Abstract
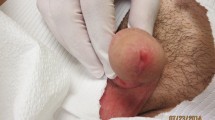
Zygomycoses are opportunistic infections caused by the Mucorales fungi. They are typically seen in immunosuppressed patients. The incidence of zygomycosis cases seems to be increasing. We report on zygomycosis in a pediatric, female stem-cell-transplant recipient. This case report underlines the difficulty of taking care of patients with zygomycosis. In fungal infections of immunosuppressive patients on broad-coverage antibiotics, foci of skin necrosis are unique and typical for zygomycoses, and may be helpful in this challenging diagnosis.



Similar content being viewed by others
References
Spellberg B, Walsh TJ, Kontoyiannis DP, Edwards J Jr, Ibrahim AS. Recent advances in the management of mucormycosis: from bench to bedside. Clin Infect Dis. 2009;48:1743–51.
Singh N, Aguado JM, Bonatti H, et al. Zygomycosis in solid organ transplant recipients: a prospective, matched case-control study to assess risks for disease and outcome. J Infect Dis. 2009;200:1002–11.
Roden MM, Zaoutis TE, Buchanan WL, et al. Epidemiology and outcome of zygomycosis: a review of 929 reported cases. Clin Infect Dis. 2005;41:634–53.
Dehority W, Willert J, Pong A. Zygomycetes infections in pediatric hematology oncology patients: a case series and review of the literature. J Pediatr Hematol Oncol. 2009;31:911–9.
Abuali MM, Posada R, Del Toro G, et al. Rhizomucor variabilis var. regularior and Hormographiella aspergillata infections in a leukemic bone marrow transplant recipient with refractory neutropenia. J Clin Microbiol. 2009;47:4176–9.
Sorensen J, Becker M, Porto L, et al. Rhinocerebral zygomycosis in a young girl undergoing allogeneic stem cell transplantation for severe aplastic anaemia. Mycoses. 2006;49(Suppl 1):31–6.
Chamilos G, Lewis RE, Kontoyiannis DP. Delaying amphotericin B-based frontline therapy significantly increases mortality among patients with hematologic malignancy who have zygomycosis. Clin Infect Dis. 2008;47:503–9.
Partridge-Hinckley K, Liddell GM, Almyroudis NG, Segal BH. Infection control measures to prevent invasive mould diseases in hematopoietic stem cell transplant recipients. Mycopathologia. 2009;168:329–37.
Trifilio S, Singhal S, Williams S, et al. Breakthrough fungal infections after allogeneic hematopoietic stem cell transplantation in patients on prophylactic voriconazole. Bone Marrow Transplant. 2007;40:451–6.
Marty FM, Cosimi LA, Baden LR. Breakthrough zygomycosis after voriconazole treatment in recipients of hematopoietic stem-cell transplants. N Engl J Med. 2004;350:950–2.
Perkhofer S, Locher M, Cuenca-Estrella M, et al. Posaconazole enhances the activity of amphotericin B against hyphae of zygomycetes in vitro. Antimicrob Agents Chemother. 2008;52:2636–8.
Antoniadou A. Outbreaks of zygomycosis in hospitals. Clin Microbiol Infect. 2009;15(Suppl 5):55–9.
Mousset S, Bug G, Heinz WJ, Tintelnot K, Rickerts V. Breakthrough zygomycosis on posaconazole prophylaxis after allogeneic stem cell transplantation. Transpl Infect Dis. 2010;12:261–4.
Lekakis LJ, Lawson A, Prante J, et al. Fatal rhizopus pneumonia in allogeneic stem cell transplant patients despite posaconazole prophylaxis: two cases and review of the literature. Biol Blood Marrow Transpl. 2009;15:991–5.
Zaoutis TE, Roilides E, Chiou CC, et al. Zygomycosis in children: a systematic review and analysis of reported cases. Pediatr Infect Dis J. 2007;26:723–7.
Roilides E, Zaoutis TE, Walsh TJ. Invasive zygomycosis in neonates and children. Clin Microbiol Infect. 2009;15(Suppl 5):50–4.
Bitar D, Van Cauteren D, Lanternier F, et al. Increasing incidence of zygomycosis (mucormycosis), France, 1997–2006. Emerg Infect Dis. 2009;15:1395–401.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kivivuori, SM., Karikoski, R., Koukila-Kähkölä, P. et al. Zygomycosis Presenting a Major Clinical Challenge: Case Report on Rhizomucor pusillus Infection in a Stem-Cell-Transplant Recipient. Mycopathologia 172, 241–245 (2011). https://doi.org/10.1007/s11046-011-9424-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-011-9424-8