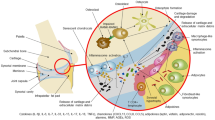
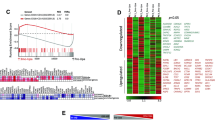
Abstract
It is recognized that CC chemokine receptor 3 (CCR3) is associated with numerous inflammatory conditions and fibroblast-like synoviocyte (FLS) invasiveness correlates with articular damage in rheumatoid arthritis (RA). However, little is known of the expression and action of CCR3 on FLS in RA. In the present study, we investigated the expression of CCR3 on dispersed synovial tissue and peripheral blood cells in RA and influence of eotaxin-1 on FLS functions by using flow cytometry analysis, FLS challenge, and real-time PCR techniques. The results showed that approximately 7.0 % dispersed synovial cells are CCR3+ cells. Among those CCR3+ cells, 38.1, 23.8, and 20.6 % cells are CD90+CD14−CD3− (representing FLS), CD14+, and CD8+ cells, respectively, indicating that FLS is one of the major populations of CCR3+ cells in the synovial tissue of RA. In peripheral blood, CD14+ CCR3+ cells are elevated, but CD8+CCR3+ cells are reduced in RA. It was found that eotaxin-1 induced upregulated expression of CCR3 and matrix metalloproteinase (MMP)-9 messenger RNAs (mRNAs) in FLS. Since an antagonist of CCR3 suppressed the action of eotaxin-1, the event appeared CCR3 dependent. Moreover, we observed that interleukin (IL)-1β induced markedly enhanced eotaxin-1 release from FLS, but TNF-α reduced eotaxin-1 release at 12 and 24 h following incubation. In conclusion, enhanced expression of CCR3 on synovial cells and increased levels of eotaxin-1 in plasma and synovial fluid (SF) of RA indicate that CCR3-mediated mechanisms may play an important role in RA. Blockage of eotaxin-1 provoked CCR3 and MMP-9 expression in FLS by antagonist of CCR3, implicating that anti-CCR3 agents may have therapeutic use for RA.







Similar content being viewed by others
Abbreviations
- FLS:
-
Fibroblast-like synoviocyte
- MFI:
-
Mean fluorescence intensity
- MMP:
-
Matrix metalloproteinase
- OA:
-
Osteoarthritis
- RA:
-
Rheumatoid arthritis
- SF:
-
Synovial fluid
References
Bartok B, Firestein GS. Fibroblast-like synoviocytes: key effector cells in rheumatoid arthritis. Immunol Rev. 2010;233:233–55.
Beck LA, Tancowny B, Brummet ME, Asaki SY, Curry SL, Penno MB, et al. Functional analysis of the chemokine receptor CCR3 on airway epithelial cells. J Immunol. 2006;177:3344–54.
Chang YH, Lin IL, Tsay GJ, Yang SC, Yang TP, Ho KT, et al. Elevated circulatory MMP-2 and MMP-9 levels and activities in patients with rheumatoid arthritis and systemic lupus erythematosus. Clin Biochem. 2008;41:955–9.
Chang X, Shen J, Yang H, Xu Y, Gao W, Wang J, et al. Upregulated expression of CCR3 in osteoarthritis and CCR3 mediated activation of fibroblast-like synoviocytes. Cytokine. 2016;77:211–9.
Fiedorczyk M, Klimiuk PA, Sierakowski S, Gindzienska-Sieskiewicz E, Chwiecko J. Serum matrix metalloproteinases and tissue inhibitors of metalloproteinases in patients with early rheumatoid arthritis. J Rheumatol. 2006;33:1523–9.
Firestein GS. Evolving concepts of rheumatoid arthritis. Nature. 2003;423:356–61.
Garcia-Vicuna R, Gomez-Gaviro MV, Dominguez-Luis MJ, Pec MK, Gonzalez-Alvaro I, Alvaro-Gracia JM, et al. CC and CXC chemokine receptors mediate migration, proliferation, and matrix metalloproteinase production by fibroblast-like synoviocytes from rheumatoid arthritis patients. Arthritis Rheum. 2004;50:3866–77.
Gaspar K, Kukova G, Bunemann E, Buhren BA, Sonkoly E, Szollosi AG, et al. The chemokine receptor CCR3 participates in tissue remodeling during atopic skin inflammation. J Dermatol Sci. 2013;71:12–21.
Giannelli G, Iannone F, Marinosci F, Covelli M, Lapadula G, Antonaci S. Infliximab therapy does not modify MMP-2 and MMP-9 serum concentrations in chronic arthritis. Clin Exp Rheumatol. 2005;23:867–72.
Jiao Z, Wang W, Ma J, Wang S, Su Z, Xu H. Notch signaling mediates TNF-alpha-induced IL-6 production in cultured fibroblast-like synoviocytes from rheumatoid arthritis. Clin Dev Immunol. 2012;2012:350209.
Katschke KJ, Rottman JB, Ruth JH, Qin S, Wu L, LaRosa G, et al. Differential expression of chemokine receptors on peripheral blood, synovial fluid, and synovial tissue monocytes/macrophages in rheumatoid arthritis. Arthritis Rheum. 2001;44:1022–32.
Kay J, Upchurch KS. ACR/EULAR 2010 rheumatoid arthritis classification criteria. Rheumatology (Oxford). 2012;51 Suppl 6:vi5–9.
Kim KS, Choi HM, Lee YA, Choi IA, Lee SH, Hong SJ, et al. Expression levels and association of gelatinases MMP-2 and MMP-9 and collagenases MMP-1 and MMP-13 with VEGF in synovial fluid of patients with arthritis. Rheumatol Int. 2011;31:543–7.
Koch AE. Chemokines and their receptors in rheumatoid arthritis: future targets? Arthritis Rheum. 2005;52:710–21.
Laragione T, Gulko PS. Liver X receptor regulates rheumatoid arthritis fibroblast-like synoviocyte invasiveness, matrix metalloproteinase 2 activation, interleukin-6 and CXCL10. Mol Med. 2012;18:1009–17.
Li GQ, Zhang Y, Liu D, Qian YY, Zhang H, Guo SY, et al. Celastrol inhibits interleukin-17A-stimulated rheumatoid fibroblast-like synoviocyte migration and invasion through suppression of NF-kappaB-mediated matrix metalloproteinase-9 expression. Int Immunopharmacol. 2012;14:422–31.
Mangieri D, Corradi D, Martorana D, Malerba G, Palmisano A, Libri I, et al. Eotaxin/CCL11 in idiopathic retroperitoneal fibrosis. Nephrol Dial Transplant. 2012;27:3875–84.
Manousou P, Kolios G, Valatas V, Drygiannakis I, Bourikas L, Pyrovolaki K, et al. Increased expression of chemokine receptor CCR3 and its ligands in ulcerative colitis: the role of colonic epithelial cells in in vitro studies. Clin Exp Immunol. 2010;162:337–47.
Miyamasu M, Nakajima T, Misaki Y, Izumi S, Tsuno N, Kasahara T, et al. Dermal fibroblasts represent a potent major source of human eotaxin: in vitro production and cytokine-mediated regulation. Cytokine. 1999;11:751–8.
Nissinen R, Leirisalo-Repo M, Tiittanen M, Julkunen H, Hirvonen H, Palosuo T, et al. CCR3, CCR5, interleukin 4, and interferon-gamma expression on synovial and peripheral T cells and monocytes in patients with rheumatoid arthritis. J Rheumatol. 2003;30:1928–34.
Privat SJ, Oo A, Waterbury LD. Production of interleukin-6, but not interleukin-8, induced by TNF-alpha or IL-1 beta in human fibroblast-like synoviocyte increases over cell passage. Proc West Pharmacol Soc. 2001;44:9–13.
Radman M, Hassanshahi G, Vazirinejad R, Arababadi MK, Karimabad MN, Khorramdelazad H, et al. Serum levels of the CC chemokines CCL2, CCL5, and CCL11 in food allergic children with different clinical manifestations. Inflammation. 2013;36:561–6.
Rankin SM, Conroy DM, Williams TJ. Eotaxin and eosinophil recruitment: implications for human disease. Mol Med Today. 2000;6:20–7.
Ruscitti P, Cipriani P, Carubbi F, Liakouli V, Zazzeroni F, Di Benedetto P, et al. The role of IL-1beta in the bone loss during rheumatic diseases. Mediators Inflamm. 2015;2015:782382.
Syversen SW, Goll GL, Haavardsholm EA, Boyesen P, Lea T, Kvien TK. A high serum level of eotaxin (CCL 11) is associated with less radiographic progression in early rheumatoid arthritis patients. Arthritis Res Ther. 2008;10:R28.
Tanner MR, Hu X, Huq R, Tajhya RB, Sun L, Khan FS, et al. KCa1.1 inhibition attenuates fibroblast-like synoviocyte invasiveness and ameliorates disease in rat models of rheumatoid arthritis. Arthritis Rheumatol. 2015;67:96–106.
Tedeschi A, Asero R, Lorini M, Marzano AV, Cugno M. Serum eotaxin levels in patients with chronic spontaneous urticaria. Eur Ann Allergy Clin Immunol. 2012;44:188–92.
Uguccioni M, Mackay CR, Ochensberger B, Loetscher P, Rhis S, LaRosa GJ, et al. High expression of the chemokine receptor CCR3 in human blood basophils. Role in activation by eotaxin, MCP-4, and other chemokines. J Clin Invest. 1997;100:1137–43.
Xue M, McKelvey K, Shen K, Minhas N, March L, Park SY, et al. Endogenous MMP-9 and not MMP-2 promotes rheumatoid synovial fibroblast survival, inflammation and cartilage degradation. Rheumatology (Oxford). 2014;53:2270–9.
Zhang H, Yang X, Yang H, Zhang Z, Lin Q, Zheng Y, et al. Modulation of mast cell proteinase-activated receptor expression and IL-4 release by IL-12. Immunol Cell Biol. 2007;85:558–66.
Zhou M, Qin S, Chu Y, Wang F, Chen L, Lu Y. Immunolocalization of MMP-2 and MMP-9 in human rheumatoid synovium. Int J Clin Exp Pathol. 2014;7:3048–56.
Acknowledgments
This project was sponsored by the grants from the “12th Five-Year” National Science and Technology Supporting Plan (2014BAI07B02); the National Natural Science Foundation of China (Nos. 81172836, 81471592, 81472016); Major Science and Technology Platform for Institution of Higher Education in Liaoning Province (2014168); the National Natural Science Foundation of Liaoning Province (2014022027, 2014022019, 2014410004); Program for Liaoning Innovation Research Team in Universities (LNIRT, LT2013017); Climbing Scholar Project for Institution of Higher Education in Liaoning Province (2013222); Allergic Disease Translational Medicine Research Center of Liaoning Province (2015225016); Liaoning Provincial Engineering Research Center for Diagnosing & Treating Inflammatory Disease (20141093); Clinical Capability Construction Project for Liaoning Provincial Hospitals (LNCCC-A06-2014, LNCCC-D26-2015); and “12th Five-Year” public welfare industry special scientific research project (2015SQ00136).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
All samples obtained were with informed consent from each patient. All experiments were approved by the Ethical Committee of The First Affiliated Hospital of Jinzhou Medical University.
Conflict of interest
The authors declare that they have no conflict of interests.
Additional information
Xin Liu, Huiyun Zhang and Xin Chang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Liu, X., Zhang, H., Chang, X. et al. Upregulated expression of CCR3 in rheumatoid arthritis and CCR3-dependent activation of fibroblast-like synoviocytes. Cell Biol Toxicol 33, 15–26 (2017). https://doi.org/10.1007/s10565-016-9356-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10565-016-9356-7