Abstract
Aim
Women aged 25–35 years, for whom cervical cancer is most problematic, are least likely to participate in the cervical screening programme. Therefore, identifying barriers to screening participation in this high-risk group is essential.
Subject and methods
A sample of 430 women completed an electronic survey of their cervical screening history and answered questions on sociodemographic, behavioural, attitudinal and informational barriers to cervical screening uptake. Logistic regression was used to predict cervical screening non attendance.
Results
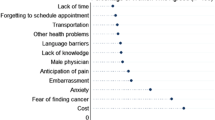
Women with more than 10 sexual partners in their lifetime were more likely, but women from ethnic minorities, less likely to participate in the cervical screening programme. Women unaware of the recommended screening interval were also less likely to be screened, as were women who believed that screening is a test for cancer. Screening was also less likely among women who endorsed the belief that screening in the absence of symptoms is unnecessary.
Conclusion
These data highlight poor knowledge of the recommended screening interval and purpose of cervical cancer screening in this high-risk group. As such, interventions that target these informational barriers might be most effective for increasing cervical screening uptake in this high-risk group.
Similar content being viewed by others
References
Amankwah E, Ngwakongnwi E, Quan H (2009) Why many visible minority women in Canada do not participate in cervical cancer screening. Ethnicity Health 14(4):337–349
Bang JY, Yadegarfar G, Soljak M, Majeed A (2012) Primary care factors associated with cervical screening coverage in England. J Public Health 34:532–538
CR-UK (2010) Cervical cancer incidence statistics. http://www.cancerresearchuk.org/cancerinfo/cancerstats/types/cervix/incidence/. Accessed 6 Jan 2014
Eaker S, Adami H, Spare P (2001) Reasons women do not attend screening for cervical cancer: a population-based study in Sweden. Prev Med 32:482–491
El-Hadad ARM (2005) Effect of a supportive educational intervention on cervical cancer screening for minority women. PhD Thesis, University of California, Los Angeles
Franceschi S et al (2009) Differences in the risk of cervical cancer and human papillomavirus infection by education level. Brit J Cancer 101:865–870
Hansen BT et al (2011) Factors associated with non-attendance, opportunistic attendance and reminded attendance to cervical screening in an organized screening program: a cross sectional study of 12,058 Norwegian women. BMC Public Health 11:264
Lancuck L et al (2010) A fall-off in cervical screening coverage of younger women in developed countries. J Med Screen 17(2):91–96
Lostao L, Joiner TE, Pettit JW (2001) Health beliefs and illness attitudes as predictors of breast cancer screening attendance. Eur J Public Health 11:274–279
NHSCSP (2012) NHS Cancer Screening Programme, Annual review. http://www.cancerscreening.nhs.uk/cervical/publications/2012review.html. Accessed 15 Dec 2013
Olesen SC, Butterworth P, Jacomb P, Tait RJ (2012) Personal factors influence use of cervical cancer screening services: epidemiological survey and linked administrative data address the limitations of previous research. BMC Health Serv Res 12:34
Oscarsson MG, Wijma BE, Benzein EG (2008) I do not need to… I do not want to… I do not give it priority…why women choose not to attend cervical cancer screening. Health Expec 11:26–34
Peto J, Gilham C, Fletcher O, Matthews FE (2004) The cervical cancer epidemic that screening has prevented in the UK. Lancet 364(9430):249–256
Rimer B (1999) The impact of tailored interventions on a community health centre population. Patient Educ Counsel 37:125–140
Tacken MAJB et al (2006) Uptake of cervical cancer screening in the Netherlands is mainly influenced by women’s beliefs about the screening and by the inviting organization. Eur J Public Health 17(2):178–185
Waller J, Jackowska M, Marlow L, Wardle J (2012) Exploring age differences in reasons for nonattendance for cervical screening: a qualitative study. BJOG 119:26–32
Wong LP, Wong YL, Low WY, Khoo EM, Shuib R (2008) Cervical cancer screening attitudes and beliefs of Malaysian women who have never had a pap smear: a qualitative study. Int J Behav Med 15:289–292
Acknowledgements
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest
All authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 38 kb)
Rights and permissions
About this article
Cite this article
Lovell, B., Wetherell, M.A. & Shepherd, L. Barriers to cervical screening participation in high-risk women. J Public Health 23, 57–61 (2015). https://doi.org/10.1007/s10389-014-0649-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-014-0649-0