Abstract
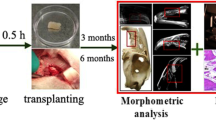
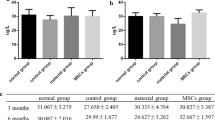
Tissue engineering strategies hold great potential for alveolar cleft reconstruction. Bone marrow stromal cells (BMSCs) from iliac crest and craniofacial regions are candidate seeding cells with site-specific characteristics and bone-repairing properties. Craniofacial BMSCs seem to possess stronger multipotency and osteogenic capabilities than BMSCs isolated from iliac crest. However, the angiogenic capabilities of these two type cell is rarely reported. We obtained human BMSCs (hBMSCs) of maxilla (M-hBMSCs) and iliac crest (I-hBMSCs) from same alveolar cleft patients to investigate the agiogenic variations using co-culture system with human umbilical vein endothelial cells (HUVECs). From in vitro comparison, M-hBMSCs allowed HUVECs to form more tube-like structures and sprouting angiogenesis by tube formation assays and 3D fibrin vasculogenic assay, respectively. By transplantation in vivo, M-hBMSCs enhanced larger size vessel like structures distributed the entire implants compared with I-hBMSCs. Western blotting was used to assess the angiogenesis related factors including hepatocyte growth factor (HGF), vascular endothelial growth factor (VEGF) and basic fibroblast growth factor (bFGF). The results showed a significant higher expression of bFGF protein in M-hBMSCs and HUVECs co-culture system both in vitro and in vivo. As bFGF could promote migration and proliferation of endothelial cells, scratch wound healing and transwell migration assays were performed as well as MTT assays and cell cycle analysis. The data suggested the effect of M-hBMSCs on HUVECs was stronger than I-hBMSCs. Taken together, these results indicated that craniofacial BMSCs seemed to have greater angiogenesis capability than iliac crest BMSCs and this might be associated with the different levels of bFGF protein expression in co-culture system.







Similar content being viewed by others
References
Aghaloo TL, Chaichanasakul T, Bezouglaia O, Kang B, Franco R, Dry SM, Atti E, Tetradis S (2010) Osteogenic potential of mandibular vs. long-bone marrow stromal cells. J Dent Res 89(11):1293–1298. doi:10.1177/0022034510378427
Akintoye SO, Lam T, Shi S, Brahim J, Collins MT, Robey PG (2006) Skeletal site-specific characterization of orofacial and iliac crest human bone marrow stromal cells in same individuals. Bone 38(6):758–768. doi:10.1016/j.bone.2005.10.027
Akintoye SO, Giavis P, Stefanik D, Levin L, Mante FK (2008) Comparative osteogenesis of maxilla and iliac crest human bone marrow stromal cells attached to oxidized titanium: a pilot study. Clin Oral Implants Res 19(11):1197–1201. doi:10.1111/j.1600-0501.2008.01592.x
Alard JE, Dueymes M, Mageed RA, Saraux A, Youinou P, Jamin C (2009) Mitochondrial heat shock protein (HSP) 70 synergizes with HSP60 in transducing endothelial cell apoptosis induced by anti-HSP60 autoantibody. FASEB J 23(8):2772–2779. doi:10.1096/fj.08-128785
Aronson J (1994) Temporal and spatial increases in blood flow during distraction osteogenesis. Clin Orthop Relat Res 301:124–131
Au P, Tam J, Fukumura D, Jain RK (2008) Bone marrow-derived mesenchymal stem cells facilitate engineering of long-lasting functional vasculature. Blood 111(9):4551–4558. doi:10.1182/blood-2007-10-118273
Beck L Jr, D’Amore PA (1997) Vascular development: cellular and molecular regulation. FASEB J 11(5):365–373
Carmeliet P, Jain RK (2011) Molecular mechanisms and clinical applications of angiogenesis. Nature 473(7347):298–307. doi:10.1038/nature10144
Chai Y, Jiang X, Ito Y, Bringas P Jr, Han J, Rowitch DH, Soriano P, McMahon AP, Sucov HM (2000) Fate of the mammalian cranial neural crest during tooth and mandibular morphogenesis. Development 127(8):1671–1679
Chaichanasakul T, Kang B, Bezouglaia O, Aghaloo TL, Tetradis S (2014) Diverse osteoclastogenesis of bone marrow from mandible versus long bone. J Periodontol 85(6):829–836. doi:10.1902/jop.2013.130376
Chim SM, Qin A, Tickner J, Pavlos N, Davey T, Wang H, Guo Y, Zeng MH, Xu J (2011) EGFL6 promotes endothelial cell migration and angiogenesis through the activation of extracellular signal-regulated kinase. J Biol Chem 286(25):22035–22046. doi:10.1074/jbc.M110.187633
Covas DT, Panepucci RA, Fontes AM, Silva WA Jr, Orellana MD, Freitas MC, Neder L, Santos AR, Peres LC, Jamur MC, Zago MA (2008) Multipotent mesenchymal stromal cells obtained from diverse human tissues share functional properties and gene-expression profile with CD146+ perivascular cells and fibroblasts. Exp Hematol 36(5):642–654. doi:10.1016/j.exphem.2007.12.015
Crisan M, Yap S, Casteilla L, Chen CW, Corselli M, Park TS, Andriolo G, Sun B, Zheng B, Zhang L, Norotte C, Peault B (2008) A perivascular origin for mesenchymal stem cells in multiple human organs. Cell Stem Cell 3(3):301–313. doi:10.1016/j.stem.2008.07.003
Dai L, Zhu J, Mao M, Li Y, Deng Y, Wang Y, Liang J, Tang L, Wang H, Kilfoy BA, Zheng T (2010) Time trends in oral clefts in Chinese newborns: data from the Chinese National Birth Defects Monitoring Network. Birth Defects Res A Clin Mol Teratol 88(1):41–47. doi:10.1002/bdra.20607
Davis GE, Stratman AN, Sacharidou A, Koh W (2011) Molecular basis for endothelial lumen formation and tubulogenesis during vasculogenesis and angiogenic sprouting. Int Rev Cell Mol Biol 288:101–165. doi:10.1016/B978-0-12-386041-5.00003-0
Deshpande SS, Gallagher KK, Donneys A, Tchanque-Fossuo CN, Sarhaddi D, Sun H, Krebsbach PH, Buchman SR (2013) Stem cell therapy remediates reconstruction of the craniofacial skeleton after radiation therapy. Stem Cells Dev 22(11):1625–1632. doi:10.1089/scd.2012.0472
Dilling CF, Wada AM, Lazard ZW, Salisbury EA, Gannon FH, Vadakkan TJ, Gao L, Hirschi K, Dickinson ME, Davis AR, Olmsted-Davis EA (2010) Vessel formation is induced prior to the appearance of cartilage in BMP-2-mediated heterotopic ossification. J Bone Miner Res 25(5):1147–1156. doi:10.1359/jbmr.091031
Dixon MJ, Marazita ML, Beaty TH, Murray JC (2011) Cleft lip and palate: understanding genetic and environmental influences. Nat Rev Genet 12(3):167–178. doi:10.1038/nrg2933
Dong W, Ge J, Zhang P, Fu Y, Zhang Z, Cheng J, Jiang H (2014) Phenotypic characterization of craniofacial bone marrow stromal cells: unique properties of enhanced osteogenesis, cell recruitment, autophagy, and apoptosis resistance. Cell Tissue Res 358(1):165–175. doi:10.1007/s00441-014-1927-4
Dong W, Zhang P, Fu Y, Ge J, Cheng J, Yuan H, Jiang H (2015) Roles of SATB2 in site-specific stemness, autophagy and senescence of bone marrow mesenchymal stem cells. J Cell Physiol 230(3):680–690. doi:10.1002/jcp.24792
Ghajar CM, Blevins KS, Hughes CC, George SC, Putnam AJ (2006) Mesenchymal stem cells enhance angiogenesis in mechanically viable prevascularized tissues via early matrix metalloproteinase upregulation. Tissue Eng 12(10):2875–2888. doi:10.1089/ten.2006.12.2875
Gnecchi M, Zhang Z, Ni A, Dzau VJ (2008) Paracrine mechanisms in adult stem cell signaling and therapy. Circ Res 103(11):1204–1219. doi:10.1161/circresaha.108.176826
Grainger SJ, Carrion B, Ceccarelli J, Putnam AJ (2013) Stromal cell identity influences the in vivo functionality of engineered capillary networks formed by co-delivery of endothelial cells and stromal cells. Tissue Eng Part A 19(9–10):1209–1222. doi:10.1089/ten.TEA.2012.0281
Hsiao ST, Asgari A, Lokmic Z, Sinclair R, Dusting GJ, Lim SY, Dilley RJ (2012) Comparative analysis of paracrine factor expression in human adult mesenchymal stem cells derived from bone marrow, adipose, and dermal tissue. Stem Cells Dev 21(12):2189–2203. doi:10.1089/scd.2011.0674
Janssen NG, Weijs WL, Koole R, Rosenberg AJ, Meijer GJ (2014) Tissue engineering strategies for alveolar cleft reconstruction: a systematic review of the literature. Clin Oral Investig 18(1):219–226. doi:10.1007/s00784-013-0947-x
Jiang F, Ma J, Liang Y, Niu Y, Chen N, Shen M (2015) Amniotic mesenchymal stem cells can enhance angiogenic capacity via MMPs in vitro and in vivo. Biomed Res Int 2015:324014. doi:10.1155/2015/324014
Kachgal S, Putnam AJ (2011) Mesenchymal stem cells from adipose and bone marrow promote angiogenesis via distinct cytokine and protease expression mechanisms. Angiogenesis 14(1):47–59. doi:10.1007/s10456-010-9194-9
Kaigler D, Pagni G, Park C-H, Tarle SA, Bartel RL, Giannobile WV (2010) Angiogenic and osteogenic potential of bone repair cells for craniofacial regeneration. Tissue Eng Part A 16(9):2809–2820. doi:10.1089/ten.tea.2010.0079
Koole R (1994) Ectomesenchymal mandibular symphysis bone graft: an improvement in alveolar cleft grafting? Cleft Palate Craniofac J 31(3):217–223. doi:10.1597/1545-1569(1994)031<0217:EMSBGA>2.3.CO;2
Koole R, Bosker H, van der Dussen FN (1989) Late secondary autogenous bone grafting in cleft patients comparing mandibular (ectomesenchymal) and iliac crest (mesenchymal) grafts. J Craniomaxillofac Surg 17(Suppl 1):28–30
Leucht P, Kim JB, Amasha R, James AW, Girod S, Helms JA (2008) Embryonic origin and Hox status determine progenitor cell fate during adult bone regeneration. Development 135(17):2845–2854. doi:10.1242/dev.023788
Li Q, Wang Z (2013) Influence of mesenchymal stem cells with endothelial progenitor cells in co-culture on osteogenesis and angiogenesis: an in vitro study. Arch Med Res 44(7):504–513. doi:10.1016/j.arcmed.2013.09.009
Lin CS, Lue TF (2013) Defining vascular stem cells. Stem Cells Dev 22(7):1018–1026. doi:10.1089/scd.2012.0504
Lin RZ, Moreno-Luna R, Zhou B, Pu WT, Melero-Martin JM (2012) Equal modulation of endothelial cell function by four distinct tissue-specific mesenchymal stem cells. Angiogenesis 15(3):443–455. doi:10.1007/s10456-012-9272-2
Ma J, Yang F, Both SK, Prins HJ, Helder MN, Pan J, Cui FZ, Jansen JA, van den Beucken JJ (2014) In vitro and in vivo angiogenic capacity of BM-MSCs/HUVECs and AT-MSCs/HUVECs cocultures. Biofabrication 6(1):015005. doi:10.1088/1758-5082/6/1/015005
Makanya AN, Hlushchuk R, Djonov VG (2009) Intussusceptive angiogenesis and its role in vascular morphogenesis, patterning, and remodeling. Angiogenesis 12(2):113–123. doi:10.1007/s10456-009-9129-5
Matsubara T, Suardita K, Ishii M, Sugiyama M, Igarashi A, Oda R, Nishimura M, Saito M, Nakagawa K, Yamanaka K, Kato Y (2004) Alveolar bone marrow as a cell source for regenerative medicine: differences between alveolar and iliac bone marrow stromal cells. J Bone Miner Res 20(3):399–409. doi:10.1359/jbmr.041117
Matsubara H, Hogan DE, Morgan EF, Mortlock DP, Einhorn TA, Gerstenfeld LC (2012) Vascular tissues are a primary source of BMP2 expression during bone formation induced by distraction osteogenesis. Bone 51(1):168–180. doi:10.1016/j.bone.2012.02.017
Mikoya T, Inoue N, Matsuzawa Y, Totsuka Y, Kajii TS, Hirosawa T (2010) Monocortical mandibular bone grafting for reconstruction of alveolar cleft. Cleft Palate Craniofac J 47(5):454–468. doi:10.1597/09-172
Osyczka AM, Damek-Poprawa M, Wojtowicz A, Akintoye SO (2009) Age and skeletal sites affect BMP-2 responsiveness of human bone marrow stromal cells. Connect Tissue Res 50(4):270–277. doi:10.1080/03008200902846262
Picchi J, Trombi L, Spugnesi L, Barachini S, Maroni G, Brodano GB, Boriani S, Valtieri M, Petrini M, Magli MC (2013) HOX and TALE signatures specify human stromal stem cell populations from different sources. J Cell Physiol 228(4):879–889. doi:10.1002/jcp.24239
Roubelakis MG, Tsaknakis G, Pappa KI, Anagnou NP, Watt SM (2013) Spindle shaped human mesenchymal stem/stromal cells from amniotic fluid promote neovascularization. PLoS ONE 8(1):e54747. doi:10.1371/journal.pone.0054747
Sacchetti B, Funari A, Michienzi S, Di Cesare S, Piersanti S, Saggio I, Tagliafico E, Ferrari S, Robey PG, Riminucci M, Bianco P (2007) Self-renewing osteoprogenitors in bone marrow sinusoids can organize a hematopoietic microenvironment. Cell 131(2):324–336. doi:10.1016/j.cell.2007.08.025
Schaaf H, Lendeckel S, Howaldt HP, Streckbein P (2010) Donor site morbidity after bone harvesting from the anterior iliac crest. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 109(1):52–58. doi:10.1016/j.tripleo.2009.08.023
Seghezzi G, Patel S, Ren CJ, Gualandris A, Pintucci G, Robbins ES, Shapiro RL, Galloway AC, Rifkin DB, Mignatti P (1998) Fibroblast growth factor-2 (FGF-2) induces vascular endothelial growth factor (VEGF) expression in the endothelial cells of forming capillaries: an autocrine mechanism contributing to angiogenesis. J Cell Biol 141(7):1659–1673
Sindet-Pedersen S, Enemark H (1990) Reconstruction of alveolar clefts with mandibular or iliac crest bone grafts: a comparative study. J Oral Maxillofac Surg 48(6):554–558 (discussion 559–560)
Smith AO, Bowers SL, Stratman AN, Davis GE (2013) Hematopoietic stem cell cytokines and fibroblast growth factor-2 stimulate human endothelial cell-pericyte tube co-assembly in 3D fibrin matrices under serum-free defined conditions. PLoS ONE 8(12):e85147. doi:10.1371/journal.pone.0085147
Stefanik D, Sarin J, Lam T, Levin L, Leboy PS, Akintoye SO (2008) Disparate osteogenic response of mandible and iliac crest bone marrow stromal cells to pamidronate. Oral Dis 14(5):465–471
Street J, Bao M, deGuzman L, Bunting S, Peale FV Jr, Ferrara N, Steinmetz H, Hoeffel J, Cleland JL, Daugherty A, van Bruggen N, Filvaroff EH (2002) Vascular endothelial growth factor stimulates bone repair by promoting angiogenesis and bone turnover. Proc Natl Acad Sci USA 99(15):9656–9661. doi:10.1073/pnas.152324099
Wang KC, Helms JA, Chang HY (2009) Regeneration, repair and remembering identity: the three Rs of Hox gene expression. Trends Cell Biol 19(6):268–275. doi:10.1016/j.tcb.2009.03.007
Watt SM, Athanassopoulos A, Harris AL, Tsaknakis G (2010) Human endothelial stem/progenitor cells, angiogenic factors and vascular repair. J R Soc Interface 7(Suppl 6):S731–S751. doi:10.1098/rsif.2010.0377.focus
Watt SM, Gullo F, van der Garde M, Markeson D, Camicia R, Khoo CP, Zwaginga JJ (2013) The angiogenic properties of mesenchymal stem/stromal cells and their therapeutic potential. Br Med Bull 108:25–53. doi:10.1093/bmb/ldt031
Zhang P, Men J, Fu Y, Shan T, Ye J, Wu Y, Tao Z, Liu L, Jiang H (2012) Contribution of SATB2 to the stronger osteogenic potential of bone marrow stromal cells from craniofacial bones. Cell Tissue Res 350(3):425–437. doi:10.1007/s00441-012-1487-4
Acknowledgments
This study was supported in part by the National Basic Research Program of China (2012CB966902), the National Natural Science Foundation of China (81271109), The Project Funded by the Priority Academic Program Development of Jiangsu Higher Education Institutions (PAPD, 2014-37) and The Project Funded by Jiangsua Provincial Commission of Health and Family Planning (Z201511).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interests
The authors declare that there is no conflict of interests regarding the publication of this paper.
Additional information
Yifei Du and Fei Jiang have contributed equal to this work.
Rights and permissions
About this article
Cite this article
Du, Y., Jiang, F., Liang, Y. et al. The angiogenic variation of skeletal site-specific human BMSCs from same alveolar cleft patients: a comparative study. J Mol Hist 47, 153–168 (2016). https://doi.org/10.1007/s10735-016-9662-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10735-016-9662-7