Abstract
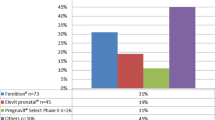
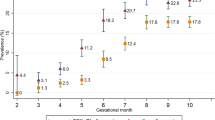
Objective To better understand the knowledge, attitudes and practices of obstetrician-gynecologists with respect to screening and treatment for iron deficiency anemia (IDA). Methods A total of 1,200 Fellows and Junior Fellows of the American College of Obstetricians and Gynecologists were invited to participate in a survey on blood disorders. Respondents completed a questionnaire regarding their patient population, screening and treatment practices for IDA, and general knowledge about IDA and its risk factors. Results Overall response rate was 42.4%. Thirty-eight percent of respondents screen non-pregnant patients regularly, based on risk factors; 30.5% screen only when symptoms of anemia are present. For pregnant patients, 50.0% of respondents screen patients at their initial visit, while 46.2% screen every trimester. Sixty-one percent of respondents supplement pregnant patients when there is laboratory evidence of anemia; 31.6% supplement all pregnant patients. Forty-two percent of respondents screen post-partum patients based on their risk factors for IDA. However, when asked to identify risk factors for post-partum anemia, slightly more than half of respondents correctly identified young age and income level as risk factors for post-partum anemia; only 18.9% correctly identified pre-pregnancy obesity as a risk factor. Conclusion There are opportunities for increased education on IDA for obstetrician-gynecologists, specifically with respect to risk factors. There also appears to be substantial practice variance regarding screening and supplementation for IDA, which may correspond to variability in professional guidelines. Increased education on IDA, especially the importance of sociodemographic factors, and further research and effort to standardize guidelines is needed.
Similar content being viewed by others
References
Albacar, G., Sans, T., Martin-Santos, R., Garcia-Esteve, L., Guillamat, R., Sanjuan, J., et al. (2011). An association between plasma ferritin concentrations measured 48 h after delivery and postpartum depression. Journal of Affective Disorders, 131(1–3), 136–142.
American College of Obstetricians and Gynecologists (2008). ACOG Practice Bulletin No. 95: Anemia in pregnancy. Obstetrics and Gynecology, 112(1):201–207.
Byams, V., Anderson, B., Grant, A., Atresh, H., & Schulkin, J. (2012). Evaluation of bleeding disorders in women with menorrhagia: A survey of obstetrician-gynecologists. American Journal of Obstetrics and Gynecology, 207(4), 269.e1-5.
Centers for Disease Control and Prevention (1998). Recommendations to prevent and control iron deficiency in the United States. MMWR Recommendations and Reports, 47(RR-3):1–29.
Cusick, S. E., Mei, Z., Freedman, D. S., Looker, A. C., Ogden, C. L., Gunter, E., & Cogswell, M. E. (2008). Unexplained decline in the prevalence of anemia among US children and women between 1988–1994 and 1999–2002. The American Journal of Clinical Nutrition, 88(6), 1611–1617.
Drukker, L., Hants, Y., Farkash, R., Ruchlemer, R., Samueloff, A., Grisaru-Granovsky, S. (2015). Iron deficiency anemia at admission for labor and delivery is associated with an increased risk for Cesearean section and adverse maternal and neonatal outcomes. Transfusion, 55(12), 2799–2806.
Institute of Medicine (1993). Iron Deficiency Anemia: Recommended Guidelines for the Prevention, Detection and Management Among U.S. Children and Women of Childbearing Age. Washington D.C.: National Academy Press.
Johnson-Wimbley, T. D., Graham, D. Y. (2011). Diagnosis and management of iron deficiency anemia in the 21st century. Therapeutic Advances in Gastroenterology, 4(3):177–184.
Mei, Z., Cogswell, M. E., Looker, A. C., Pfeiffer, C. M., Cusick, S. E., Lacher, D. A., & Grummer-Strawn, L. M. (2011). Assessment of iron status in U.S. pregnant women from the National Health and Nutrition Examination Study (NHANES) 1999–2006. The American Journal of Clinical Nutrition, 93(6), 1312–1320.
Radlowski, E. C., Johnson, R. W. (2013). Perinatal iron deficiency and neurocognitive development. Frontiers in Human Neuroscience, 7(585):1–11.
Scholl, T. O., Reilly, T. (2000). Anemia, iron and pregnancy outcome. The Journal of Nutrition, 130(2S Suppl), 443S–447S.
Scholl, T. O. (2005). Iron status during pregnancy: Setting the stage for mother and infant. The American Journal of Clinical Nutrition, 81(5), 1218S–1222S.
United States Preventive Services Task Force (2015). Screening for iron deficiency anemia and iron supplementation in pregnant women to improve maternal health and birth outcomes: U.S. Preventive Services Task Force Recommendation Statement. Annals of Internal Medicine, 163(7):529–536.
World Health Organization (2008). Worldwide prevalence of anemia 1993–2005. Geneva: World Health Organization.
World Health Organization (2013). Global health estimates summary tables: DALYs by cause, age and sex. Geneva: World Health Organization.
Acknowledgements
This study is supported by grant UA6MC19010, from the U.S. Department of Health and Human Services, Health Resources and Services Administration, Maternal and Child Health Research Program.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Rights and permissions
About this article
Cite this article
Marcewicz, L.H., Anderson, B.L., Byams, V.R. et al. Screening and Treatment for Iron Deficiency Anemia in Women: Results of a Survey of Obstetrician-Gynecologists. Matern Child Health J 21, 1627–1633 (2017). https://doi.org/10.1007/s10995-016-2252-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-016-2252-1