Abstract
Objectives
Radiopacity of dental materials enables clinician to radiographically diagnose secondary caries and marginal defects which are usually located on the proximal gingival margin. The aim of this study was to measure the radiopacity of 33 conventional resin composites, 16 flowable resin composites, and 7 glass ionomer cements and to compare the results with the radiopacity values declared by the manufacturers.
Materials and methods
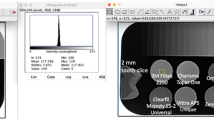
From each restorative material, six 2-mm-thick disk-shaped specimens were fabricated and eight 2-mm-thick sections of teeth were made and used as reference. The material samples and tooth sections were digitally radiographed together with the aluminum stepwedge. Gray values were obtained from the radiographic images and radiopacity values were calculated and statistically analyzed. Post hoc Tukey’s honestly significant difference test was used to calculate significant differences in radiopacity values between materials and reference dentin and enamel values.
Results
The radiopacity values of all 56 restorative materials were above the dentin reference radiopacity value; however, 4 out of 33 conventional composites and 3 out of 16 flowable resin composites had significantly lower radiopacity than enamel (p < 0.05). There were up to 1.53 mm eq Al differences between the measured and the manufacturers’ declared radiopacity values of some materials.
Conclusions
Majority of the materials exceed enamel radiopacity and would not hamper radiographic diagnosis of secondary caries. However, manufacturers’ data are not always reliable.
Clinical relevance
Materials with radiopacity lower than enamel might be misinterpreted as secondary enamel caries on radiographic images, especially when applied as initial increment on the proximal gingival margin.

Similar content being viewed by others
References
Matteson SR, Phillips C, Kantor ML, Leinedecker T (1989) The effect of lesion size, restorative material, and film speed on the detection of recurrent caries. Oral Surg Oral Med Oral Pathol 68(2):232–237
Shah PM, Sidhu SK, Chong BS, Ford TR (1997) Radiopacity of resin-modified glass ionomer liners and bases. J Prosthet Dent 77(3):239–242
Willems G, Noack MJ, Inokoshi S, Lambrechts P, Van Meerbeek B, Braem M, Roulet JF, Vanherle G (1991) Radiopacity of composites compared with human enamel and dentine. J Dent 19(6):362–365
Mjör IA, Toffenetti F (2000) Secondary caries: a literature review with case reports. Quintessence Int 31(3):165–179
Attar N, Tam LE, McComb D (2003) Flow, strength, stiffness and radiopacity of flowable resin composites. J Can Dent Assoc 69(8):516–521
Mongkolnam P, Tyas MJ (1994) Light-cured lining materials: a laboratory study. Dent Mater 10(3):196–202
Taira M, Toyooka H, Miyawaki H, Yamaki M (1993) Studies on radiopaque composites containing ZrO2–SiO2 fillers prepared by the sol–gel process. Dent Mater 9(3):167–171
Oikarinen KS, Nieminen TM, Mäkäräinen H, Pyhtinen J (1993) Visibility of foreign bodies in soft tissue in plain radiographs, computed tomography, magnetic resonance imaging, and ultrasound. An in vitro study. Int J Oral Maxillofac Surg 22(2):119–124
Kafas P, Upile T, Angouridakis N, Stavrianos C, Dabarakis N, Jerjes W (2009) Dysaesthesia in the mental nerve distribution triggered by a foreign body: a case report. Cases J 2:169. doi:10.1186/1757-1626-2-169
Poorterman JH, Aartman IH, Kalsbeek H (1999) Underestimation of the prevalence of approximal caries and inadequate restorations in a clinical epidemiological study. Community Dent Oral Epidemiol 27(5):331–337
Mjör I (1998) The location of clinically diagnosed secondary caries. Quintessence Int 29:313–317
Gu S, Rasimick BJ, Deutsch AS, Musikant BL (2006) Radiopacity of dental materials using a digital X-ray system. Dent Mater 22(8):765–770
Nomoto R, Mishima A, Kobayashi K, McCabe JF, Darvell BW, Watts DC, Momoi Y, Hirano S (2008) Quantitative determination of radio-opacity: equivalence of digital and film X-ray systems. Dent Mater 24(1):141–147
Watts DC, McCabe JF (1999) Aluminium radiopacity standards for dentistry: an international survey. J Dent 27(1):73–78
Haiter-Neto F, dos Anjos Pontual A, Frydenberg M, Wenzel A (2007) A comparison of older and newer versions of intraoral digital radiography systems: diagnosing noncavitated proximal carious lesions. J Am Dent Assoc 138(10):1353–1359, quiz 1382–1353
Sabbagh J, Vreven J, Leloup G (2004) Radiopacity of resin-based materials measured in film radiographs and storage phosphor plate (Digora). Oper Dent 29(6):677–684
Murchison DF, Charlton DG, Moore WS (1999) Comparative radiopacity of flowable resin composites. Quintessence Int 30(3):179–184
Sidhu SK, Shah PM, Chong BS, Pitt Ford TR (1996) Radiopacity of resin-modified glass-ionomer restorative cements. Quintessence Int 27(9):639–643
Turgut MD, Attar N, Onen A (2003) Radiopacity of direct esthetic restorative materials. Oper Dent 28(5):508–514
Ergücü Z, Türkün LS, Onem E, Güneri P (2010) Comparative radiopacity of six flowable resin composites. Oper Dent 35(4):436–440
Salzedas LM, Louzada MJ, de Oliveira Filho AB (2006) Radiopacity of restorative materials using digital images. J Appl Oral Sci 14(2):147–152
Hara AT, Serra MC, Haiter-Neto F, Rodrigues AL Jr (2001) Radiopacity of esthetic restorative materials compared with human tooth structure. Am J Dent 14(6):383–386
Hara AT, Serra MC, Rodrigues Júnior AL (2001) Radiopacity of glass-ionomer/composite resin hybrid materials. Braz Dent J 12(2):85–89
Choi KK, Ferracane JL, Hilton TJ, Charlton D (2000) Properties of packable dental composites. J Esthet Dent 12(4):216–226
International Standards Organization (2000) ISO 4049:2000, dentistry—polymer-based filling, restorative and luting materials, 3rd edn. ISO, Geneva
Watts DC (1987) Radiopacity vs. composition of some barium and strontium glass composites. J Dent 15(1):38–43
Cook WD (1981) An investigation of the radiopacity of composite restorative materials. Aust Dent J 26(2):105–112
Bouschlicher MR, Cobb DS, Boyer DB (1999) Radiopacity of compomers, flowable and conventional resin composites for posterior restorations. Oper Dent 24(1):20–25
Goshima T, Goshima Y (1990) Radiographic detection of recurrent carious lesions associated with composite restorations. Oral Surg Oral Med Oral Pathol 70(2):236–239
Berry HM Jr (1983) Cervical burnout and Mach band: two shadows of doubt in radiologic interpretation of carious lesions. J Am Dent Assoc 106(5):622–625
Espelid I, Tveit AB, Erickson RL, Keck SC, Glasspoole EA (1991) Radiopacity of restorations and detection of secondary caries. Dent Mater 7(2):114–117
Ferdianakis K (1998) Microleakage reduction from newer esthetic restorative materials in permanent molars. J Clin Pediatr Dent 22(3):221–229
Leevailoj C, Cochran MA, Matis BA, Moore BK, Platt JA (2001) Microleakage of posterior packable resin composites with and without flowable liners. Oper Dent 26(3):302–307
Malmström HS, Schlueter M, Roach T, Moss ME (2002) Effect of thickness of flowable resins on marginal leakage in class II composite restorations. Oper Dent 27(4):373–380
Payne JH 4th (1999) The marginal seal of class II restorations: flowable composite resin compared to injectable glass ionomer. J Clin Pediatr Dent 23(2):123–130
Estafan AM, Estafan D (2000) Microleakage study of flowable composite resin systems. Compend Contin Educ Dent 21(9):705–708, 710, 712; quiz 714
Jain P, Belcher M (2000) Microleakage of class II resin-based composite restorations with flowable composite in the proximal box. Am J Dent 13(5):235–238
Andersson-Wenckert IE, van Dijken JW, Hörstedt P (2002) Modified class II open sandwich restorations: evaluation of interfacial adaptation and influence of different restorative techniques. Eur J Oral Sci 110(3):270–275
Warren JA Jr (1986) Glass ionomer: its emerging role as an intermediary dental base. Fla Dent J 57(2):21, 23–24
Prévost AP, Forest D, Tanguay R, DeGrandmont P (1990) Radiopacity of glass ionomer dental materials. Oral Surg Oral Med Oral Pathol 70(2):231–235
Collares FM, Ogliari FA, Lima GS, Fontanella VR, Piva E, Samuel SM (2010) Ytterbium trifluoride as a radiopaque agent for dental cements. Int Endod J 43(9):792–797. doi:10.1111/j.1365-2591.2010.01746.x
de Abreu MJ, Tavares D, Vierira DF (1977) Radiopacity of restorative materials. Oper Dent 2(1):3–16
el-Mowafy OM, Brown JW, McComb D (1991) Radiopacity of direct ceramic inlay restoratives. J Dent 19(6):366–368
Jandt KD, Al-Jasser AM, Al-Ateeq K, Vowles RW, Allen GC (2002) Mechanical properties and radiopacity of experimental glass–silica–metal hybrid composites. Dent Mater 18(6):429–435
Stanford CM, Fan PL, Schoenfeld CM, Knoeppel R, Stanford JW (1987) Radiopacity of light-cured posterior composite resins. J Am Dent Assoc 115(5):722–724
Beyer-Olsen EM, Orstavik D (1981) Radiopacity of root canal sealers. Oral Surg Oral Med Oral Pathol 51(3):320–328
Tagger M, Katz A (2003) Radiopacity of endodontic sealers: development of a new method for direct measurement. J Endod 29(11):751–755
Abreu Júnior M, Tyndall DA, Platin E, Ludlow JB, Phillips C (1999) Two- and three-dimensional imaging modalities for the detection of caries. A comparison between film, digital radiography and tuned aperture computed tomography (TACT). Dentomaxillofac Radiol 28(3):152–157
Abreu M Jr, Mol A, Ludlow JB (2001) Performance of RVGui sensor and Kodak Ektaspeed Plus film for proximal caries detection. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 91(3):381–385
Borg E, Gröndahl K, Gröndahl HG (1997) Marginal bone level buccal to mandibular molars in digital radiographs from charge-coupled device and storage phosphor systems. An in vitro study. J Clin Periodontol 24(5):306–312
Borg E, Källqvist A, Gröndahl K, Gröndahl HG (1998) Film and digital radiography for detection of simulated root resorption cavities. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 86(1):110–114
Camps J, Pommel L, Bukiet F (2004) Evaluation of periapical lesion healing by correction of gray values. J Endod 30(11):762–766
Hintze H, Wenzel A (2002) Influence of the validation method on diagnostic accuracy for caries. A comparison of six digital and two conventional radiographic systems. Dentomaxillofac Radiol 31(1):44–49
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hitij, T., Fidler, A. Radiopacity of dental restorative materials. Clin Oral Invest 17, 1167–1177 (2013). https://doi.org/10.1007/s00784-012-0797-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-012-0797-y