ABSTRACT
Purpose
To test targeted liposomes in an effort to improve drug transport across cellular barriers into the brain.
Methods
Therefore we prepared Mitoxantrone (MTO) entrapping, rigid and fluid liposomes, equipped with a 19-mer angiopeptide as ligand for LDL lipoprotein receptor related protein (LRP) targeting.
Results
Fluid, ligand bearing liposomes showed in vitro the highest cellular uptake and transcytosis and were significantly better than the corresponding ligand-free liposomes and rigid, ligand-bearing vesicles. Treatment of mice, transplanted with human breast cancer cells subcutaneously and into the brain, with fluid membrane liposomes resulted in a significant reduction in the tumor volume by more than 80% and in a clear reduction in drug toxicity. The improvement was mainly depended on liposome fluidity while the targeting contributed only to a minor degree. Pharmacokinetic parameters were also improved for liposomal MTO formulations in comparison to the free drug. So the area under the curve was increased and t1/2 was extended for liposomes.
Conclusion
Our data show that it is possible to significantly improve the therapy of brain metastases if MTO-encapsulating, fluid membrane liposomes are used instead of free MTO. This effect could be further enhanced by fluid, ligand bearing liposomes.






Similar content being viewed by others
Abbreviations
- BBB:
-
blood–brain barrier
- DMEM:
-
Dulbecco’s Modified Eagle Medium
- FCS:
-
foetal calf serum
- LDL:
-
low-density lipoprotein
- LRP:
-
LDL-lipoprotein receptor related protein
- LUV:
-
large unilamellar vesicles
- MDCK:
-
Madin-Darby canine kidney
- MTO:
-
mitoxantrone
- PIT:
-
post insertion technology
- RTV:
-
relative tumor volume
REFERENCES
Abbott NJ, Patabendige AA, Dolman DE, Yusof SR, Begley DJ. Structure and function of the blood–brain barrier. Neurobiol Dis. 2010;37(1):13–25.
Pardridge WM. Preparation of Trojan horse liposomes (THLs) for gene transfer across the blood–brain barrier. Cold Spring Harb Protoc. 2010;(4) (2010), db.
Agarwal A, Lariya N, Saraogi G, Dubey N, Agrawal H, Agrawal GP. Nanoparticles as novel carrier for brain delivery: a review. Curr Pharm Des. 2009;15(8):917–25.
Blasi P, Schoubben A, Giovagnoli S, Rossi C, Ricci M. Lipid nanoparticles for drug delivery to the brain: in vivo veritas. J Biomed Nanotechnol. 2009;5(4):344–50.
Patel MM, Goyal BR, Bhadada SV, Bhatt JS, Amin AF. Getting into the brain: approaches to enhance brain drug delivery. CNS Drugs. 2009;23(1):35–58.
Tiwari SB, Amiji MM. A review of nanocarrier-based CNS delivery systems. Curr Drug Deliv. 2006;3(2):219–32.
Pardridge WM. Biopharmaceutical drug targeting to the brain. J Drug Target. 2010;18(3):157–67.
Orthmann A, Zeisig R, Koklic T, Sentjurc M, Wiesner B, Lemm M, et al. Impact of membrane properties on uptake and transcytosis of colloidal nanocarriers across an epithelial cell barrier model. J Pharm Sci. 2010;99(5):2423–33.
Chamberlain MC. Anticancer therapies and CNS relapse: overcoming blood–brain and blood-cerebrospinal fluid barrier impermeability. Expert Rev Neurother. 2010;10(4):547–61.
Laquintana V, Trapani A, Denora N, Wang F, Gallo JM, Trapani G. New strategies to deliver anticancer drugs to brain tumors. Expert Opin Drug Deliv. 2009;6(10):1017–32.
Orthmann A, Fichtner I, Zeisig R. Improving the transport of chemotherapeutic drugs across the blood–brain barrier. Expert Rev Clin Pharmacol. 2011;4(4):465–78.
Cerletti A, Drewe J, Fricker G, Eberle AN, Huwyler J. Endocytosis and transcytosis of an immunoliposome-based brain drug delivery system. J Drug Target. 2000;8(6):435–46.
Boado RJ. Blood–brain barrier transport of non-viral gene and RNAi therapeutics. Pharm Res. 2007;24(9):1772–87.
McNeeley KM, Karathanasis E, Annapragada AV, Bellamkonda RV. Masking and triggered unmasking of targeting ligands on nanocarriers to improve drug delivery to brain tumors. Biomaterials. 2009;30(23–24):3986–95.
Feng B, Tomizawa K, Michiue H, Miyatake S, Han XJ, Fujimura A, et al. Delivery of sodium borocaptate to glioma cells using immunoliposome conjugated with anti-EGFR antibodies by ZZ-His. Biomaterials. 2009;30(9):1746–55.
Demeule M, Currie JC, Bertrand Y, Che C, Nguyen T, Regina A, Gabathuler R, Castaigne JP, Beliveau R. Involvement of the low-density lipoprotein receptor-related protein in the transcytosis of the brain delivery vector angiopep-2. J Neurochem. 2008;106(4):1534–44.
Li Y, Cam J, Bu G. Low-density lipoprotein receptor family: endocytosis and signal transduction. Mol Neurobiol. 2001;23(1):53–67.
Lillis AP, Van Duyn LB, Murphy-Ullrich JE, Strickland DK. LDL receptor-related protein 1: unique tissue-specific functions revealed by selective gene knockout studies. Physiol Rev. 2008;88(3):887–918.
Hussain MM, Strickland DK, Bakillah A. The mammalian low-density lipoprotein receptor family. Annu Rev Nutr. 1999;19:141–72.
Demeule M, Regina A, Che C, Poirier J, Nguyen T, Gabathuler R, Castaigne JP, Beliveau R. Identification and design of peptides as a new drug delivery system for the brain. J Pharmacol Exp Ther. 2008;324(3):1064–72.
Regina A, Demeule M, Che C, Lavallee I, Poirier J, Gabathuler R, et al. Antitumour activity of ANG1005, a conjugate between paclitaxel and the new brain delivery vector Angiopep-2. Br J Pharmacol. 2008;155(2):185–97.
Che C, Yang G, Thiot C, Lacoste MC, Currie JC, Demeule M, et al. New Angiopep-modified doxorubicin (ANG1007) and etoposide (ANG1009) chemotherapeutics with increased brain penetration. J Med Chem. 2010;53(7):2814–24.
Chan WC, White PD. Fmoc solid phase peptide synthesis – A practical Approach. Oxford: Oxford University Press; 2000.
Fritze A, Hens F, Kimpfler A, Schubert R, Peschka-Süss R. Remote loading of doxorubicin into liposomes driven by a transmembrane phosphate gradient. Biochim Biophys Acta. 2006;1758(10):1633–40.
Gantert M, Lewrick F, Adrian JE, Rossler J, Steenpass T, Schubert R, et al. Receptor-specific targeting with liposomes in vitro based on sterol-PEG(1300) anchors. Pharm Res. 2009;26(3):529–38.
Zeisig R, Müller K, Maurer N, Arndt D, Fahr A. The composition-dependent presence of free (micellar) alkylphospholipid in liposomal formulations of octadecyl-1,1-dimethyl-piperidino-4-yl-phosphate affects its cytotoxic activity in vitro. J Membr Biol. 2001;182(1):61–9.
Naundorf H, Fichtner I, Saul GJ, Haensch W, BÜttner B. Establishment and characteristics of two new human mammary carcinoma lines serially transplantable in nude mice. J Cancer Res Clin Oncol. 1993;119(11):652–6.
Johnson JL, Ahmad A, Khan S, Wang YF, Abu-Qare AW, Ayoub JE, et al. Improved liquid chromatographic method for mitoxantrone quantification in mouse plasma and tissues to study the pharmacokinetics of a liposome entrapped mitoxantrone formulation. J Chromatogr B Analyt Technol Biomed Life Sci. 2004;799(1):149–55.
Diehl KH, Hull R, Morton D, Pfister R, Rabemampianina Y, Smith D, et al. A good practice guide to the administration of substances and removal of blood, including routes and volumes. J Appl Toxicol. 2001;21(1):15–23.
Pflanzner T, Janko MC, André-Dohmen B, Reuss S, Weggen S, Roebroek AJ, Kuhlmann CR, Pietrzik CU. LRP1 mediates bidirectional transcytosis of amyloid-beta across the blood–brain barrier. Neurobiol Aging. 2011;32(12):2323e1-11.
Gubernator J, Chwastek G, Korycinska M, Stasiuk M, Grynkiewicz G, Lewrick F, et al. The encapsulation of idarubicin within liposomes using the novel EDTA ion gradient method ensures improved drug retention in vitro and in vivo. J Control Release. 2010;146(1):68–75.
Ramsay E, Alnajim J, Anantha M, Zastre J, Yan H, Webb M, Waterhouse D, Bally M. A novel liposomal irinotecan formulation with significant anti-tumour activity: use of the divalent cation ionophore A23187 and copper-containing liposomes to improve drug retention. Eur J Pharm Biopharm. 2008;68(3):607–17.
Zucker D, Barenholz Y. Optimization of vincristine-topotecan combination–paving the way for improved chemotherapy regimens by nanoliposomes. J Control Release. 2010;146(3):326–33.
Ishida T, Harashima H, Kiwada H. Liposome clearance. Biosci Rep. 2002;22(2):197–224.
Zeisig R, Eue I, Kosch M, Fichtner I, Arndt D. Preparation and properties of sterically stabilized hexadecylphosphocholine (miltefosine)-liposomes and influence of this modification on macrophage activation. Biochim Biophys Acta. 1996;1283(2):177–84.
Xi X, Yang F, Chen D, Luo Y, Zhang D, Gu N, et al. A targeting drug-delivery model via interactions among cells and liposomes under ultrasonic excitation. Phys Med Biol. 2008;53(12):3251–65.
Torchilin VP. Recent approaches to intracellular delivery of drugs and DNA and organelle targeting. Annu Rev Biomed Eng. 2006;8:343–75.
Bhaskar S, Tian F, Stoeger T, Kreyling W, de la Fuente JM, Grazu V, Borm P, Estrada G, Ntziachristos V, Razansky D. Multifunctional Nanocarriers for diagnostics, drug delivery and targeted treatment across blood–brain barrier: perspectives on tracking and neuroimaging. Part Fibre Toxicol. 2010;7(3):3. doi:10.1186/1743-8977-7-3.
Yemisci M, Bozdag S, Cetin M, Soylemezoglu F, Capan Y, Dalkara T, et al. Treatment of malignant gliomas with mitoxantrone-loaded poly (lactide-co-glycolide) microspheres. Neurosurgery. 2006;59(6):1296–302.
Boiardi A, Eoli M, Salmaggi A, Lamperti E, Botturi A, Broggi G, et al. Systemic temozolomide combined with loco-regional mitoxantrone in treating recurrent glioblastoma. J Neurooncol. 2005;75(2):215–20.
Boiardi A, Eoli M, Salmaggi A, Lamperti E, Botturi A, Solari A, et al. Local drug delivery in recurrent malignant gliomas. Neurol Sci. 26 2005; Suppl 1(S37–9):S37–S39.
Kawano K, Onose E, Hattori Y, Maitani Y. Higher liposomal membrane fluidity enhances the in vitro antitumor activity of folate-targeted liposomal mitoxantrone. Mol Pharm. 2009;6(1):98–104.
van Rooy I, Mastrobattista E, Storm G, Hennink WE, Schiffelers RM. Comparison of five different targeting ligands to enhance accumulation of liposomes into the brain. J Control Release. 2011;150(1):30–6.
Zeisig R, Koklic T, Wiesner B, Fichtner I, Sentjurc M. Increase in fluidity in the membrane of MT3 breast cancer cells correlates with enhanced cell adhesion in vitro and increased lung metastasis in NOD/SCID mice. Arch Biochem Biophys. 2007;459(1):98–106.
ACKNOWLEDGMENTS & DISCLOSURES
This project was financed in part by a grant of the Federal Ministry of Economics and Technology of Germany, PRO INNO II (KA0453401UL7). The authors gratefully acknowledge the excellent technical support of Annika Hoffmann (EPO GmbH, Berlin) and the valuable discussions about post insertion technology with Ronny Rüger (Friedrich-Schiller-Universität Jena). We also thank Lipoid GmbH Ludwigshafen for providing us with egg phosphatidylcholine.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
S1
Vesicle stability over time during storage in PBS. Changes in vesicle diameter were followed by dynamic light scattering (PCS) measurements. Stock solutions of liposomes were appropriately diluted and measured in triplicate at each predefined time point. Mean unimodal diameters ± S.D. are shown. (PDF 11 kb)
S2
LRP receptor expression by cells used. Cells were incubated with 50 μg/ml of the fluorescence labeled peptide 2 for indicated times at 37°C and 4°C. Two-color immunofluorescence cytometry was used to quantify the expression of LRP receptor on cellular surface using 10000 cells. Cell populations were gated and the percentage of cells positive for LRP receptor was calculated based on the mean fluorescence intensity (mFI) from histogram plot. (PDF 4 kb)
S3
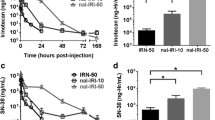
MTO concentration versus time in the heart. NMRI:nu/nu mice were injected with 5 mg/kg MTO as solution or encapsulated in liposomes at t = 0 and mice were sacrificed at pre-defined time points. MTO concentration was determined as described in Material and Methods by HPLC. All data represent the mean ± S.D. for 3 samples, each determined in duplicate. (PDF 19 kb)
S4
MTO concentration versus time in the kidney. For details see S3 (PDF 18 kb)
S5
MTO concentration versus time in the liver. For details see S3 (PDF 18 kb)
S6
MTO concentration versus time in the s.c. tumor. For details see S3 (PDF 21 kb)
S7
MTO concentration versus time in the spleen. For details see S3 (PDF 19 kb)
S8
MTO concentration versus time in the lung. For details see S3 (PDF 19 kb)
S9
Concentration of MTO in different organs at t = 15 min. NMRI:nu/nu mice were injected with 5 mg/kg MTO as solution or encapsulated in liposomes at t = 0 and mice were sacrificed at pre-defined time points. MTO concentration was determined as described in Material and Methods by HPLC. All data represent the mean ± S.D. for 3 samples, each determined in duplicate. Insert: Concentration of MTO in the brain. (PDF 36 kb)
S10
Tumor growth versus time of s.c. tumor. MT-3 cells were transplanted s.c. into the left flank (5*106) and into the brain (5*103) of each nude mouse. Mice were treated i.v. with liposomes containing MTO or with free MTO, each in a dose of 4 mg/kg at day 3, 7 and 10. Control mice received saline solution. Diameter of subcutaneously growing tumor was measured twice weekly. Mice were sacrificed at day 22. Data were obtained from two independently performed experiments and are given as mean values +/− S.D (n: 5–16). (PDF 6 kb)
S11
Body weight change over time. Body weight of mice, which were treated as described in Fig. S9, was measured twice a week. Given is the relative change in body weight (in%) as compared to the start of the experiment. *: significantly different to saline treated group. **: significantly different to saline treated and to L fluid-LG treated group. #: three mice died after the third treatment because of drug related toxicity. (P < 0.05) (PDF 8 kb)
Rights and permissions
About this article
Cite this article
Orthmann, A., Zeisig, R., Süss, R. et al. Treatment of Experimental Brain Metastasis with MTO-Liposomes: Impact of Fluidity and LRP-Targeting on the Therapeutic Result. Pharm Res 29, 1949–1959 (2012). https://doi.org/10.1007/s11095-012-0723-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-012-0723-7