Abstract
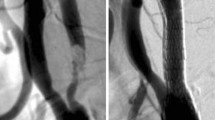
A 74-year-old woman exhibited sensory aphasia with abrupt blood pressure elevation 3 h after clipping of an unruptured large left middle cerebral artery aneurysm. Perfusion computed tomography and single-photon emission computed tomography demonstrated hyperperfusion in one of the distal parent artery areas. She gradually improved and was discharged without neurological deficits. Increased distal blood flow after occlusion of the large cerebral aneurysm and postischemic reperfusion after temporary occlusion of the parent artery during surgery presumably played an important role in the occurrence of this fairly rare condition associated with aneurysm surgery.


Similar content being viewed by others
References
Araki Y, Andoh H, Yamada M, Nakatani K, Andoh T, Sakai N (1999) Permissible arterial occlusion time in aneurysm surgery. Postoperative hyperperfusion caused by temporary clipping. Neurol Med Chir (Tokyo) 39:901–907
Kuroki K, Taguchi H, Yukawa O (2006) Hyperperfusion syndrome after clipping of an unruptured aneurysm. Neurol Med Chir (Tokyo) 46:248–250
Maruya J, Nishimaki K, Minakawa T (2011) Hyperperfusion syndrome after neck clipping of a ruptured aneurysm on a dolichoectatic middle cerebral artery. J Stroke Cerebrovasc Dis 20:260–263
Murakami H, Ibata M, Nakamura A, Ushioda T (2002) Ipsilateral hyperperfusion after neck clipping of a giant internal carotid artery aneurysm. J Neurosurg 97:1233–1236
Schoser BGH, Heesen C, Eckert B, Thie A (1997) Cerebral hyperperfusion injury after percutaneous transluminal angioplasty of extracranial arteries. J Neurol 244:101–104
Sugino T, Ohtaki M, Wanibuchi M, Kin S, Houkin K (2010) Hyperperfusion syndrome after clipping an unruptured cerebral aneurysm. Neurol Med Chir (Tokyo) 50:306–309
Acknowledgments
This study was supported in part by JSPS KAKENHI, grant numbers 25462235 and 26461278.
Patient consent
The patient/next of kin/guardian has consented to the submission of the case report for submission to the journal.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
Comments
Very well written case report describing a case with transient hyperperfusion syndrome after elective surgery for a large MCA bifurcation aneurysm. The authors describe the possible mechanisms, including temporary occlusion of 10 min in total divided into three rounds, but their main hypothesis is that aneurysm occlusion led to an increase in flow through the inferior M2 trunk and hence a hyper perfusion syndrome in the angular area. This is substantiated by their intro flow measurements. Intraoperative Doppler ultrasound flowmetry revealed that the blood flow of the M2 segments distal to the aneurysm before and after clipping were 75 and 50 ml/min (superior trunk) and 22 and 48 ml/min (inferior trunk), respectively. In my personal experience, I have had similar cases, but never performed this thorough intro and post investigations, something I commend the authors for. I use temporary clipping in the vast majority of aneurysm cases and have never seen hyperperfusion syndrome postop unless there was a large or giant aneurysm, so I believe that the hyper perfusion is secondary to clipping of the aneurysm, thereby leading to reduced attenuation of flow in the M2 branches.
Torstein Meling
Oslo, Norway
Rights and permissions
About this article
Cite this article
Kayahara, T., Takeda, R., Kikkawa, Y. et al. Hyperperfusion syndrome after aneurysm surgery: a case report. Acta Neurochir 157, 1855–1857 (2015). https://doi.org/10.1007/s00701-015-2567-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-015-2567-5