Abstract
Previous studies reported that estrogen receptor β (ERβ) is localized to mitochondria, whereas little is known about the physiological functions of mitochondrial ERβ. In the present study, we explored the role of mitochondrial ERβ in regulating apoptosis using stable ERβ-expressing and ERβ knockdown cells lines. We found that exogenous ERβ was mainly expressed in mitochondrial but not in nuclear after ERβ overexpression and protected cells from apoptosis induced by hydrogen peroxide (H2O2), ultraviolet (UV), and staurosporine (STS). Moreover, overexpression of ERβ prevented Bax activation, cytochrome c release, caspase-3 activation, and PARP cleavage during apoptosis. Furthermore, knockdown of ERβ significantly suppressed the expression of ERβ in mitochondrial and promoted cell apoptosis induced by H2O2, UV, and STS. Downregulation of ERβ also enhanced Bax activation, cytochrome c release, caspase-3 activation and PARP cleavage. In addition, our study discovered that mitochondrial ERβ interacted with proapoptotic protein Bad in a ligand-independent manner, which suggests that mitochondrial ERβ inhibits Bad, and prevents Bax activation and cytochrome c release. Collectively, the results of this study support that mitochondrial ERβ prevents cell apoptosis via the mitochondrial apoptotic pathway in a ligand-independent manner.
Similar content being viewed by others
Introduction
Estrogen is a key signaling molecule regulating numerous physiological processes, including cell proliferation, cell differentiation, development, memory, cognition, immune function, reproduction, and behavior. Several lines of evidence have shown that estrogen exerts its physiological effects through binding to specific estrogen receptors (ERs) [1, 2]. There are two different isoforms of ERs, usually referred to as ERα and ERβ which are encoded by genes at different chromosomal locations. It is generally accepted that ERs are members of nuclear hormone receptor superfamily of ligand-dependent transcription factors and mediate the transcriptions of ER-specific target genes in response to hormone 17β-estradiol (E2) [3]. As transcription factors, ERα and ERβ activated by E2 can differentially regulate gene expressions through recruiting different co-activators to specific promoters [4].
ERβ has been initially identified in the mid-1990s, but its functions are less clear compared with ERα. Studies showed that treatment with selective ER agonists could result in reduction of dendritic spines and neuronal cell death, as observed in mouse brain and rat cerebellar granule cell cultures originating from neonatal females [5, 6]. ERα and ERβ have many common characteristics in the molecular structures. There have high sequence homology in their DNA and ligand-binding domains, while the sequences in the N terminus (12 %) and C terminus (9 %) show very low degree of similarity [7]. Moreover, several studies have suggested that ERβ is involved in non-genomic events in different cells and animal models [8, 9]. Intriguingly, in certain systems, endogenous ERβ appears to be completely excluded from the nucleus and does not migrate into the nucleus upon E2 exposure. Therefore, it is not surprising that ERβ has much lower transcriptional activities in the nucleus compared with ERα [10–12].
A number of studies have suggested that E2 affects mitochondrial functions, which explains the differences between male and female mitochondria [13]. The effects of estrogen on cells from nuclear actions of E2/ERs can indirectly affect mitochondrial function [14]. Mitochondria play a vital role in cell metabolism, ionic homeostasis, synthesis of biological molecules, and apoptosis. Mitochondria not only synthesize endogenous E2 by aromatase, but also accept exogenous E2 [15]. Recent studies have shown that ERβ is localized to the mitochondria in many different cell types, including rat primary neuron [16, 17], human hepatocellular liver carcinoma cells [18], and human breast adenocarcinoma cells (MCF-7 and MCF-F10) [19]. All available evidences suggest that ERβ may function as a mitochondrial component, whereas the exact molecular mechanisms underlying the functions of mitochondrial ERβ is poorly understood.
In the current study, we first confirmed the mitochondrial localization of ERβ using immunofluorescence staining and Western blotting analysis in different types of cancer cells. Then we investigated if the mitochondrial ERβ plays a role in the apoptosis of these cancer cell lines and the underlying mechanisms.
Materials and methods
Cell culture
MCF-7, A549, SH-SY5Y, COS-7, and HEK 293T cells were cultured in DMEM medium (GBICO, Co. Ltd., Grand Island, NY) containing 10 % fetal calf serum (FCS, GBICO, Co. Ltd., Grand Island, NY), 50 units/ml penicillin, and 50 μg/ml streptomycin. The cells were maintained in a humidified, 37 °C incubator with 5 % CO2. Then, the cells were cultivated in DMEM supplemented with 10 % charcoal-treated FCS (GIBCO, Co. Ltd., Grand Island, NY) for at least 5 days and were subjected to different treatments. Phenol red-free medium was used in all experiments.
Chemicals, plasmids, and antibodies
Staurosporine (STS) and hydrogen peroxide (H2O2) were procured from Sigma (St. Louis, MO). GFP-ERβ expression plasmid was provided by Matsuda [20]. Flag-Bad expression plasmid was a gift from Fukamizu [21]. Anti-ERβ antibody, anti-β-actin antibody, and anti-Histone H3 antibody were purchased from Santa Cruz Biotechnology (Santa Cruz, CA). Anticleaved caspase 3 antibody, anticleaved PARP antibody, anti-cytochrome c antibody, anti-COX IV antibody, anti-Bax antibody, anti-Bad antibody, anti-Bcl-2 antibody, anti-Bcl-XL antibody, anti-Flag, and anti-GAPDH antibody were purchased from Cell Signaling Technology (Beverly, MA). Anti-Bax (6A7) antibody was purchased from Abcam (Cambridge, UK). Anti-GFP antibody was purchased from Proteintech Group, Inc. (Campell Park, Chicago).
Cell transfection and treatment
Transient transfection experiments were performed using X-treme GENE HP DNA transfection reagent (Roche Applied Science, Mannheim, Germany) according to the manufacturer’s recommendations. A549 and COS-7 cells were seeded onto 22-mm culture glasses cover slips or 60-mm plates the day before transfection. The cells were maintained in Opti-MEM medium (Invitrogen) during transfection, and 8 h later, the culture medium was replaced with fresh culture medium. After 48 h, the cells were subjected to the live cell-imaging experiments. More than 80 % of transfection efficiency was achieved after transfection to A549 and COS-7 cells. For stable transfection experiments, the cells were selected using 600 μg/ml G418 (Sigma), and the colonies were screened for the GFP-ERβ expression by Western blotting.
Immunofluorescence
To demonstrate mitochondrial localization of ERβ, MCF-7, SH-SY5Y, and A549 cells grown on glass cover slips were stained with Mito Tracker Deep Red 633 (100 nM; Molecular Probes, Inc.) at 37 °C for 30 min. Then the cells were fixed with 3.7 % paraformaldehyde for 15 min, followed by permeabilization in 100 % methanol for 10 min at −20 °C. Next, the cells were incubated in blocking buffer (5 % bovine serum albumin in PBS) for 1 h at room temperature, followed by incubation with anti-ERβ and anti-β-actin antibodies (diluted 1:200 in blocking buffer) at 4 °C overnight. Then the cells were washed three times in phosphate-buffered saline (PBS) for 5 min each and incubated with Alexa Fluor 488-conjugated goat anti-mouse secondary antibody for β-actin and Alexa Fluor 555-conjugated goat anti-rabbit secondary antibody for ERβ (diluted 1:300 in blocking buffer; Invitrogen) at room temperature for 1.5 h. Images were acquired using a confocal microscope through a 40× oil immersion objective (NA = 1.3) (LSM710-ConfoCor; Zeiss).
Cell viability assays
A549, SH-SY5Y, and COS-7 cells were seeded onto 96-well microplates at a density of 1 × 104 cells per well the day before transfection. Cells transfected with 250 ng plasmid DNA were subjected to different treatments (STS, H2O2, and UV). Cell viability was assessed by cell counting kit-8 (CCK-8; Dojindo Molecular Technologies, Rockville, MD) according to the manufacturer’s protocol. Cell viability and proliferation were determined by measuring the absorbance at 450 nm in a microplate reader (Thermo, Varioskan Flash).
Confocal laser scanning imaging
Live cell-imaging experiments were performed with a confocal laser scanning microscope (LSM710-ConfoCor; Carl Zeiss Co., Ltd.). Cells were observed with a 40× oil immersion objective lens (NA = 1.3) in a microchamber module connected to a temperature and CO2 controllers (CTI-controller 3700 digital and Temp-control 37-2 digital; Zeiss, Jena, Germany). The cells were maintained at 37 °C, 5 % CO2 during the entire duration of the experiment. GFP fluorescence was excited with a 488-nm Ar-Ion laser, and the fluorescence emission was detected using a 465–510-nm band pass filter. DsRed-mit fluorescence was excited with a 543-nm He–Ne laser, and the fluorescence emission was detected through a 650-nm long pass filter. During the entire experimental period, the exciting powers of 488- and 543-nm laser were kept at the minimum level (1–2 %) to reduce the possible effects of exciting light.
Subcellular fractionation
Mitochondria were isolated using Mitochondria Isolation Kit from Pierce Chemical Co. (Rockford, IL). To prepare nuclear and cytosolic extracts, COS-7 cells were washed twice with ice-cold PBS and disrupted with 200 μl of lysis buffer (10 mM Tris, pH 7.5, 10 mM NaCl, 3 mM MgCl2, 0.05 % Nonidet P-40, 1 mM EGTA, 1 mM sodium orthovanadate, 50 mM sodium fluoride, 100 mM phenylmethylsulfonyl fluoride, 10 mg/ml leupeptin, 10 mg/ml aprotinin, 5 mg/ml pepstatin A, and 1 nM okadaic acid). Nuclear and cytosolic extracts were obtained as described previously [22].
RNA interference (RNAi)
ERβ expression was knocked down by ERβ-shRNA. ERβ-shRNA and the control vector were kindly provided by Carroll [23]. In brief,, A549 and SH-S5Y5 cells were seeded onto 96-well microplates at a density of 1 × 104 cells per well one day before transfection. Cells were transfected with 250 μg ERβ-shRNA or the control vector using X-tremeGENE HP DNA transfection reagent (Roche Applied Science, Mannheim, Germany) according to the manufacturer’s recommendations. After transfection, the cells were selected using 800 μg/mL G418. The efficiency of ERβ-shRNA knockdown in each clonal population was determined by Western blotting analysis.
Western blotting analysis
Western blotting analysis was conducted as described previously [24]. In brief, A549, SH-SY5Y, COS-7 and HEK 293T cells were washed three times with PBS and lysed with 150 μl of lysis buffer (20 mM Tris, pH 7.4, 150 mM NaCl, 2 mM EDTA, 2 mM EGTA, 1 mM sodium orthovanadate, 50 mM sodium fluoride, 1 % TritonX-100, 0.1 % SDS, and 100 mM phenylmethylsulfonyl fluoride). The lysates were collected in microcentrifuge tubes. Protein concentrations were determined by Bradford method. The lysates were stored at −80 °C. The extracts were mixed with Laemmli sample buffer (2 % SDS) and placed in boiling water for 5 min prior to electrophoresis. Proteins (60 μg protein per sample was used for the Western blot analysis throughout the study) were separated in 10 % SDS–polyacrylamide gels for detecting GFP-ERβ, ERβ, cleaved-PARP, GAPDH, and β-actin, and in 15 % SDS–polyacrylamide gels for detecting Bax (6A7), Bcl-2, Bcl-xl, Bad, cleaved-caspase 3, COX IV, and Histone H3. After electrophoresis, the separated proteins were transferred to PVDF membranes and incubated with primary antibodies against GFP-ERβ (1:500), ERβ (1:500), GAPDH (1:1,000), COX IV (1:1,000), Histone H3 (1:500), Bax (6A7) (1:500), Bcl-2(1:1,000), Bcl-xl (1:1,000), Bad (1:1,000), cleaved-caspase 3 (1:1,000), cleaved-PARP (1:1,000), or β-actin (1:1,000). Bax (6A7). Cleaved-PARP and β-actin were labeled with IRDye® 800CW conjugated goat anti-mouse secondary antibodies (Rockland Immunochemicals, Gilbertsville, PA). GFP-ERβ, ERβ, Bcl-2, Bcl-xl, Bad, cleaved-caspase 3, COX IV, and Histone H3 were labeled with IRDye® 680RD-conjugated goat anti-rabbit secondary antibodies. The fluorescence was quantified with a LI-COR Odyssey Scanning Infrared Fluorescence Imaging System CLx (LI-COR, Inc., Lincoln, NE).
Co-immunoprecipitations (CO-IP)
Mitochondrial lysates (400 μg) or whole-cell lysates (600 μg) were mixed with control IgG or antibodies against Bad or GFP. Then the mixtures were incubated on a rocker at room temperature for 2 h. The immune complexes were captured by the addition of protein G/A-agarose (Roche Applied Sciences, Indianapolis, IN) diluted 1:5 with PBS, followed by incubation at 4 °C overnight. The beads were washed three times with PBS and collected by centrifugation at 12,000 rpm for 1 min. Finally, the beads were resuspended with 100 μl of 5× Laemmli sample buffer, and proteins were detected by Western blotting analysis.
Statistical analysis
All experiments were repeated independently a minimum of three times. Data are represented as mean ± S.E.M. Student t test was used for comparisons involving only two groups. Statistical analyses were performed by ANOVA followed by Student–Newman–Keuls (S–N–K) method for the multiple comparison. Differences were considered statistically significant at p < 0.05. Statistical analyses were performed using SPSS statistics version 13.0 (SPSS Inc, USA).
Results
ERβ was localized to mitochondria
To determine whether ERβ is localized to mitochondria, cells were co-stained with ERβ and Mito Tracker Deep Red 633 followed by fluorescence microscopy analysis. As shown in Fig. 1a, ERβ staining co-localized with Mito Tracker Deep Red 633 in A549, SH-SY5Y, and MCF-7 cells, whereas low levels of ERβ were present in the nucleus. To further confirm the mitochondrial localization of ERβ, mitochondria were isolated from A549, SH-SY5Y, and MCF-7 cells, and Western blotting analysis was performed to identify endogenous ERβ in the mitochondria. As shown in Fig. 1b, c, ERβ staining was predominantly in the mitochondria with faint staining of the nucleus. Next, COS-7 cells lacking endogenous ERβ were used to investigate the localization of overexpressed ERβ. pEGFP-ERβ was co-transfected with DsRed-mit plasmid into COS-7 cells. As shown in Fig. 1d, GFP-ERβ co-localized with DsRed-mit, and GFP-ERβ were not present in the nucleus. To determine if the GFP expression affects the localization of GFP-ERβ, GFP empty vector was co-transfected with DsRed-mit plasmid into COS-7 cells. We found that GFP was distributed throughout the cytosol and nucleus (Fig. 1d). Subcellular fractionation studies were also performed to confirm the presence of GFP-ERβ in the mitochondria. Western blotting analysis showed that GFP-ERβ was present mainly in the mitochondria but not in cytosol or nucleus (Fig. 1e, f). GAPDH, Histone H3, and COX IV served as markers for cytoplasmic, nuclear, and mitochondrial fractions, respectively. Altogether, these results demonstrate that although ERβ is considered a nuclear transcription factor, it also exists in mitochondria in certain cancer cell lines.
ERβ is localized to mitochondria. a Immunofluorescence analysis of mitochondrial ERβ (green emission) in A549, SH-SY5Y, and MCF-7 cells with ERβ specific antibody. Mitochondria were labeled with Mito Tracker Deep Red 633 (red emission), and cytoskeleton was labeled with β-actin antibody (purple). Bar = 10 μm (n = 3). b Western blotting analysis of the expression levels of ERβ in cytosol, nucleus, and mitochondria in A549, SH-SY5Y, and MCF-7 cells. GAPDH, Histone H3, and COXIV served as markers for cytosolic, nuclear, and mitochondrial fractions, respectively. c Quantitative analysis of the expression levels of ERβ in nucleus and mitochondria. (n = 3, *p < 0.05 vs indicated group). d GFP-ERβ and DsRed-mit expression plasmids were co-transfected into COS-7 cells. 48 h later, the mitochondrial (red emission) localization of GFP-ERβ (green emission) was observed by confocal microscopy. Bar = 10 μm (n = 3). e GFP-ERβ and DsRed-mit expression plasmids were co-transfected into COS-7 cells. 48 h later, cytosol, nucleus, and mitochondria were isolated, and the expression levels of GFP-ERβ were detected by Western blotting analysis. f Quantitative analysis of the expression levels of GFP-ERβ in nucleus and mitochondria. (n = 3, *p < 0.05 vs indicated group)
Overexpression of mitochondrial ERβ protected cells against apoptosis induced by different stimuli
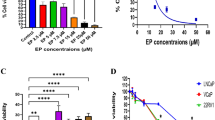
Previous study has reported that ERβ is involved in the mitochondrial functions and cell apoptosis [25], while the molecular mechanisms underlying the functions of mitochondrial ERβ remain unclear. To determine whether mitochondrial ERβ promotes cell survival, we established two GFP-ERβ stable-expressing cell lines (A549 and COS-7 cells) and investigated the effects of overexpressed ERβ on cell viability induced by different apoptotic stimuli. First, the mitochondrial fractions of A549 cells were isolated, and the expression of GFP-ERβ in the mitochondria was determined by Western blotting analysis. As shown in Fig. 2a, we found that GFP-ERβ was highly expressed in mitochondria compared with the control. Subsequently, we investigated if overexpression of ERβ affects cell viability induced by different apoptosis-inducing agents. As shown in Fig. 2b–d, the results showed that cell viability was dramatically reduced in a dose-dependent manner compared with the control. Furthermore, overexpression of ERβ in A549 cells significantly prevented H2O2, UV, and STS induced decrease in cell viability (Fig. 2b–d). These results were confirmed in COS-7 cells (Fig. 2e–h). COX IV served as the loading control. These results suggest that mitochondrial ERβ protects some cancer cells against apoptosis induced by H2O2, UV, and STS.
Overexpression of ERβ prevents cell apoptosis induced by different apoptotic stimuli. a Overexpression of GFP-ERβ in A549 cells was measured by Western blotting analysis. b–d Cell viability of A549 cells treated with different doses of H2O2, UV, and STS was measured by CCK-8 assay. (n = 3, *p < 0.05 vs untreated group; # p < 0.05 vs indicated group). e Overexpression of GFP-ERβ in COS-7 cells was measured by Western blotting analysis. f–h Cell viability of COS-7 cells treated with different doses of H2O2, UV, and STS was measured by CCK-8 assay. (n = 3, *p < 0.05 vs untreated group; # p < 0.05 vs indicated group). i, k Western blotting analysis of cleaved caspase-3 and cleaved PARP in GFP-ERβ overexpressing A549 and COS-7 cells treated with different apoptotic stimuli. j, l Quantitative analysis of the expression levels of activated caspase-3 and cleaved PARP. (n = 3, *p < 0.05 vs control group; # p < 0.05 vs indicated group)
Caspase-3 activation and PARP cleavage are hallmarks of cell apoptosis, so we measured activated caspase-3 and cleaved PARP in A549 and COS-7 cells under different treatments. As shown in Fig. 2i, k, H2O2, UV, and STS exposures resulted in significant activation of caspase-3 and PARP cleavage compared with the control group. Overexpression of GFP-ERβ in A549 cells dramatically suppressed caspase-3 activation and PARP cleavage induced by H2O2, UV, and STS (Fig. 2i, j). Exogenous expression of GFP-ERβ was detected by Western blotting analysis (Fig. 2i). β-actin served as the loading control. Similar results were obtained from COS-7 cells (Fig. 2k, l). Taken together, these results indicate that mitochondrial ERβ exerts an anti-apoptotic role in a ligand-independent manner upon different apoptotic stimuli.
Knockdown of mitochondrial ERβ sensitized cells to different apoptotic stimuli
To investigate if downregulation of mitochondrial ERβ affects cell viability upon different apoptotic stimuli, we established two stable A549 and SH-SY5Y ERβ knockdown cell lines. As shown in Fig. 3a, we found that the expression levels of endogenous ERβ in A549 cells were significantly decreased by ERβ-shRNA compared with the control cells. Subsequently, ERβ knockdown A549 cells were treated with different doses of H2O2, UV, and STS. As shown in Fig. 3b–d, knockdown of ERβ dramatically reduced cell viability in a dose-dependent manner in A549 cells compared with the control cells. The results were confirmed in SH-SY5Y cells (Fig. 3e–h). These data imply that knockdown of mitochondrial ERβ promotes cell apoptosis.
Downregulation of ERβ promotes cell apoptosis induced by different apoptotic stimuli. a Knockdown of endogenous ERβ in A549 cells by ERβ-shRNA was measured by Western blotting analysis. b–d Cell viability of A549 cells treated with different doses of H2O2, UV, and STS was measured by CCK-8 assay. (n = 3, *p < 0.05 vs untreated group; # p < 0.05 vs indicated group). e Knockdown of endogenous ERβ in SH-SY5Y cells by ERβ-shRNA was measured by Western blotting analysis. f–h Cell viability of SH-SY5Y cells treated with different doses of H2O2, UV, and STS was measured by CCK-8 assay. (n = 3, *p < 0.05 vs untreated group; # p < 0.05 vs indicated group). i, k Western blotting analysis of activated caspase-3 and cleaved PARP in ERβ knockdown A549 and SH-SY5Y cells treated with different apoptotic stimuli. j, l: Quantitative analysis of the expression levels of activated caspase-3 and cleaved PARP. (n = 3, *p < 0.05 vs control group; # p < 0.05 vs indicated group)
To further investigate the effects of downregulation of ERβ on cell apoptosis, the activated caspase-3 and cleaved PARP in A549 and SH-SY5Y cells were measured. As shown in Fig. 3 I, H2O2, UV, and STS exposures resulted in significant caspase-3 activation and PARP cleavage compared with the control. Knockdown of ERβ in A549 cells further enhanced caspase-3 activation and PARP cleavage (Fig. 3j). Knockdown of endogenous ERβ was detected by Western blotting analysis (Fig. 3i). β-actin served as the loading control. Similar results were obtained from SH-SY5Y cells (Fig. 3h, l). Taken together, these results demonstrate that knockdown of mitochondrial ERβ promotes cell apoptosis induced by different stimuli, suggesting that mitochondrial ERβ is involved in the mitochondrial apoptotic signaling pathway.
Mitochondrial ERβ modulated the mitochondrial function and integrity through preventing Bax activation and cytochrome c release
Previous study has shown that ERβ regulates mitochondrial gene expression and protects the integrity of mitochondria as a mitochondrial component [26]. However, the molecular mechanisms of how ERβ maintains mitochondrial integrity during cell apoptosis are poorly understood. To investigate whether mitochondrial ERβ is involved in the mitochondrial apoptotic signaling pathway, we isolated the mitochondria and assessed the activation of Bax and the release of cytochrome c in the GFP-ERβ overexpressing A549 and COS-7 cells during cell apoptosis. Western blotting analysis was performed to detect the activation of Bax using 6A7 antibody against activated Bax [27, 28]. As shown in Fig. 4a–c, H2O2, UV, and STS exposures resulted in a significant elevation of Bax in mitochondrial extracts compared with the control. Concomitant with Bax activation, cytochrome c was released from mitochondria. Interestingly, overexpression of GFP-ERβ markedly suppressed Bax activation and cytochrome c release induced by H2O2, UV, and STS (data not shown), suggesting that ERβ may act as a mitochondrial component and protect mitochondria from damage. COX IV served as the loading control. Similar results were obtained from COS-7 cells (Fig. 4d–f).
Mitochondrial ERβ mediates Bax activation and cytochrome c release induced by different apoptotic stimuli. a Western blotting analysis of activated Bax and cytochrome c in A549 cells overexpressing GFP-ERβ under different apoptotic stimuli. b, c Quantitative analysis of the expression levels of activated Bax and cytochrome c from mitochondrial fractions. (n = 3, *p < 0.05 vs indicated group). d Western blotting analysis of activated Bax and cytochrome c in COS-7 cells overexpressing GFP-ERβ under different apoptotic stimuli. e, f Quantitative analysis of the expression levels of activated Bax and cytochrome c from mitochondrial fractions. (n = 3, *p < 0.05 vs indicated group). g Knockdown of endogenous ERβ in A549 cells by ERβ-shRNA was measured by Western blotting analysis. h, i Quantitative analysis of the expression levels of activated Bax and cytochrome c from mitochondrial fractions. (n = 3, *p < 0.05 vs indicated group). j Knockdown of endogenous ERβ in SH-SY5Y cells by ERβ-shRNA was measured by Western blotting analysis. k, l Quantitative analysis of the expression levels of activated Bax and cytochrome c from mitochondrial fractions. (n = 3, *p < 0.05 vs indicated group)
We assumed that ERβ prevents apoptosis by interfering with the mitochondrial signaling pathway, so we investigated if knockdown of endogenous mitochondrial ERβ could promote activation of Bax and induce cytochrome c release during cell apoptosis. As shown in Fig. 4g–i, we found that H2O2, UV, and STS exposures resulted in a significant elevation of activated Bax and release of cytochrome c from mitochondria compared with the control. Furthermore, downregulation of ERβ further enhanced the activation of Bax and release of cytochrome c induced by H2O2, UV, and STS (data not shown). Similar results were obtained from SH-SY5Y cells (Fig. 4 J-K). Altogether, these results indicate that mitochondrial ERβ participates in the mitochondrial apoptotic signaling pathway via suppression of Bax activation and cytochrome c release.
Mitochondrial ERβ interacted with pro-apoptotic protein Bad
Because ERβ knockdown cells showed increased cell apoptosis in response to different stimuli, we further explored whether the expression levels of some Bcl-2 family members were changed in ERβ knockdown cells during apoptosis. As shown in Fig. 5a, no significant change was observed in the expression levels of Bcl-xl, Bax, Bad and Bcl-2.
ERβ was co-immunoprecipitated with pro-apoptotic protein Bad. a Western blotting analysis of different Bcl-2 family members in A549 cells and ERβ-shRNA cells. b Endogenous Bad from mitochondrial fractions was immunoprecipitated with anti-Bad antibody, and Western blotting analysis was performed using anti-ERβ antibody. Similarly, endogenous ERβ from mitochondrial fractions was immunoprecipitated with anti-ERβ antibody, and the Western blotting analysis was performed using anti-Bad antibody. n = 3. COXIV and GAPDH served as the controls for the mitochondrial and cytosolic fractions, respectively. IP, immunoprecipitation. c A549 cells were co-transfected with GFP-ERβ and Flag-Bad expression plasmids. Immunoprecipitation was performed using anti-GFP or anti-Flag antibody. n = 3. d HEK 293T cells were co-transfected with GFP-ERβ and Flag-Bad expression plasmids. Immunoprecipitation was performed using anti-GFP or anti-Flag antibody. n = 3
To investigate if mitochondrial ERβ inhibits cell apoptosis through the interaction with pro-apoptotic mitochondrial proteins, co-immunoprecipitations were performed to determine if ERβ interacts with Bad in A549 cells. As shown in Fig. 5b, endogenous ERβ was co-immunoprecipitated with Bad, but not control IgG in the mitochondrial fraction by a Bad antibody. Similarly, endogenous Bad was co-immunoprecipitated with ERβ, but not control IgG in the mitochondrial fraction by an ERβ antibody.
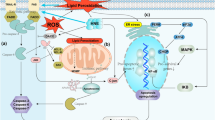
Subsequently, we investigated whether exogenous ERβ and Bad form complexes in A549 cells. GFP-ERβ and Flag-Bad expression plasmids were co-transfected into A549 cells. As shown in Fig. 5c, antibody against the GFP efficiently co-immunoprecipitated with Flag-Bad in the transfected cells. Similarly, antibody against the Flag also efficiently co-immunoprecipitated with GFP-ERβ in the transfected cells. The similar results were obtained from HEK 293T cells cotransfected with GFP-ERβ and Flag-Bad expression plasmids (Fig. 5d). Collectively, these results demonstrate that ERβ inhibits cell apoptosis via the interaction with pro-apoptotic protein Bad and suggest that ERβ indirectly suppresses Bax activation and cytochrome c release via inhibition of Bad (Figure 6).
Discussion
In the current study, we investigated the functions of mitochondrial ERβ during cell apoptosis induced by different stimuli.The results of the study showed that ERβ was localized to the mitochondria in different cancer cells lines, including ERβ-positive MCF-7 breast cancer cells, Overexpression of ERβ significantly suppressed cell apoptosis upon different apoptotic stimuli, and downregulation of ERβ significantly enhanced cell apoptosis, indicating that ERβ exerts its anti-apoptotic functions in a ligand-independent manner. Furthermore, we found that mitochondrial ERβ modulated Bax activation and cytochrome c release during apoptosis. These effects were achieved through the interaction between mitochondrial ERβ and pro-apoptotic protein Bad, which might inhibit Bax translocation to mitochondria and prevent cell apoptosis.
Although ERβ is known as a member of the nuclear receptor superfamily of transcription factors activated by its endogenous ligand E2 in different cell lines and tissues [29, 30], little is known about the subcellular localization of ERβ. Recent studies showed that ERβ is found in the mitochondria in many different cell types, including hippocampal neurons, primary cardiomyocytes, and MCF-7 cells [17, 19]. Consistent with previous studies, we observed that ERβ not only existed in the nucleus, but also presented in the mitochondria in different cancer cells lines. It has also been proven that ERβ is transcriptionally active within the mitochondria, and estrogen-responsive elements (mtEREs), a key regulatory region for mtDNA gene transcription, have been identified in the displacement loop (D-loop) of human mitochondrial DNA (mtDNA) [19, 31]. In addition, previous studies indicate that ERβ could bind to the mtEREs from the MCF-7 and MDA-MB-231 cell mitochondrial extracts [19]. Mitochondrial ERβ is reported to increase the transcript levels of cytochrome c oxidase subunit I (CO I) and CO II encoded by mtDNA [32], promote the activity of the respiratory chain [16], and inhibit cell apoptosis induced by transforming growth factor-β [33]. Furthermore, mitochondrial ERβ has been show to protect mitochondria against oxidative stress through increasing the expression of manganese superoxide dismutase (MnSOD) [34]. These evidences indicate that ERβ serves as a mitochondrial component and protects mitochondrial integrity and functions.
It has been reported that mitochondrial ERs promoted cell survival and prevented cell apoptosis in an estrogen-dependent manner in the breast cancer cells [25]. In our study, physiological functions of mitochondrial ERβ was studied by overexpression and downregulation of the ERβ expression. The results showed that the ERβ was predominantly located in the mitochondria in A549, MCF-7, and SH-SY5Y cells. Moreover, the vast majority of the transfected ERβ also expressed in the mitochondria in COX-7 which lacks endogenous ERβ. Further functional analysis revealed that overexpression of ERβ prevented cell apoptosis, whereas knockdown of ERβ promoted cell apoptosis. These findings indicate that the observed effects on cell apoptosis are largely linked to mitochondrial ERβ. Moreover, mitochondrial ERβ upregulates the activity of MnSOD induced by E2 and prevents ROS formation during UV-mediated cell apoptosis [25]. In the present study, we proposed a model that mitochondrial ERβ regulates cell apoptosis in a ligand-independent manner. The study results showed that overexpression of ERβ significantly enhanced cell survival in a ligand-independent manner in different cell lines, whereas downregulation of ERβ by shRNA dramatically increased cell apoptosis upon apoptotic stimuli. Some studies revealed that ERβ regulates MAPK signaling in a ligand-independent manner in osteoblasts [35], and downregulation of ERβ in murine hippocampal cell leads to a decrease in mitochondrial membrane potential and an increase in the activity of cytochrome c oxidase in the absence of E2 stimulation. Mitochondrial membrane potential collapse is one of the early events in cell apoptosis, and these evidences suggest a key role of mitochondrial ERβ in regulating cell apoptosis in the absence of E2. Collectively, these observations indicate that mitochondrial ERβ regulates apoptosis in both ligand-dependent and ligand-independent manners.
It is well known that mitochondrial apoptotic pathway mediated by Bcl-2 family proteins plays a key role in cell death, while some nuclear proteins with transcription-independent functions can also translocate to mitochondria and induce cell apoptosis. For instance, mitochondrial-localized p53 is reported to interact with Bcl-xl [36] or Bax [37] and induce cell apoptosis. In addition, it has been shown that p53 directly interacts with pro-apoptotic protein Bak, leading to Bak oligomerization at the mitochondrial outer membrane and cytochrome c release from mitochondria [38]. Similarly, the nuclear orphan receptor Nur77/TR3 interacts with anti-apoptotic protein Bcl-2, changes the conformation of Bcl-2, and converts it to a pro-apoptotic protein [39]. In the present study, we identified the anti-apoptotic functions of mitochondrial ERβ in different cancer cell lines. The results showed that mitochondrial ERβ directly interacted with pro-apoptotic protein Bad, which could promote Bax translocation and cytochrome c release. The study data indicate that ERβ acts as a mitochondrial component and protects mitochondrial functions. Although ERβ is localized to the mitochondria in several cell lines, the mitochondrial-localizing signal sequence of ERβ has yet to be identified. Further studies are needed to explore the molecular mechanisms of importing ERβ into mitochondria.
In summary, we demonstrated that mitochondrial ERβ interacts with pro-apoptotic protein Bad, which suppresses Bax activation and cytochrome c release. Our study provides new clues for exploring the molecular mechanisms of mitochondrial ERβ in regulating apoptosis. More importantly, this new insights into mitochondrial ERβ may have implications for finding potential therapeutic targets to induce apoptosis in cancer cells.
References
Nadal-Serrano M, Sastre-Serra J, Pons DG, Miro AM, Oliver J, Roca P (2012) The ERalpha/ERbeta ratio determines oxidative stress in breast cancer cell lines in response to 17beta-estradiol. J Cell Biochem 113:3178–3185
Thomas C, Gustafsson JA (2011) The different roles of ER subtypes in cancer biology and therapy. Nat Rev Cancer 11:597–608
Mangelsdorf DJ, Thummel C, Beato M, Herrlich P, Schutz G, Umesono K, Blumberg B, Kastner P, Mark M, Chambon P, Evans RM (1995) The nuclear receptor superfamily: the second decade. Cell 83:835–839
Chang EC, Charn TH, Park SH, Helferich WG, Komm B, Katzenellenbogen JA, Katzenellenbogen BS (2008) Estrogen Receptors alpha and beta as determinants of gene expression: influence of ligand, dose, and chromatin binding. Mol Endocrinol 22:1032–1043
Le HH, Belcher SM (2010) Rapid signaling actions of environmental estrogens in developing granule cell neurons are mediated by estrogen receptor ss. Endocrinology 151:5689–5699
Tan XJ, Dai YB, Wu WF, Kim HJ, Barros RP, Richardson TI, Yaden BC, Warner M, McKinzie DL, Krishnan V, Gustafsson JA (2012) Reduction of dendritic spines and elevation of GABAergic signaling in the brains of mice treated with an estrogen receptor beta ligand. Proc Natl Acad Sci USA 109:1708–1712
Ascenzi P, Bocedi A, Marino M (2006) Structure-function relationship of estrogen receptor alpha and beta: impact on human health. Mol Aspects Med 27:299–402
Majidi M, Al-Wadei HA, Takahashi T, Schuller HM (2007) Nongenomic beta estrogen receptors enhance beta1 adrenergic signaling induced by the nicotine-derived carcinogen 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone in human small airway epithelial cells. Cancer Res 67:6863–6871
Pandini G, Genua M, Frasca F, Squatrito S, Vigneri R, Belfiore A (2007) 17beta-estradiol up-regulates the insulin-like growth factor receptor through a nongenotropic pathway in prostate cancer cells. Cancer Res 67:8932–8941
Cowley SM, Hoare S, Mosselman S, Parker MG (1997) Estrogen receptors alpha and beta form heterodimers on DNA. J Biol Chem 272:19858–19862
Curtis HS, Couse JF, Korach KS (2000) Estrogen receptor transcription and transactivation: estrogen receptor knockout mice: what their phenotypes reveal about mechanisms of estrogen action. Breast Cancer Res 2:345–352
Lubahn DB, Moyer JS, Golding TS, Couse JF, Korach KS, Smithies O (1993) Alteration of reproductive function but not prenatal sexual development after insertional disruption of the mouse estrogen receptor gene. Proc Natl Acad Sci USA 90:11162–11166
Borras C, Sastre J, Garcia-Sala D, Lloret A, Pallardo FV, Vina J (2003) Mitochondria from females exhibit higher antioxidant gene expression and lower oxidative damage than males. Free Radic Biol Med 34:546–552
Wang X, Simpkins JW, Dykens JA, Cammarata PR (2003) Oxidative damage to human lens epithelial cells in culture: estrogen protection of mitochondrial potential, ATP, and cell viability. Invest Ophthalmol Vis Sci 44:2067–2075
Moats RN, Ramirez VD (1998) Rapid uptake and binding of estradiol-17beta-6-(O-carboxymethyl)oxime:125I-labeled BSA by female rat liver. Biol Reprod 58:531–538
Chen JQ, Yager JD, Russo J (2005) Regulation of mitochondrial respiratory chain structure and function by estrogens/estrogen receptors and potential physiological/pathophysiological implications. Biochim Biophys Acta 1746:1–17
Yang SH, Liu R, Perez EJ, Wen Y, Stevens SJ, Valencia T, Brun-Zinkernagel AM, Prokai L, Will Y, Dykens J, Koulen P, Simpkins JW (2004) Mitochondrial localization of estrogen receptor beta. Proc Natl Acad Sci USA 101:4130–4135
Solakidi S, Psarra AM, Sekeris CE (2005) Differential subcellular distribution of estrogen receptor isoforms: localization of ERalpha in the nucleoli and ERbeta in the mitochondria of human osteosarcoma SaOS-2 and hepatocarcinoma HepG2 cell lines. Biochim Biophys Acta 1745:382–392
Chen JQ, Eshete M, Alworth WL, Yager JD (2004) Binding of MCF-7 cell mitochondrial proteins and recombinant human estrogen receptors alpha and beta to human mitochondrial DNA estrogen response elements. J Cell Biochem 93:358–373
Matsuda K, Nishi M, Takaya H, Kaku N, Kawata M (2008) Intranuclear mobility of estrogen receptor alpha and progesterone receptors in association with nuclear matrix dynamics. J Cell Biochem 103:136–148
Sakamaki J, Daitoku H, Ueno K, Hagiwara A, Yamagata K, Fukamizu A (2011) Arginine methylation of BCL-2 antagonist of cell death (BAD) counteracts its phosphorylation and inactivation by Akt. Proc Natl Acad Sci USA 108:6085–6090
Huang L, Tang Y, Xing D (2013) Activation of nuclear estrogen receptors induced by low-power laser irradiation via PI3-K/Akt signaling cascade. J Cell Physiol 228:1045–1059
Byer SJ, Eckert JM, Brossier NM, Clodfelder-Miller BJ, Turk AN, Carroll AJ, Kappes JC, Zinn KR, Prasain JK, Carroll SL (2011) Tamoxifen inhibits malignant peripheral nerve sheath tumor growth in an estrogen receptor-independent manner. Neuro Oncol 13:28–41
Huang L, Wu S, Xing D (2011) High fluence low-power laser irradiation induces apoptosis via inactivation of Akt/GSK3beta signaling pathway. J Cell Physiol 226:588–601
Pedram A, Razandi M, Wallace DC, Levin ER (2006) Functional estrogen receptors in the mitochondria of breast cancer cells. Mol Biol Cell 17:2125–2137
Yang SH, Sarkar SN, Liu R, Perez EJ, Wang X, Wen Y, Yan LJ, Simpkins JW (2009) Estrogen receptor beta as a mitochondrial vulnerability factor. J Biol Chem 284:9540–9548
Miller AV, Hicks MA, Nakajima W, Richardson AC, Windle JJ, Harada H (2013) Paclitaxel-induced apoptosis is BAK-dependent, but BAX and BIM-independent in breast tumor. PLoS One 8:e60685
Zou H, Volonte D, Galbiati F (2012) Interaction of caveolin-1 with Ku70 inhibits Bax-mediated apoptosis. PLoS One 7:e39379
Andreescu CE, Milojkovic BA, Haasdijk ED, Kramer P, De Jong FH, Krust A, De Zeeuw CI, De Jeu MT (2007) Estradiol improves cerebellar memory formation by activating estrogen receptor beta. J Neurosci 27:10832–10839
Damdimopoulos AE, Spyrou G, Gustafsson JA (2008) Ligands differentially modify the nuclear mobility of estrogen receptors alpha and beta. Endocrinology 149:339–345
Psarra AM, Sekeris CE (2008) Steroid and thyroid hormone receptors in mitochondria. IUBMB Life 60:210–223
Chen JQ, Delannoy M, Cooke C, Yager JD (2004) Mitochondrial localization of ERalpha and ERbeta in human MCF7 cells. Am J Physiol Endocrinol Metab 286:E1011–E1022
Stirone C, Duckles SP, Krause DN, Procaccio V (2005) Estrogen increases mitochondrial efficiency and reduces oxidative stress in cerebral blood vessels. Mol Pharmacol 68:959–965
Robb EL, Stuart JA (2011) Resveratrol interacts with estrogen receptor-beta to inhibit cell replicative growth and enhance stress resistance by upregulating mitochondrial superoxide dismutase. Free Radic Biol Med 50:821–831
Aguirre JI, Plotkin LI, Gortazar AR, Millan MM, O’Brien CA, Manolagas SC, Bellido T (2007) A novel ligand-independent function of the estrogen receptor is essential for osteocyte and osteoblast mechanotransduction. J Biol Chem 282:25501–25508
Xu H, Tai J, Ye H, Kang CB, Yoon HS (2006) The N-terminal domain of tumor suppressor p53 is involved in the molecular interaction with the anti-apoptotic protein Bcl-Xl. Biochem Biophys Res Commun 341:938–944
Chipuk JE, Kuwana T, Bouchier-Hayes L, Droin NM, Newmeyer DD, Schuler M, Green DR (2004) Direct activation of Bax by p53 mediates mitochondrial membrane permeabilization and apoptosis. Science 303:1010–1014
Leu JI, Dumont P, Hafey M, Murphy ME, George DL (2004) Mitochondrial p53 activates Bak and causes disruption of a Bak-Mcl1 complex. Nat Cell Biol 6:443–450
Lin B, Kolluri SK, Lin F, Liu W, Han YH, Cao X, Dawson MI, Reed JC, Zhang XK (2004) Conversion of Bcl-2 from protector to killer by interaction with nuclear orphan receptor Nur77/TR3. Cell 116:527–540
Acknowledgments
The authors thank Dr. Andrew L Wong for excellent technical assistance. They also thank Dr. Steven L. Carroll for kindly providing the ERβ-shRNA construct, and Dr. Ken-Ichi Matsuda and Dr. Akiyoshi Fukamizu for providing the GFP-ERβ and Flag-Bad constructs, respectively.
Conflict of interest
The authors have no financial or personal relationships with other people or organizations that could inappropriately influence their work.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Jiayi Liang and Qiang Xie have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Liang, J., Xie, Q., Li, P. et al. Mitochondrial estrogen receptor β inhibits cell apoptosis via interaction with Bad in a ligand-independent manner. Mol Cell Biochem 401, 71–86 (2015). https://doi.org/10.1007/s11010-014-2293-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-014-2293-y