Abstract
Aim
One of the contemporary debates between science and economics is concerned with why, and to what extent, financial cost and economic efficiency considerations affect scientific inquiry into possible solutions to human illnesses. This study inquires into clinical drug trials for multiple sclerosis (MS) in the European Union to determine the validity of a prevailing claim, advanced in the medical community, that the clinical efficacy of these drugs is undermined by cost and efficiency considerations.
Subjects and methods
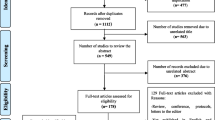
The first part of the study is devoted to a review of pharmacoeconomic literature (2000–2012) on clinical drug testing for MS, particularly in the member countries of the European Union. The second part presents survey results of discontinued clinical trials that we gathered from European Union registries.
Results
The study finds that cost and efficiency considerations exist in a limited number of trials in the European Union. Specifically, about 1/5 of MS drugs do not reach the pharmaceutical markets even if there may be some supporting efficacy data, or negative safety data is absent, during testing/experimentation. Their direct and controlling impact on decisions to withdraw suspend or prematurely terminate (as well as initiate) clinical testing and efficacy data collection for MS does not appear to be consistent. However, these could extend prevailing theoretical debates about the proper scope of clinical drug efficacy in MS.
Conclusion
The study suggests that pharmacoeconomic approaches to clinical efficacy help broaden and enhance our understanding and choices of disease management options for MS sufferers, their families and health care providers in the European Union and elsewhere. Finally, there is some empirical evidence to indicate an inverse relationship between transaction costs and drug marketability: The higher the transaction costs of clinical testing, the lower is the drug's potential for funding and eventual marketing

Similar content being viewed by others
References
Baumhackl U, Kappos L, Radue EW, Freitag P, Guseo A, Daumer M, Mertin J (2005) A randomized, double-blind, placebo controlled study of oral hydrolytic enzymes in relapsing multiple sclerosis. Mult Scler 11:166–168
Bryant J, Clegg A, Milne R (2001) Systematic review of immunomodulatory drugs for the treatment of people with multiple sclerosis: is there good quality evidence on effectiveness and cost? J Neurol Neurosurg Psychiatry 70:574–579
CAMMS223 Trial Investigators, Coles AJ, Compston DA, Selmaj KW, Lake SL, Moran S, Margolin DH, Norris K, Tandon PK (2008) Alemtuzumab vs. interferon beta-1a in early multiple sclerosis. N Engl J Med 359:1786–1801
Chilcott J, McCabe C, Tappenden P, O’Hagan A, Cooper NJ, Abrams K, Claxton K (2003) Modelling the cost effectiveness of interferon beta and glatiramer acetate in the management of multiple sclerosis. BMC 326:522–526
Coase R (1937) The nature of the firm. Economica 4:386–405
Couzin J (2005) Drug discovery: magnificent obsession. Science 307:1712–1715
Curtiss FR (2007) Pharmacoeconomic modeling of drug therapies for multiple sclerosis: are we building houses on sand? J Manag Care Pharm 13:245–261
Dahlman CJ (1979) The problem of externality. J Law Econ 21:141–162
European Union Clinical Trials Register, https://www.clinicaltrialsregister.eu/ctr-search/search?query=multiple+sclerosis. Accessed February 24, 2012
Fuller GN, Bone I (2001) Disease modifying treatment in multiple sclerosis. J Neurol Neurosurg Psychiatry 71:i20–ii21
Hauser S (1994) Multiple sclerosis and other demyelinating diseases. In: Isselbacher KJ, Martin JB, Fauci AS (eds) Harrison’s principles of internal medicine. McGraw-Hill, New York, pp 2287–2295
Holmoy T, Celius EG (2008) Cost-effectiveness of natalizumab in multiple sclerosis. Expert Rev Pharm Outcomes Res 8:11–21
Kendrick M, Johnson KI (2000) Long-term treatment of multiple sclerosis with interferon may be cost effective. PharmacoEconomics 18:45–53
Kleinschnitz C, Meuth SG, Wiendl H (2008) The trials and errors in MS therapy. Int MS J 15:79–90
MacLean HJ, Freedman MS (2001) Immunologic therapy for relapsing-remitting multiple sclerosis. Curr Neurol Neurosci Rep 1:277–285
Maggon K (2010) Daclizumab (Biogen, Abbott) Review: multiple sclerosis. http://knol.google.com/k/daclizumab-biogen-abbott-review-multiple-sclerosis#Clinical_trials. Accessed July 11, 2011
National Institute of Neurological Disorders and Stroke (NINDS) Multiple sclerosis information page. http://www.ninds.nih.gov/disorders/multiple_sclerosis/multiple_sclerosis.htm. Accessed May 13, 2007
O’Connor PS, Goodman AD, Kappos L, Lublin FD, Miller DH, Polman CH, Rudick RA, Forrestal F, Jurgensen S, Panzara MA, Sandrock AW (2009) Return of disease activity after cessation of natalizumab. Mult Scler 15:S240
Pugliatti M, Rosati G, Carton H, Riise T, Drulovic J, Vecsei L, Milanov I (2006) The epidemiology of multiple sclerosis in Europe. Eur J Neurol 13:700–722
Ryan M (2008) Multiple sclerosis. In: Dipiro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey LM (eds) Pharmacotherapy a pathophysiologic approach. McGraw Hill, New York, pp 431–441
Sorensen PS, Mellgren SI, Svenningsson A, Elovaara I, Frederiksen JL, Beiske AG, Myhr KM, Søgaard LV, Olsen IC, Sandberg-Wollheim M (2009) NORdic trial of oral Methylprednisolone as add-on therapy to Interferon beta-1a for treatment of relapsing-remitting multiple sclerosis (NORMIMS study): a randomised, placebo-controlled trial. Lancet Neurol 8:519–529
Tan IL, Lycklama à Nijeholt GJ, Polman CH, Adèr HJ, Barkhof F (2000) Linomide in the treatment of multiple sclerosis: MRI results from prematurely terminated phase-III trials. Mult Scler 6:99–104
Weinshenker BG, Noseworthy JH (2001) Multiple sclerosis: study design, sample sizes and pitfalls. In: Guiloff RJ (ed) Clinical trials in neurology. Springer, London, pp 371–386
Wiendl H, Hohlfeld R (2002) Therapeutic approaches in multiple sclerosis: lessons from failed and interrupted treatment trials. BioDrugs 16:183–200
Wiendl H, Neuhaus O, Kappos L, Hohlfeld R (2000) Multiple sclerosis: current review of failed and discontinued clinical trials of drug treatment. Nervenarzt 71:597–610
Conflict of interest
The author declares that no conflict of interest exists.
Financial disclosure
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mendoza, R.L. Pharmacoeconomics and clinical trials in multiple sclerosis: baseline data from the European Union. J Public Health 22, 211–218 (2014). https://doi.org/10.1007/s10389-013-0561-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-013-0561-z