Abstract
Background
Serum uric acid level is regulated by gender, dietary habit, genetic predisposition, and renal function, and is associated with the development of renal and cardiovascular diseases. This study prospectively investigated the association between serum uric acid levels and mortality in a community-based population.
Methods
Three thousand four hundred and eighty-seven subjects regardless of the antihyperuricemic medication (45 % male; mean age 62 years old) from the Takahata town in Japan participated in this study and were followed up for 8 years (median 7.5 years). We examined the association between serum uric acid levels at baseline and the all-cause and cardiovascular mortality, respectively, in this population.
Results
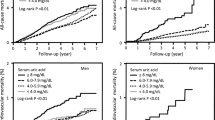
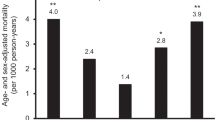
One hundred seventy-nine subjects died during the follow-up period, with 49 deaths attributed to cardiovascular causes. Kaplan–Meier analysis revealed that the all-cause mortality was significantly higher along with the increase in serum uric acid levels at baseline among female (Log-rank P < 0.01), but not male subjects (P = 0.97). Cox-proportional hazard model analysis with adjustment for possible confounders including age, renal function, and comorbidities revealed that hyperuricemia (uric acid ≥7.0 mg/dL) was an independent risk factor for all-cause and cardiovascular mortality, respectively, in female [hazard ratio (HR) 5.92, 95 % confidence interval (CI) 2.10–14.6 for all-cause mortality, and HR 10.7, 95 % CI 1.76–50.2 for cardiovascular mortality], but not male subjects.
Conclusion
Hyperuricemia was an independent risk for all-cause and cardiovascular mortality in female, but not among the male subjects in a community-based population.



Similar content being viewed by others
References
Hsu CY, Iribarren C, McCulloch CE, Darbinian J, Go AS. Risk factors for end-stage renal disease: 25-year follow-up. Arch Intern Med. 2009;169:342–50.
Zhao G, Huang L, Song M, Song Y. Baseline serum uric acid level as a predictor of cardiovascular disease related mortality and all-cause mortality: a meta-analysis of prospective studies. Atherosclerosis. 2013;231:61–8.
Niskanen LK, Laaksonen DE, Nyyssönen K, et al. Uric acid level as a risk factor for cardiovascular and all-cause mortality in middle-aged men. Arch Intern Med. 2004;164:1546–51.
Kim SY, Guevara JP, Kim KM, Choi HK, Heitjan DF, Albert DA. Hyperuricemia and risk of stroke: a systematic review and meta-analysis. Arthritis Care Res. 2009;61:885–92.
Li M, Hou W, Zhang X, Hu L, Tang Z. Hyperuricemia and risk of stroke: a systematic review and meta-analysis of prospective studies. Atherosclerosis. 2014;232:265–70.
Tomita M, Mizuno S, Yamanaka H, et al. Does hyperuricemia affect mortality? A prospective cohort study of Japanese male workers. J Epidemiol. 2000;10:403–9.
Sakata K, Hashimoto T, Ueshima H, et al. Absence of an association between serum uric acid and mortality from cardiovascular disease: NIPPON DATA 80, 1980–1994. National integrated projects for prospective observation of non-communicable diseases and its trend in the aged. Eur J Epidemiol. 2001;17:461–8.
Palmer TM, Nordestgaard BG, Benn M, et al. Association of plasma uric acid with ischaemic heart disease and blood pressure: mendelian randomization analysis of two large cohorts. BMJ. 2013;347:f4262.
Freedman DS, Williamson DF, Gunter EW, Byers T. Relation of serum uric acid to mortality and ischemic heart disease. Am J Epidemiol. 1995;141:637–44.
Fang J, Alderman MH. Serum uric acid and cardiovascular mortality: the NHANES I epidemiologic follow-up study, 1971–1992. National health and nutrition examination survey. JAMA. 2000;283:2404–10.
Kim SY, Guevara JP, Kim KM, Choi HK, Heitjan DF, Albert DA. Hyperuricemia and coronary heart disease: a systematic review and meta-analysis. Arthritis Care Res (Hoboken). 2010;62:170–80.
Dawson J, Jeemon P, Hetherington L, et al. Serum uric acid level, longitudinal blood pressure, renal function, and long-term mortality in treated hypertensive patients. Hypertension. 2013;62:105–11.
Iseki K, Ikemiya Y, Inoue T, Iseki C, Kinjo K, Takishita S. Significance of hyperuricemia as a risk factor for developing ESRD in a screened cohort. Am J Kidney Dis. 2004;44:642–50.
Madero M, Sarnak MJ, Wang X, et al. Uric acid and long-term outcomes in CKD. Am J Kidney Dis. 2009;53:796–803.
Konta T, Kudo K, Sato H, et al. Albuminuria is an independent predictor of all-cause and mortality in the Japanese population: the Takahata study. Clin Exp Nephrol. 2013;6:805–10.
WHO/IASO/IOTF. The Asia–Pacific perspective: redefining obesity and its treatment. Health Communications Australia Pty Ltd, 2000, pp. 15–21.
Matsuo S, Imai E, Horio M, et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53:982–92.
Antón FM, García Puig J, Ramos T, González P, Ordás J, et al. Sex differences in uric acid metabolism in adults: evidence for a lack of influence of estradiol-17 beta (E2) on the renal handling of urate. Metabolism. 1986;35:343–8.
Khosla S, Melton LJ, Atkinson EJ, O’Fallon WM. Relationship of serum sex steroid levels to longitudinal changes in bone density in young versus elderly men. J Clin Endocrinol Metab. 2013;86:3555–61.
McCord JM. Oxygen-derived free radicals in postischemic tissue injury. N Engl J Med. 1985;312:159–63.
Yu MA, Sánchez-Lozada LG, Johnson RJ, Kang DH. Oxidative stress with an activation of the renin-angiotensin system in human vascular endothelial cells as a novel mechanism of uric acid-induced endothelial dysfunction. J Hypertens. 2010;28:1234–42.
Kang DH, Park SK, Lee IK, Johnson RJ. Uric acid-induced C-reactive protein expression: implication on cell proliferation and nitric oxide production of human vascular cells. J Am Soc Nephrol. 2005;16:3553–62.
Acknowledgments
This study was supported in part by a Grant-in-Aid from the 21st Century Center of Excellence (COE) and Global COE program of the Japan Society for the Promotion of Science and by a Grant-in-Aid for Scientific Research (C) (15K09240).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All of the authors declare no competing financial interests.
About this article
Cite this article
Kamei, K., Konta, T., Ichikawa, K. et al. Serum uric acid levels and mortality in the Japanese population: the Yamagata (Takahata) study. Clin Exp Nephrol 20, 904–909 (2016). https://doi.org/10.1007/s10157-016-1228-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-016-1228-1