Abstract
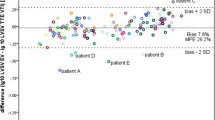
A novel algorithm of impedance cardiography referred to as electrical velocimetry (EV) has been introduced for non-invasive determination of cardiac output (CO). Previous validation studies yielded diverging results and no comparison with the non-invasive gold standard cardiac magnetic resonance imaging (CMR) has been performed. We therefore aimed to prospectively assess the accuracy and reproducibility of EV compared to CMR. 152 consecutive stable patients undergoing CMR were enrolled. EV measurements were taken twice before or after CMR in supine position and averaged over 20 s (AESCULON®, Osypka Medical, Berlin, Germany). Bland–Altman analysis showed insufficient agreement of EV and CMR with a mean bias of 1.2 ± 1.4 l/min (bias 23 ± 26 %, percentage error 51 %). Reproducibility was high with 0.0 ± 0.3 l/min (bias 0 ± 8 %, percentage error 15 %). Outlier analysis revealed gender, height, CO and stroke volume (SV) by CMR as independent predictors for larger variation. Stratification of COCMR in quintiles demonstrated a good agreement for low values (<4.4 l/min) with bias increasing significantly with quintile as high as 3.1 ± 1.1 l/min (p < 0.001). Reproducibility was not affected (p = 0.71). Subgroup analysis in patients with arrhythmias (p = 0.19), changes in thoracic fluid content (p = 0.51) or left heart failure (p = 0.47) could not detect significant differences in accuracy. EV showed insufficient agreement with CMR and good reproducibility. Gender, height and increasing CO and SV were associated with increased bias while not affecting reproducibility. Therefore, absolute values should not be used interchangeably in clinical routine. EV yet may find its place for clinical application with further investigation on its trending ability pending.


Similar content being viewed by others
References
Pohost GM, Hung L, Doyle M. Clinical use of cardiovascular magnetic resonance. Circulation. 2003;108(6):647–53.
Kubicek WG, Karnegis JN, Patterson RP, Witsoe DA, Mattson RH. Development and evaluation of an impedance cardiac output system. Aerosp Med. 1966;37(12):1208–12.
Appel PL, Kram HB, Mackabee J, Fleming AW, Shoemaker WC. Comparison of measurements of cardiac output by bioimpedance and thermodilution in severely ill surgical patients. Crit Care Med. 1986;14(11):933–5.
Franko E, Van De Water J, Wang X. Ideal measurement of cardiac output: is impedance cardiography the answer? Vasc Endovascular Surg. 1991;25:550–8.
Carvalho P, Paiva R, Henriques J, Antunes M, Quintal I, Muehlsteff J. Robust characteristic points for ICG-definition and comparative analysis. Biosignals Rome, Italy; 2011. p. 161–8.
Norozi K, Beck C, Osthaus WA, Wille I, Wessel A, Bertram H. Electrical velocimetry for measuring cardiac output in children with congenital heart disease. Br J Anaesth. 2008;100(1):88–94.
Osthaus WA, Huber D, Beck C, Winterhalter M, Boethig D, Wessel A, Sumpelmann R. Comparison of electrical velocimetry and transpulmonary thermodilution for measuring cardiac output in piglets. Paediatr Anaesth. 2007;17(8):749–55.
Schmidt C, Theilmeier G, Van Aken H, Korsmeier P, Wirtz SP, Berendes E, Hoffmeier A, Meissner A. Comparison of electrical velocimetry and transoesophageal Doppler echocardiography for measuring stroke volume and cardiac output. Br J Anaesth. 2005;95(5):603–10.
Suttner S, Schollhorn T, Boldt J, Mayer J, Rohm KD, Lang K, Piper SN. Noninvasive assessment of cardiac output using thoracic electrical bioimpedance in hemodynamically stable and unstable patients after cardiac surgery: a comparison with pulmonary artery thermodilution. Intensive Care Med. 2006;32(12):2053–8.
Tomaske M, Knirsch W, Kretschmar O, Woitzek K, Balmer C, Schmitz A, Bauersfeld U, Weiss M. Cardiac output measurement in children: comparison of Aesculon cardiac output monitor and thermodilution. Br J Anaesth. 2008;100(4):517–20.
Zoremba N, Bickenbach J, Krauss B, Rossaint R, Kuhlen R, Schalte G. Comparison of electrical velocimetry and thermodilution techniques for the measurement of cardiac output. Acta Anaesthesiol Scand. 2007;51(10):1314–9.
Raue W, Swierzy M, Koplin G, Schwenk W. Comparison of electrical velocimetry and transthoracic thermodilution technique for cardiac output assessment in critically ill patients. Eur J Anaesthesiol. 2009;26(12):1067–71.
Petter H, Erik A, Bjorn E, Goran R. Measurement of cardiac output with non-invasive Aesculon impedance versus thermodilution. Clin Physiol Funct Imaging. 2011;31(1):39–47.
Heringlake M, Handke U, Hanke T, Eberhardt F, Schumacher J, Gehring H, Heinze H. Lack of agreement between thermodilution and electrical velocimetry cardiac output measurements. Intensive Care Med. 2007;33(12):2168–72.
Tomaske M, Knirsch W, Kretschmar O, Balmer C, Woitzek K, Schmitz A, Bauersfeld U, Weiss M. Evaluation of the Aesculon cardiac output monitor by subxiphoidal Doppler flow measurement in children with congenital heart defects. Eur J Anaesthesiol. 2009;26(5):412–5.
Trinkmann F, Berger M, Hoffmann U, Borggrefe M, Kaden JJ, Saur J. A comparative evaluation of electrical velocimetry and inert gas rebreathing for the non-invasive assessment of cardiac output. Clin Res Cardiol. 2011;100(10):935–43.
Grollmuss O, Demontoux S, Capderou A, Serraf A, Belli E. Electrical velocimetry as a tool for measuring cardiac output in small infants after heart surgery. Intensive Care Med. 2012;38(6):1032–9.
Bernstein D, Osypka M. Apparatus and method for determining an approximation of the stroke volume and the cardiac output of the heart. US Patent 6,511,438 B2; 2003.
Papavassiliu T, Kuhl HP, Schroder M, Suselbeck T, Bondarenko O, Bohm CK, Beek A, Hofman MM, van Rossum AC. Effect of endocardial trabeculae on left ventricular measurements and measurement reproducibility at cardiovascular MR imaging. Radiology. 2005;236(1):57–64.
Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet. 1986;1(8476):307–10.
Critchley LA, Critchley JA. A meta-analysis of studies using bias and precision statistics to compare cardiac output measurement techniques. J Clin Monit Comput. 1999;15(2):85–91.
Woltjer HH, Bogaard HJ, van der Spoel HI, de Vries PM. The influence of weight on stroke volume determination by means of impedance cardiography in cardiac surgery patients. Intensive Care Med. 1996;22(8):766–71.
Hoetink AE, Faes TJ, Schuur EH, Gorkink R, Goovaerts HG, Meijer JH, Heethaar RM. Comparing spot electrode arrangements for electric impedance cardiography. Physiol Meas. 2002;23(2):457–67.
Tan KH, Lai FO, Hwang NC. Measurement of cardiac output using Physio Flow with different positions of electrode placement. Singapore Med J. 2006;47(11):967–70.
Dhingra VK, Fenwick JC, Walley KR, Chittock DR, Ronco JJ. Lack of agreement between thermodilution and fick cardiac output in critically ill patients. Chest. 2002;122(3):990–7.
van Grondelle A, Ditchey RV, Groves BM, Wagner WW Jr, Reeves JT. Thermodilution method overestimates low cardiac output in humans. Am J Physiol. 1983;245(4):H690–2.
Stetz CW, Miller RG, Kelly GE, Raffin TA. Reliability of the thermodilution method in the determination of cardiac output in clinical practice. Am Rev Respir Dis. 1982;126(6):1001–4.
Saur J, Fluechter S, Trinkmann F, Papavassiliu T, Schoenberg S, Weissmann J, Haghi D, Borggrefe M, Kaden JJ. Noninvasive determination of cardiac output by the inert-gas-rebreathing method—comparison with cardiovascular magnetic resonance imaging. Cardiology. 2009;114(4):247–54.
Trinkmann F, Sampels M, Doesch C, Papavassiliu T, Brade J, Schmid-Bindert G, Hoffmann U, Borggrefe M, Kaden JJ, Saur J. Is arterial pulse contour analysis using Nexfin a new option in the noninvasive measurement of cardiac output?—A pilot study. J Cardiothorac Vasc Anesth. 2013;27(2):283–7.
Trinkmann F, Doesch C, Papavassiliu T, Weissmann J, Haghi D, Gruettner J, Schoenberg SO, Borggrefe M, Kaden JJ, Saur J. A novel noninvasive ultrasonic cardiac output monitor: comparison with cardiac magnetic resonance. Clin Cardiol. 2010;33(2):E8–14.
Tan HL, Pinder M, Parsons R, Roberts B, van Heerden PV. Clinical evaluation of USCOM ultrasonic cardiac output monitor in cardiac surgical patients in intensive care unit. Br J Anaesth. 2005;94(3):287–91.
Williams BO, Caird FI. Accuracy of the impedance cardiogram in the measurement of cardiac output in the elderly. Age Ageing. 1985;14(5):277–81.
Berman IR, Scheetz WL, Jenkins EB, Hufnagel HV. Transthoracic electrical impedance s a guide to intravascular overload. Arch Surg. 1971;102(1):61–4.
Penney BC. Theory and cardiac applications of electrical impedance measurements. Crit Rev Biomed Eng. 1986;13(3):227–81.
Pomerantz M, Delgado F, Eiseman B. Clinical evaluation of transthoracic electrical impedance as a guide to intrathoracic fluid volumes. Ann Surg. 1970;171(5):686–94.
Saur J, Trinkmann F, Doesch C, Weissmann J, Hamm K, Schoenberg SO, Borggrefe M, Haghi D, Kaden JJ. Non-invasive measurement of cardiac output during atrial fibrillation: comparison between cardiac magnetic resonance imaging and inert gas rebreathing. Cardiology. 2010;115(3):212–6.
Tang WH, Tong W. Measuring impedance in congestive heart failure: current options and clinical applications. Am Heart J. 2009;157(3):402–11.
Voss F, Becker R, Hauck M, Katus HA, Bauer A. The basic pacing rate in CRT patients: the higher the better? Clin Res Cardiol. 2009;98(4):219–23.
Tonelli AR, Alkukhun L, Arelli V, Ramos J, Newman J, McCarthy K, Pichurko B, Minai OA, Dweik RA. Value of impedance cardiography during 6-minute walk test in pulmonary hypertension. Clin Transl Sci. 2013;6(6):474–80.
Lee WT, Brown A, Peacock AJ, Johnson MK. Use of non-invasive haemodynamic measurements to detect treatment response in precapillary pulmonary hypertension. Thorax. 2011;66(9):810–4.
Flinck M, Graden A, Milde H, Flinck A, Hellstrom M, Bjork J, Nyman U. Cardiac output measured by electrical velocimetry in the CT suite correlates with coronary artery enhancement: a feasibility study. Acta Radiol. 2010;51(8):895–902.
Liu Y, Pian-Smith MC, Leffert LR, Minehart RD, Torri A, Cote C, Kacmarek RM, Jiang Y. Continuous measurement of cardiac output with the electrical velocimetry method in patients under spinal anesthesia for cesarean delivery. J Clin Monit Comput. 2014. doi:10.1007/s10877-014-9645-8.
Kupersztych-Hagege E, Teboul JL, Artigas A, Talbot A, Sabatier C, Richard C, Monnet X. Bioreactance is not reliable for estimating cardiac output and the effects of passive leg raising in critically ill patients. Br J Anaesth. 2013;111(6):961–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical statement
The study protocol was approved by the institutional Ethics Committee and conducted in accordance with the Declaration of Helsinki. Informed consent was obtained from all participants.
Rights and permissions
About this article
Cite this article
Trinkmann, F., Berger, M., Doesch, C. et al. Comparison of electrical velocimetry and cardiac magnetic resonance imaging for the non-invasive determination of cardiac output. J Clin Monit Comput 30, 399–408 (2016). https://doi.org/10.1007/s10877-015-9731-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-015-9731-6