Abstract
The feasibility and clinical utility of the endotracheal cardiac output monitor (ECOM) to optimize intraoperative hemodynamics and improve short-term outcome in off-pump coronary artery bypass grafting (OPCAB) is unknown. We aimed to compare ECOM with a standard of care in that specific surgical setting. Twenty consecutive adult ECOM-monitored patients undergoing OPCAB were prospectively included (ECOM group) and retrospectively compared to 42 patients scheduled for similar surgery without ECOM monitoring (Control group). The primary endpoint was the global rate of postoperative admission to the intensive care unit (ICU). Secondary endpoints were the time to extubation, the length of stay in ICU and in hospital, the postoperative levels of lactate and troponin and the feasibility of ECOM. The rate of postoperative admission to the ICU was 38/42 (90%) in the Control group versus 11/20 (55%) in the ECOM group, P = 0.008. None unexpected admission for hemodynamic instability was observed in the ECOM group. The time to extubation, the length of stay in ICU, and both troponin level at admission and lactate level at H6 were all significantly decreased in the ECOM group. On a scale ranging from 0 to 5, convenience and satisfaction regarding ECOM were 4.30 ± 1.17 and 3.45 ± 0.68, respectively. The systematic use of ECOM is associated with a significant reduction in the rate of admission to the ICU and an improvement in immediate outcome in OPCAB.

Similar content being viewed by others
References
Kapoor PM, Kakani M, Chowdhury U, Choudhury M, Lakshmy R, Kiran U. Early goal-directed therapy in moderate to high-risk cardiac surgery patients. Ann Card Anaesth. 2008;11:27–34.
Aya HD, Cecconi M, Hamilton M, Rhodes A. Goal-directed therapy in cardiac surgery: a systematic review and meta-analysis. Br J Anaesth. 2013;110:510–7.
Donati A, Loggi S, Preiser J-C, Orsetti G, Munch C, Gabbannelli V, et al. Goal-directed intraoperative therapy reduces morbidity and length of hospital stay in high-risk surgical patients. Chest. 2007;132(6):1817–24.
Grocott MPW, Mythen MG, Gan TJ. Perioperative fluid management and clinical outcomes in adults. Anesth Analg. 2005;100:1093–106.
Hamilton MA, Cecconi M, Rhodes A. A systematic review and meta-analysis on the use of preemptive hemodynamic intervention to improve postoperative outcomes in moderate and high-risk surgical patients. Anesth Analg. 2011;112:1392–402.
Jhanji S, Vivian-Smith A, Lucena-Amaro S, Watson D, Hinds CJ, Pearse RM. Haemodynamic optimisation improves tissue microvascular flow and oxygenation after major surgery: a randomised controlled trial. Crit Care Lond Engl. 2010;14:R151.
Fellahi J-L, Brossier D, Dechanet F, Fischer M-O, Saplacan V, Gerard J-L, et al. Early goal-directed therapy based on endotracheal bioimpedance cardiography: a prospective, randomized controlled study in coronary surgery. J Clin Monit Comput. 2015;29(3):351–8.
Goepfert MS, Richter HP, Zu Eulenburg C, Gruetmacher J, Rafflenbeul E, Roeher K, et al. Individually optimized hemodynamic therapy reduces complications and length of stay in the intensive care unit: a prospective, randomized controlled trial. Anesthesiology. 2013;119(4):824–36.
Pearse R, Dawson D, Fawcett J, Rhodes A, Grounds RM, Bennett ED. Early goal-directed therapy after major surgery reduces complications and duration of hospital stay. A randomised, controlled trial. Crit Care Lond Engl. 2005;9(6):R687–R93.
Huffmyer J, Raphael J. The current status of off-pump coronary bypass surgery. Curr Opin Anaesthesiol. 2011;24:64–9.
Deppe A-C, Arbash W, Kuhn EW, Slottosch I, Scherner M, Liakopoulos O, et al. Current evidence of coronary artery bypass grafting off-pump versus on-pump: a systematic review with meta-analysis of over 16 900 patients investigated in randomized controlled trials. Eur J Cardio-Thorac Surg. 2016;49(4):1031–41.
Chaudhry UAR, Harling L, Sepehripour AH, Stavridis G, Kokotsakis J, Ashrafian H, et al. Beating-heart versus conventional on-pump coronary artery bypass grafting: a meta-analysis of clinical outcomes. Ann Thorac Surg 2015;100:2251–60.
Fellahi J-L, Fischer M-O. Electrical bioimpedance cardiography: an old technology with new hopes for the future. J Cardiothorac Vasc Anesth. 2014;28:755–60.
Ball TR, Culp BC, Patel V, Gloyna DF, Ciceri DP, Culp WC. Comparison of the endotracheal cardiac output monitor to thermodilution in cardiac surgery patients. J Cardiothorac Vasc Anesth. 2010;24:762–6.
Maus TM, Reber B, Banks DA, Berry A, Guerrero E, Manecke GR. Cardiac output determination from endotracheally measured impedance cardiography: clinical evaluation of endotracheal cardiac output monitor. J Cardiothorac Vasc Anesth. 2011;25:770–5.
Fellahi J-L, Fischer M-O, Rebet O, Massetti M, Gérard J-L, Hanouz J-L. A comparison of endotracheal bioimpedance cardiography and transpulmonary thermodilution in cardiac surgery patients. J Cardiothorac Vasc Anesth. 2012;26:217–22.
Fellahi J-L, Fischer M-O, Dalbera A, Massetti M, Gérard J-L, Hanouz J-L. Can endotracheal bioimpedance cardiography assess hemodynamic response to passive leg raising following cardiac surgery? Ann Intensive Care. 2012;2:26.
Møller-Sørensen H, Hansen KL, Østergaard M, Andersen LW, Møller K. Lack of agreement and trending ability of the endotracheal cardiac output monitor compared with thermodilution. Acta Anaesthesiol Scand. 2012;56:433–40.
van der Kleij SCJ, Koolen BB, Newhall DA, Gerritse BM, Rosseel PMJ, Rijpstra TA, et al. Clinical evaluation of a new tracheal impedance cardiography method. Anaesthesia. 2012;67:729–33.
Thonnerieux M, Alexander B, Binet C, Obadia J-F, Bastien O, Desebbe O. The ability of esCCO and ECOM monitors to measure trends in cardiac output during alveolar recruitment maneuver after cardiac surgery: a comparison with the pulmonary thermodilution method. Anesth Analg. 2015;121:383–91.
Wallace AW, Salahieh A, Lawrence A, Spector K, Owens C, Alonso D. Endotracheal cardiac output monitor. Anesthesiology. 2000;92:178–89.
Kapoor PM, Chowdhury U, Mandal B, Kiran U, Karnatak R. Trans-esophageal echocardiography in off-pump coronary artery bypass grafting. Ann Card Anaesth. 2009;12:167.
Kirov MY, Lenkin AI, Kuzkov VV, Suborov EV, Slastilin VY, Borodin VV, et al. Single transpulmonary thermodilution in off-pump coronary artery bypass grafting: haemodynamic changes and effects of different anaesthetic techniques. Acta Anaesthesiol Scand. 2007;51:426–33.
Smetkin AA, Hussain A, Kuzkov VV, Bjertnæs LJ, Kirov MY. Validation of cardiac output monitoring based on uncalibrated pulse contour analysis vs transpulmonary thermodilution during off-pump coronary artery bypass grafting. Br J Anaesth. 2014;112:1024–31.
Acknowledgements
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Funding
Departmental funding only.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Verbal consent was obtained from all individual participants included in the study.
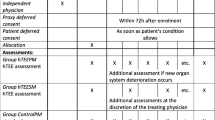
Appendix 1: Scales for feasibility of ECOM in off-pump coronary surgery
Appendix 1: Scales for feasibility of ECOM in off-pump coronary surgery

Rights and permissions
About this article
Cite this article
Leclercq, T., Lilot, M., Schulz, T. et al. Endotracheal bioimpedance cardiography improves immediate postoperative outcome: a case-control study in off-pump coronary surgery. J Clin Monit Comput 32, 81–87 (2018). https://doi.org/10.1007/s10877-017-9996-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-017-9996-z