Abstract
Objective
The objective of this study was to determine the effect of alcohol consumption on outcomes among women undergoing in vitro fertilization (IVF).
Design
This study is a retrospective cohort study.
Setting
This study was performed in a private academically affiliated IVF center.
Patients
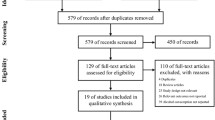
Patients included women presenting for their first IVF cycle from July 2004 through October 2012.
Intervention
Women completed self-administered questionnaires before their first IVF cycle, which included report of usual alcohol consumption. Women were categorized as non-drinkers, social drinkers, or daily drinkers, as well as by the number of drinks consumed per week. Competing risks analysis was used to calculate the cumulative incidence of live birth after 6 cycles stratified by alcohol consumption.
Main outcome measures
Main outcome measures included spontaneous abortion, clinical pregnancy, and live birth following IVF.
Results
There were 591 (27.7%) non-drinkers, 1466 (68.7%) social drinkers, and 77 (3.6%) daily drinkers (total n = 2134). In the first cycle, compared to non-drinkers, daily drinkers had a twofold increased risk of spontaneous abortion (adjusted risk ratio [aRR] 2.2; 95% confidence interval [CI] 1.1–4.5) among all cycle starts, and while their risk of live birth was 30% lower (aRR 0.7; 95% CI 0.4–1.3), the sample size was small, and it was not significantly lower. By the end of 6 cycles, social drinkers and daily drinkers did not differ from non-drinkers in their cumulative incidence of live birth (56.1, 50.6, and 52.1%, respectively; both P ≥ 0.28).
Conclusion
There was a trend towards lower risk of live birth among daily drinkers. Daily drinkers had an increased risk of spontaneous abortion in the first cycle, but the number of daily drinkers was small.

Similar content being viewed by others
References
Larkby C, Day N. The effects of prenatal alcohol exposure. Alcohol Health Res World. 1997;21(3):192–8.
Mutsaerts MA, Groen H, Huiting HG, Kuchenbecker WK, Sauer PJ, Land JA, Stolk RP, Hoek A. The influence of maternal and paternal factors on time to pregnancy—a Dutch population-based birth-cohort study: the GECKO Drenthe study. Hum Reprod. 2012;27(2):583–93.
Hakim RB, Gray RH, Zacur H. Alcohol and caffeine consumption and decreased fertility. Fertil Steril. 1998;70(4):632–7.
Rasch V. Cigarette, alcohol, and caffeine consumption: risk factors for spontaneous abortion. Acta Obstet Gynecol Scand. 2003;82(2):182–8.
Gill J. The effects of moderate alcohol consumption on female hormone levels and reproductive function. Alcohol Alcohol. 2000;35(5):417–23.
Li Y, Lin H, Li Y, Cao J. Association between socio-psycho-behavioral factors and male semen quality: systematic review and meta-analyses. Fertil Steril. 2011;95(1):116–23.
Gaur DS, Talekar MS, Pathak VP. Alcohol intake and cigarette smoking: impact of two major lifestyle factors on male fertility. Indian J Pathol Microbiol. 2010;53(1):35–40.
Klonoff-Cohen H, Lam-Kruglick P, Gonzalez C. Effects of maternal and paternal alcohol consumption on the success rates of in vitro fertilization and gamete intrafallopian transfer. Fertil Steril. 2003;79(2):330–9.
Rossi BV, Berry KF, Hornstein MD, Cramer DW, Ehrlich S, Missmer SA. Effect of alcohol consumption on in vitro fertilization. Obstet Gynecol. 2011;117(1):136–42.
Eaton JL, Hacker MR, Harris D, Thornton KL, Penzias AS. Assessment of day-3 morphology and euploidy for individual chromosomes in embryos that develop to the blastocyst stage. Fertil Steril. 2009;91(6):2432–6.
American Society for Reproductive Medicine Practice Committee Documents. Criteria for number of embryos to transfer: a committee opinion. Fertil Steril. 2013;99(1):44–6.
Malizia BA, Hacker MR, Penzias AS. Cumulative live-birth rates after in vitro fertilization. N Engl J Med. 2009;360(3):236–43.
Fine J, Gray R. A proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc. 1999;94(446):496–509.
Luke B, Brown MB, Wantman E, Lederman A, Gibbons W, Schattman GL, Lobo RA, Leach RE, Stern JE. Cumulative birth rates with linked assisted reproductive technology cycles. N Engl J Med. 2012;366(26):2483–91.
Pepe MS, Mori M. Kaplan-Meier, marginal or conditional probability curves in summarizing competing risks failure time data? Stat Med. 1993;12(8):737–51.
Cavallo F, Russo R, Zotti C, Camerlengo A, Ruggenini AM. Moderate alcohol consumption and spontaneous abortion. Alcohol Alcohol. 1995;30(2):195–201.
Eggert J, Theobald H, Engfeldt P. Effects of alcohol consumption on female fertility during an 18-year period. Fertil Steril. 2004;81(2):379–83.
Gaskins AJ, Rich-Edwards JW, Williams PL, Toth TL, Missmer SA, Chavarro JE. Prepregnancy low to moderate alcohol intake is not associated with risk of spontaneous abortion or stillbirth. J Nutr. 2016.
Parazzini F, Tozzi L, Chatenoud L, Restelli S, Luchini L, La VC. Alcohol and risk of spontaneous abortion. Hum Reprod. 1994;9(10):1950–3.
Tolstrup JS, Kjaer SK, Munk C, Madsen LB, Ottesen B, Bergholt T, Gronbaek M. Does caffeine and alcohol intake before pregnancy predict the occurrence of spontaneous abortion? Hum Reprod. 2003;18(12):2704–10.
American Society for Reproductive Medicine. Assisted reproductive technologies: a guide for patients 2016 [cited 2016 Jun 9].
Del Boca FK, Darkes J. The validity of self-reports of alcohol consumption: state of the science and challenges for research. Addiction. 2003;98(Suppl 2):1–12.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The institutional review board at Beth Israel Deaconess Medical Center approved this study (#2015P-000047).
Funding
This work was supported by the National Institute of Environmental Health Sciences training grant T32 ES 07069 and the National Institute of Child Health and Development Contraception and Infertility Research Loan Repayment Program, which both supported LED.
Electronic supplementary material
ESM 1
(DOCX 11 kb)
Rights and permissions
About this article
Cite this article
Dodge, L.E., Missmer, S.A., Thornton, K.L. et al. Women’s alcohol consumption and cumulative incidence of live birth following in vitro fertilization. J Assist Reprod Genet 34, 877–883 (2017). https://doi.org/10.1007/s10815-017-0923-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-017-0923-5