Abstract
This document, from the International Society for Clinical Electrophysiology of Vision (ISCEV), presents an updated and revised ISCEV Standard for full-field clinical electroretinography (ffERG or simply ERG). The parameters for Standard flash stimuli have been revised to accommodate a variety of light sources including gas discharge lamps and light emitting diodes. This ISCEV Standard for clinical ERGs specifies six responses based on the adaptation state of the eye and the flash strength: (1) Dark-adapted 0.01 ERG (rod ERG); (2) Dark-adapted 3 ERG (combined rod-cone standard flash ERG); (3) Dark-adapted 3 oscillatory potentials; (4) Dark-adapted 10 ERG (strong flash ERG); (5) Light-adapted 3 ERG (standard flash “cone” ERG); and (6) Light-adapted 30 Hz flicker ERG. ISCEV encourages the use of additional ERG protocols for testing beyond this minimum standard for clinical ERGs.
Similar content being viewed by others
Introduction
The full-field electroretinogram (ERG) is a widely used electrophysiologic test of retinal function. In 1989, ISCEV standardised basic clinical ERG protocols so that comparable ERGs could be recorded throughout the world [1]. Because of advances in knowledge and techniques, this ISCEV Standard is reviewed regularly. This document supersedes the 2008 version [2]. In this revision, the sources and spectral composition of flash stimuli and of the light-adapting background light are redefined to include stimuli generated by light emitting diodes (LEDs) or other sources. This change formally recognizes the widespread current use of LED stimuli, while retaining the option of stimulation with xenon gas discharge lamps within the Standard for all ERG stimuli. This updated standard includes CIE coordinates for the stimuli and definitions of both the photopic and scotopic strength of the standard stimuli.
The defined ISCEV Standard ERG series includes six protocols. These are named according to the stimulus (flash strength in cd·s·m−2) and the state of adaptation.
-
1.
Dark-adapted 0.01 ERG (a rod-driven response of on bipolar cells).
-
2.
Dark-adapted 3 ERG (combined responses arising from photoreceptors and bipolar cells of both the rod and cone systems; rod dominated).
-
3.
Dark-adapted 10 ERG (combined response with enhanced a-waves reflecting photoreceptor function).
-
4.
Dark-adapted oscillatory potentials (responses primarily from amacrine cells).
-
5.
Light-adapted 3 ERG (responses of the cone system; a-waves arise from cone photoreceptors and cone Off- bipolar cells; the b-wave comes from On- and Off-cone bipolar cells).
-
6.
Light-adapted 30 Hz flicker ERG (a sensitive cone-pathway-driven response).
This ISCEV Standard describes basic procedures that allow reproducible recordings that are comparable across laboratories. Standard ERG tests can be selected as indicated for specific patients. In the absence of sufficient clinical information or expertise to guide selective testing, it is recommended that all six Standard ERGs be recorded. It is intended that ISCEV Standard ERG protocols be used widely, but not to the exclusion of other tests or protocols that are not covered by this Standard. Electrophysiologists are encouraged to extend test protocols as required when clinically relevant to maximize the diagnostic value of the ERG for their patients and for clinical trials. “Appendix” lists additional ERG tests that are widely used in clinical electrophysiology laboratories.
ISCEV publishes and maintains other Standards for clinical electrophysiologic testing: specifically, multifocal ERGs [3], pattern ERGs [4], electro-oculograms [5] and visual evoked potential [6] as well as technical and calibration guidelines for clinical electrodiagnostic testing [7]. The ISCEV website should be consulted for current updates (www.ISCEV.org/standards). ISCEV recommends that commercial recording equipment has the capability of allowing extended protocols to accommodate comprehensive and specialist testing in addition to the Standard ERG protocols. This document is not a safety standard, and it does not mandate particular procedures for individual patients or define the qualifications of those administering or interpreting the tests.
Basic technology
Electrodes
Recording electrodes
Electrodes that contact the cornea, bulbar conjunctiva or skin on the lower eyelid are used as active electrodes connected to the positive input for recording ISCEV Standard full-field ERGs. These include contact lens electrodes, conductive fibers and foils, conjunctival wire loops, corneal wicks and skin electrodes. Contact lens electrodes provide the highest amplitude and most stable recordings; such electrodes should be centrally transparent with an optical opening as large as possible and typically incorporate a device to hold the lids apart. The corneal surface should be protected during use with a non-irritating and non-allergenic ionic conductive solution (i.e., contact lens wetting solutions or artificial tears containing sodium chloride and no more viscous than 0.5 % methyl cellulose). Topical anesthesia is necessary for contact lens electrodes but may not be required for other types of corneal and conjunctival electrodes. The ERG signal amplitude is lower with non-contact lens electrodes. For ERGs recorded with the active electrode on the lower eyelid near the eye, signal averaging may be required to obtain reliable responses in typical eyes. Skin electrodes on the lower eyelid may not be suitable to evaluate attenuated pathological ERGs. Those recording ERGs must master the technical requirements of their chosen electrode to obtain good contact, consistent electrode positioning, acceptable electrode impedance and to ensure that waveforms are comparable to those of ISCEV Standard ERGs. Reference amplitude ranges for standard ERGs are electrode specific. Re-scaling data for different types of electrode is acceptable for occasional cases but should not be used routinely in place of electrode-specific data.
Reference electrodes
Reference electrodes (those connected to the negative input of the recording system) may be incorporated into the contact lens-speculum assembly in contact with the conjunctiva. These “bipolar electrodes” are the most electrically stable configuration although “monopolar” contact lens electrodes with a separate reference generally produce larger amplitudes. Alternatively, skin electrodes placed near each orbital rim, temporal to the eye are used as the reference electrode for the corresponding eye. Avoid placing reference electrodes over muscle masses (to minimize electromyogram interference). Other reference positions deviate from this standard.
Common electrode
A separate electrode should be attached to an indifferent point and connected to the common input of the recording system. Typical locations are on earlobe, mastoid or the forehead.
Skin electrode characteristics
The impedance of the skin electrodes measured between 10 and 100 Hz should normally be 5 kΩ or less [7]. Ideally, the recording and reference electrodes should have similar impedance levels. For skin electrodes, the skin should be prepared by cleaning, and a suitable conductive paste or gel (if not integral to the electrode) applied to ensure good electrical connections.
Electrode stability
In the absence of light stimulation and eye movement, the baseline voltage should be stable. Reference electrodes may need to be non-polarizable to achieve this stability.
Electrode cleaning
Recording ERGs involves the exposure of corneal electrodes to tears, and there is potential exposure of skin electrodes to blood if there is any break in the surface of the skin. Electrodes (if not disposable) must be suitably cleaned and sterilized after each use to prevent transmission of infectious agents. The cleaning protocol should follow manufacturers’ recommendations and meet current local standards for devices that contact skin and tears.
Stimulation
Light diffusion
Full-field (ganzfeld) stimulation must be used to provide uniform luminance over the entire visual field of the test subject. This is usually achieved using a dome or integrating sphere. A fixation spot should be provided, and stimulators should allow observation of the eye to monitor fixation. It is incumbent on manufacturers and users of to verify that stimulation meets the full-field requirement of this standard.
Stimulus duration
This ISCEV Standard is based on flash stimuli with durations that are shorter than the integration time of any photoreceptor. The maximum acceptable duration of any stimulus flash is 5 ms.
Stimulus wavelength
To achieve standardized retinal stimulation, the spectrum of stimulus flashes must take account of the different spectral sensitivity of rods and cones. Standard flash and background are defined as visibly white, with CIE co-ordinates near x = 0.31, y = 0.32 (Note 1). Both photopic and scotopic luminance levels are specified for each stimulus, although the established convention of naming the stimulus according to its photopic luminance has been retained in this standard. It is important to comply with scotopic levels for rod-dominated ERGs (i.e., dark-adapted conditions).
Colored filters or colored LEDs can be used to enhance the separation of rod and cone ERGs, but these are not part of the ISCEV Standard ERG (Note 2).
Stimulus strength
Flash stimuli are quantified by their time-integrated luminance as measured at the position of the eye (Note 3). This is a measurement of luminous energy per unit solid angle (steradian) per unit area. The units are candela-seconds per meter squared (cd·s·m−2). Stimulus strengths falling within the ranges specified in Table 1 are compliant with the ISCEV Standard.
The flash stimuli and light-adapting background used for the ISCEV Standard ERGs described below are as follows:
-
The weak flash stimulus strength is 0.010 photopic cd·s·m−2 with a scotopic strength of 0.025 scotopic cd·s·m−2.
-
The standard flash stimulus is 3.0 photopic cd·s·m−2 with a scotopic strength of 7.5 scotopic cd·s·m−2.
-
The standard strong flash stimulus is 10 photopic cd·s·m−2 with a scotopic strength of 25 scotopic cd·s·m−2.
-
Light-adapting and background luminance is 30 photopic cd m−2 with a scotopic strength of 75 scotopic cd m−2.
Nomenclature
Stimulus (and response) names are described by the state of light adaptation and the flash strength in photopic cd·s·m−2 with the understanding that the strength in scotopic cd·s·m−2 will be 2.5 times higher. For example, the dark-adapted response to 3.0 cd·s·m−2 is called the “Dark-adapted 3 ERG.” In addition, descriptive terms (such as “rod response,” “mixed rod-cone response,” etc.) may be used where there is no ambiguity. This scheme of naming should also apply to non-standard stimuli, used in extended protocols or because of equipment limitations (e.g., if flashes of 15 cd·s·m−2 are used under dark-adapted conditions they should be specified as a “Dark-adapted 15 ERG.”).
Adjustment of stimulus strength and background luminance: Methods for modifying both the stimulus and background are required. Stimulation systems should be capable of producing flashes over a range of at least 3 log units in strength in steps of not more than 0.3 log unit. Changing stimulus strength or background luminance should not change the spectral composition of either the flash or background light. The stimulus and background requirements for a range of other ERG tests will be more extensive, and ISCEV recommends that equipment manufacturers exceed this minimum standard.
Stimulus and background calibration
The user or manufacturer must document the strength of each flash stimulus based on measurements made with an integrating photometer capable of recording the total output of very brief flashes and placed at the location of the eye. The photometer must meet international standards for photometric measurements and have appropriate filters for measurements based on both the photopic and scotopic luminous efficiency functions (luminosity curves). For stroboscopic stimulators that use discharge lamps, light output per flash may vary with the flash repetition rate; therefore, separate calibrations may be needed for single flash and for rapidly flickering stimuli. For LED stimulators, output does not vary significantly with repetition rate. The background luminance is calibrated at the position of the eye with a photometer in non-integrating mode. Users may consult the current ISCEV technical guidelines for details [7]. Manufacturers of stimulators should supply or specify a suitable photometer and/or devices to verify the calibrations of their equipment.
Stimulus and background light output may change over time due to aging or other changes in light sources, in power supplies, attenuation systems or in the reflectance or transmission of the ganzfeld dome. Responsibility for electronic stability and warnings about sources of instability rests with the manufacturers of the equipment; responsibility for checking the calibration rests with users. The frequency with which the calibration of flashes and backgrounds should be verified varies from system to system. Correct calibration can only be assumed between periods of stable measurements.
Electronic recording equipment
Patient isolation
The patient should be electrically isolated according to current standards for safety of clinical biologic recording systems in the user’s country. In the absence of more stringent national requirements, the equipment should meet the specifications defined in the general standard for Medical Electrical Equipment IEC 60601-1.
Input characteristics
The recording system should have a minimum input impedance of 10 MΩ (preferably much higher) and be capable of handling the large steady offset voltages that may be introduced by the electrodes. Ideally, the recording system will allow the electrodes to be connected using shielded cables.
Frequency bandwidth and sampling
The system should record frequencies that include at least the range from 0.3 to 300 Hz. To avoid a loss of information, ERGs should be digitized at a rate of 1 kHz or higher in each channel after appropriate anti-aliasing filtering. The digitizer should have an effective resolution of 1 μV or less.
Other filtering
The recording system should be capable of filtering the ERG signals for such purposes as extracting oscillatory potentials either prior to recording them or on replay. The band pass for ISCEV Standard ERG recordings, except the oscillatory potentials, is broad. The corner frequencies (3 dB attenuation) are specified as ranging from <0.3 to >300 Hz. Roll-off characteristics of the filters are not standardized by ISCEV, but users should be aware that any changes to the filter characteristics or corner frequency of either the high- or low-pass filters will change the amplitude and peak times of ERGs. Ideally, comparisons between ERGs should be made with signals filtered in exactly the same way or using post hoc corrections for differences in filter characteristics.
“Notch filters” that remove a relatively narrow band of frequencies have sometimes been used to improve the appearance of records marred by pickup of mains or other periodic interfering signals. Such filters distort the waveform and should not be used. Post hoc methods are more suitable for removing interference of this kind.
Real-time ERG display
It is important that ERG waveforms are displayed during testing so that the operator can continuously monitor stability and make adjustments during the test procedure if necessary.
Calibration/recalibration of recording equipment
The basic timing of the stimulating and recording equipment is set by the system clocks and these should be accurate to within ±0.01 %. The voltage to digital conversion of the recorded signals should be accurate to ±2 %. These characteristics should initially be guaranteed by the manufacturer of the equipment and are unlikely to change unless there is an electronic fault. As such faults may not be immediately obvious, the timing and voltage sensitivity should be checked from time to time according to the advice of the manufacturer.
Storing ERG data
Digital records of all ERGs should be stored. Whenever possible, these should be records of individual ERG waveforms rather than averages only, which may be distorted by artifact. The duration of each stored record should be at least 300 ms (including a pre-stimulus baseline of 50 ms) to facilitate post hoc removal of interference although shorter traces may be displayed in reports. Each Standard ERG should be replicated at least once, and each replication should be stored.
Averaging
Averaging is not normally required to record quantifiable ERGs with standard ERG electrodes in typical eyes. However, averaging a small number of ERGs reduces variability and background noise and facilitates the estimation of variability. Averaging may be essential to identify and measure pathologic ERGs of low amplitude. Artifact rejection must be a part of any averaging system.
Clinical protocol
Preparation of the patient
Pupillary dilatation
The pupils should be maximally dilated, and the pupil size noted before and at the end of recording the ERGs in this ISCEV Standard.
Pre-adaptation to light or dark
The recording conditions outlined below specify 20 min of dark adaptation before recording dark-adapted ERGs, and 10 min of light adaptation before recording light-adapted ERGs. The choice of whether to begin with dark-adapted or light-adapted conditions is up to the user, provided these adaptation requirements are met. Following dark adaptation, weak flashes should be presented before stronger flash stimuli to minimize the effects of partial light adaptation from exposure to flashes during the testing sequence. If contact lens electrodes are used, the wearing time can be minimized by dark-adapting before inserting the electrodes under dim red light at the end of the adaptation period. Care should be used to avoid strong red light, and a brief period of additional dark adaptation, approximately 5 min, is recommended for recovery after lens insertion.
Pre-exposure to light
Fluorescein angiography, fundus photography and other imaging techniques using strong illumination systems should be avoided directly before ERG testing. If these examinations have been performed, we recommend least 30-min recovery time in ordinary room illumination before beginning ERG testing.
Fixation
Patients should be instructed to look at a fixation point incorporated into the stimulus dome. A stable gaze is important so that eye movements do not alter the position of the electrode on the eye, produce electrical artifacts, or allow blockage of light by the electrode or eyelid. Fixation points should not interfere with dark adaptation (e.g., a weak red LED with a wavelength of 625 nm or longer for dark-adapted recordings) and should be visible in light-adapted conditions (e.g., by adjustment to a stronger fixation light or by using a dark fixation spot). Patients who cannot see the fixation target may be instructed to look straight ahead and keep their eyes steady. Patients should be monitored to assess compliance and any difficulties in eye opening or fixation should be noted.
Dark-adapted 0.01 ERG (rod-system response)
Dark-adapt the patient for a minimum of 20 min (longer if the patient had been exposed to unusually bright light) before recording dark-adapted ERG. The Dark-adapted 0.01 ERG is normally the first signal to be measured after dark adaptation, since it is the most affected by light adaptation. The stimulus is a weak white flash of 0.010 photopic cd·s·m−2 with a scotopic strength of 0.025 scotopic cd·s·m−2. The minimum interval between flashes is 2 s.
Dark-adapted 3 ERG (combined rod and cone system responses)
The Dark-adapted 3 ERG is typically recorded directly following the Dark-adapted 0.01 ERG recording since light adaptation by the weaker stimulus is not clinically significant. The strength of the standard flash is 3.0 photopic cd·s·m−2 with a scotopic strength of 7.5 scotopic cd·s·m−2. There should be an interval of at least 10 s between stimulus flashes.
Dark-adapted 10 ERG (combined responses to stronger flash)
The Standard strong flash is 10 photopic cd·s·m−2, with a scotopic strength of 25 scotopic cd·s·m−2. In comparison with the dark-adapted 3 ERG, the dark-adapted 10 ERG is characterized by a larger a-wave with better definition of peak time, greater distinction of negative ERG waveforms (for recognition of diseases with relative b-wave reduction) and enhanced oscillatory potential amplitudes. In addition, this ERG may give more reliable responses in patients with opaque media or immature retinae. The dark-adapted 10 stimulus does not saturate the ERG and even stronger flashes may be useful (Note 4).
The Dark-adapted 10 ERG should be recorded after the Dark-adapted 3.0 ERG, with an interval of at least 20 s between strong flash stimuli.
Dark-adapted 3 oscillatory potentials: Standard dark-adapted oscillatory potentials are recorded from dark-adapted eyes, using the 3.0 cd·s·m−2 standard flash stimulus and may be recorded separately or derived from ERG waveforms by post hoc filtering. Oscillatory potential waveforms are obtained using a high-pass filter to remove frequencies of 75 Hz and below from the ERG waveform. The low-pass filter setting of 300 Hz or above is the same as for other ERG tests. There are several types of analog and digital high-pass filters, which influence the oscillatory potential waveform (e.g., introducing phase shifts or ringing). The simplest method of digital filtering is to remove all Fourier components of the ERG with frequencies <75 Hz. Other high-pass filters with a corner frequency between 75 and 100 Hz may be used if their characteristics are documented in the report. More information about filter selection and use is presented in the ISCEV technical guidelines [7].
The characteristics of the oscillatory potentials change after the first stimulus and amplitudes increase with longer inter-stimulus intervals. Only the OPs to the second and subsequent flashes should be retained or averaged. For standard dark-adapted oscillatory potentials, there should be at minimum of 10 s between stimulus flashes.
Light-adapted 3.0 ERG (single-flash cone response)
A minimum of 10-min light adaptation is required in dark-adapted patients to achieve stable and reproducible light-adapted ERGs and to maximize the response of the cone system and minimize rod input. The strength of the full-field background luminance for standard light adaptation is 30 photopic cd·s·m−2 (with a scotopic strength of 75 scotopic cd·s·m−2) measured at the location of the eye. Following light adaptation, standard stimulus flashes of 3.0 photopic cd·s·m−2 are delivered on the light-adapting background with at least 0.5 s between flashes.
Light-adapted 30 Hz flicker ERG
Flicker ERGs selectively reflect activity of the cone system, as rods do not respond at this rate. These should be obtained under the same conditions of light adaptation as the Light-adapted 3 ERG, using a train of brief (<5 ms), full-field flashes of 3.0 cd·s·m−2. Flashes should be presented at a rate of approximately 30 stimuli per second (acceptable range 28–33 Hz). Laboratories should choose a consistent frequency, avoiding exact multiples of the line frequency of the electricity supply or of local instruments, and may choose a frequency to facilitate analysis in the frequency domain (Note 5). The response to the initial onset of a flickering stimulus includes a transient response from the light-adapted rods; thus, the first few waves of the response should be discarded so that stable conditions are reached. Laboratories may incorporate pauses of ≥300 ms between short bursts of flicker so that this initial waveform can be identified.
Some xenon discharge lamps do not produce full output while flickering at these high frequencies and separate calibration or adjustment of the flash strength may be needed to conform to the standard.
ERG analysis and reporting
Single-flash ERGs
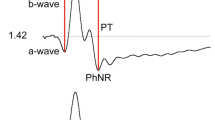
A-wave and b-wave amplitude, and peak time (also called implicit time) are measured when present for all single-flash ERGs except oscillatory potentials. According to current convention, the a-wave amplitude is measured from the average, pre-stimulus baseline to the a-wave trough. The b-wave amplitude is measured from a-wave trough to b-wave peak; the a-wave and b-wave peak times are measured from the time of the flash to the peak of the wave (see Fig. 1). The peak time of the a- and b-waves will depend on flash duration if measured from the beginning of the stimulus flash. This effect is sufficiently small for it to be ignored when the stimulus duration is less than a millisecond, for example when stimuli are generated by a xenon flash tube. For longer flashes of up to 5 ms, such as those generated by LEDs, the time to peak should be measured from the midpoint of the flash to compensate for the effect of stimulus duration on the peak times (Note 6).
Diagram of the six basic ERGs defined by the ISCEV Standard. These waveforms are exemplary only and are not intended to indicate minimum, maximum or typical values. Bold arrowheads indicate the stimulus flash; solid arrows illustrate a-wave and b-wave amplitudes dotted arrows exemplify how to measure time-to-peak (t, implicit time or peak time)
Oscillatory potentials
There is considerable debate about how to measure and describe oscillatory potentials (Note 7). Their appearance is highly dependent upon adaptation state and characteristics of the high-pass filter used to separate them from the ERG. There are usually three main positive peaks often followed by a fourth smaller one. Simply observing the presence and waveform of the OP peaks and their normality relative to the laboratory’s reference data may be adequate for most clinical applications.
Flicker ERGs
The amplitude of a flicker ERG is measured from trough to peak of a typical wave. Care should be taken to avoid the largest or smallest peak-to-trough amplitude. The response to the initial onset of the flicker, which may resemble a single-flash ERG, should always be excluded. The peak time of the flicker ERG is measured from the midpoint of the stimulus flash to the following peak (avoiding the initial waveform). It is helpful to average several typical measurements to determine the peak timing and amplitude of the flicker ERG. Alternatively, flicker ERGs can be examined in the frequency domain (Note 5).
Reference values (normal ranges)
Each laboratory should establish or confirm typical reference values for its own equipment, recording protocols and patient population giving attention to appropriate sample sizes. Because some ERG parameters (such as b-wave amplitude) are not normally distributed, interpretations based on standard deviation may be misleading. The median value (not the mean) should be used to define reference values, and the actual values on either side of the median that bracket 90 percent of the reference range of ERGs (in other words, the 5th and 95th % should be determined by direct tabulation of ERGs).
Note that ERG amplitudes increase rapidly in early infancy and decrease with age in adults, most substantially in elderly populations. Thus, reference values should be adjusted for age. Ocular pigmentation and high refractive errors can also impact ERG amplitudes and patients with characteristics that differ from the reference data should be noted. Although myopia alone does not severely compromise ERGs, patients with high myopia often have ERG amplitudes below the lower limits of the typical reference range. Although circadian variation of the ERG is small under ordinary recording conditions, the time of ERG recording should be noted on all records.
All ERG reporting, including reports of non-standard ERG techniques (whether for local records or for publication) should include reference values that show the range of normal. Some manufacturers distribute reference values for the protocols that they provide, and several large series have been published that give normative data. These may be useful for evaluation of ERGs recorded from similar populations using similar techniques with matching stimulus and recording parameters.
Reporting ISCEV Standard ERGs
Standardization of ERG reporting is critical to the goal of having comparable data worldwide. ERG reports should include representative reproduced waveforms of each of the Standard ERGs displayed with amplitude and time calibrations and labeled with stimulus variables and the state of light or dark adaptation. ERG tracings should include at least 20 ms of baseline prior to the stimulus for single-flash ERGs and, where feasible, should indicate the stimulus time for each flash with a marker or line (for flicker as well as for single-flash ERGs). At least, two responses from each stimulus condition should be displayed to demonstrate the degree of consistency or variability. The time-integrated luminance (photopic cd·s·m−2) of the stimulus flashes and the background luminance (photopic cd m−2) should be given in absolute values. In general, the scotopic time-integrated luminance (scotopic cd·s·m−2) values are presumed to fall within the ISCEV Standards. Ideally, the scotopic values should also be specified when reporting dark-adapted ERGs.
Reports should indicate explicitly whether there were any deviations from the current ISCEV Standard in techniques or recording parameters. All reports should give the patient’s results listed along with reference values and ranges. Finally, reports should note the time of testing, pupil diameters and the type and position of the corneal electrode. Conditions not specified by the standard such as sedation or anesthesia, and the level of compliance should also be documented.
Pediatric ERG recording
ERGs can be recorded from infants and young children. The younger the infant, the more chance that adult norms will not apply. ERGs mature during infancy, and signals from very young infants must be interpreted with caution. Very young or premature infants require special recording protocols and norms outside of this ISCEV Standard. Later in infancy and childhood, ERGs approach adult waveforms and amplitudes. Specifically, somewhat lower ERG amplitudes and longer peak times generally apply below 6–12 months of age under dark-adapted conditions, and below 2–3 months of age under light-adapted conditions. Below 6 months of age, the Dark-adapted 3 ERG may be poorly defined in healthy infants; Dark-adapted 10 ERGs are usually well defined in infants without retinal disease at all ages.
Many pediatric patients can be studied without sedation or general anesthesia. Small infants can be swaddled if necessary. Noncompliant children (especially ages 2–6 years for whom containment can be difficult) may become compliant with oral sedation. Medical guidelines should be followed with respect to indications, risks, medical monitoring requirements and the choice of a sedative/relaxant versus general anesthesia. Considering the variability of pediatric records, there will generally be little effect on ERG amplitude or waveform with sedation or light anesthesia, although full anesthesia may affect ERGs.
Contact lens electrodes with eyelid specula are suitable for infants and young children, and pediatric sizes will be required. Other types of corneal and skin electrodes vary in their applicability to children; greater comfort may be offset by greater electrode movement or smaller ERG amplitudes. To minimize artifact, special care is required with children to monitor electrode position and compliance.
Pediatric ERGs should ideally be compared to those from typical subjects of the same age, although there may be little reference data available. Because movement and poor fixation can make pediatric records variable, several repetitions of each ERG should be recorded to recognize reproducible waveforms and choose the best examples. Standard protocols may occasionally need to be abbreviated to obtain the ERGs most critical to the diagnostic question under investigation. Stronger flashes may help to reveal poorly developed ERGs. Reports should note the degree of cooperation and any medications used.
Notes
-
1.
The historic ISCEV standard stimuli took account of the rod and cone spectral sensitivities by stipulating that standard stimuli should be provided by xenon flash tubes thus defining (with sufficient precision) the spectrum of the broad-band standard flashes. More recent, ISCEV Standards specified the standard flashes as visibly white, broad-spectrum, flash stimuli with a color temperature near 7000 K. LEDs have several advantages over discharge lamps: more consistent output between flashes (including flashes presented at high frequencies); lower power requirements; less heat generation; no ultraviolet or infrared output; and more stable long-term output (i.e., avoiding deterioration common to other types of light sources). However, LEDs are available to produce light with a wide range of spectral distributions and may differ substantially from those of typical discharge lamps. This means that flashes produced by LEDs and xenon bulbs that are of equal strength for the cones may be very different for the rods and care must be taken to ensure that the appropriate scotopic luminance values are achieved when LEDs are used as a light source. LED-generated luminances of 0.01, 3.0 and 10.0 photopic cd·s·m−2 may not yield scotopic equivalents within the standard range (Table 1) under dark-adapted conditions.
The new definition specifies CIE co-ordinates, which acknowledges that the actual spectrum of light generated by LEDs will be very different from that of a black-body radiator. The scotopic/photopic ratio of a black-body radiator with a color temperature of 7000 K is 2.5. This ratio of 2.5 (acceptable range 2.25–2.75) should be applied to the definition based on CIE co-ordinates. To measure the scotopic/photopic ratio of flashes, separate measurements can be made using an integrating photometer with photopic and scotopic filters or this information may be provided by the manufacturers’ calibration system. In general, flashes compliant with the historic definition comply fully with this revised ISCEV Standard unless their wavelength spectra are unusual. The ISCEV Standard flash (x = 0.31, y = 0.32) is similar to the CIE standard Illuminant C which is described as “indirect sunlight.”
-
2.
Chromatic stimuli offer certain advantages in the separation of cone and rod ERGs. The calibration and description of ERGs for of colored stimuli are beyond the basic ISCEV Standard.
-
3.
The word “intensity” is widely used to describe the strength of ERG flashes. However, in photometry, “intensity” quantifies directional power per unit area, generally from a point source. Luminance is the appropriate term for steady-state (e.g., background light) surfaces (e.g., ganzfeld exit ports) as used for ERGs. Time-integrated luminance is the appropriate term for brief flashes, which is the integral of luminance over the flash duration; for simplicity, we use “strength” here.
-
4.
Additional strong flashes of up to 200 cd·s·m−2 increase the a-wave amplitude approaching saturation. Although not defined as ISCEV Standard ERGs, stronger flashes can be used for eyes with attenuated ERG amplitudes and for those with poorly defined a-waves.
-
5.
Frequency domain analysis of the flicker ERG is useful to detect attenuated ERG signals and provides information that may be physiologically relevant about the magnitude and phase of the harmonic components of the response. The magnitude and phase of individual harmonic components do not relate directly to amplitude and peak times of the flicker ERG (unless the magnitude and phase of all the harmonic components is taken into account).
-
6.
As a rule of thumb, components with peak times shorter than three times the flash duration will differ from those generated by a microsecond-duration stimulus. The assumption of equivalence of peak times evoked by millisecond and by microsecond stimuli is based on coincidence of the brief flash with the midpoint of the longer flash stimulus. By triggering at the midpoint of the flash or by subtracting half the flash length from the peak times, the effect of stimulus duration on peak time can be canceled. Not all effects of stimulus duration are eliminated using a mid-point trigger; the slope of the leading edge of the a-wave varies with stimulus duration and mid-point triggering does not apply to flicker ERGs where separate reference data are necessary for millisecond and microsecond stimuli.
-
7.
An overall index of oscillatory potential amplitude can be obtained by summing the amplitude measurements of the three major peaks, preferably from lines spanning the bases of the adjacent troughs, but alternatively from adjacent troughs directly (to allow use of measuring cursors with digitized systems). Some authors advise measurement of individual peaks.
Abbreviations
- ERG:
-
Electroretinogram
- ISCEV:
-
International Society for Clinical Electrophysiology of Vision
References
Marmor MF, Arden GB, Nilsson SE, Zrenner E (1989) Standard for clinical electroretinography. Arch Ophthalmol 107:816–819
Marmor MF, Fulton AB, Holder GE, Miyaki Y, Brigell M, Bach M (2008) Standard for clinical electroretinography (2008 update). Doc Ophthalmol 118:69–77
Hood DC, Bach M, Brigell M, Keating D, Kondo M, Lyons JS, Marmor MF, McCulloch DL, Palmowski-Wolfe AM (2012) ISCEV Standard for clinical multifocal electroretinography (2011 edition). Doc Ophthalmol 124:1–13
Bach M, Brigell MG, Hawlina M, Holder GE, Johnson MA, McCulloch DL, Meigen T, Viswanathan S (2013) ISCEV Standard for clinical pattern electroretinography (PERG)—2012 update. Doc Ophthalmol 126:1–7
Marmor MF, Brigell MG, Westall CA, Bach M (2011) ISCEV Standard for Clinical Electro-oculography (2010 Update). Doc Ophthalmol 122:1–7
Odom JV, Bach M, Brigell M, Holder GE, McCulloch DL, Tormene AP, Vaegan AGB (2010) ISCEV Standard for clinical visual evoked potentials (2009 update). Doc Ophthalmol 120:111–119
Brigell M, Bach M, Barber C, Moskowitz A, Robson J (2003) Guidelines for calibration of stimulus and recording parameters used in clinical electrophysiology of vision. Doc Ophthalmol 107:185–193
Acknowledgments
We are grateful to many ISCEV members for their constructive input into this document, in particular John Robson, Chris Hogg, Quintin Davis, Jason McAnany and Ulrich Kellner. The information from the ISCEV survey of full-field electroretinography practice (December 2012, <http://www.iscev.org/misc.html>) was helpful and we thank the 109 respondents.
Author information
Authors and Affiliations
Corresponding author
Additional information
For the International Society for Clinical Electrophysiology of Vision (ISCEV)
Appendix
Rights and permissions
About this article
Cite this article
McCulloch, D.L., Marmor, M.F., Brigell, M.G. et al. ISCEV Standard for full-field clinical electroretinography (2015 update). Doc Ophthalmol 130, 1–12 (2015). https://doi.org/10.1007/s10633-014-9473-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10633-014-9473-7