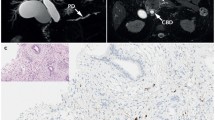
Abstract
Biliary epithelial cells preferentially respond to various insults under chronic pathological conditions leading to reactively atypical changes, hyperplasia, or the development of biliary neoplasms (such as biliary intraepithelial neoplasia, intraductal papillary neoplasm of the bile duct, and cholangiocarcinoma). Moreover, benign biliary strictures can be caused by a variety of disorders (such as IgG4-related sclerosing cholangitis, eosinophilic cholangitis, and follicular cholangitis) and often mimic malignancies, despite their benign nature. In addition, primary sclerosing cholangitis is a well-characterized precursor lesion of cholangiocarcinoma and many other chronic inflammatory disorders increase the risk of malignancies. Because of these factors and the changes in biliary epithelial cells, biliary strictures frequently pose a diagnostic challenge. Although the ability to differentiate neoplastic from non-neoplastic biliary strictures has markedly progressed with the advance in radiological modalities, brush cytology and bile duct biopsy examination remains effective. However, no single modality is adequate to diagnose benign biliary strictures because of the low sensitivity. Therefore, understanding the underlying causes by compiling the entire clinical, laboratory, and imaging data; considering the under-recognized causes; and collaborating between experts in various fields including cytopathologists with multiple approaches is necessary to achieve an accurate diagnosis.



Similar content being viewed by others
References
Bowlus CL, Olson KA, Gershwin ME (2016) Evaluation of indeterminate biliary strictures. Nat Rev Gastroenterol Hepatol 13(1):28–37
Katabathina VS, Dasyam AK, Dasyam N, Hosseinzadeh K (2014) Adult bile duct strictures: role of MR imaging and MR cholangiopancreatography in characterization. Radiographics 34(3):565–586
Kirchner GI, Rummele P (2015) Update on sclerosing cholangitis in critically Ill patients. Viszeralmedizin 31(3):178–184
Nashed C, Sakpal SV, Shusharina V, Chamberlain RS (2010) Eosinophilic cholangitis and cholangiopathy: a sheep in wolves clothing. HPB Surg 2010:906496
Lee JY, Lim JH, Lim HK (2005) Follicular cholangitis mimicking hilar cholangiocarcinoma. Abdom Imaging 30(6):744–747
Zepeda-Gomez S, Baron TH (2011) Benign biliary strictures: current endoscopic management. Nat Rev Gastroenterol Hepatol 8(10):573–581
Kaffes AJ (2015) Management of benign biliary strictures: current status and perspective. J Hepatobiliary Pancreat Sci 22(9):657–663
Navaneethan U, Njei B, Lourdusamy V, Konjeti R, Vargo JJ, Parsi MA (2015) Comparative effectiveness of biliary brush cytology and intraductal biopsy for detection of malignant biliary strictures: a systematic review and meta-analysis. Gastrointest Endosc 81(1):168–176
Nanda A, Brown JM, Berger SH, Lewis MM, Barr Fritcher EG, Gores GJ, Keilin SA, Woods KE, Cai Q, Willingham FF (2015) Triple modality testing by endoscopic retrograde cholangiopancreatography for the diagnosis of cholangiocarcinoma. Therap Adv Gastroenterol 8(2):56–65
Sadeghi A, Mohamadnejad M, Islami F, Keshtkar A, Biglari M, Malekzadeh R, Eloubeidi MA (2016) Diagnostic yield of EUS-guided FNA for malignant biliary stricture: a systematic review and meta-analysis. Gastrointest Endosc 83(2):290–298 (e1)
Navaneethan U, Hasan MK, Lourdusamy V, Njei B, Varadarajulu S, Hawes RH (2015) Single-operator cholangioscopy and targeted biopsies in the diagnosis of indeterminate biliary strictures: a systematic review. Gastrointest Endosc 82(4):608–614
Fujita T, Kojima M, Kato Y, Gotohda N, Takahashi S, Konishi M, Kinoshita T (2010) Clinical and histopathological study of “follicular cholangitis”: sclerosing cholangitis with prominent lymphocytic infiltration masquerading as hilar cholangiocarcinoma. Hepatol Res 40(12):1239–1247
Wakai T, Shirai Y, Sakata J, Maruyama T, Ohashi T, Korira PV, Ajioka Y, Hatakeyama K (2012) Clinicopathological features of benign biliary strictures masquerading as biliary malignancy. Am Surg 78(12):1388–1391
de Vries AB, Janse M, Blokzijl H, Weersma RK (2015) Distinctive inflammatory bowel disease phenotype in primary sclerosing cholangitis. World J Gastroenterol 21(6):1956–1971
Sano H, Nakazawa T, Ando T, Hayashi K, Naitoh I, Okumura F, Miyabe K, Yoshida M, Takahashi S, Ohara H, Joh T (2011) Clinical characteristics of inflammatory bowel disease associated with primary sclerosing cholangitis. J Hepatobiliary Pancreat Sci 18(2):154–161
Aadland E, Schrumpf E, Fausa O, Elgjo K, Heilo A, Aakhus T, Gjone E (1987) Primary sclerosing cholangitis: a long-term follow-up study. Scand J Gastroenterol 22(6):655–664
Nakazawa T, Naitoh I, Hayashi K, Sano H, Miyabe K, Shimizu S, Joh T (2014) Inflammatory bowel disease of primary sclerosing cholangitis: a distinct entity? World J Gastroenterol 20(12):3245–3254
Tanaka A, Takikawa H (2013) Geoepidemiology of primary sclerosing cholangitis: a critical review. J Autoimmun 46:35–40
Weismüller TJ, Talwalkar JA, Ponsioen CY, Gotthardt DN, Marschall HU, Naess S, Holm K, Weersma RK, Lazaridis KN, Fevery J, Trivedi PJ, Schramm C, Chazouilleres O, Müller T, Farkkila M, Almer S, Pereira S, Mason AL, Floreani A, Milkiewicz P, Harley H, Pares A, de Vries L, Manser C, Gatselis N, Berg C, Lenzen H, de Valle MB, Imam M, Kirchner G, de Leuw P, Zimmer V, Fabris L, Braun F, Hirschfield GM, Marzioni M, Juran BD, Strassburg CP, Beuers U, Manns MP, Schrumpf E, Karlsen TH, Bergquist A, Boberg KM (2014) Primary sclerosing cholangitis from a global perspective—a multicenter, retrospective, observational study of the international PSC study group. J Hepatol 60(1, Supplement):S3
Tanaka A, Tazuma S, Okazaki K, Tsubouchi H, Inui K, Takikawa H (2014) Nationwide survey for primary sclerosing cholangitis and IgG4-related sclerosing cholangitis in Japan. J Hepatobiliary Pancreat Sci 21(1):43–50
Tanaka A, Tazuma S, Okazaki K, Tsubouchi H, Inui K, Takikawa H (2015) Clinical profiles of patients with primary sclerosing cholangitis in the elderly. J Hepatobiliary Pancreat Sci 22(3):230–236
Yimam KK, Bowlus CL (2014) Diagnosis and classification of primary sclerosing cholangitis. Autoimmun Rev 13(4–5):445–450
Lindor KD, Kowdley KV, Harrison ME, American College of G (2015) ACG clinical guideline: primary sclerosing cholangitis. Am J Gastroenterol 110(5):646–659 (quiz 660)
Hirschfield GM, Karlsen TH, Lindor KD, Adams DH (2013) Primary sclerosing cholangitis. The Lancet 382(9904):1587–1599
Angulo P, Maor-Kendler Y, Lindor KD (2002) Small-duct primary sclerosing cholangitis: a long-term follow-up study. Hepatology 35(6):1494–1500
Kaplan GG, Laupland KB, Butzner D, Urbanski SJ, Lee SS (2007) The burden of large and small duct primary sclerosing cholangitis in adults and children: a population-based analysis. Am J Gastroenterol 102(5):1042–1049
Mieli-Vergani G, Vergani D (2016) Sclerosing cholangitis in children and adolescents. Clin Liver Dis 20(1):99–111
Sarkar S, Bowlus CL (2016) Primary sclerosing cholangitis: multiple phenotypes, multiple approaches. Clin Liver Dis 20(1):67–77
Berntsen NL, Klingenberg O, Juran BD, Benito de Valle M, Lindkvist B, Lazaridis KN, Boberg KM, Karlsen TH, Hov JR (2015) Association between HLA haplotypes and increased serum levels of IgG4 in patients with primary sclerosing cholangitis. Gastroenterology 148(5):924–927 (e2)
Matsubayashi H, Igarashi K, Kishida Y, Yoshida Y, Sasaki K, Ono H (2014) Sclerosing cholangitis with thumbprint appearance and incomplete steroid response. J Dig Dis 15(10):578–582
Liu JZ, Hov JR, Folseraas T, Ellinghaus E, Rushbrook SM, Doncheva NT, Andreassen OA, Weersma RK, Weismuller TJ, Eksteen B, Invernizzi P, Hirschfield GM, Gotthardt DN, Pares A, Ellinghaus D, Shah T, Juran BD, Milkiewicz P, Rust C, Schramm C, Muller T, Srivastava B, Dalekos G, Nothen MM, Herms S, Winkelmann J, Mitrovic M, Braun F, Ponsioen CY, Croucher PJ, Sterneck M, Teufel A, Mason AL, Saarela J, Leppa V, Dorfman R, Alvaro D, Floreani A, Onengut-Gumuscu S, Rich SS, Thompson WK, Schork AJ, Naess S, Thomsen I, Mayr G, Konig IR, Hveem K, Cleynen I, Gutierrez-Achury J, Ricano-Ponce I, van Heel D, Bjornsson E, Sandford RN, Durie PR, Melum E, Vatn MH, Silverberg MS, Duerr RH, Padyukov L, Brand S, Sans M, Annese V, Achkar JP, Boberg KM, Marschall HU, Chazouilleres O, Bowlus CL, Wijmenga C, Schrumpf E, Vermeire S, Albrecht M, Consortium U-P, Rioux JD, Alexander G, Bergquist A, Cho J, Schreiber S, Manns MP, Farkkila M, Dale AM, Chapman RW, Lazaridis KN, International PSCSG, Franke A, Anderson CA, Karlsen TH, International IBDGC (2013) Dense genotyping of immune-related disease regions identifies nine new risk loci for primary sclerosing cholangitis. Nat Genet 45(6):670–675
Nakanuma Y, Sasaki M, Harada K (2015) Autophagy and senescence in fibrosing cholangiopathies. J Hepatol 62(4):934–945
Trivedi PJ, Hirschfield GM (2016) The immunogenetics of autoimmune cholestasis. Clin Liver Dis 20(1):15–31
Naitoh I, Zen Y, Nakazawa T, Ando T, Hayashi K, Okumura F, Miyabe K, Yoshida M, Nojiri S, Kanematsu T, Ohara H, Joh T (2011) Small bile duct involvement in IgG4-related sclerosing cholangitis: liver biopsy and cholangiography correlation. J Gastroenterol 46(2):269–276
Deshpande V, Sainani NI, Chung RT, Pratt DS, Mentha G, Rubbia-Brandt L, Lauwers GY (2009) IgG4-associated cholangitis: a comparative histological and immunophenotypic study with primary sclerosing cholangitis on liver biopsy material. Mod Pathol 22(10):1287–1295
Folseraas T, Boberg KM (2016) Cancer risk and surveillance in primary sclerosing cholangitis. Clin Liver Dis 20(1):79–98
Trikudanathan G, Navaneethan U, Njei B, Vargo JJ, Parsi MA (2014) Diagnostic yield of bile duct brushings for cholangiocarcinoma in primary sclerosing cholangitis: a systematic review and meta-analysis. Gastrointest Endosc 79(5):783–789
Navaneethan U, Njei B, Venkatesh PG, Vargo JJ, Parsi MA (2014) Fluorescence in situ hybridization for diagnosis of cholangiocarcinoma in primary sclerosing cholangitis: a systematic review and meta-analysis. Gastrointest Endosc 79(6): 943–950 (e3)
Benito de Valle M, Muller T, Bjornsson E, Otten M, Volkmann M, Guckelberger O, Wiedenmann B, Sadik R, Schott E, Andersson M, Berg T, Lindkvist B (2014) The impact of elevated serum IgG4 levels in patients with primary sclerosing cholangitis. Dig Liver Dis 46(10):903–908
Mendes FD, Jorgensen R, Keach J, Katzmann JA, Smyrk T, Donlinger J, Chari S, Lindor KD (2006) Elevated serum IgG4 concentration in patients with primary sclerosing cholangitis. Am J Gastroenterol 101(9):2070–2075
Zhang L, Lewis JT, Abraham SC, Smyrk TC, Leung S, Chari ST, Poterucha JJ, Rosen CB, Lohse CM, Katzmann JA, Wu TT (2010) IgG4+ plasma cell infiltrates in liver explants with primary sclerosing cholangitis. Am J Surg Pathol 34(1):88–94
Navaneethan U, Venkatesh PG, Choudhary M, Shen B, Kiran RP (2013) Elevated immunoglobulin G4 level is associated with reduced colectomy-free survival in patients with primary sclerosing cholangitis and ulcerative colitis. J Crohns Colitis 7(2):e35–e41
Zen Y, Quaglia A, Portmann B (2011) Immunoglobulin G4-positive plasma cell infiltration in explanted livers for primary sclerosing cholangitis. Histopathology 58(3):414–422
Fischer S, Trivedi PJ, Ward S, Greig PD, Therapondos G, Hirschfield GM (2014) Frequency and significance of IgG4 immunohistochemical staining in liver explants from patients with primary sclerosing cholangitis. Int J Exp Pathol 95(3):209–215
Ohara H, Okazaki K, Tsubouchi H, Inui K, Kawa S, Kamisawa T, Tazuma S, Uchida K, Hirano K, Yoshida H, Nishino T, Ko SB, Mizuno N, Hamano H, Kanno A, Notohara K, Hasebe O, Nakazawa T, Nakanuma Y, Takikawa H, Research Committee of Ig GrD, Research Committee of Intractable Diseases of L, Biliary T, Ministry of Health L, Welfare J, Japan Biliary A (2012) Clinical diagnostic criteria of IgG4-related sclerosing cholangitis 2012. J Hepatobiliary Pancreat Sci 19(5):536–542
Deshpande V, Zen Y, Chan JK, Yi EE, Sato Y, Yoshino T, Kloppel G, Heathcote JG, Khosroshahi A, Ferry JA, Aalberse RC, Bloch DB, Brugge WR, Bateman AC, Carruthers MN, Chari ST, Cheuk W, Cornell LD, Fernandez-Del Castillo C, Forcione DG, Hamilos DL, Kamisawa T, Kasashima S, Kawa S, Kawano M, Lauwers GY, Masaki Y, Nakanuma Y, Notohara K, Okazaki K, Ryu JK, Saeki T, Sahani DV, Smyrk TC, Stone JR, Takahira M, Webster GJ, Yamamoto M, Zamboni G, Umehara H, Stone JH (2012) Consensus statement on the pathology of IgG4-related disease. Mod Pathol 25(9):1181–1192
Stone JH, Zen Y, Deshpande V (2012) IgG4-related disease. N Engl J Med 366(6):539–551
Brito-Zeron P, Ramos-Casals M, Bosch X, Stone JH (2014) The clinical spectrum of IgG4-related disease. Autoimmun Rev 13(12):1203–1210
Inoue D, Yoshida K, Yoneda N, Ozaki K, Matsubara T, Nagai K, Okumura K, Toshima F, Toyama J, Minami T, Matsui O, Gabata T, Zen Y (2015) IgG4-related disease: dataset of 235 consecutive patients. Medicine (Baltimore) 94(15):e680
Zen Y, Kawakami H, Kim JH (2016) IgG4-related sclerosing cholangitis: all we need to know. J Gastroenterol 51(4):295–312
Nakazawa T, Naitoh I, Hayashi K, Miyabe K, Simizu S, Joh T (2013) Diagnosis of IgG4-related sclerosing cholangitis. World J Gastroenterol 19(43):7661–7670
Nakazawa T, Ikeda Y, Kawaguchi Y, Kitagawa H, Takada H, Takeda Y, Makino I, Makino N, Naitoh I, Tanaka A (2015) Isolated intrapancreatic IgG4-related sclerosing cholangitis. World J Gastroenterol 21(4):1334–1343
Ohara H, Nakazawa T, Kawa S, Kamisawa T, Shimosegawa T, Uchida K, Hirano K, Nishino T, Hamano H, Kanno A, Notohara K, Hasebe O, Muraki T, Ishida E, Naitoh I, Okazaki K (2013) Establishment of a serum IgG4 cut-off value for the differential diagnosis of IgG4-related sclerosing cholangitis: a Japanese cohort. J Gastroenterol Hepatol 28(7):1247–1251
Graham RPD, Smyrk TC, Chari ST, Takahashi N, Zhang L (2014) Isolated IgG4-related sclerosing cholangitis: a report of 9 cases. Hum Pathol 45(8):1722–1729
Okazaki K, Uchida K, Koyabu M, Miyoshi H, Ikeura T, Takaoka M (2014) IgG4 cholangiopathy—current concept, diagnosis, and pathogenesis. J Hepatol 61(3):690–695
Hart PA, Zen Y, Chari ST (2015) Recent advances in autoimmune pancreatitis. Gastroenterology 149(1):39–51
Khosroshahi A, Wallace ZS, Crowe JL, Akamizu T, Azumi A, Carruthers MN, Chari ST, Della-Torre E, Frulloni L, Goto H, Hart PA, Kamisawa T, Kawa S, Kawano M, Kim MH, Kodama Y, Kubota K, Lerch MM, Löhr M, Masaki Y, Matsui S, Mimori T, Nakamura S, Nakazawa T, Ohara H, Okazaki K, Ryu JH, Saeki T, Schleinitz N, Shimatsu A, Shimosegawa T, Takahashi H, Takahira M, Tanaka A, Topazian M, Umehara H, Webster GJ, Witzig TE, Yamamoto M, Zhang W, Chiba T, Stone JH (2015) International consensus guidance statement on the management and treatment of IgG4-related disease. Arthritis Rheumatol 67(7):1688–1699
Oseini AM, Chaiteerakij R, Shire AM, Ghazale A, Kaiya J, Moser CD, Aderca I, Mettler TA, Therneau TM, Zhang L, Takahashi N, Chari ST, Roberts LR (2011) Utility of serum immunoglobulin G4 in distinguishing immunoglobulin G4-associated cholangitis from cholangiocarcinoma. Hepatology 54(3):940–948
Stone JH, Brito-Zerón P, Bosch X, Ramos-Casals M (2015) Diagnostic approach to the complexity of IgG4-related disease. Mayo Clin Proc 90(7):927–939
Carruthers MN, Khosroshahi A, Augustin T, Deshpande V, Stone JH (2015) The diagnostic utility of serum IgG4 concentrations in IgG4-related disease. Ann Rheum Dis 74(1):14–18
Ngwa TN, Law R, Murray D, Chari ST (2014) Serum immunoglobulin G4 level is a poor predictor of immunoglobulin G4-related disease. Pancreas 43(5):704–707
Harada K, Shimoda S, Kimura Y, Sato Y, Ikeda H, Igarashi S, Ren XS, Sato H, Nakanuma Y (2012) Significance of immunoglobulin G4 (IgG4)-positive cells in extrahepatic cholangiocarcinoma: molecular mechanism of IgG4 reaction in cancer tissue. Hepatology 56(1):157–164
Wallace ZS, Deshpande V, Mattoo H, Mahajan VS, Kulikova M, Pillai S, Stone JH (2015) IgG4-related disease: clinical and laboratory features in one hundred twenty-five patients. Arthritis Rheumatol 67(9):2466–2475
Khosroshahi A, Cheryk LA, Carruthers MN, Edwards JA, Bloch DB, Stone JH (2014) Spuriously low serum IgG4 concentrations caused by the prozone phenomenon in patients with IgG4-related disease. Arthritis Rheumatol 66(1):213–217
Boonstra K, Culver EL, de Buy Wenniger LM, van Heerde MJ, van Erpecum KJ, Poen AC, van Nieuwkerk KM, Spanier BW, Witteman BJ, Tuynman HA, van Geloven N, van Buuren H, Chapman RW, Barnes E, Beuers U, Ponsioen CY (2014) Serum immunoglobulin G4 and immunoglobulin G1 for distinguishing immunoglobulin G4-associated cholangitis from primary sclerosing cholangitis. Hepatology 59(5):1954–1963
Wallace ZS, Mattoo H, Carruthers M, Mahajan VS, Della Torre E, Lee H, Kulikova M, Deshpande V, Pillai S, Stone JH (2015) Plasmablasts as a biomarker for IgG4-related disease, independent of serum IgG4 concentrations. Ann Rheum Dis 74(1):190–195
Mattoo H, Mahajan VS, Della-Torre E, Sekigami Y, Carruthers M, Wallace ZS, Deshpande V, Stone JH, Pillai S (2014) De novo oligoclonal expansions of circulating plasmablasts in active and relapsing IgG4-related disease. J Allergy Clin Immunol 134(3):679–687
Smit WL, Culver EL, Chapman RW (2016) New thoughts on immunoglobulin G4-related sclerosing cholangitis. Clin Liver Dis 20(1):47–65
Zen Y, Harada K, Sasaki M, Sato Y, Tsuneyama K, Haratake J, Kurumaya H, Katayanagi K, Masuda S, Niwa H, Morimoto H, Miwa A, Uchiyama A, Portmann BC, Nakanuma Y (2004) IgG4-related sclerosing cholangitis with and without hepatic inflammatory pseudotumor, and sclerosing pancreatitis-associated sclerosing cholangitis: do they belong to a spectrum of sclerosing pancreatitis? Am J Surg Pathol 28(9):1193–1203
Zen Y, Nakanuma Y, Portmann B (2012) Immunoglobulin G4-related sclerosing cholangitis: pathologic features and histologic mimics. Semin Diagn Pathol 29(4):205–211
Harada K, Nakanuma Y (2014) Cholangiocarcinoma with respect to IgG4 reaction. Int J Hepatol 2014:803876
Huggett MT, Culver EL, Kumar M, Hurst JM, Rodriguez-Justo M, Chapman MH, Johnson GJ, Pereira SP, Chapman RW, Webster GJ, Barnes E (2014) Type 1 autoimmune pancreatitis and IgG4-related sclerosing cholangitis is associated with extrapancreatic organ failure, malignancy, and mortality in a prospective UK cohort. Am J Gastroenterol 109(10):1675–1683
Straub BK, Esposito I, Gotthardt D, Radeleff B, Antolovic D, Flechtenmacher C, Schirmacher P (2011) IgG4-associated cholangitis with cholangiocarcinoma. Virchows Arch 458(6):761–765
Oh HC, Kim JG, Kim JW, Lee KS, Kim MK, Chi KC, Kim YS, Kim KH (2008) Early bile duct cancer in a background of sclerosing cholangitis and autoimmune pancreatitis. Intern Med 47(23):2025–2028
Ohtani H, Ishida H, Ito Y, Yamaguchi T, Koizumi M (2011) Autoimmune pancreatitis and biliary intraepithelial neoplasia of the common bile duct: a case with diagnostically challenging but pathogenetically significant association. Pathol Int 61(8):481–485
Hart PA, Smyrk TC, Chari ST (2015) Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4. Mod Pathol 28(2):238–247
Lin J, Cummings OW, Greenson JK, House MG, Liu X, Nalbantoglu I, Pai R, Davidson DD, Reuss SA (2015) IgG4-related sclerosing cholangitis in the absence of autoimmune pancreatitis mimicking extrahepatic cholangiocarcinoma. Scand J Gastroenterol 50(4):447–453
Matsubayashi H, Uesaka K, Sugiura T, Ohgi K, Sasaki K, Ono H (2014) IgG4-related sclerosing cholangitis without obvious pancreatic lesion: difficulty in differential diagnosis. J Dig Dis 15(7):394–403
Hamano H, Kawa S, Horiuchi A, Unno H, Furuya N, Akamatsu T, Fukushima M, Nikaido T, Nakayama K, Usuda N, Kiyosawa K (2001) High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med 344(10):732–738
Kawakami H, Zen Y, Kuwatani M, Eto K, Haba S, Yamato H, Shinada K, Kubota K, Asaka M (2010) IgG4-related sclerosing cholangitis and autoimmune pancreatitis: histological assessment of biopsies from Vater’s ampulla and the bile duct. J Gastroenterol Hepatol 25(10):1648–1655
Umemura T, Zen Y, Hamano H, Kawa S, Nakanuma Y, Kiyosawa K (2007) Immunoglobin G4-hepatopathy: association of immunoglobin G4-bearing plasma cells in liver with autoimmune pancreatitis. Hepatology 46(2):463–471
Hokuto D, Yamato I, Nomi T, Yasuda S, Obara S, Yamada T, Chihiro K, Nakajima Y (2015) Eosinophilic cholangitis coexisted with idiopathic thrombocytopenic purpura: report of a case. Hepatol Res 45(5):595–600
Fragulidis GP, Vezakis AI, Kontis EA, Pantiora EV, Stefanidis GG, Politi AN, Koutoulidis VK, Mela MK, Polydorou AA (2016) Eosinophilic cholangitis-a challenging diagnosis of benign biliary stricture: a case report. Medicine (Baltimore) 95(1):e2394
Leegaard M (1980) Eosinophilic cholecystitis. Acta Chir Scand 146(4):295–296
Butler TW, Feintuch TA, Caine WP Jr (1985) Eosinophilic cholangitis, lymphadenopathy, and peripheral eosinophilia: a case report. Am J Gastroenterol 80(7):572–574
Goode EC, Simpson Bw, Rushbrook SM, Rushbrook SM (2013) A rare cause of cholangiopathy. Gastroenterology 144(7):e14–e15
Yagawa Y, Yasuda H, Sugimoto M, Koda K, Suzuki M, Yamazaki M, Tezuka T, Kosugi C, Higuchi R, Watayo Y (2008) Two cases of eosinophilic cholangitis caused biliary obstruction. Jpn J Gastroenterol Surg 41(5):533–539
Usuki N, Toyoshima M, Mikami S, Katsuyama E (2011) A case of eosinophilic cholangitis. Jpn J Clin Radiol 56(2):261–264
Oh SR, Kim D, Kim TH (2012) Eosinophilic cholangiopathy. Gastrointest Endosc 75(3):669–670
Platt ML, Kiesling VJ Jr, Vaccaro JA (1990) Eosinophilic ureteritis associated with eosinophilic cholangitis: a case report. J Urol 144(1):127–129
Grauer L, Padilla Iii VM, Bouza L, Barkin JS (1993) Eosinophilic sclerosing cholangitis associated with hypereosinophilic syndrome. Am J Gastroenterol 88(10):1764–1769
Kroemer A, Sabet-Baktach M, Doenecke A, Ruemmele P, Scherer MN, Schlitt HJ, Breidert M (2012) Eosinophilic cholangitis and wirsungitis as cause of simultaneous bile duct obstruction and pancreatitis. Z Gastroenterol 50(8):766–770
Rodgers MS, Allen JP, Koea JB, McCall JL (2001) Eosinophilic cholangitis: a case of ‘malignant masquerade’. HPB (Oxford) 3(3):235–239
Raptou G, Pliakos I, Hytiroglou P, Papavramidis S, Karkavelas G (2009) Severe eosinophilic cholangitis with parenchymal destruction of the left hepatic lobe due to hydatid disease. Pathol Int 59(6):395–398
Rosengart TK, Rotterdam H, Ranson JHC (1990) Eosinophilic cholangitis: a self-limited cause of extrahepatic biliary obstruction. Am J Gastroenterol 85(5):582–585
Matsumoto N, Yokohama K, Nakai K, Yamamoto T, Otani T, Ogawa M, Tanaka N, Iwasaki A, Arakawa Y, Sugitani M (2007) A case of eosinophilic cholangitis: imaging findings of contrast-enhanced ultrasonography, cholangioscopy, and intraductal ultrasonography. World J Gastroenterol 13(13):1995–1997
Miura F, Asano T, Amano H, Yoshida M, Toyota N, Wada K, Kato K, Takada T, Fukushima J, Kondo F, Takikawa H (2009) Resected case of eosinophilic cholangiopathy presenting with secondary Sclerosing cholangitis. World J Gastroenterol 15(11):1394–1397
Shanti CM, Lucas CE, Tyburski JG, Tyburski JG, Soulen RL, Soulen Rl, Lucas DR (2001) Eosinophilic abscess and eosinophilic pseudotumor presenting as bile duct masses: a report of 2 cases. Surgery 130(1):104–108
Chen WH, Yu CC, Wu CC, Jan YJ (2009) Eosinophilic cholangitis with obstructive jaundice mimicking bile duct carcinoma. J Hepatobiliary Pancreat Surg 16(2):242–245
Burnett AS, Bailey J, Oliver JB, Ahlawat S, Chokshi RJ (2014) Sensitivity of alternative testing for pancreaticobiliary cancer: a 10-y review of the literature. J Surg Res 190(2):535–547
Takikawa H (1999) Recent status of primary sclerosing cholangitis in Japan. J Hepatobiliary Pancreat Surg 6(4):352–355
Iwamuro M, Yamamoto K, Kawamoto H, Terada R, Ogawa T, Nose S (2009) Eosinophilic cholangitis with initial clinical features indistinguishable from IgG4-related cholangitis. Intern Med 48(13):1143–1147
Zen Y, Ishikawa A, Ogiso S, Heaton N, Portmann B (2012) Follicular cholangitis and pancreatitis - clinicopathological features and differential diagnosis of an under-recognized entity. Histopathology 60(2):261–269
Aoki T, Kubota K, Oka T, Hasegawa K, Hirai I, Makuuchi M (2003) Follicular cholangitis: another cause of benign biliary stricture. Hepatogastroenterology 50(51):639–642
Fujii M, Shiode J, Niguma T, Ito M, Ishiyama S, Fujiwara A, Nose S, Yoshioka M, Mimura T (2014) A case of follicular cholangitis mimicking hilar cholangiocarcinoma. Clin J Gastroenterol 7(1):62–67
Mizuuchi Y, Aishima S, Hattori M, Ushijima Y, Aso A, Takahata S, Ohtsuka T, Ueda J, Tanaka M, Oda Y (2014) Follicular pancreatitis, report of a case clinically mimicking pancreatic cancer and literature review. Pathol Res Pract 210(2):118–122
Gupta RK, Xie BH, Patton KT, Lisovsky M, Burks E, Behrman SW, Klimstra D, Deshpande V (2016) Follicular pancreatitis: a distinct form of chronic pancreatitis—an additional mimic of pancreatic neoplasms. Hum Pathol 48:154–162
Zakaria A, Al-Obeidi S, Daradkeh S (2013) Primary non-Hodgkin’s lymphoma of the common bile duct: a case report and literature review. Asian J Surg doi:10.1016/j.asjsur.2013.09.009
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interests regarding the publication of this paper.
Rights and permissions
About this article
Cite this article
Nguyen Canh, H., Harada, K. Adult bile duct strictures: differentiating benign biliary stenosis from cholangiocarcinoma. Med Mol Morphol 49, 189–202 (2016). https://doi.org/10.1007/s00795-016-0143-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00795-016-0143-6