymeric micro/nanoparticles, liposomes, emulsions) that deliver antigen into antigen-presenting cells (APCs) and improve/regulate antigen presentation by APCs; and molecular immunopotentiators (e.g. ligands for Toll-like receptors (TLRs) and NOD-like receptors (NLRs), cytokines, α-GalCer) that activate innate immune response by targeting receptors (e.g. pattern recognition receptors) on innate immune cells [1, 8–10]. Particles-based adjuvants act by combined mechanisms, such as having comparable size to pathogens which facilitates recognition and phagocytosis by APCs, activating NALP3 inflammasome of APCs, and regulating the pathway of antigen presentation [11, 12]. Particles antigen delivery systems could also induce cellular immune responses. Although particles show excellent adjuvant activity, their efficacy can be further improved by incorporating molecular adjuvants within particles. Molecular adjuvants are effective in inducing protective immunity. Among these molecular immunopotentiators, agonists for TLRs are widely investigated and show excellent adjuvant activity. Imiquimod (IMQ), agonist for TLR-7, is a FDA-approved immunomodulatory small-molecule compound in the imidazoquinoline family [13, 14]. IMQ has already been approved for topical treatment in humans [15]. IMQ binds TLR-7 which is expressed within endosomal compartments of macrophages and dendritic cells, activates MyD88 signaling cascade, and ultimately induces secretion of inflammatory cytokines IL-1β, IL-6, TNF-α, and IFN-α [14]. One problem for molecular adjuvants is that high adjuvant doses are required, because of adjuvant solubility, uptake efficiency by APCs, and so on.
We hypothesized that encapsulating molecular immunopotentiators with particles adjuvants could overcome the drawback of molecular immunopotentiators, and improve adjuvant activity of particles, achieving better efficacy in accelerating vaccine-induced immune response. In this study, we chose FDA-approved biodegradable polymer poly(lactic-co-glycolic acid) (PLGA) and immunopotentiator IMQ, and fabricated IMQ-loaded PLGA microparticles by O/W emulsion-solvent evaporation method combined with premix membrane emulsification technique. We hypothesized that PLGA microparticles could improve IMQ internalization by APCs and subsequent APCs activation. At the same time, activated APCs might phagocytize more particles and antigen, inducing effective antigen presentation and subsequent antigen-specific immune response. To verify our hypothesis, in vitro and in vivo experiments were performed to evaluate the adjuvant effect of IMQ-loaded PLGA microparticles, using model antigen ovalbumin (OVA) and H5N1 influenza split vaccine as antigen.
Materials and Methods
Mice, Reagents, and Materials
Mice used in this study were purchased from Vital River Laboratories (Beijing, China). All animal experiments were performed in accordance with the Guide for the Care and Use of Laboratory Animals, and were approved by the Experimental Animal Ethics Committee in Beijing. PLGA (75/25, Mw ≈ 13 kDa) was purchased from Lakeshore Biomaterials (Birmingham, AL, USA). Poly(vinyl alcohol) (PVA-217, degree of polymerization 1700, degree of hydrolysis 88.5%) was ordered from Kuraray (Tokyo, Japan). Imiquimod (IMQ) was ordered from Enzo Life Sciences (Farmingdale, New York, USA). Ovalbumin (OVA) was supplied by Sigma-Aldrich (St. Louis, MO, USA). Influenza virus split vaccine (A/Anhui/1/2005(H5N1)) and alum adjuvant (aluminum hydroxide gels) were kindly provided by Hualan Vaccine Inc. (Henan, China). Peptides (OVA257–264 and OVA323–339) were synthesized by GL Biochem (Shanghai, China). Hemagglutinin (HA, A/Anhui/1/2005(H5N1)) was ordered from Sino Biological Inc. (Beijing, China). Premix membrane emulsification equipment (FMEM-500 M) was provided by the National Engineering Research Center for Biotechnology (Beijing, China). Shirasu porous glass (SPG) membrane was provided by SPG Technology Co. Ltd. (Sadowara, Japan). The medium for splenocytes culture was RPMI 1640 (Gibco, Carlsbad, CA, USA) with 10% (v/v) fetal bovine serum (Gibco, Carlsbad, CA, USA). All mouse cytokine ELISA kits and fluorochrome-conjugated anti-mouse antibodies for flow cytometric use, were obtained from eBioscience (San Diego, CA, USA), unless otherwise indicated. ELISpotPLUS kits were obtained from Mabtech AB (Nacka Strand, Sweden). All other reagents were of analytical grade.
Preparation and Characterization of PLGA Microparticles and Vaccine Formulations
PLGA microparticles were prepared using a two-step procedure by combining the solvent evaporation method and the premix membrane emulsification technique, as described before with some modifications (Fig. 1a) [12]. Briefly, 650 mg PLGA dissolved in 13 mL dichloromethane was added into 65 mL PVA solution (1.5%, m/v) and magnetically stirred at 450 rpm for 90 s to form coarse emulsion. (To prepare IMQ-loaded PLGA microparticles, 20 mg IMQ and 650 mg PLGA were co-dissolved in 13 mL dichloromethane.) Nearly uniform-sized droplets were obtained by extruding the coarse emulsion through SPG membrane (pore size, 2.8 μm) for four times. Inactive and cheap nitrogen was employed to form pressure to drive emulsion through microporous SPG membrane. . Solidification of emulsion droplets into microparticles was achieved by magnetically stirring the emulsion overnight to evaporate the organic solvent dichloromethane. Then, PLGA microparticles were collected by centrifugation (5000 × g, 5 min), and further washed with deionized water for three times to remove the residual PVA and free IMQ. Finally, PLGA microparticles were lyophilized and stored at room temperature.
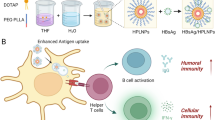
(a) Schematic illustration of preparation of PLGA microparticles by the O/W emulsion–solvent evaporation method combined with the premix membrane emulsification technique. (b) Schematic illustration of vaccine formulation adjuvanted by IMQ-loaded PLGA microparticles. (c) Size distribution and zeta potential of different microparticles. (d) Scanning electron micrographs of different microparticles. The scale bar in (d) represents 1 μm.
The hydrodynamic size and zeta potential of microparticles were measured by a Nano-ZS Zeta Sizer (Malvern Instruments Ltd., Malvern, UK). Microparticles morphology was characterized by scanning electron microscopy (JEM-6700 F, JEOL Ltd., Tokyo, Japan). Nano Measurer 1.2 software was employed to measure the size of microparticles according to the scanning electron micrographs.
The imiquimod content within microparticles was determined by high performance liquid chromatography, according to previously described method [16, 17]. Briefly, 5 mg microparticles were dissolved in 300 μL acetonitrile, and then 700 μL 0.1 M HCl was added. The mixture was filtered and then injected into a reverse-phase HPLC system (HPLC, LC-20AT, Shimadzu) to determine the concentration of imiquimod. Sample injection volume was 40 μL. The detection was carried out at 40°C using a Hypersil GOLD C18 chromatographic column (250 × 4.6 mm, 5 μm, Thermo). The mobile phase was a mixture of 10 mM PBS (phosphate buffered saline) containing 0.1% triethylamine (pH 2.45) and acetonitrile in the ratio of 7:3 (v/v). The flow rate was kept 1.4 mL/min, and the UV detection wavelength was set at 245 nm.
Vaccine formulations were prepared by incubating microparticles (or alum adjuvant) within antigen solution for 4 h at 25°C in a vertical mixer (Table S1, S2). 10 μM PBS was used as buffer solution. The obtained vaccine formulations was conserved at 4°C for subsequent animals immunization. Micro BCA kit was utilized to measure the antigen adsorption level onto adjuvants. The mixture was centrifuged (5000 × g, 5 min), and antigen concentration in the supernatant was detected. Antigen adsorption efficiency (AE) was calculated according to the following formula: AE (%) = (total antigen-antigen in supernatant)/total antigen ×100%.
In Vitro Assays-Antigen Uptake by APCs and APCs Activation
Bone marrow-derived dendritic cells (BMDCs) were isolated from the femurs and tibia of C57BL/6 mice (male, 4–6 weeks) and cultured in vitro in the presence of 10 ng/mL murine granulocyte macrophage colony-stimulating factor (GM-CSF) (Hangzhou Clongene Biotech, China) and 50 ng/mL murine interleukin-4 (IL-4) (PeproTech, USA) [18]. Peritoneal macrophages (pMΦs) were harvested from pre-stimulated C57BL/6 mice (female, 6–8 weeks), according to a previously described protocol [19]. To detect antigen uptake, different vaccine formulations (Alexa Fluor 488-labelled OVA, 5 μg/mL; microparticles, 100 μg/mL) were incubated with pMΦs in 24-well plates. At the indicated time points, cells were collected and stained with anti-mouse CD11b antibody (eBiosciences). Flow cytometer (BD Calibur) was used to detect the percentage of antigen-positive pMΦs. To evaluate APCs activation, BMDCs or pMΦs were cultured in 24-well plates, and incubated with OVA (5 μg/mL) and microparticles (100 μg/mL), or OVA (5 μg/mL) alone, for 24 h. Then, cells were harvested and the supernatant was collected. Concentrations of cytokines (IL-1β, IL-6, TNF-α) in the supernatant were determined by ELISA kits.
Immunization Studies
For OVA model antigen, 32 female C57BL/6 mice (6–8 weeks) were randomly divided into four groups (n = 8) and intramuscularly immunized with 100 μL (50 μL/hind leg) of different vaccine formulations containing 25 μg of antigen (OVA). Mice were immunized three times at 2-week intervals (Fig. S1). Blood samples were collected from the caudal vein before each immunization and 10 days after the third immunization. Sera was separated and stored at −70°C for later analysis. At 10 days after the third immunization, splenocytes were collected for in vitro proliferation, cytokine response, and flow cytometric assays.
For H5N1 influenza split vaccine, 25 female Balb/c mice (5–6 weeks) were randomly divided into five groups (n = 5) and intramuscularly immunized with 100 μL (50 μL/hind leg) of different vaccine formulations containing 3 μg of HA. Mice were immunized twice at a 2-week interval (Fig. S1). Blood samples were collected from the caudal vein before each immunization and 14 days after the second immunization. Sera was separated and stored at −70°C for later antibody detection. At 14 days after the second immunization, splenocytes were collected for in vitro cytokine response assay.
Determination of Antigen-Specific IgG and IgG Subclasses
Antigen-specific IgG, IgG1, IgG2a, and IgG2b in the serum were quantitatively determined by enzyme-linked immunosorbent assay (ELISA) in accordance with a protocol described previously [5]. Briefly, 96-well ELISA plates (Costar, Corning, New York, USA) were coated overnight at 4°C with 2 μg of OVA (or 0.2 μg of influenza split vaccine) per well in coating buffer (0.05 M CBS, pH 9.6). Plates were washed with PBST (0.01 M PBS containing 0.05% (m/v) Tween 20, pH 7.4) and blocked by incubating with 2% (m/v) BSA (Roche, Basel, Switzerland) in PBST for 60 min at 37°C. After washes with PBST, 100 μL per well of appropriate sera dilutions were added to the plates, serially diluted two-fold in dilution buffer (PBST containing 0.1% (m/v) BSA), and incubated for 30 min at 37°C. Plates were then washed and incubated with 100 μL horseradish peroxidase-conjugated goat antibodies against either mouse IgG (Sigma-Aldrich, St. Louis, MO, USA), IgG1, IgG2a, or IgG2b (Santa Cruz, CA, USA) (IgG diluted 1:20000; IgG1, IgG2a and IgG2b diluted 1:2000) for 30 min at 37°C. Thereafter, the plates were washed again with PBST, and 100 μL of 3,3′,5,5′-tetramethylbenzidine (TMB) substrate was added to each well and incubated for 20 min at room temperature. After stopping the reaction by adding 50 μL of 2 M H2SO4 to each well, the optical density (OD, 450 nm) was measured by an Infinite M200 Microplate Spectrophotometer (Tecan, Männedorf, Switzerland). Titers were given as the reciprocal sample dilution corresponding to twice higher OD than that of the negative sera.
Hemagglutination Inhibition (HI) Assay
To further evaluate the efficacy of particles-adjuvanted H5N1 influenza vaccine, the HI assay was performed to detect anti-HA antibody levels, according to previously described method [12].
Determination of Cytokine Levels in Splenocytes Culture Supernatant
For mice immunized with OVA antigen, splenocytes were collected 10 days after the third immunization, and stimulated with antigen (OVA, 50 μg/mL; splenocytes, 4 × 106 cells/mL) for 85 h at 37°C in a humid atmosphere with 5% CO2. The supernatant was collected by centrifugation (500 × g, 5 min). IFN-γ, IL-4, and granzyme B levels in the supernatant were measured by Ready-to-use Sandwich ELISA kits (eBioscience, San Diego, CA), and IL-5, IL-6, IL-12, and TNF-α levels in the supernatant were detected by ProcartaPlex Mouse Essential Th1/Th2 Cytokine Panel (eBioscience, San Diego, CA), according to the manufacturer’s instructions.
For mice immunized with H5N1 influenza split vaccine, splenocytes were collected 14 days after the second immunization, and stimulated with HA (2.5 μg/mL; splenocytes, 5 × 106 cells/mL) or IYSTVASSL peptide (1 μg/mL; splenocytes, 5 × 106 cells/mL) for 65 h at 37°C in a humid atmosphere with 5% CO2. Concentrations of IFN-γ and granzyme B in the culture supernatant were measured by Ready-to-use Sandwich ELISA kits (eBioscience, San Diego, CA).
Splenocyte Proliferation Assay
Splenocytes were harvested from C57BL/6 mice immunized with OVA antigen, 10 days after the third immunization. Splenocyte proliferation assay was carried out as previously described method [5, 20]. Briefly, splenocytes (1.2 × 106 cells/mL), stimulated with OVA (50 μg/mL) or not, were seeded in triplicate (100 μL/well) in a 96-well plate and incubated at 37°C in a humid atmosphere with 5% CO2. After 40 h, 10 μL of CCK-8 solution (Dojindo, Japan) was added to each well, and the plates were incubated for an additional 4 h. The absorbance at 450 nm (with 620 nm as reference) was measured by an Infinite M200 Microplate Spectrophotometer (Tecan, Männedorf, Switzerland). The results were expressed as the proliferation index (PI): PI = OD (450 nm) for stimulated cultures/OD (450 nm) for non-stimulated cultures.
Evaluation of T Cell Activation and Memory T Cell Responses by Flow Cytometry
Ten days after the third immunization, splenocytes were collected from OVA antigen-immunized C57BL/6 mice. Frequencies of activated T cells and memory T cells in splenocytes were measured by flow cytometry. Cells were cultured in RPMI 1640 supplemented with 10% fetal bovine serum (4.0 × 106 cells/mL) and re-stimulated with peptide for 60 h. Cells stimulated with MHC I peptide (OVA257–264, 1 μg/mL) were stained with the following set of fluorochrome-conjugated anti-mouse antibodies: Alexa Fluor 488–anti-CD8α, PE–anti-CD44, APC–anti-CD62L, and eFluor 450–anti-CD69 (eBioscience). Cells stimulated with MHC II peptide (OVA323–339, 2 μg/mL) were stained with the following set of fluorochrome-conjugated anti-mouse antibodies: eFluor 450–anti-CD4, PE–anti-CD44, APC–anti-CD62L, and FITC–anti-CD69 (eBioscience). After washing, cell samples were examined by Beckman Coulter CyAn™ ADP flow cytometer, and data were analyzed by Summit software (version 4.3).
Statistical Analysis
All data in this study were shown as the mean ± standard error of the mean (SEM). Statistical analysis was performed using GraphPad Prism 5.0 software (San Diego, CA, USA). Differences among multiple groups were tested using one-way ANOVA followed by Tukey’s multiple comparison. Differences between two groups were tested by an unpaired, two-tailed Student’s t-test. Significant differences between the groups were expressed as: *p < 0.05, **p < 0.01, and ***p < 0.001.
Results and Discussion
Characteristics of PLGA Microparticles and Vaccine Formulations
The objective of this study is to investigate the adjuvanticity of immunopotentiator-loaded microparticles. To perform this study, blank and IMQ-loaded PLGA microparticles were prepared by O/W emulsion–solvent evaporation method combined with the premix SPG membrane emulsification technique, as shown in Fig. 1a [12]. The diameters of blank PLGA microparticles (PMPs) and IMQ-loaded PLGA microparticles (IPMPs) were 1038 ± 12.41 and 979.0 ± 19.73 nm, respectively (Table I, Fig. 1c). Scanning electron micrographs revealed that both PMPs and IPMPs were spherical particles with narrow size distributions (Fig. 1d). Thus, similar sizes were acquired for PMPs and IPMPs. The zeta potential of both microparticles were −31.93 ± 0.32 and −22.90 ± 0.29 mV, respectively (Table I, Fig. 1c). The IMQ content in IPMPs was 22.51 ± 2.30 μg/mg, as determined by high performance liquid chromatography (Table I). As shown in Fig. S6, the in vitro release profile indicated that IMQ encapsulated within PLGA microparticles was released in a sustained manner, with the burst effect appearing in the first 24 h. In this study, vaccine formulations were prepared by mixing antigen with adjuvants (Fig. 1b). Antigen adsorption efficiency analysis indicated that little antigen adsorbed onto microparticles surface (<5%), and more than 80% of antigen was adsorbed by alum adjuvant (aluminum hydroxide gels).
In Vitro Study of Antigen Uptake and APCs Activation
Antigen-presenting cells (APCs) play important roles in antigen presentation and subsequent initiation of adaptive immune responses. Antigen uptake by APCs is a prerequisite of antigen presentation and subsequent T cells activation. After fabricating PMPs and IPMPs, we firstly evaluated their effects on antigen uptake by macrophages, a kind of professional APCs. We incubated different vaccine formulations with peritoneal macrophages (pMΦs), and detected antigen uptake by flow cytometer. After incubation for 2 and 4 h, compared to soluble antigen, both PMPs and IPMPs significantly improved antigen uptake (Fig. 2A1, A2). No difference in antigen uptake existed between PMPs- and IPMPs-adjuvanted vaccines. When incubated for 12 h, pMΦs incubated with IPMPs vaccine internalized more antigen than those for PMPs vaccine (Fig. 2A3). We attributed this enhanced antigen uptake to IMQ. We assumed that IMQ released from IPMPs could improve APCs activation, after IPMPs were internalized by APCs. Activated APCs then phagocytized more particles and antigen.
Effects of PMPs and IPMPs on antigen uptake by pMΦ, and activation of BMDCs and pMΦ. Different vaccine formulations (Alexa Fluor 488-labelled OVA, 5 μg/mL; microparticles, 100 μg/mL) were incubated with pMΦs in 24-well plates. At the indicated time points, the percentages of antigen-positive pMΦs were detected using flow cytometer (A1, 2 h; A2, 4 h; A3, 12 h). BMDCs or pMΦs were cultured in 24-well plates, and incubated with OVA (5 μg/mL) and microparticles (100 μg/mL), or OVA (5 μg/mL) alone, for 24 h. Then, cells were harvested and the supernatant was collected. Concentrations of cytokines (IL-1β, IL-6, TNF-α) in the supernatant were determined by ELISA kits. *p < 0.05; **p < 0.01; ***p < 0.001.
In order to verify our hypothesis, we further detected the efficacies of PMPs and IPMPs in activating in vitro cultured APCs (bone marrow-derived dendritic cells and peritoneal macrophages, BMDCs and pMΦs). Inflammatory cytokines are mediators of APCs activity, and secretion of inflammatory cytokines is a hallmark of activated APCs function [21]. Therefore, we measured the concentrations of inflammatory cytokines (IL-1β, IL-6, and TNF-α) in the supernatant of BMDCs and pMΦs incubated in vitro with different vaccine formulations (antigen (OVA) or antigen (OVA)-particles mixture). As shown in Fig. 2, compared to antigen, PMPs increased the secretion of IL-1β and TNF-α by BMDCs and pMΦs (Fig. 2B1, B3, C1, C3). What’s more, IPMPs induced significantly more inflammatory cytokines secretion by BMDCs and pMΦs than PMPs (Fig. 2b, c). Expression of MHC molecules and co-stimulatory molecule (CD86) on APCs also indicates the activation level of APCs. Consequently, we determined the expression of MHC II and CD86 molecules on pMΦs. Results indicated that pMΦs treated with IPMPs vaccine expressed significantly higher levels of MHC II and CD86 than those for PMPs vaccine (Fig. S2 in Supplementary Data). Taken together, combining IMQ within microparticles significantly improved the efficacy of PLGA microparticles in activating APCs. This could be attributed to the action of IMQ. When IPMPs were phagocytized by pMΦs or BMDCs, IMQs were released from microparticles and bound to TLR-7 in endosomes, activating subsequent signal pathways and inducing activation of APCs. After evaluating the effects on APCs activation by in vitro assays, to further assess the adjuvant activity of PMPs and IPMPs, relevant in vivo assays were performed as follows.
Systemic Antibody Responses in Vaccinated Mice
Firstly, we measured how microparticles adjuvant affected systemic antibody responses. IgG, IgG1, IgG2a, and IgG2b titers in serum were detected by ELISA. As shown in Fig. 3A1-A3, at any time points (14, 28, or 38 days after first immunization), IPMPs vaccine elicited the highest IgG titer, followed by PMPs vaccine, and then soluble antigen. We also detected the IgG subclass profiles, i.e. IgG1, IgG2a, and IgG2b titers in sera. These results were same to above-mentioned IgG titers, showing better efficacy of IPMPs in inducing antigen-specific IgG1 (Fig. 2B1-B3), IgG2a (Fig. 2C1-C3), and IgG2b (Fig. 2D1-D3). IgG is consisted of structurally and functionally distinct subclasses, and IgG1, IgG2a, and IgG2b are main IgG subclasses induced by protein antigens [12, 22]. IgG2a and IgG2b are the most effective in activating immune cells (such as macrophages and monocytes), and ratios of IgG2a/IgG1 and IgG2b/IgG1 indicate the Th1/Th2 polarization [12, 22, 23]. Therefore, we analyzed the ratios of IgG2a/IgG1 and IgG2b/IgG1 for IgG antibody elicited by different vaccine formulations. As shown in Fig. S3 in Supplementary Data, the ratios of IgG2a/IgG1 (Fig. S3A) and IgG2b/IgG1 (Fig. S3B) for IgG induced by IPMPs vaccine were higher than those for PMPs vaccine, suggesting that IPMPs showed more potent adjuvanticity to induce Th1-polarized immune response. Taken together, incorporation of IMQ within microparticles significantly promoted the efficacy of PLGA microparticles in evoking antigen-specific antibody responses.
Antigen-specific IgG antibody responses in C57BL/6 mice immunized with different vaccine formulations (OVA as antigen). Mice (n = 8) were intramuscularly vaccinated on day 0, 14, and 28 as described in the Methods section. (A1-A3) IgG titers, (B1-B3) IgG1, (C1-C3) IgG2a, and (D1-D3) IgG2b in the serum at the indicated time points after first immunization. Data are shown as the mean ± SEM (n = 8). *p < 0.05; **p < 0.01; ***p < 0.001.
Cytokine Levels Secreted by Ex Vivo re-Stimulated Splenocytes
Since we observed that IPMPs displayed better efficacy in antibody response in mice compared to PMPs, we next explored whether these microparticles could also alter the cytokine secretion profiles in mice. Splenocytes harvested from vaccinated mice were re-stimulated ex vivo with OVA, and Th1 (IFN-γ, IL-12, TNF-α) and Th2 (IL-4, IL-5, IL-6) cytokines in the supernatant were determined. As shown in Fig. 4a, microparticles adjuvants improved IFN-γ secretion by splenocytes, and the IFN-γ level produced by splenocytes from mice immunized by IPMPs vaccine was higher than that for PMPs vaccine. Significant differences in IL-12 and IL-5 secretion were observed between IPMPs vaccine and soluble antigen (p < 0.01, Fig. 4b, e). Similar TNF-α and IL-4 levels were produced by splenocytes from mice immunized with both microparticles-adjuvanted vaccine formulations, which were significantly higher than that for soluble antigen (Fig. 4c, d). As shown in Fig. 4f, with respect to IL-6 secretion, no difference was observed between PMPs vaccine and soluble antigen. However, IPMPs vaccine induced significantly more IL-6 production than PMPs vaccine and soluble antigen (p < 0.05). In order to analyze the Th1/Th2 bias, we calculated the ratio of IFN-γ to IL-4. Result showed that IPMPs induced larger IFN-γ/IL-4 ratio, indicating stronger Th1 polarization (Fig. S4 in Supplementary Data). This result was consistent with the above-described IgG subclasses ratios. We also determined the degranulation of CD8+ T cells by detecting release of granzyme B, to evaluate the cytotoxic phenotype of CD8+ T cells induced by different vaccine formulations [24]. As shown in Fig. 5, more granzyme B was released from antigen-specific CD8+ T cells from mice immunized with microparticles-adjuvanted vaccines as compared to soluble antigen, and significant difference existed between groups of IPMPs vaccine and soluble antigen (p < 0.05). On the whole, compared to PMPs, IPMPs induced higher levels of both cytokines (Th1 and Th2 cytokines) and granzyme B secretion by splenocytes, indicating stronger immune responses.
Cytokine secretion by splenocytes. C57BL/6 mice (n = 8) were immunized with different vaccine formulations (OVA as antigen) for three times as described in the Methods section. Splenocytes were harvested 10 days after the third immunization, and restimulated with OVA (50 μg/mL) in culture for 85 h ex vivo. Concentrations of IFN-γ (A), IL-12 (B), TNF-α (C), IL-4 (D), IL-5 (E), and IL-6 (F) in the supernatant were measured. Data are expressed as the mean ± SEM (n = 8). *p < 0.05; **p < 0.01; ***p < 0.001.
Granzyme B secretion by splenocytes. C57BL/6 mice (n = 8) were immunized with different vaccine formulations (OVA as antigen) for three times as described in the Methods section. Splenocytes were harvested 10 days after the third immunization, and restimulated with OVA (50 μg/mL) in culture for 85 h ex vivo. Concentrations of granzyme B in the supernatant were measured. Data are expressed as the mean ± SEM (n = 8). *p < 0.05.
Splenocyte Proliferation Assay
An ex vivo splenocyte proliferation assay was performed to evaluate the effects of both microparticles on splenocyte proliferative responses. As shown in Fig. 6, under the stimulation of OVA, splenocytes collected from mice immunized with IPMPs vaccine proliferated more efficiently than those collected from mice immunized with PMPs vaccine (p < 0.05) or soluble antigen (p < 0.01). Therefore, we believed that IPMPs vaccine evoked more potent antigen-specific immune responses than other formulations.
Proliferative responses of splenocytes responding to antigen ex vivo. C57BL/6 mice (n = 8) were immunized with different vaccine formulations (OVA as antigen) for three times as described in the Methods section. Splenocytes were harvested 10 days after the third immunization and restimulated ex vivo with antigen for 40 h. Splenocyte proliferation was measured using CCK-8 kit, and the proliferation index was calculated. Data are expressed as the mean ± SEM (n = 8). *p < 0.05; **p < 0.01.
T Cell Activation Assays
CD69 is an early marker of activated lymphocytes [25, 26]. Therefore, we determined the frequencies of CD69+ T cells in splenocytes harvested from immunized mice by flow cytometry, to evaluate activation of T cells. As shown in Fig. 7, expression of CD69 on CD4+ T cells (Fig. 7a) and CD8+ T cells (Fig. 7b) from mice immunized with IPMPs vaccine was significantly more than those for PMPs vaccine and soluble antigen. Representative FACS histograms of the mean percentages were shown in Fig. 7c, d. These results indicated that IPMPs vaccine formulation induced more potent T cell activation than other formulations.
Frequency of activated (CD69+) CD4+ and CD8+ T cells in splenocytes. C57BL/6 mice (n = 8) were immunized with different vaccine formulations (OVA as antigen) for three times as described in the Methods section. Splenocytes were harvested 10 days after the third immunization and restimulated ex vivo with antigen for 85 h. The frequency of CD69+CD4+ T cells (a) and CD69+CD8+ T cells (b) were measured by flow cytometry. FACS histograms in (c) and (d) are representative of the mean percentages of 8 mice in each group. Data in (a) and (b) are expressed as the mean ± SEM (n = 8). *p < 0.05; **p < 0.01.
Memory T Cell Responses
The aim of vaccination is to induce protective immunity, i.e. immunological memory. Here, we determined the frequencies of central-memory (CD44hiCD62Lhi) and effector-memory (CD44hiCD62Llow) T cells in splenocytes harvested from immunized mice by flow cytometry, to assess memory T cell responses. The frequency of CD44hiCD62Lhi central-memory CD4+ T cells in splenocytes harvested from mice immunized with IPMPs vaccine was higher than those for PMPs vaccine and soluble antigen (Fig. 8a). Significant differences in frequencies of CD44hiCD62Llow effector-memory CD4+ T cells (Fig. 8b), CD44hiCD62Lhi central-memory CD8+ T cells (Fig. 8c), and CD44hiCD62Llow effector-memory CD8+ T cells (Fig. 8d) were observed between IPMPs vaccine and soluble antigen (p < 0.05). With regard to CD44hiCD62Llow effector-memory CD4+ T cells (Fig. 8b) and CD44hiCD62Lhi central-memory CD8+ T cells (Fig. 8c) T cells, significant differences existed between PMPs- and IPMPs-adjuvanted vaccine formulations (p < 0.05). Representative FACS plots of the mean percentages for CD4+ T cells and CD8+ T cells were shown in Fig. 8e and f, respectively. In summary, IPMPs-based vaccine formulation elicited the strongest memory T cell responses. Central memory T cells which are located in lymphoid tissues have long life span and high proliferative capacity to produce effector cells to deal with pathogen infection [27]. Although having less proliferative potential than central memory T cells, effector memory T cells traffic through nonlymphoid tissues and can rapidly respond to antigen re-exposure [28]. Therefore, stronger memory T cell responses indicate better vaccine efficacy.
Frequency of central (CD44hiCD62Lhi)/effector (CD44hiCD62Llow) memory CD4+ and CD8+ T cells. C57BL/6 mice (n = 8) were immunized with different vaccine formulations (OVA as antigen) for three times as described in the Methods section. Splenocytes were harvested 10 days after the third immunization and restimulated ex vivo with antigen for 85 h. The frequency of CD44hiCD62Lhi CD4+ T cells (a), CD44hiCD62Llow CD4+ T cells (b), CD44hiCD62Lhi CD8+ T cells (c), and CD44hiCD62Llow CD8+ T cells (d) were measured by flow cytometry. FACS plots in (e) and (f) are representative of the mean percentages of eight mice in each group. Data in (a), (b), (c), and (d) are expressed as the mean ± SEM (n = 8). *p < 0.05.
Adjuvant Effects of IMQ-Loaded PLGA Microparticles for H5N1 Influenza Split Vaccine
As mentioned above, we have investigated the adjuvanticity of IPMPs for model antigen ovalbumin (OVA), and found that combining IMQ within microparticles significantly improved the adjuvant effects of PLGA microparticles. To further investigate the adjuvant activity, we evaluated the effects of IPMPs on immune response to H5N1 influenza split vaccine in mice.
We firstly assessed antigen-specific antibody titers in sera. No significant difference in IgG titers was observed between groups of blank and IMQ-loaded PLGA microparticles-adjuvanted vaccine formulations (Fig. 9a, b). As shown in Fig. 9c, both blank and IMQ-loaded PLGA microparticles-adjuvanted vaccine formulations elicited significantly higher haemagglutinin inhibition titers than soluble antigen (p < 0.05).
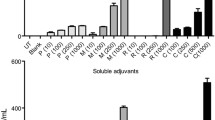
Adjuvant effects of IMQ-loaded PLGA MPs for H5N1 influenza split vaccine. Female Balb/c mice (5–6 weeks, n = 5) were intramuscularly immunized twice with 100 μL (50 μL/hind leg) of different vaccine formulations containing 3 μg of HA, at a 2-week interval. Blood samples were collected from the caudal vein before each immunization and 14 days after the second immunization. At 14 days after the second immunization, splenocytes were collected for ex vivo cytokine response assay. (a) IgG titer in serum at 14 days after the first immunization; (b) IgG titer in serum at 28 days after the first immunization; (c) Hemagglutination Inhibition (HI) titer in serum at 28 days after the first immunization; (d) IFN-γ concentration in the culture supernatant of splenocytes stimulated with HA ex vivo; Concentrations of IFN-γ (e) and granzyme B (f) in the culture supernatant of splenocytes stimulated with IYSTVASSL peptide ex vivo. *p < 0.05; **p < 0.01.
Then, we evaluated cellular immune responses by determining cytokines secretion by splenocytes re-stimulated by antigen in vitro. As shown in Fig. 9d, e, IMQ-loaded PLGA microparticles-adjuvanted vaccine, but not PLGA microparticles-based vaccine, induced significantly more IFN-γ secretion by splenocytes than alum-adjuvanted vaccine and soluble antigen (p < 0.05). We also carried out ELISpot assay to evaluate production of IFN-γ by splenocytes. The results (Fig. S5) were similar to above-mentioned data by ELISA assay, both indicating that IMQ-loaded PLGA microparticles induced more IFN-γ secretion by splenocytes. Release of granzyme B was determined to evaluate the degranulation of CD8+ T cells. Result indicated that both microparticles-adjuvanted vaccine formulations induced significantly more granzyme B release than alum-based vaccine and soluble antigen (p < 0.05, Fig. 9f). IMQ-loaded PLGA microparticles-based vaccine developed slightly more granzyme B release than PLGA microparticles-adjuvanted vaccine. Previous reports showed that cellular immunity played important role in influenza vaccines (especially in protecting against mutated viruses), and should deserve more attentions [29]. Results here suggested that IMQ-loaded PLGA microparticles showed better efficacy in augmenting cellular immune response, because the Th1 cytokine IFN-γ could directly improve cell-mediated immunity, [30] and degranulation of CD8+ T cells played an important role in CTL response. Further virus challenge study should be carried out to confirm whether the improved cellular immunity could provide better protection against influenza virus infection.
Adjuvants are required to ensure the efficacy of subunit vaccines (such as recombinant or purified proteins) with better safety profiles. Although adjuvant based on molecular immunopotentiators show excellent adjuvant activity, their uses are limited by some factors, such as adjuvant solubility, uptake efficiency by immune cells, system distribution and potential toxicity, and so on [7, 15]. Particle-based delivery systems are another kind of promising vaccine adjuvant. Incorporation of molecular adjuvants within particle delivery systems could overcome some drawbacks of molecular adjuvants, and improve the adjuvanticity of particles, achieving more potent adjuvant activity. In this study, we fabricated IMQ-loaded PLGA microparticles from FDA-approved polymer PLGA and immunopotentiator IMQ, and evaluated their adjuvanticity for model antigen ovalbumin and H5N1 influenza split vaccine. In vitro and in vivo studies showed that incorporation of IMQ into PLGA microparticles significantly augmented immune responses (especially cellular immune response) to antigen mixed with microparticles. This study suggested that IMQ-loaded PLGA microparticles were promising robust adjuvant platform for subunit vaccines.
Conclusions
In this study, IMQ-loaded PLGA microparticles were prepared from FDA-approved polymer PLGA and immunopotentiator IMQ, and their adjuvant effects were investigated, using model antigen ovalbumin (OVA) and H5N1 influenza split vaccine as antigens. In vitro study showed that incorporation of IMQ into microparticles significantly improved the efficacy of PLGA microparticles in activating BMDCs and pMΦs, and improving antigen uptake. In vivo studies showed that IMQ-loaded PLGA microparticles-adjuvanted vaccine (OVA) induced more potent immune responses, including higher IgG titer, more cytokines secretion, stronger splenocyte proliferation and activation, and stronger memory T cell response, than PLGA microparticles-based vaccine. IgG subclass profile and cytokine secretion level by splenocytes indicated that IMQ-loaded PLGA microparticles elicited more Th1-polarized immune response, in comparison to PLGA microparticles. In vivo study using H5N1 influenza split vaccine as antigen also confirmed the effects of IMQ-loaded PLGA microparticles on antigen-specific cellular immune response. These results showed that incorporation of IMQ into microparticles enhanced the adjuvanticity of PLGA microparticles. Considering the safety profiles (PLGA and IMQ, both approved by FDA) and the adjuvanticity of IMQ-loaded PLGA microparticles, we conclude that this kind of immunopotentiator-loaded polymeric microparticles are promising robust adjuvant platform for subunit vaccines.
Abbreviations
- Ag:
-
Antigen
- Alum:
-
Aluminum hydroxide gels
- APCs:
-
Antigen-presenting cells
- BMDCs:
-
Bone marrow-derived dendritic cells
- ELISA:
-
Enzyme-linked immunosorbant assay
- ELISpot:
-
Enzyme-linked immunospot
- HA:
-
Hemagglutination
- HI:
-
Hemagglutination inhibition
- PMPs:
-
PLGA microparticles (PLGA)
- IPMPs:
-
IMQ-loaded PLGA microparticles (IMQ-PLGA)
- pMΦ:
-
Peritoneal macrophages
- SEM:
-
Standard errors of mean
- TMB:
-
3,3´,5,5´-tetramethylbenzidine
References
Sahdev P, Ochyl LJ, Moon JJ. Biomaterials for nanoparticle vaccine delivery systems. Pharm Res. 2014;31(10):2563–82.
Ulmer JB, Valley U, Rappuoli R. Vaccine manufacturing: challenges and solutions. Nat Biotechnol. 2006;24(11):1377–83.
Broaders KE, Cohen JA, Beaudette TT, Bachelder EM, Fréchet JMJ. Acetalated dextran is a chemically and biologically tunable material for particulate immunotherapy. Proc Natl Acad Sci U S A. 2009;106(14):5497–502.
Sokolova V, Knuschke T, Kovtun A, Buer J, Epple M, Westendorf AM. The use of calcium phosphate nanoparticles encapsulating Toll-like receptor ligands and the antigen hemagglutinin to induce dendritic cell maturation and T cell activation. Biomaterials. 2010;31(21):5627–33.
Zhang W, Wang L, Liu Y, Chen X, Liu Q, Jia J, et al. Immune responses to vaccines involving a combined antigen–nanoparticle mixture and nanoparticle-encapsulated antigen formulation. Biomaterials. 2014;35(23):6086–97.
Moyle PM, Toth I. Modern subunit vaccines: development, components, and research opportunities. Chem Med Chem. 2013;8(3):360–76.
Fischer NO, Rasley A, Blanchette C. Nanoparticles and antigen delivery: understanding the benefits and drawbacks of different delivery platforms. Nanomedicine. 2014;9(4):373–6.
Foged C. Subunit vaccines of the future: the need for safe, customized and optimized particulate delivery systems. Ther Deliv. 2011;2(8):1057–77.
Kornbluth RS, Stone GW. Immunostimulatory combinations: designing the next generation of vaccine adjuvants. J Leukocyte Biol. 2006;80(5):1084–102.
Coffman RL, Sher A, Seder RA. Vaccine adjuvants: putting innate immunity to work. Immunity. 2010;33(4):492–503.
Rizwan SB, McBurney WT, Young K, Hanley T, Boyd BJ, Rades T, et al. Cubosomes containing the adjuvants imiquimod and monophosphoryl lipid A stimulate robust cellular and humoral immune responses. J Control Release. 2013;165(1):16–21.
Zhang W, Wang L, Liu Y, Chen X, Li J, Yang T, et al. Comparison of PLA microparticles and Alum as adjuvants for H5N1 influenza split vaccine: adjuvanticity evaluation and preliminary action mode analysis. Pharm Res. 2014;31(4):1015–31.
Prins RM, Craft N, Bruhn KW, Khan-Farooqi H, Koya RC, Stripecke R, et al. The TLR-7 agonist, imiquimod, enhances dendritic cell survival and promotes tumor antigen-specific T cell priming: relation to central nervous system antitumor immunity. J Immunol. 2006;176(1):157–64.
Bachelder EM, Beaudette TT, Broaders KE, Fréchet JMJ, Albrecht MT, Mateczun AJ, et al. In vitro analysis of acetalated dextran microparticles as a potent delivery platform for vaccine adjuvants. Mol Pharm. 2010;7(3):826–35.
Primard C, Poecheim J, Heuking S, Sublet E, Esmaeili F, Borchard G. Multifunctional PLGA-based nanoparticles encapsulating simultaneously hydrophilic antigen and hydrophobic immunomodulator for mucosal immunization. Mol Pharm. 2013;10(8):2996–3004.
Paula DD, Martins CA, Bentley MVLB. Development and validation of HPLC method for imiquimod determination in skin penetration studies. Biomed Chromatogr. 2008;22(12):1416–23.
Bachute MT, Turwale SL. A rapid and validated reverse phase liquid chromatographic method for determination of imiquimod from topical cream formulations. J Pharm Res. 2013;6(1):73–7.
Liu Y, Yin Y, Wang L, Zhang W, Chen X, Yang X, et al. Surface hydrophobicity of microparticles modulates adjuvanticity. J Mater Chem B. 2013;1(32):3888–96.
Selvarajan K, Moldovan L, Chandrakala AN, Litvinov D, Parthasarathy S. Peritoneal macrophages are distinct from monocytes and adherent macrophages. Atherosclerosis. 2011;219(2):475–83.
Liu Y, Yin Y, Wang LY, Zhang WF, Chen XM, Yang XX, et al. Engineering biomaterial-associated complement activation to improve vaccine efficacy. Biomacromolecules. 2013;14(9):3321–8.
Murtaugh MP, Foss DL. Inflammatory cytokines and antigen presenting cell activation. Vet Immunol Immunop. 2002;87(3–4):109–21.
Nimmerjahn F, Ravetch JV. Divergent immunoglobulin G subclass activity through selective Fc receptor binding. Science. 2005;310(5753):1510–2.
Woof JM. Tipping the scales toward more effective antibodies. Science. 2005;310(5753):1442–3.
Stano A, Scott EA, Dane KY, Swartz MA, Hubbell JA. Tunable T cell immunity towards a protein antigen using polymersomes vs. solid-core nanoparticles. Biomaterials. 2013;34(17):4339–46.
Marzio R, Mauël J, Betz-Corradin S. CD69 and regulation of the immune function. Immunopharm Immunot. 1999;21(3):565–82.
Lindsey W, Lowdell M, Marti G, Abbasi F, Zenger V, King K, et al. CD69 expression as an index of T-cell function: assay standardization, validation and use in monitoring immune recovery. Cytotherapy. 2007;9(2):123–32.
Thakur A, Pedersen LE, Jungersen G. Immune markers and correlates of protection for vaccine induced immune responses. Vaccine. 2012;30(33):4907–20.
Patel A, Zhang Y, Croyle M, Tran K, Gray M, Strong J, et al. Mucosal delivery of adenovirus-based vaccine protects against Ebola virus infection in mice. J Infect Dis. 2007;196(Supplement 2):S413–20.
Schotsaert M, Saelens X, Leroux-Roels G. Influenza vaccines: T-cell responses deserve more attention. Expert Rev Vaccines. 2012;11(8):949–62.
Ma Y, Zhuang Y, Xie X, Wang C, Wang F, Zhou D, et al. The role of surface charge density in cationic liposome-promoted dendritic cell maturation and vaccine-induced immune responses. Nanoscale. 2011;3(5):2307–14.
Acknowledgments and Disclosures
Weifeng Zhang and Lianyan Wang contributed equally to this work. This work was financially supported by the 973 Program (Grant No. 2013CB531500), National Science and Technology Major Project of the Ministry of Science and Technology of China (Grant No. 2014ZX09102045), and Special Fund for Agro-scientific Research in the Public Interest (201303046).
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 1839 kb)
Rights and permissions
About this article
Cite this article
Zhang, W., Wang, L., Yang, T. et al. Immunopotentiator-Loaded Polymeric Microparticles as Robust Adjuvant to Improve Vaccine Efficacy. Pharm Res 32, 2837–2850 (2015). https://doi.org/10.1007/s11095-015-1666-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-015-1666-6