Abstract
Introduction
All elderly Germans are legally obliged to have health insurance. About 90 % of this population are members of social health insurances (SHI) whose premiums are generally income-related and independent of health status. For most of these members, holding social health insurance is mandatory. As a consequence, genuine information about preferences for health insurance is not available. The aim of this study was therefore to determine and analyze the willingness to pay (WTP) for health insurance among elderly Germans.
Methods
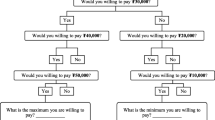
Data from a population-based 8-year follow-up of a large cohort study conducted in the Saarland, Germany was used. Participants aged 57–84 years passed a geriatric assessment and responded to a health economic questionnaire. Individuals’ WTP was elicited based on a contingent valuation method with a payment card.
Results
Mean monthly WTP per capita for health insurance amounted to €260. This corresponded to about 20 % of individual disposable income. Regression analyses showed that WTP increased significantly with higher income, male gender, higher educational level, and privately insured status. In contrast, neither increasing morbidity level nor higher individual health care costs influenced WTP significantly.
Discussion
The relatively large extent of average WTP for health insurance indicates that the elderly would probably accept higher contributions to SHI rather than policy efforts to reduce contributions. The identified determinants of WTP might indicate that elderly generally approve the principle of solidarity of the SHI with contributions depending on income rather than morbidity.
Similar content being viewed by others
References
Binam, J., Onana, Y., Nkelzok, V.R.: Community prepayment of health care and estimation of the willingness to pay in Cameroon: evidence of rural households in the Centre region. Institute of Agricultural Research for Development, Yaounde (2004)
Binam, J., Nkama, A.N., Nkenda, R.: Estimating the Willingness to Pay for Community Health Prepayment Schemes in Rural Area: A Case Study of the Use of Contingent Valuation Surveys in Central Cameroon. Institute of Agricultural Research for Development, Yaounde (2004)
Mathiyazaghan, K.: Willingness to pay for rural health insurance through community participation in India. Int. J. Health Plan. Manag. 13(1), 47–67 (1998)
Jain, A., Swetha, S., Johar, Z., Raghavan, R.: Acceptability of, and Willingness to pay for, Community Health Insurance in Rural India. J. Epidemiol. Glob. Health 4(3), 159–167 (2014)
Dror, D.M., Radermacher, R., Koren, R.: Willingness to pay for health insurance among rural and poor persons: field evidence from seven micro health insurance units in India. Health Policy 82(1), 12–27 (2007)
Asgary, A., Willis, K., Taghvaei, A.A., Rafeian, M.: Estimating rural households’ willingness to pay for health insurance. Eur. J. Health Econ. 5(3), 209–215 (2004)
Ataguba, J., Ichoku, E.H., Fonta, W., Okpanachi, A., Okon, U.: An estimation of the willingness to pay for community healthcare risk-sharing prepayment scheme and the medical poverty trap: evidence from rural Nigeria. In: 5th Poverty and Economic Policy (PEP) Research Network General Meeting (2006)
Onwujekwe, O., Okereke, E., Onoka, C., Uzochukwu, B., Kirigia, J., Petu, A.: Willingness to pay for community-based health insurance in Nigeria: do economic status and place of residence matter? Health Policy Plan. 25(2), 155–161 (2010)
Dong, H., Kouyate, B., Cairns, J., Sauerborn, R.: Differential willingness of household heads to pay community-based health insurance premia for themselves and other household members. Health Policy Plan. 19(2), 120–126 (2004)
Dong, H., Kouyate, B., Cairns, J., Mugisha, F., Sauerborn, R.: Willingness-to-pay for community-based insurance in Burkina Faso. Health Econ. 12(10), 849–862 (2003)
Dong, H., Kouyate, B., Cairns, J., Sauerborn, R.: Inequality in willingness-to-pay for community-based health insurance. Health Policy 72(2), 149–156 (2005)
Dong, H., Kouyate, B., Snow, R., Mugisha, F., Sauerborn, R.: Gender’s effect on willingness-to-pay for community-based insurance in Burkina Faso. Health Policy 64(2), 153–162 (2003)
Asenso-Okyere, W.K., Osei-Akoto, I., Anum, A., Appiah, E.N.: Willingness to pay for health insurance in a developing economy. A pilot study of the informal sector of Ghana using contingent valuation. Health Policy 42(3), 223–237 (1997)
Gustafsson-Wright, E., Asfaw, A., van der Gaag, J.: Willingness to pay for health insurance: an analysis of the potential market for new low-cost health insurance products in Namibia. Soc. Sci. Med. 69(9), 1351–1359 (2009)
Khan, J.A., Ahmed, S.: Impact of educational intervention on willingness-to-pay for health insurance: a study of informal sector workers in urban Bangladesh. Health Econ. Rev. 3(1), 1–10 (2013)
Ying, X.H., Hu, T.W., Ren, J., Chen, W., Xu, K., Huang, J.H.: Demand for private health insurance in Chinese urban areas. Health Econ. 16(10), 1041–1050 (2007)
Bärnighausen, T., Liu, Y., Zhang, X., Sauerborn, R.: Willingness to pay for social health insurance among informal sector workers in Wuhan, China: a contingent valuation study. BMC Health Serv. Res. 7(1), 114 (2007)
Bustamante, A.V., Ojeda, G., Castaneda, X.: Willingness to pay for cross-border health insurance between the United States and Mexico. Health Aff. (Millwood) 27(1), 169–178 (2008)
Block, M.A.G., Bustamante, A.V., de la Sierra, L.A., Cardoso, A.M.: Redressing the limitations of the affordable Care Act for Mexican immigrants through bi-national health insurance: a willingness to pay study in Los Angeles. J. Immigr. Minor. Health 16(2), 179–188 (2012)
Shafie, A., Hassali, M.: Willingness to pay for voluntary community-based health insurance: findings from an exploratory study in the state of Penang, Malaysia. Soc. Sci, Med (2013)
Passon, A., Lüngen, M., Gerber, A., Redaelli, M., Stock, S.: Das Krankenversicherungssystem in Deutschland. In: Lauterbach, K.W., Stock, S., Brunner, H. (eds.) Gesundheitsökonomie, pp. 105–136. Verlag Hans Huber, Bern (2009)
Statistisches Bundesamt: Bevölkerung Deutschlands bis 2060–2012. koordinierte Bevölkerungsvorausberechnung. Statistisches Bundesamt, Wiesbaden (2009)
Breyer, F., Felder, S.: Life expectancy and health care expenditures: a new calculation for Germany using the costs of dying. Health Policy (Amsterdam, Netherlands) 75(2), 175–186 (2006)
Löw, M., Stegmaier, C., Ziegler, H., Rothenbacher, D., Brenner, H.: Epidemiological investigations of the chances of preventing, recognizing early and optimally treating chronic diseases in an elderly population (ESTHER study). Dtsch. Med. Wochenschr. 129(49), 2643–2647 (2004). doi:10.1055/s-2004-836089
Roick, C., Kilian, R., Matschinger, H., Bernert, S., Mory, C., Angermeyer, M.C.: German adaptation of the client sociodemographic and service receipt inventory—an instrument for the cost of mental health care. Psychiatr. Prax. 28(Suppl 2), S84–S90 (2001)
König, H.H., Born, A., Heider, D., Matschinger, H., Heinrich, S., Riedel-Heller, S.G., Surall, D., Angermeyer, M.C., Roick, C.: Cost-effectiveness of a primary care model for anxiety disorders. Br. J. Psychiatry 195(4), 308–317 (2009)
Klose, T.: The contingent valuation method in health care. Health Policy 47(2), 97–123 (1999)
Olsen, J.A., Smith, R.D.: Theory versus practice: a review of ‘willingness-to-pay’ in health and health care. Health Econ. 10(1), 39–52 (2001)
Ryan, M., Scott, D., Reeves, C., Bate, A., Van Teijlingen, E., Russell, E., Napper, M., Robb, C.: Eliciting public preferences for healthcare: a systematic review of techniques. Health Technology Assessment (Winchester, England) 5(5), 1 (2001)
Bayoumi, A.M.: The measurement of contingent valuation for health economics. Pharmacoeconomics 22(11), 691–700 (2004)
Smith, R.D.: Construction of the contingent valuation market in health care: a critical assessment. Health Econ. 12(8), 609–628 (2003)
Heider, D., Matschinger, H., Müller, H., Saum, K.-U., Quinzler, R., Haefeli, W.E., Wild, B., Lehnert, T., Brenner, H., König, H.-H.: Health care costs in the elderly in Germany: an analysis applying Andersen’s behavioral model of health care utilization. BMC Health Serv. Res 14(1), 71 (2014)
Linn, B.S., Linn, M.W., Gurel, L.: Cumulative illness rating scale. J. Am. Geriatr. Soc. 16(5), 622–626 (1968)
Miller, M., Paradis, C., Houck, P., Mazumdar, S., Stack, J., Rifai, A., Mulsant, B., Reynolds, C.: Rating chronic medical illness burden in geropsychiatric practice and research: application of the Cumulative Illness Rating Scale. Psychiatry Res. 41(3), 237–248 (1992)
Cameron, T.A.: The impact of grouping coarseness in alternative grouped-data regression models. J. Econom. 35(1), 37–57 (1987)
Manning, W.G.: The logged dependent variable, heteroscedasticity, and the retransformation problem. J. Health Econ. 17(3), 283–295 (1998)
Long, J.S., Ervin, L.H.: Using heteroscedasticity consistent standard errors in the linear regression model. Am. Stat. 54(3), 217–224 (2000)
Efron, B., Tibshirani, R.: Bootstrap methods for standard errors, confidence intervals, and other measures of statistical accuracy. Stat. Sci. 1, 54–75 (1986)
O’Brien, B.J., Drummond, M.F., Labelle, R.J., Willan, A.: In search of power and significance: issues in the design and analysis of stochastic cost-effectiveness studies in health care. Med. Care 32(2), 150–163 (1994)
White, I.R., Royston, P., Wood, A.M.: Multiple imputation using chained equations: issues and guidance for practice. Stat. Med. 30(4), 377–399 (2011)
Graham, J.W., Olchowski, A.E., Gilreath, T.D.: How many imputations are really needed? Some practical clarifications of multiple imputation theory. Prev. Sci. 8(3), 206–213 (2007)
Bundesministerium für Finanzen: Lohn- und Einkommenssteuerrechner. https://www.bmf-steuerrechner.de/bl2009/? (2014). Accessed 14 February 2014
Acknowledgments
This study was funded by the German Federal Ministry of Education and Research (Grant numbers 01ET0717, 01ET0718, 01ET0719, 01ET1004A, 01ET1004B, 01ET1004C).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bock, JO., Heider, D., Matschinger, H. et al. Willingness to pay for health insurance among the elderly population in Germany. Eur J Health Econ 17, 149–158 (2016). https://doi.org/10.1007/s10198-014-0663-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10198-014-0663-8