Abstract
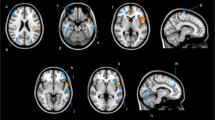
A limited number of studies have associated adjuvant chemotherapy with structural brain changes. These studies had small sample sizes and were conducted shortly after cessation of chemotherapy. Results of these studies indicate local gray matter volume decrease and an increase in white matter lesions. Up till now, it is unclear if non-CNS chemotherapy is associated with long-term structural brain changes. We compared focal and total brain volume (TBV) of a large set of non-CNS directed chemotherapy-exposed breast cancer survivors, on average 21 years post-treatment, to that of a population-based sample of women without a history of cancer. Structural MRI (1.5T) was performed in 184 chemotherapy-exposed breast cancer patients, mean age 64.0 (SD = 6.5) years, who had been diagnosed with cancer on average 21.1 (SD = 4.4) years before, and 368 age-matched cancer-free reference subjects from a population-based cohort study. Outcome measures were: TBV and total gray and white matter volume, and hippocampal volume. In addition, voxel based morphometry was performed to analyze differences in focal gray matter. The chemotherapy-exposed breast cancer survivors had significantly smaller TBV (−3.5 ml, P = 0.019) and gray matter volume (−2.9 ml, P = 0.003) than the reference subjects. No significant differences were observed in white matter volume, hippocampal volume, or local gray matter volume. This study shows that adjuvant chemotherapy for breast cancer is associated with long-term reductions in TBV and overall gray matter volume in the absence of focal reductions. The observed smaller gray matter volume in chemotherapy-exposed survivors was comparable to the effect of almost 4 years of age on gray matter volume reduction. These volume differences might be associated with the slightly worse cognitive performance that we observed previously in this group of breast cancer survivors.
Similar content being viewed by others
References
Ahles TA, Saykin AJ (2007) Candidate mechanisms for chemotherapy-induced cognitive changes. Nat Rev Cancer 7(3):192–201. doi:10.1038/ncr2073
Brown MS, Simon JH, Stemmer SM, Stears JC, Scherzinger A, Cagnoni PJ, Jones RB (1995) MR and proton spectroscopy of white matter disease induced by high-dose chemotherapy with bone marrow transplant in advanced breast carcinoma. Am J Neuroradiol 16(10):2013–2020
Choi SM, Lee SH, Yang YS, Kim BC, Kim MK, Cho KH (2001) 5-Fluorouracil-induced leukoencephalopathy in patients with breast cancer. J Korean Med Sci 16(3):328–334
de Ruiter MB, Reneman L, Boogerd W, Veltman DJ, Caan M, Douaud G, Lavini C, Linn SC, Boven E, van Dam FS, Schagen SB (2011) Late effects of high-dose adjuvant chemotherapy on white and gray matter in breast cancer survivors: converging results from multimodal magnetic resonance imaging. Hum Brain Mapp (in Press) doi:10.1002/hbm.21422
Deprez S, Amant F, Yigit R, Porke K, Verhoeven J, Van den Stock J, Smeets A, Christiaens MR, Leemans A, Van Hecke W, Vandenberghe J, Vandenbulcke M, Sunaert S (2011) Chemotherapy-induced structural changes in cerebral white matter and its correlation with impaired cognitive functioning in breast cancer patients. Hum Brain Mapp 32(3):480–493. doi:10.1002/hbm.21033
Abraham J, Haut MW, Moran MT, Filburn S, Lemiuex S, Kuwabara H (2008) Adjuvant chemotherapy for breast cancer: effects on cerebral white matter seen in diffusion tensor imaging. Clin Breast Cancer 8(1):88–91
Inagaki M, Yoshikawa E, Matsuoka Y, Sugawara Y, Nakano T, Akechi T, Wada N, Imoto S, Murakami K, Uchitomi Y (2007) Smaller regional volumes of brain gray and white matter demonstrated in breast cancer survivors exposed to adjuvant chemotherapy. Cancer 109(1):146–156. doi:10.1002/cncr.22368
Yoshikawa E, Matsuoka Y, Inagaki M, Nakano T, Akechi T, Kobayakawa M, Fujimori M, Nakaya N, Akizuki N, Imoto S, Murakami K, Uchitomi Y (2005) No adverse effects of adjuvant chemotherapy on hippocampal volume in Japanese breast cancer survivors. Breast Cancer Res Treat 92(1):81–84. doi:10.1007/s10549-005-1412-6
McDonald BC, Conroy SK, Ahles TA, West JD, Saykin AJ (2010) Gray matter reduction associated with systemic chemotherapy for breast cancer: a prospective MRI study. Breast Cancer Res Treat 123(3):819–828. doi:10.1007/s10549-010-1088-4
Brown MS, Stemmer SM, Simon JH, Stears JC, Jones RB, Cagnoni PJ, Sheeder JL (1998) White matter disease induced by high-dose chemotherapy: longitudinal study with MR imaging and proton spectroscopy. Am J Neuroradiol 19(2):217–221
Centers for Disease C, Prevention (2011) Cancer survivors–United States, 2007. Morb Mortal Wkly Rep 60(9):269–272
de Ruiter MB, Reneman L, Boogerd W, Veltman DJ, van Dam FS, Nederveen AJ, Boven E, Schagen SB (2010) Cerebral hyperesponsiveness and cognitive impairment 10 years after chemotherapy for breast cancer. Hum Brain Mapp 32(8):1206–1219. doi:10.1002/hbm.21102
Nash M, Pribiag H, Fournier AE, Jacobson C (2009) Central nervous system regeneration inhibitors and their intracellular substrates. Mol Neurobiol 40(3):224–235. doi:10.1007/s12035-009-8083-y
Koppelmans V, Schagen SB, Poels MM, Boogerd W, Seynaeve C, Lugt AV, Breteler MM (2011) Incidental findings on brain magnetic resonance imaging in long-term survivors of breast cancer treated with adjuvant chemotherapy. Eur J Cancer doi: 10.1016/j.ejca.2011.06.026
Hofman A, Breteler MM, van Duijn CM, Janssen HL, Krestin GP, Kuipers EJ, Stricker BH, Tiemeier H, Uitterlinden AG, Vingerling JR, Witteman JC (2009) The Rotterdam Study: 2010 objectives and design update. Eur J Epidemiol 24(9):553–572. doi:10.1007/s10654-009-9386-z
Ikram MA, van der Lugt A, Niessen WJ, Krestin GP, Koudstaal PJ, Hofman A, Breteler MM, Vernooij MW (2011) The Rotterdam scan study: design and update up to 2012. Eur J Epidemiol 26(10):811–824. doi:10.1007/s10654-011-9624-z
Ikram MA, Vrooman HA, Vernooij MW, van der Lijn F, Hofman A, van der Lugt A, Niessen WJ, Breteler MM (2008) Brain tissue volumes in the general elderly population. The Rotterdam scan study. Neurobiol Aging 29(6):882–890. doi:10.1016/j.neurobiolaging.2006.12.012
Radloff LS (1977) The CES-D scale: a self report depression scale for research in the genetal population. Appl Psychol Meas 1:385–401
Klein A, Andersson J, Ardekani BA, Ashburner J, Avants B, Chiang MC, Christensen GE, Collins DL, Gee J, Hellier P, Song JH, Jenkinson M, Lepage C, Rueckert D, Thompson P, Vercauteren T, Woods RP, Mann JJ, Parsey RV (2009) Evaluation of 14 nonlinear deformation algorithms applied to human brain MRI registration. Neuroimage 46(3):786–802. doi:10.1016/j.neuroimage.2008.12.037
van Tol MJ, van der Wee NJ, van den Heuvel OA, Nielen MM, Demenescu LR, Aleman A, Renken R, van Buchem MA, Zitman FG, Veltman DJ (2010) Regional brain volume in depression and anxiety disorders. Arch Gen Psychiatry 67(10):1002–1011. doi:10.1001/archgenpsychiatry.2010.121
van der Lijn F, den Heijer T, Breteler MM, Niessen WJ (2008) Hippocampus segmentation in MR images using atlas registration, voxel classification, and graph cuts. Neuroimage 43(4):708–720. doi:10.1016/j.neuroimage.2008.07.058
Coffey CE, Saxton JA, Ratcliff G, Bryan RN, Lucke JF (1999) Relation of education to brain size in normal aging: implications for the reserve hypothesis. Neurology 53(1):189–196
Dotson VM, Davatzikos C, Kraut MA, Resnick SM (2009) Depressive symptoms and brain volumes in older adults: a longitudinal magnetic resonance imaging study. J Psychiatry Neurosci 34(5):367–375
Han R, Yang YM, Dietrich J, Luebke A, Mayer-Proschel M, Noble M (2008) Systemic 5-fluorouracil treatment causes a syndrome of delayed myelin destruction in the central nervous system. J Biol 7(4):12. doi:10.1186/jbiol69
Seigers R, Schagen SB, Beerling W, Boogerd W, van Tellingen O, van Dam FS, Koolhaas JM, Buwalda B (2008) Long-lasting suppression of hippocampal cell proliferation and impaired cognitive performance by methotrexate in the rat. Behav Brain Res 186(2):168–175. doi:10.1016/j.bbr.2007.08.004
Koppelmans V, Breteler MMB, Boogerd W, Seynaeve C, Gundy C, Schagen SB (2011) Neuropsychological performance in breast cancer survivors more than 20 years after adjuvant chemotherapy. Journal of Clinical Oncology accepted for publication
Yamada TH, Denburg NL, Beglinger LJ, Schultz SK (2010) Neuropsychological outcomes of older breast cancer survivors: cognitive features ten or more years after chemotherapy. J Neuropsychiatry Clin Neurosci 22(1):48–54. doi:10.1176/appi.neuropsych.22.1.48
Dietrich J, Han R, Yang Y, Mayer-Proschel M, Noble M (2006) CNS progenitor cells and oligodendrocytes are targets of chemotherapeutic agents in vitro and in vivo. J Biol 5(7):22. doi:10.1186/jbiol50
Joshi G, Sultana R, Tangpong J, Cole MP, St Clair DK, Vore M, Estus S, Butterfield DA (2005) Free radical mediated oxidative stress and toxic side effects in brain induced by the anti cancer drug adriamycin: insight into chemobrain. Free Radic Res 39(11):1147–1154. doi:10.1080/10715760500143478
Acknowledgment
This research was supported by a grant from the Dutch Cancer Society (2007-3797) to SBS and MMBB.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Monique M. B. Breteler and Sanne B. Schagen contributed equally.
Rights and permissions
About this article
Cite this article
Koppelmans, V., de Ruiter, M.B., van der Lijn, F. et al. Global and focal brain volume in long-term breast cancer survivors exposed to adjuvant chemotherapy. Breast Cancer Res Treat 132, 1099–1106 (2012). https://doi.org/10.1007/s10549-011-1888-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-011-1888-1