Abstract
Introduction
Robotically guided radiofrequency (RF) ablation offers greater catheter stability that may improve lesion depth. We performed a non-randomised comparison of patients undergoing ventricular tachycardia (VT) ablation either manually or robotically using the Hansen Sensei system for recurrent implantable defibrillator (ICD) therapy.
Methods
Patients with infarct-related scar underwent VT ablation using the Hansen system to assess feasibility compared with patients undergoing manual VT ablation during a similar time period. Power delivery during robotic ablation was restricted to 30 W at 60 s. VT inducibility was checked at the end of the procedure. Pre-ablation ICD therapy burdens over 6 months were compared with post-ablation therapy averaged to a 6-month period.
Results
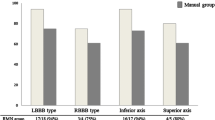
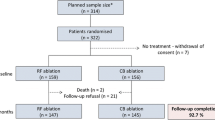
Twelve consecutive patients who underwent robotic VT ablation were compared to 12 consecutive patients undergoing a manual ablation. Patient demographics and comorbidities were similar in the two groups. A higher proportion of robotic cases were urgent (9/12 (75 %)) vs. manual (4/12 (33 %)) (p = 0.1). Post-ablation VT stimulation did not induce clinical VT in 11/12 (92 %) in each group. There were no peri-procedural complications related to ablation delivery. Patients were followed up for approximately 2 years. Averaged over 6 months, robotic ICD therapy burdens fell from 32 (5–400) events to 2.5 (0–11) (p = 0.015). Therapy burden fell from 14 (10–25) to 1 (0–5) (p = 0.023) in the manual group. There was no difference in long-term outcome (p = 0.60) and mortality (4/12 (33 %), p = 1.0).
Conclusion
Robotically guided VT ablation is both feasible and safe when compared to manual ablation with good acute and long-term outcomes.



Similar content being viewed by others
References
Schron, E. B., Exner, D. V., Yao, Q., Jenkins, L. S., Steinberg, J. S., Cook, J. R., Kutalek, S. P., Friedman, P. L., Bubien, R. S., Page, R. L., & Powell, J. (2002). Quality of life in the antiarrhythmics versus implantable defibrillators trial: impact of therapy and influence of adverse symptoms and defibrillator shocks. Circulation, 105, 589–594.
Poole, J. E., Johnson, G. W., Hellkamp, A. S., Anderson, J., Callans, D. J., Raitt, M. H., Reddy, R. K., Marchlinski, F. E., Yee, R., Guarnieri, T., Talajic, M., Wilber, D. J., Fishbein, D. P., Packer, D. L., Mark, D. B., Lee, K. L., & Bardy, G. H. (2008). Prognostic importance of defibrillator shocks in patients with heart failure. The New England Journal of Medicine, 359, 1009–1017.
Gonska, D.-B., Cao, K., Schaumann, A., Dorszewski, A., von zur Muhlen, F., & Kreuzer, H. (1994). Catheter ablation of ventricular tachycardia in 136 patients with coronary artery disease: results and long-term follow-up. Journal of the American College of Cardiology, 24, 1506–1514.
Dinov, B., Fiedler, L., Schönbauer, R., Bollmann, A., Rolf, S., Piorkowski, C., Hindricks, G., & Arya, A. (2014). Outcomes in catheter ablation of ventricular tachycardia in dilated nonischemic cardiomyopathy compared with ischemic cardiomyopathy: results from the Prospective Heart Centre of Leipzig VT (HELP-VT) Study. Circulation, 129(7), 728–736.
Kuck, K. H., Schaumann, A., Eckardt, L., Willems, S., Ventura, R., Delacrétaz, E., Pitschner, H. F., Kautzner, J., Schumacher, B., Hansen, P. S., & VTACH study group. (2010). Catheter ablation of stable ventricular tachycardia before defibrillator implantation in patients with coronary heart disease (VTACH): a multicentre randomized controlled trial. Lancet, 375, 31–40.
Kanagaratnam, P., Koa-Wing, M., Wallace, D. T., Goldenberg, A. S., Peters, N. S., & Davies, D. W. (2008). Experience of robotic catheter ablation in humans using a novel remotely steerable catheter sheath. Journal of Interventional Cardiac Electrophysiology, 21(1), 19–26.
Okumura, Y., Johnson, S. B., Bunch, T. J., Henz, B. D., O’Brien, C. J., & Packer, D. L. (2008). A systematical analysis of in vivo contact forces on virtual catheter tip/tissue surface contact during cardiac mapping and intervention. Journal of Cardiovascular Electrophysiology, 19, 632–640.
Koa-Wing, M., Kojodjojo, P., Malcolme-Lawes, L. C., Salukhe, T. V., Linton, N. W., Grogan, A. P., Bergman, D., Lim, P. B., Whinnett, Z. I., McCarthy, K., Ho, S. Y., O’Neill, M. D., Peters, N. S., Davies, D. W., & Kanagaratnam, P. (2009). Robotically assisted ablation produces more rapid and greater signal attenuation than manual ablation. Journal of Cardiovascular Electrophysiology, 20, 1398–1404.
Malcolme-Lawes, L. C., Lim, P. B., Koa-Wing, M., Whinnett, Z. I., Jamil-Copley, S., Hayat, S., Francis, D. P., Kojodjojo, P., Davies, D. W., Peters, N. S., & Kanagaratnam, P. (2013). Robotic assistance and general anaesthesia improve catheter stability and increase signal attenuation during atrial fibrillation ablation. Europace, 15(1), 41–47.
Wazni, O. M., Barrett, C., Martin, D. O., Shaheen, M., Tarakji, K., Baranowski, B., Hussein, A., Callahan, T., Dresing, T., Bhargava, M., Kanj, M., Tchou, P., Natale, A., & Saliba, W. (2009). Experience with the Hansen robotic system for atrial fibrillation ablation—lessons learned and techniques modified: Hansen in the real world. Journal of Cardiovascular Electrophysiology, 20, 1193–1196.
Di Biase, L., Wang, Y., Horton, R., Gallinghouse, G. J., Mohanty, P., Sanchez, J., Patel, D., Dare, M., Canby, R., Price, L. D., Zagrodzky, J. D., Bailey, S., Burkhardt, J. D., & Natale, A. (2009). Ablation of atrial fibrillation utilizing robotic catheter navigation in comparison to manual navigation and ablation: single-centre experience. Journal of Cardiovascular Electrophysiology, 20(12), 1328–1335.
Hlivak, P., Mlcochova, H., Peichl, P., Cihak, R., Witchterle, D., & Kautzner, J. (2011). Robotic navigation in catheter ablation for paroxysmal atrial fibrillation: midterm efficacy and predictors of postablation arrhythmia recurrence. Journal of Cardiovascular Electrophysiology, 22(5), 534–540.
Steven, D., Rostock, T., Servatius, H., Hoffmann, B., Drewitz, I., Müllerleile, K., Meinertz, T., & Willems, S. (2008). Robotic versus conventional ablation for common-type atrial flutter: a prospective randomized trial to evaluate the effectiveness of remote catheter navigation. Heart Rhythm, 5, 1556–1560.
Lorgat, F., Pudney, E., & van Deventer, H. (2013). Robotically assisted ventricular tachycardia substrate modification ablation with the novel Lynx(TM) integrated sheath and RF ablation catheter. Cardiovascular Journal of Africa, 24(3), e9–e11.
Duncan, E., Johns, N., Schilling, R. J., & Sporton, S. (2011). Robotic catheter navigation within the left ventricle. Pacing and Clinical Electrophysiology, 34(11), 102–104.
Koa-Wing, M., Linton, N. W., Kojodjojo, P., O’Neill, M. D., Peters, N. S., Wyn Davies, D., & Kanagaratnam, P. (2009). Robotic catheter ablation of ventricular tachycardia in a patient with congenital heart disease and Rastelli repair. Journal of Cardiovascular Electrophysiology, 20, 1163–1166.
Valderrábano, M., Dave, A. S., Báez-Escudero, J. L., & Rami, T. (2011). Robotic catheter ablation of ventricular tachycardia: initial experience. Heart Rhythm, 8, 1837–1846.
Wright, I. J., Kojodjojo, P., Jamil-Copley, S., Davies, D. W., Stanbridge, R. D., & Kanagaratnam, P. (2013). Sustained tachycardia in a cardiac resynchronization therapy recipient: what is the mechanism of tachycardia? Pacing and Clinical Electrophysiology, 36(11), 1427–1430.
Tung, R., Mathuria, N., Michowitz, Y., Yu, R., Buch, E., Bradfield, J., Mandapati, R., Wiener, I., Boyle, N., & Shivkumar, K. (2012). Functional pace-mapping responses for identification of targets for catheter ablation of scar-mediated ventricular tachycardia. Circulation. Arrhythmia and Electrophysiology, 5(2), 264–272.
Tilz, R. R., Makimoto, H., Lin, T., Rillig, A., Deiss, S., Wissner, E., Mathew, S., Metzner, A., Rausch, P., Kuck, K. H., & Ouyang, F. (2014). Electrical isolation of substrate after myocardial infarction: a novel ablation strategy for unmappable ventricular tachycardias: feasibility and clinical outcome. Europace, 16, 1041–1053.
Vergara, P., Trevisi, N., Ricco, A., Petracca, F., Baratto, F., Cireddu, M., Bisceglia, C., Maccabelli, G., & Della Bella, P. J. (2012). Late potentials abolition as an additional technique for reduction of arrhythmia recurrence in scar related ventricular tachycardia ablation. Journal of Cardiovascular Electrophysiology, 23(6), 621–627.
Soejima, K., Suzuki, M., Maisel, W. H., Brunckhorst, C. B., Delacretaz, E., Blier, L., Tung, S., Khan, H., & Stevenson, W. G. (2001). Catheter ablation in patients with multiple and unstable ventricular tachycardias after myocardial infarction: short ablation lines guided by reentry circuit isthmuses and sinus rhythm mapping. Circulation, 104, 664–669.
Di Biase, L., Natale, A., Barrett, C., Tan, C., Elayi, C. S., Ching, C. K., Wang, P., Al-Ahmad, A., Arruda, M., Burkhardt, J. D., Wisnoskey, B. J., Chowdhury, P., De Marco, S., Armaganijan, L., Litwak, K. N., Schweikert, R. A., & Cummings, J. E. (2009). Relationship between catheter forces, lesion characteristics, ‘popping’, and char formation: experience with robotic navigation system. Journal of Cardiovascular Electrophysiology, 20, 436–440.
El-Damaty, A., & Sapp, J. L. (2011). The role of catheter ablation for ventricular tachycardia in patients with ischemic heart disease. Current Opinion in Cardiology, 26(1), 30–39.
Yokokawa, M., Desjardins, B., Crawford, T., Good, E., Morady, F., & Bogun, F. (2013). Reasons for recurrent ventricular tachycardia after catheter ablation of post-infarction ventricular tachycardia. Journal of the American College of Cardiology, 61(1), 66–73.
Stevenson, W. G., Wilber, D. J., Natale, A., Jackman, W. M., Marchlinski, F. E., Talbert, T., Gonzalez, M. D., Worley, S. J., Daoud, E. G., Hwang, C., Schuger, C., Bump, T. E., Jazayeri, M., Tomassoni, G. F., Kopelman, H. A., Soejima, K., Nakagawa, H., & Multicenter Thermocool VT Ablation Trial Investigators. (2008). Irrigated radiofrequency catheter ablation guided by electroanatomic mapping for recurrent ventricular tachycardia after myocardial infarction: the multicenter thermocool ventricular tachycardia ablation trial. Circulation, 118, 2773–2782.
Tanner, H., Hindricks, G., Volkmer, M., Furniss, S., Kuhlkamp, V., Lacroix, D., DE Chillou, C., Almendral, J., Caponi, D., Kuck, K. H., & Kottkamp, H. (2010). Catheter ablation of recurrent scar-related ventricular tachycardia using electroanatomical mapping and irrigated ablation technology: results of the prospective multicenter Euro-VT-Study. Journal of Cardiovascular Electrophysiology, 21, 47–53.
Financial support
This study has been performed independently by the authors listed at Imperial College Healthcare NHS Trust, London, UK. Dr Vishal Luther is funded by a British Heart Foundation Clinical Research Training Fellowship Award (no. FS/15/12/31239). Dr Shahnaz Jamil-Copley is funded by grant PG/10/37/28347 from the British Heart Foundation. We acknowledge the ElectroCardioMaths Programme of the British Heart Foundation Centre of Research Excellence, Programme Grant RG/10/11/28457, and the National Institute for Health Research Biomedical Research Centre. Dr D. Wyn Davies has received consulting fees and research grants from Hansen Medical. Dr Prapa Kanagaratnam has received consulting fees and research grants from Hansen Medical and Biosense Webster.
Authors contributions
VL contributed data analysis/interpretation, statistics and drafting article. SJC contributed data analysis/interpretation, statistics and drafting article and is joint first author. MKW contributed data analysis/interpretation and drafting article. MSS contributed data analysis/interpretation and statistics. IJW, NWL, PBL, ZW, SH, DL, NSP and DWD contributed data collection and approval of article. PK contributed concept/design, critical revision of article and approval of article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Luther, V., Jamil-Copley, S., Koa-Wing, M. et al. Non-randomised comparison of acute and long-term outcomes of robotic versus manual ventricular tachycardia ablation in a single centre ischemic cohort. J Interv Card Electrophysiol 43, 175–185 (2015). https://doi.org/10.1007/s10840-015-9992-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-015-9992-5