Abstract
Objectives
This study aims to compare lipophilic and hydrophilic statin therapy on clinical outcomes of heart failure (HF) using a systematic review and an adjusted indirect comparison meta-analysis. Outcomes were all-cause mortality, cardiovascular mortality, cardiovascular hospitalization and hospitalization for worsening HF.
Methods
We conducted a search of PubMed, EMBASE and Cochrane databases until 31st December 2014 for randomized control trials (RCTs) in HF evaluating statins versus placebo. Identified RCTs and their respective abstracted information were grouped according to statin type evaluated and analyzed separately. Outcomes were initially pooled with the Peto’s one-step method, producing odd ratios (OR) and 95 % confidence intervals (CI) for each statin type. Using these pooled estimates, we performed adjusted indirect comparisons of lipophilic versus hydrophilic statin for each outcome.
Results
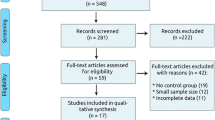
Thirteen studies involving 10,966 patients were identified and analyzed. Lipophilic statins were superior to hydrophilic rosuvastatin regarding all-cause mortality (OR 0 · 50; 95 % CI, 0 · 11–0 · 89; p = 0 · 01), cardiovascular mortality (OR 0 · 61; 0 · 25–0 · 97; p = 0 · 009), and hospitalization for worsening HF (OR 0 · 52; 0 · 21–0 · 83; p = 0 · 0005). However, both statins were comparable with regards to cardiovascular hospitalization [OR 0 · 80 (0 · 31, 1 · 28); p = 0 · 36].
Conclusions
Lipophilic statin treatment shows significant decreases in all-cause mortality, cardiovascular mortality and hospitalization for worsening HF compared with rosuvastatin treatment. This meta-analysis provides preliminary evidence that lipophilic statins offer better clinical outcomes in HF till data from head to head comparisons are available.





Similar content being viewed by others
References
Callender T, Woodward M, Roth G, Farzadfar F, Lemarie JC, et al. Heart Failure Care in Low- and Middle-Income Countries: A Systematic Review and Meta-Analysis. PLoS Med. 2014. doi:10.1371/journal.pmed.1001699.
Bui AL, Horwich TB, Fonarow GC. Epidemiology and risk profile of heart failure. Nat Rev Cardiol. 2011;8:30–41.
Kjekshus JPT, Olsson AG, Faergeman O, Pyorala K. The effects of simvastatin on the incidence of heart failure in patients with coronary heart disease. J Card Fail. 1997;3:249–54.
Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. The Long-Term Intervention with Pravastatin in Ischaemic Disease (LIPID) Study Group. New Engl J Med 1998; 339:1349–1357.
Bonsu KO, Kadirvelu A, Reidpath DD. Statins in heart failure: do we need another trial? Vasc Health Risk Manag. 2013;9:303–19.
Go AS, Lee WY, Yang J, Lo JC, Gurwitz JH. Statin therapy and risks for death and hospitalization in chronic heart failure. JAMA. 2006;296:2105–11.
Anker SDCA, Winkler R, et al. Statin use and survival in patients with chronic heart failure: results from two observational studies with 5200 patients. Int J Cardiol. 2006;112:234–42.
Ray JG, Gong Y, Sykora K, Tu JV. Statin use and survival outcomes in elderly patients with heart failure. Arch Intern Med. 2005;165:62–7.
Foody JM, Shah R, Galusha D, et al. Statin and mortality among elderly patients hospitalized with heart failure. Circulation. 2006;113:1086–92.
Hognestad A, Dickstein K, Myhre E, Snapinn S, Kjekshus J. Effect of combined statin and beta-blocker treatment on one-year morbidity and mortality after acute myocardial infarction associated with heart failure. Am J Cardiol. 2004;93:603–6.
Yamada T, Node K, Mine T, Morita T, Kioka H, et al. Long-term effect of atorvastatin on neurohumoral activation and cardiac function in patients with chronic heart failure: A prospective randomized controlled study. Am Heart J. 2007;153:1055.e1051–8.
Bielecka-Dabrowa A, Goch JH, Mikhailidis DP, Rysz J, Maciejewski M, et al. (2009) The influence of atorvastatin on parameters of inflammation and function of the left ventricle in patients with dilated cardiomyopathy. Med Sci Monit. 2009;15:12–23.
Sola S, Mir MQS, Rajagopalan S, Helmy T, Tandon N, et al. Statin Therapy Is Associated With Improved Cardiovascular Outcomes and Levels of Inflammatory Markers in Patients With Heart Failure. J Card Fail. 2005;11:607–12.
Vrtovec B, Okrajsek R, Golicnik A, Ferjan M, Starc V, et al. Atorvastatin therapy may reduce the incidence of sudden cardiac death in patients with advanced chronic heart failure. J Card Fail. 2008;14:140–4.
Hamaad A, Sosin M, Lip GY, MacFadyen RJ. Short-term adjuvant atorvastatin improves frequency domain indices of heart rate variability in stable systolic heart failure. Cardiovasc Drugs Ther. 2005;19:183–7.
Hong YJ, Jeong MH, Hyun DW, Hur SH, Kim KB, et al. Prognostic significance of simvastatin therapy in patients with ischemic heart failure who underwent percutaneous coronary intervention for acute myocardial infarction. Am J Cardiol. 2005;95:619–22.
Kjekshus J, Apetrei E, Barrios V, Bohm M, Cleland JG, et al. Rosuvastatin in older patients with systolic heart failure. N Engl J Med. 2007;357:2248–61.
Tavazzi L, Maggioni AP, Marchioli R, Barlera S, Franzosi MG, et al. Effect of rosuvastatin in patients with chronic heart failure (the GISSI-HF trial): a randomised, double-blind, placebo-controlled trial. Lancet. 2008;372:1231–9.
Lipinski MJ, Cauthen CA, Biondi-Zoccai GG, Abbate A, Vrtovec B, et al. Meta-analysis of randomized controlled trials of statins versus placebo in patients with heart failure. Am J Cardiol. 2009;104:1708–16.
Zhang S, Zhang L, Sun A, Jiang H, Qian J, et al. Efficacy of statin therapy in chronic systolic cardiac insufficiency: a meta-analysis. Eur J Intern Med. 2011;22:478–84.
Schachter M. Chemical, pharmacokinetic and pharmacodynamic properties of statins: an update. Fundam Clin Pharmacol. 2005;19:117–25.
Nezasa K, Higaki K, Matsumura T, Inazawa K, Hasegawa H, et al. Liver-specific distribution of rosuvastatin in rats: comparison with pravastatin and simvastatin. Drug Metab Dispos. 2002;30:1158–63.
Ford JS, Tayek JA. Lipophilicity and cardiovascular outcome in patients with CHF. Am Heart J. 2008;156:e7. author reply e9.
Bucher HC, Guyatt GH, Griffith LE, Walter SD. The results of direct and indirect treatment comparisons in meta-analysis of randomized controlled trials. J Clin Epidemiol. 1997;50:683–91.
Biondi-Zoccai G, Lotrionte M, Agostoni P, Abbate A, Romagnoli E, et al. Adjusted indirect comparison meta-analysis of prasugrel versus ticagrelor for patients with acute coronary syndromes. Int J Cardiol. 2011;150:325–31.
Moher D, Liberati A, Tetzlaff J, Altman D. PRISMA G Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535.
Bonsu KO, Kadirvelu A, Reidpath DD. Lipophilic versus hydrophilic statin therapy for heart failure: a protocol for an adjusted indirect comparison meta-analysis. Syst Rev. 2013;2:22.
Jadad A, Moore R, Carroll D, Jenkinson C, Reynolds D, et al. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials. 1996;17:1–12.
Krum H, Ashton E, Reid C, Kalff V, Rogers J, et al. Double-Blind, randomized, placebo-controlled study of high-dose hmg coa reductase inhibitor therapy on ventricular remodeling, pro-inflammatory cytokines and neurohormonal parameters in patients with chronic systolic heart failure. J Card Fail. 2007;13:1–7.
Node K, Fujita M, Kitakaze M, Hori M, Liao JK. Short-term statin therapy improves cardiac function and symptoms in patients with idiopathic dilated cardiomyopathy. Circulation. 2003;108:839–43.
Takano H, Mizuma H, Kuwabara Y, Sato Y, Shindo S, et al. Effects of pitavastatin in Japanese patients with chronic heart failure: the Pitavastatin Heart Failure Study (PEARL Study). Circ J. 2013;77:917–25.
Wojnicz R, Wilczek K, Nowalany-Kozielska E, Szygula-Jurkiewicz B, Nowak J, et al. Usefulness of atorvastatin in patients with heart failure due to inflammatory dilated cardiomyopathy and elevated cholesterol levels. Am J Cardiol. 2006;97:899–904.
Xie RQ, Cui W, Liu F, Yang C, Pei WN, et al. Statin therapy shortens QTc, QTcd, and improves cardiac function in patients with chronic heart failure. Int J Cardiol. 2010;140:255–7.
Guyatt GH, Oxman AD, Schünemann HJ, Tugwell P, Knottnerus A. GRADE guidelines: A new series of articles in the Journal of Clinical Epidemiology. J Clin Epidemiol. 2011;64:380–2.
Brozek J OA, Schunemann H. GRADEpro. [Computer program]. Version 3.2 for Windows. 2008
Wells GA SS, Chen L, Khan M, Coyle D. Indirect treatment comparison [computer program]. Ottawa: Canadian Agency for Drugs and Technologies in Health Version 1.0.(2009)
Edwards SJ, Clarke MJ, Wordsworth S, Borrill J. Indirect comparisons of treatments based on systematic reviews of randomised controlled trials. Int J Clin Pract. 2009;63:841–54.
Ioannidis J, Patsopoulos N, Evangelou E. Uncertainty in heterogeneity estimates in meta-analyses. BMJ. 2007;335:914–6.
Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics. 1994;50:1088–101.
Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315:629–34.
Preiss D, Campbell RT, Murray HM, Ford I, Packard CJ, et al. The effect of statin therapy on heart failure events: a collaborative meta-analysis of unpublished data from major randomized trials. Eur Heart J 2015. Eur Heart J. 2015;36:1536–46.
Liu G, Zheng X-X, Xu Y-L, Lu J, Hui R-T, et al. Effects of lipophilic statins for heart failure: a meta-analysis of 13 randomised controlled trials. Heart, Lung, Circulation. 2014;23:970–7.
Brunner-La Rocca HP, Esler MD, Jennings GL, Kaye DM. Effect of cardiac sympathetic nervous activity on mode of death in congestive heart failure. Eur Heart J. 2001;22:1136–43.
Nishiyama KTT, Yamaji M, Kawahara C, Yamamoto T, Fujii M, et al. Dose-dependent prognostic effect of carvedilol in patients with chronic heart failure: Special reference to transcardiac gradient of norepinephrine. Circ J. 2009;73:2270–5.
Verberne HJBL, Somsen GA, van Eck-Smit BL. Prognostic value of myocardial 123I-metaiodobenzylguanidine (MIBG) parameters in patients with heart failure: A systematic review. Eur Heart J. 2008;29:1147–59.
Tsutamoto T, Sakai H, Ibe K, Yamaji M, Kawahara C, et al. Effect of atorvastatin vs. rosuvastatin on cardiac sympathetic nerve activity in non-diabetic patients with dilated cardiomyopathy. Circ J. 2011;75:2160–6.
Sano H, Kasama S, Fujimoto S, Toyama T, Takama N, et al. Effects of statin therapy on cardiac sympathetic nerve activity and left ventricular remodeling in patients with chronic heart failure: a propensity score-matched analysis. Medicine. 2014;93:e214.
Lewandowski J, Symonides B, Gaciong Z, Siński M. The effect of statins on sympathetic activity: a meta-analysis. Clin Auton Res. 2015;25:125–31.
Ueland T, Gullestad L, Nymo SH, Yndestad A, Aukrust P, et al. Inflammatory cytokines as biomarkers in heart failure. Clin Chim Acta. 2015;443:71–7.
Liquori ME, Christenson RH, Collinson PO, Defilippi CR. Cardiac biomarkers in heart failure. Clin Biochem. 2014;47:327–37.
De Matos LDGG, Rondon MU, Soufen HN, Tirone AP, Barretto AC, et al. Impact of 6 months of therapy with carvedilol on muscle sympathetic nerve activity in heart failure patients. J Card Fail. 2004;10:496–502.
Grassi G, Cattaneo BM, Seravalle G, Lanfranchi A, Pozzi M, Morganti A, et al. Effects of chronic ACE inhibition on sympathetic nerve traffic and baroreflex control of circulation in heart failure. Circulaton. 1997;96:1173–9.
Hikosaka MYF, Yuyama R, Mimura J, Kawamura A, Motohiro M, et al. Candesartan and arterial baroreflex sensitivity and sympathetic nerve activity in patients with mild heart failure. J Cardiovasc Pharmacol. 2002;40:875–80.
Bonsu KO, Reidpath DD, Kadirvelu A. Effects of Statin Treatment on Inflammation and Cardiac function in Heart Failure: An Adjusted Indirect Comparison Meta-analysis of Randomised Trials. Cardiovasc Ther. 2015. doi:10.1111/1755-5922.12150.
Jansen JP, Fleurence R, Devine B, Itzler R, Barrett A, et al. Interpreting indirect treatment comparisons and network meta-analysis for health-care decision making: report of the ISPOR Task Force on Indirect Treatment Comparisons Good Research Practices: part 1. Value Health. 2011;14:417–28.
Song F, Harvey I, Lilford R. Adjusted indirect comparison may be less biased than direct comparison for evaluating new pharmaceutical interventions. J Clin Epidemiol. 2008;61:455–63.
Lip GY, Larsen TB, Skjoth F, Rasmussen LH. Indirect comparisons of new oral anticoagulant drugs for efficacy and safety when used for stroke prevention in atrial fibrillation. J Am Coll Cardiol. 2012;60:738–46.
Rasmussen LH, Larsen TB, Graungaard T, Skjoth F, Lip GY. Primary and secondary prevention with new oral anticoagulant drugs for stroke prevention in atrial fibrillation: indirect comparison analysis. BMJ. 2012;345:e7097.
Acknowledgments
We are grateful to Dr Lee Chiang Sheng (LCS) and Dr Vishnuprasad Baktavatsalam (VB) for the technical assistance.
Authors’ Contributions
KOB conceived the original idea and refined it with AK and DDR. KOB wrote the initial draft and conducted the analysis of the data. AK and DDR contributed to subsequent drafts. All authors edited and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interests
The authors declare that there are no competing interests.
Authors’ Disclosure
All three authors have nothing of potential conflict of interest to disclose
Rights and permissions
About this article
Cite this article
Bonsu, K.O., Reidpath, D.D. & Kadirvelu, A. Lipophilic Statin Versus Rosuvastatin (Hydrophilic) Treatment for Heart Failure: a Meta-Analysis and Adjusted Indirect Comparison of Randomised Trials. Cardiovasc Drugs Ther 30, 177–188 (2016). https://doi.org/10.1007/s10557-015-6636-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-015-6636-z