Abstract
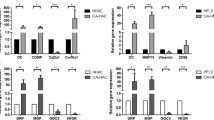
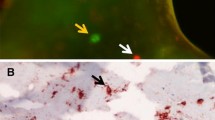
Osteoporosis (OP) and osteoarthritis (OA) are the most common joint diseases, with a high incidence in the elderly population. OP is characterized by trabecular bone remodeling and reabsorption, whereas articular cartilage and subchondral bone remodeling are major features of OA. Although classically considered as independent or even conflicting processes, clinical coexistence of OP and OA was recently described. Transglutaminase 2 (TG2) expression is considered a biomarker of OA, but its role in osteoporotic bone remodeling is still uncertain. We investigated TG2 and bone biological markers (Osteocalcin, Osteopontin, and Sclerostin) in osteoporotic and osteoarthritic osteocartilagineous tissue (n = 54) and human chondrocyte cultures in vitro by immunohistochemistry, immunofluorescence and RT-PCR. Histomorphometric evaluation of bone trabecular remodeling was also performed. In cartilage, TG2 expression was faint in control and OP and significantly less than in OA and OP + OA chondrocytes; the opposite was found for Osteocalcin, whereas Osteopontin and Sclerostin expression was similar. In the subchondral trabecular bone, osteocytes/osteoblasts TG2 expression was slight and similar comparing control, OP, OA, and OP + OA group, whereas Osteocalcin and Osteopontin expression was lower in OP compared to control, OA and OP + OA. Increased TG2 and reduced Osteocalcin expression were maintained in human osteoarthritic chondrocytes in vitro. Histomorphometric analysis confirmed reduced trabecular bone mass in OP and OP + OA compared with OA patients. TG2 represented a suitable biomarker of osteoarthritic chondrocyte activation, whereas osteocalcin and osteopontin characterized osteoporotic osteocyte/osteoblast changes; differences were lost in OP + OA patients, suggesting careful consideration when coexistence of the two diseases occurs.




Similar content being viewed by others
References
Ardawi MS, Al-Kadi HA, Rouzi AA, Qari MH (2011) Determinants of serum sclerostin in healthy pre- and postmenopausal women. J Bone Miner Res 26:2812–2822. doi:10.1002/jbmr.479
Arden NK, Crozier S, Smith H, Anderson F, Edwards C, Raphael H, Cooper C (2006) Knee pain, knee osteoarthritis, and the risk of fracture. Arthritis Rheum 55:610–615. doi:10.1002/art.22088
Bei R, Budillon A, Masuelli L, Cereda V, Vitolo D, Di Gennaro E, Ripavecchia V, Palumbo C, Ionna F, Losito S, Modesti A, Kraus MH, Muraro R (2004) Frequent overexpression of multiple ErbB receptors by head and neck squamous cell carcinoma contrasts with rare antibody immunity in patients. J Pathol 204:317–325. doi:10.1002/path.1642
Beil FT, Seitz S, Priemel M, Barvencik F, von Domarus C, Rueger JM, Amling M, Pogoda P (2008) Pathophysiology and pathomorphology of osteoporosis. Eur J Trauma Emerg Surg 34:527–534. doi:10.1007/s00068-008-8201-y
Beninati S, Senger DR, Cordella-Miele E, Mukherjee AB, Chackalaparampil I, Shanmugam V, Singh K, Mukherjee BB (1994) Osteopontin: its transglutaminase-catalyzed posttranslational modifications and cross-linking to fibronectin. J Biochem 115:675–682
Bergink AP, van der Klift M, Hofman A, Verhaar JA, van Leeuwen JP, Uitterlinden AG, Pols HA (2003) Osteoarthritis of the knee is associated with vertebral and nonvertebral fractures in the elderly: the Rotterdam Study. Arthritis Rheum 49:648–657. doi:10.1002/art.11380
Berry PA, Maciewicz RA, Cicuttini FM, Jones MD, Hellawell CJ, Wluka AE (2010) Markers of bone formation and resorption identify subgroups of patients with clinical knee osteoarthritis who have reduced rates of cartilage loss. J Rheumatol 37:1252–1259. doi:10.3899/jrheum.091055
Bhadada SK, Rastogi A, Steenackers E, Boudin E, Arya A, Dhiman V, Bhansali A, Van Hul W (2013) Novel SOST gene mutation in a sclerosteosis patient and her parents. Bone 52:707–710. doi:10.1016/j.bone.2012.10.009
Cassinelli G, Zuco V, Petrangolini G, De Cesare M, Tortoreto M, Lanzi C, Cominetti D, Zaffaroni N, Orlandi A, Passeri D, Meco D, Di Francesco AM, Riccardi R, Bucci F, Pisano C, Zunino F (2012) The curative efficacy of namitecan (ST1968) in preclinical models of pediatric sarcoma is associated with antiangiogenic effects. Biochem Pharmacol 84:163–171. doi:10.1016/j.bcp.2012.04.005
Cervelli V, Scioli MG, Gentile P, Doldo E, Bonanno E, Spagnoli LG, Orlandi A (2012) Platelet-rich plasma greatly potentiates insulin-induced adipogenic differentiation of human adipose-derived stem cells through a serine/threonine kinase Akt-dependent mechanism and promotes clinical fat graft maintenance. Stem Cells Transl Med 1:206–220. doi:10.5966/sctm.2011-0052
Chan BY, Fuller ES, Russell AK, Smith SM, Smith MM, Jackson MT, Cake MA, Read RA, Bateman JF, Sambrook PN, Little CB (2011) Increased chondrocyte sclerostin may protect against cartilage degradation in osteoarthritis. Osteoarthr Cartil 19:874–885. doi:10.1016/j.joca.2011.04.014
Chang IC, Chiang TI, Yeh KT, Lee H, Cheng YW (2010) Increased serum osteopontin is a risk factor for osteoporosis in menopausal women. Osteoporos Int 21:1401–1409. doi:10.1007/s00198-009-1107-7
Chen JS, Mehta K (1999) Tissue transglutaminase: an enzyme with a split personality. Int J Biochem Cell Biol 31:817–836. doi:10.1016/S1357-2725(99)00045-X
Chen Y, Bal BS, Gorski JP (1992) Calcium and collagen binding properties of osteopontin, bone sialoprotein, and bone acidic glycoprotein-75 from bone. J Biol Chem 267:24871–24878
Collins DH, McElligotte TF (1960) Sulphate (35SO4) uptake by chondrocytes in relation to histological changes in osteoarthritic human articular cartilage. Ann Rheum Dis 19:318–330. doi:10.1136/ard.19.4.318
Cumming RG, Klineberg RJ (1993) Epidemiological study of the relation between arthritis of the hip and hip fractures. Ann Rheum Dis 52:707–710. doi:10.1136/ard.52.10.717
Dempster DW, Compston JE, Drezner MK, Glorieux FH, Kanis JA, Malluche H, Meunier PJ, Ott SM, Recker RR, Parfitt AM (2013) Standardized nomenclature, symbols, and units for bone histomorphometry: a 2012 update of the report of the ASBMR Histomorphometry Nomenclature Committee. J Bone Miner Res 28:2–17. doi:10.1002/jbmr.1805
Denhardt DT, Noda M (1998) Osteopontin expression and function: role in bone remodeling. J Cell Biochem Suppl 30–31:92–102. doi:10.1002/(SICI)1097-4644(1998)72:30/31+92:AID-JCB13>3.0.CO;2-A
Dequeker J, Johnell O (1993) Osteoarthritis protects against femoral neck fracture: the MEDOS study experience. Bone 14(Suppl 1):S51–S56. doi:10.1186/1471-2474-11-274
Dieppe PA, Lohmander LS (2005) Pathogenesis and management of pain in osteoarthritis. Lancet 365:965–973. doi:10.1016/S0140-6736(05)71086-2
Eastell R, Hannon RA (2008) Biomarkers of bone health and osteoporosis risk. Proc Nutr Soc 67:157–162. doi:10.1017/S002966510800699X
Felson DT (2009) Developments in the clinical understanding of osteoarthritis. Arthritis Res Ther 11:203. doi:10.1186/ar2531
Fesus L, Piacentini M (2002) Transglutaminase 2: an enigmatic enzyme with diverse functions. Trends Biochem Sci 27:534–539. doi:10.1016/S0968-0004(02)02182-5
Funck-Brentano T, Cohen-Solal M (2011) Crosstalk between cartilage and bone: when bone cytokines matter. Cytokine Growth Factor Rev 22:91–97. doi:10.1016/j.cytogfr.2011.04.003
Gao SG, Li KH, Zeng KB, Tu M, Xu M, Lei GH (2010) Elevated osteopontin level of synovial fluid and articular cartilage is associated with disease severity in knee osteoarthritis patients. Osteoarthr Cartil 18:82–87. doi:10.1016/j.joca.2009.07.009
Goldring MB, Goldring SR (2010) Articular cartilage and subchondral bone in the pathogenesis of osteoarthritis. Ann N Y Acad Sci 1192:230–237. doi:10.1111/j.1749-632.2009.05240.x
Harris WH (1969) Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end-result study using a new method of result evaluation. J Bone Jt Surg Am 51:737–755
Heath DJ, Downes S, Verderio E, Griffin M (2001) Characterization of tissue transglutaminase in human osteoblast-like cells. J Bone Miner Res 16:1477–1485. doi:10.1359/jbmr.2001.16.8.1477
Heiland GR, Zwerina K, Baum W, Kireva T, Distler JH, Grisanti M, Asuncion F, Li X, Ominsky M, Richards W, Schett G, Zwerina J (2010) Neutralisation of Dkk-1 protects from systemic bone loss during inflammation and reduces sclerostin expression. Ann Rheum Dis 69:2152–2159. doi:10.1136/ard.2010.132852
Hinton R, Moody RL, Davis A, Thomas S (2002) Osteoarthritis: diagnosis and therapeutic considerations. Am Fam Physician 65:841–848
Jakob M, Démarteau O, Schäfer D, Stumm M, Heberer M, Martin I (2003) Enzymatic digestion of adult human articular cartilage yields a small fraction of the total available cells. Connect Tissue Res 44:173–180
Johnell O, Kanis JA (2006) An estimate of the worldwide prevalence and disability associated with osteoporotic fractures. Osteoporos Int 17:1726–1733. doi:10.1007/s00198-006-0172-4
Johnson VL, Hunter DJ (2014) The epidemiology of osteoarthritis. Best Pract Res Clin Rheumatol 28:5–15. doi:10.1016/j.berh.2014.01.004
Johnson K, Hashimoto S, Lotz M, Pritzker K, Terkeltaub R (2001) Interleukin-1 induces pro-mineralizing activity of cartilage tissue transglutaminase and factor XIIIa. Am J Pathol 159:149–163. doi:10.1016/S0002-9440(10)61682-3
Kaartinen MT, Pirhonen A, Linnala-Kankkunen A, Mäenpää PH (1997) Transglutaminase-catalyzed cross-linking of osteopontin is inhibited by osteocalcin. J Biol Chem 272:22736–22741. doi:10.1074/jbc.272.36.22736
Kaartinen MT, El-Maadawy S, Räsänen NH, McKee MD (2002) Tissue transglutaminase and its substrates in bone. J Bone Miner Res 17:2161–2173. doi:10.1359/jbmr.2002.17.12.2161
Karsdal MA, Leeming DJ, Dam EB, Henriksen K, Alexandersen P, Pastoureau P, Altman RD, Christiansen C (2008) Should subchondral bone turnover be targeted when treating osteoarthritis? Osteoarthr Cartil 16:638–646. doi:10.1016/j.joca.2008.01.014
Krause C, Korchynskyi O, de Rooij K, Weidauer SE, de Gorter DJ, van Bezooijen RL, Hatsell S, Economides AN, Mueller TD, Löwik CW, ten Dijke P (2010) Distinct modes of inhibition by sclerostin on bone morphogenetic protein and Wnt signaling pathways. J Biol Chem 285:41614–41626. doi:10.1074/jbc.M110.153890
Kuliwaba JS, Findlay DM, Atkins GJ, Forwood MR, Fazzalari NL (2000) Enhanced expression of osteocalcin mRNA in human osteoarthritic trabecular bone of the proximal femur is associated with decreased expression of interleukin-6 and interleukin-11 mRNA. J Bone Miner Res 15:332–341. doi:10.1359/jbmr.2000.15.2.332
Li J, Zhang H, Yang C, Li Y, Dai Z (2016) An overview of osteocalcin progress. J Bone Miner Metab. doi:10.1007/s00774-015-0734-7
Lorand L, Graham RM (2003) Transglutaminases: crosslinking enzymes with pleiotropic functions. Nat Rev Mol Cell Biol 4:140–156. doi:10.1038/nrm1014
Manenti G, Capuani S, Fanucci E, Assako EP, Masala S, Sorge R, Iundusi R, Tarantino U, Simonetti G (2013) Diffusion tensor imaging and magnetic resonance spectroscopy assessment of cancellous bone quality in femoral neck of healthy, osteopenic and osteoporotic subjects at 3T: preliminary experience. Bone 55:7–15. doi:10.1016/j.bone.2013.03.004
Matsui Y, Iwasaki N, Kon S, Takahashi D, Morimoto J, Matsui Y, Denhardt DT, Rittling S, Minami A, Uede T (2009) Accelerated development of aging-associated and instability-induced osteoarthritis in osteopontin-deficient mice. Arthritis Rheum 60:2362–2371. doi:10.1002/art.24705
McKee MD, Glimcher MJ, Nanci A (1992) High-resolution immunolocalization of osteopontin and osteocalcin in bone and cartilage during endochondral ossification in the chicken tibia. Anat Rec 234:479–492. doi:10.1002/ar.1092340404
Mukherjee BB, Nemir M, Beninati S, Cordella-Miele E, Singh K, Chackalaparampil I, Shanmugam V, DeVouge MW, Mukherjee AB (1995) Interaction of osteopontin with fibronectin and other extracellular matrix molecules. Ann N Y Acad Sci 760:201–212. doi:10.1111/j.1749-6632.1995.tb44631.x
Nilsdotter A, Bremander A (2011) Measures of hip function and symptoms: Harris Hip Score (HHS), Hip Disability and Osteoarthritis Outcome Score (HOOS), Oxford Hip Score (OHS), Lequesne Index of Severity for Osteoarthritis of the Hip (LISOH), and American Academy of Orthopedic Surgeons (AAOS) Hip and Knee Questionnaire. Arthritis Care Res (Hoboken) 63(Suppl 11):S200–S207. doi:10.1002/acr.20549
Orlandi A, Ferlosio A, Ciucci A, Sesti F, Lifschitz-Mercer B, Gabbiani G, Spagnoli LG, Czernobilsky B (2004) Cellular retinol-binding protein-1 expression in endometrial stromal cells: physiopathological and diagnostic implications. Histopathology 45:511–517. doi:10.1111/j.1365-2559.2004.01963.x
Orlandi A, Ciucci A, Ferlosio A, Pellegrino A, Chiariello L, Spagnoli LG (2005) Increased expression and activity of matrix metalloproteinases characterize embolic cardiac myxomas. Am J Pathol 166:1619–1628. doi:10.1016/S0002-9440(10)62472-8
Orlandi A, Oliva F, Taurisano G, Candi E, Di Lascio A, Melino G, Spagnoli LG, Tarantino U (2009) Transglutaminase-2 differently regulates cartilage destruction and osteophyte formation in a surgical model of osteoarthritis. Amino Acids 36:755–763. doi:10.1007/s00726-008-0129-3
Piters E, Culha C, Moester M, Van Bezooijen R, Adriaensen D, Mueller T, Weidauer S, Jennes K, de Freitas F, Löwik C, Timmermans JP, Van Hul W, Papapoulos S (2010) First missense mutation in the SOST gene causing sclerosteosis by loss of sclerostin function. Hum Mutat 31:E1526–E1543. doi:10.1002/humu.21274
Power J, Poole KE, van Bezooijen R, Doube M, Caballero-Alías AM, Lowik C, Papapoulos S, Reeve J, Loveridge N (2010) Sclerostin and the regulation of bone formation: effects in hip osteoarthritis and femoral neck fracture. J Bone Miner Res 25:1867–1876. doi:10.1002/jbmr.70
Pullig O, Weseloh G, Gauer S, Swoboda B (2000a) Osteopontin is expressed by adult human osteoarthritic chondrocytes: protein and mRNA analysis of normal and osteoarthritic cartilage. Matrix Biol 19:245–255. doi:10.1016/S0945-053X(00)00068-8
Pullig O, Weseloh G, Ronneberger D, Käkönen S, Swoboda B (2000b) Chondrocyte differentiation in human osteoarthritis: expression of osteocalcin in normal and osteoarthritic cartilage and bone. Calcif Tissue Int 67:230–240. doi:10.1007/s002230001108
Ravaud P, Ayral X, Dougados M (1999) Radiologic progression of hip and knee osteoarthritis. Osteoarthr Cartil 7:222–229. doi:10.1007/s10067-015-3146-0
Robling AG, Niziolek PJ, Baldridge LA, Condon KW, Allen MR, Alam I, Mantila SM, Gluhak-Heinrich J, Bellido TM, Harris SE, Turner CH (2008) Mechanical stimulation of bone in vivo reduces osteocyte expression of Sost/sclerostin. J Biol Chem 283:5866–5875. doi:10.1074/jbc.M705092200
Rosenthal AK, Derfus BA, Henry LA (1997) Transglutaminase activity in aging articular chondrocytes and articular cartilage vesicles. Arthritis Rheum 40:966–970. doi:10.1002/art.1780400526
Roudier M, Li X, Niu QT, Pacheco E, Pretorius JK, Graham K, Yoon BR, Gong J, Warmington K, Ke HZ, Black RA, Hulme J, Babij P (2013) Sclerostin is expressed in articular cartilage but loss or inhibition does not affect cartilage remodeling during aging or following mechanical injury. Arthritis Rheum 65:721–731. doi:10.1002/art.37802
Ryan LM, McCarty DJ (1997) Calcium pyrophosphate crystal deposition disease, pseudogout, and articular condrocalcinosis. In: Koopman W (ed) Arthritis and allied conditions: a textbook of rheumatology, 13th edn. Williams and Wilkins, Baltimore, pp 2103–2126
Sanchez C, Deberg MA, Bellahcène A, Castronovo V, Msika P, Delcour JP, Crielaard JM, Henrotin YE (2008) Phenotypic characterization of osteoblasts from the sclerotic zones of osteoarthritic subchondral bone. Arthritis Rheum 58:442–455. doi:10.1002/art.23159
Sarahrudi K, Thomas A, Albrecht C, Aharinejad S (2012) Strongly enhanced levels of sclerostin during human fracture healing. J Orthop Res 30:1549–1555. doi:10.1002/jor.22129
Semënov M, Tamai K, He X (2005) SOST is a ligand for LRP5/LRP6 and a Wnt signaling inhibitor. J Biol Chem 280:26770–26775. doi:10.1074/jbc.M504308200
Spagnoli LG, Orlandi A, Marino B, Mauriello A, De Angelis C, Ramacci MT (1995) Propionyl-l-carnitine prevents the progression of atherosclerotic lesions in aged hyperlipemic rabbits. Atherosclerosis 114:29–44. doi:10.1016/0021-9150(94)05460-Z
Standal T, Borset M, Sundan A (2004) Role of osteopontin in adhesion, migration, cell survival and bone remodeling. Exp Oncol 26:179–184
Summey BT Jr, Graff RD, Lai TS, Greenberg CS, Lee GM (2002) Tissue transglutaminase localization and activity regulation in the extracellular matrix of articular cartilage. J Orthop Res 20:76–82. doi:10.1016/S0736-0266(01)00064-X
Tarantino U, Ferlosio A, Arcuri G, Spagnoli LG, Orlandi A (2013) Transglutaminase 2 as a biomarker of osteoarthritis: an update. Amino Acids 44:199–207. doi:10.1007/s00726-011-1181-y
Tarantino U, Celi M, Rao C, Feola M, Cerocchi I, Gasbarra E, Ferlosio A, Orlandi A (2014) Hip osteoarthritis and osteoporosis: clinical and histomorphometric considerations. Int J Endocrinol 2014:372021. doi:10.1155/2014/372021
Thomázy VA, Davies PJ (1999) Expression of tissue transglutaminase in the developing chicken limb is associated both with apoptosis and endochondral ossification. Cell Death Differ 6:146–154
Vestergaard P, Rejnmark L, Mosekilde L (2009) Osteoarthritis and risk of fractures. Calcif Tissue Int 84:249–256. doi:10.1007/s00223-009-9224-z
Wanby P, Nobin R, Von SP, Brudin L, Carlsson M (2016) Serum levels of the bone turnover markers dickkopf-1, sclerostin, osteoprotegerin, osteopontin, osteocalcin and 25-hydroxyvitamin D in Swedish geriatric patients aged 75 years or older with a fresh hip fracture and in healthy controls. J Endocrinol Invest. doi:10.1007/s40618-015-0421-5
WHO (1994) Assessment of fracture risk and its application to screening for postmenopausal osteoporosis. Report of a WHO Study Group. World Health Organ Tech Rep Ser 843:1–129
Winkler DG, Sutherland MK, Geoghegan JC, Yu C, Hayes T, Skonier JE, Shpektor D, Jonas M, Kovacevich BR, Staehling-Hampton K, Appleby M, Brunkow ME, Latham JA (2003) Osteocyte control of bone formation via sclerostin, a novel BMP antagonist. EMBO J 22:6267–6276. doi:10.1093/emboj/cdg599
Wozniak M, Fausto A, Carron CP, Meyer DM, Hruska KA (2000) Mechanically strained cells of the osteoblast lineage organize their extracellular matrix through unique sites of alphavbeta3-integrin expression. J Bone Miner Res 15:1731–1745. doi:10.1359/jbmr.2000.15.9.1731
Wright NC, Lisse JR, Walitt BT, Eaton CB, Chen Z (2011) Arthritis increases the risk for fractures–results from the Women’s Health Initiative. J Rheumatol 38:1680–1688. doi:10.3899/jrheum.101196
Zhang ZM, Li ZC, Jiang LS, Jiang SD, Dai LY (2010) Micro-CT and mechanical evaluation of subchondral trabecular bone structure between postmenopausal women with osteoarthritis and osteoporosis. Osteoporos Int 21:1383–1390. doi:10.1007/s00198-009-1071-2
Zoch ML, Clemens TL, Riddle RC (2016) New insights into the biology of osteocalcin. Bone 82:42–49. doi:10.1016/j.bone.2015.05.046
Acknowledgments
The authors acknowledge ASI (Italian Space Agency) and University of Rome “Tor Vergata” (Spatial Biomedicine Center) for partially founding this study (number search DC-DTE-2011-033). Thanks to S. Cappelli for technical assistance and to M. Feola and C. Rao for collection of clinical data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the University of “Tor Vergata”, Ethic Committees and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study. This article does not contain any studies with animals performed by any of the authors.
Additional information
Handling Editors: S. Beninati, M. Piacentini, C.M. Bergamini.
C. Tarquini and R. Mattera contributed equally to the paper. A. Orlandi and U. Tarantino contributed equally to the paper.
Rights and permissions
About this article
Cite this article
Tarquini, C., Mattera, R., Mastrangeli, F. et al. Comparison of tissue transglutaminase 2 and bone biological markers osteocalcin, osteopontin and sclerostin expression in human osteoporosis and osteoarthritis. Amino Acids 49, 683–693 (2017). https://doi.org/10.1007/s00726-016-2290-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-016-2290-4