Abstract
Purpose
Obesity and oversupply of glucose, e.g., due to nutritional factors may shape the tumor microenvironment favorable for tumor progression. O-GlcNAcylation, a reversible modification of intracellular proteins, influences on several cellular functions and is connected to many diseases including cancer. Glycosaminoglycan hyaluronan (HA) enhances tumor progression and in breast cancer HA accumulation associates strongly with poor outcome. In vitro studies have suggested that O-GlcNAcylation may enhance HA synthesis. The aim of this study was to investigate the correlations between O-GlcNAcylation, HA-related parameters, and disease outcome in a clinical breast cancer material consisting of 278 breast cancer cases.
Methods
In microscopic analyses, O-GlcNAc staining of the breast carcinoma cells was evaluated in several randomly picked high-power fields of each section. The extent of cytoplasmic O-GlcNAc staining was graded as either low or high according to the intensity of the staining and the percentage of stained cells. The extent of nuclear O-GlcNAc staining was categorized as either low or high according to the percentage of stained nuclei.
Results
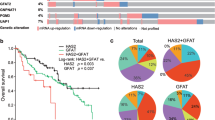
A high extent of both cytoplasmic and nuclear O-GlcNAcylation correlated with an increased relapse rate, development of distant metastases, and poor outcome. A high extent of cytoplasmic O-GlcNAcylation correlated also with the accumulation of all hyaluronan synthase (HAS1-3) proteins and with a large amount of HA in the tumor stroma. In addition, a high extent of nuclear O-GlcNAcylation associated with obesity.
Conclusions
The results suggest a mechanistic association between increased O-GlcNAcylation and HA synthesis, leading to a HA-rich microenvironment favorable for breast cancer progression.


Similar content being viewed by others
Abbreviations
- FDG-PET:
-
18F-fluorodeoxyglucose-positron emission tomography
- HBP:
-
Hexosamine biosynthetic pathway
- UDP-GlcNAc:
-
Uridine diphosphate N-acetylglucosamine
- HA:
-
Hyaluronan
- HAS:
-
Hyaluronan synthase
- UDP-GlcUA:
-
Uridine diphosphate glucuronic acid
- HER2:
-
Human epidermal growth factor receptor 2
- OGT:
-
O-GlcNAc transferase
- OGA, MGEA5:
-
O-GlcNAcase
- PB:
-
Phosphate buffer
- BSA:
-
Bovine serum albumin
- ER:
-
Estrogen receptor
- PR:
-
Progesterone receptor
- BMI:
-
Body mass index
- DFS:
-
Disease-free survival
- OS:
-
Overall survival
References
Gambhir SS (2002) Molecular imaging of cancer with positron emission tomography. Nat Rev Cancer 2:683–693
Warburg O (1956) On the origin of cancer cells. Science 123:309–314
Vander Heiden MG, Cantley LC, Thompson CB (2009) Understanding the Warburg effect: the metabolic requirements of cell proliferation. Science 324:1029–1033
Ma Z, Vosseller K (2013) O-GlcNAc in cancer biology. Amino Acids 45:719–733
Vigetti D, Viola M, Karousou E et al (2014) Metabolic control of hyaluronan synthases. Matrix Biol 35:8–13
Tammi RH, Passi AG, Rilla K et al (2011) Transcriptional and post-translational regulation of hyaluronan synthesis. FEBS J 278:1419–1428
Weigel PH, DeAngelis PL (2007) Hyaluronan synthases: a decade-plus of novel glycosyltransferases. J Biol Chem 282:36777–36781
Sironen RK, Tammi M, Tammi R et al (2011) Hyaluronan in human malignancies. Exp Cell Res 317:383–391
Toole BP (2004) Hyaluronan: from extracellular glue to pericellular cue. Nat Rev Cancer 4:528–539
Auvinen P, Tammi R, Kosma VM et al (2013) Increased hyaluronan content and stromal cell CD44 associate with HER2 positivity and poor prognosis in human breast cancer. Int J Cancer 132:531–539
Auvinen P, Rilla K, Tumelius R et al (2014) Hyaluronan synthases (HAS1-3) in stromal and malignant cells correlate with breast cancer grade and predict patient survival. Breast Cancer Res Treat 143:277–286
Torres CR, Hart GW (1984) Topography and polypeptide distribution of terminal N-acetylglucosamine residues on the surfaces of intact lymphocytes. Evidence for O-linked GlcNAc. J Biol Chem 259:3308–3317
Fardini Y, Dehennaut V, Lefebvre T et al (2013) O-GlcNAcylation: a new cancer hallmark? Front Endocrinol (Lausanne) 4:99
Haltiwanger RS, Holt GD, Hart GW (1990) Enzymatic addition of O-GlcNAc to nuclear and cytoplasmic proteins. Identification of a uridine diphospho-N-acetylglucosamine: peptide beta-N-acetylglucosaminyltransferase. J Biol Chem 265:2563–2568
Haltiwanger RS, Blomberg MA, Hart GW (1992) Glycosylation of nuclear and cytoplasmic proteins. Purification and characterization of a uridine diphospho-N-acetylglucosamine: polypeptide beta-N-acetylglucosaminyltransferase. J Biol Chem 267:9005–9013
Dong DL, Hart GW (1994) Purification and characterization of an O-GlcNAc selective N-acetyl-beta-d-glucosaminidase from rat spleen cytosol. J Biol Chem 269:19321–19330
Gao Y, Wells L, Comer FI et al (2001) Dynamic O-glycosylation of nuclear and cytosolic proteins: cloning and characterization of a neutral, cytosolic beta-N-acetylglucosaminidase from human brain. J Biol Chem 276:9838–9845
Zachara NE, Hart GW (2004) O-GlcNAc a sensor of cellular state: the role of nucleocytoplasmic glycosylation in modulating cellular function in response to nutrition and stress. Biochim Biophys Acta 1673:13–28
Hart GW, Slawson C, Ramirez-Correa G et al (2011) Cross talk between O-GlcNAcylation and phosphorylation: roles in signaling, transcription, and chronic disease. Annu Rev Biochem 80:825–858
Hart GW, Housley MP, Slawson C (2007) Cycling of O-linked beta-N-acetylglucosamine on nucleocytoplasmic proteins. Nature 446:1017–1022
Slawson C, Hart GW (2011) O-GlcNAc signalling: implications for cancer cell biology. Nat Rev Cancer 11:678–684
Gu Y, Mi W, Ge Y et al (2010) GlcNAcylation plays an essential role in breast cancer metastasis. Cancer Res 70:6344–6351
Krzeslak A, Forma E, Bernaciak M et al (2012) Gene expression of O-GlcNAc cycling enzymes in human breast cancers. Clin Exp Med 12:61–65
Champattanachai V, Netsirisawan P, Chaiyawat P et al (2013) Proteomic analysis and abrogated expression of O-GlcNAcylated proteins associated with primary breast cancer. Proteomics 13:2088–2099
Caldwell SA, Jackson SR, Shahriari KS et al (2010) Nutrient sensor O-GlcNAc transferase regulates breast cancer tumorigenesis through targeting of the oncogenic transcription factor FoxM1. Oncogene 29:2831–2842
Jiang K, Gao Y, Hou W et al (2016) Proteomic analysis of O-GlcNAcylated proteins in invasive ductal breast carcinomas with and without lymph node metastasis. Amino Acids 48:365–374
Vigetti D, Deleonibus S, Moretto P et al (2012) Role of UDP-N-acetylglucosamine (GlcNAc) and O-GlcNAcylation of hyaluronan synthase 2 in the control of chondroitin sulfate and hyaluronan synthesis. J Biol Chem 287:35544–35555
Deen AJ, Arasu UT, Pasonen-Seppanen S et al (2016) UDP-sugar substrates of HAS3 regulate its O-GlcNAcylation, intracellular traffic, extracellular shedding and correlate with melanoma progression. Cell Mol Life Sci 73(16):3183–3204
McShane LM, Altman DG, Sauerbrei W et al (2006) REporting recommendations for tumor MARKer prognostic studies (REMARK). Breast Cancer Res Treat 100:229–235
Janetzko J, Walker S (2014) The making of a sweet modification: structure and function of O-GlcNAc transferase. J Biol Chem 289:34424–34432
van den Brandt PA, Spiegelman D, Yaun SS et al (2000) Pooled analysis of prospective cohort studies on height, weight, and breast cancer risk. Am J Epidemiol 152:514–527
Protani M, Coory M, Martin JH (2010) Effect of obesity on survival of women with breast cancer: systematic review and meta-analysis. Breast Cancer Res Treat 123:627–635
Chan DS, Vieira AR, Aune D et al (2014) Body mass index and survival in women with breast cancer-systematic literature review and meta-analysis of 82 follow-up studies. Ann Oncol 25:1901–1914
Ostrowski A, van Aalten DM (2013) Chemical tools to probe cellular O-GlcNAc signalling. Biochem J 456:1–12
Rilla K, Oikari S, Jokela TA et al (2013) Hyaluronan synthase 1 (HAS1) requires higher cellular UDP-GlcNAc concentration than HAS2 and HAS3. J Biol Chem 288:5973–5983
Tuhkanen H, Anttila M, Kosma VM et al (2004) Genetic alterations in the peritumoral stromal cells of malignant and borderline epithelial ovarian tumors as indicated by allelic imbalance on chromosome 3p. Int J Cancer 109:247–252
Green TM, Alpaugh ML, Barsky SH et al (2015) Breast cancer-derived extracellular vesicles: characterization and contribution to the metastatic phenotype. Biomed Res Int 2015:634865
Coughlin SS, Calle EE, Teras LR et al (2004) Diabetes mellitus as a predictor of cancer mortality in a large cohort of US adults. Am J Epidemiol 159:1160–1167
Acknowledgments
We thank Kari Kotikumpu and Eija Rahunen (Institute of Biomedicine, Anatomy, University of Eastern Finland, Finland) for technical help with O-GlcNAc immunostaining, Tuomas Selander (Science Service Center, Kuopio University Hospital, Finland) for assistance with the statistical analyses, and Ewen MacDonald for English language editing.
Funding
This study was supported by the Special Government Funding (EVO/VTR) of Kuopio University Hospital (Grant Nos. 5654132 and 5053101) and a Grant from Cancer Society of North Savo. The funders were not involved in the collection, management, or analysis of the data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Ethical approval for this study was provided by the Ethics Committee of the University of Eastern Finland and by the National Supervisory Authority for Welfare and Health. The execution of this study complies with the current laws of Finland.
Rights and permissions
About this article
Cite this article
Tiainen, S., Oikari, S., Tammi, M. et al. High extent of O-GlcNAcylation in breast cancer cells correlates with the levels of HAS enzymes, accumulation of hyaluronan, and poor outcome. Breast Cancer Res Treat 160, 237–247 (2016). https://doi.org/10.1007/s10549-016-3996-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-016-3996-4