Abstract
Background
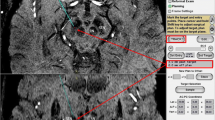
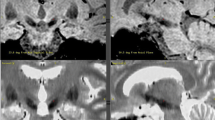
Successful deep brain stimulation is mostly dependent on accurate positioning of the leads at the optimal target points. We investigated whether the identification of the subthalamic nucleus in T2-weighted 3-T MRI, fluid-attenuated inversion recovery 3-T MRI and susceptibility-weighted 3-T MRI is confirmed by intraoperative neurological microelectrode recording.
Methods
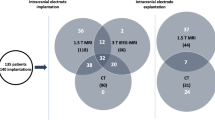
We evaluated 182 microelectrode recording leads in 21 patients with bilateral deep brain stimulation, retrospectively. Consequently, 728 electrode contact positions in T2-weighted 3-T MRI, 552 electrode contact positions in fluid-attenuated inversion recovery 3-T MRI and 490 electrode contact positions in susceptibility-weighted 3-T MRI were evaluated for a positive nucleus subthalamicus signal.
Results
The highest sensitivity was measured for fluid-attenuated inversion recovery 3-T MRI with 82.5 %, while the highest specificity was observed for susceptibility-weighted 3-T MRI with 90.6 %. The negative predictive value was nearly equal for susceptibility-weighted MRI and fluid-attenuated inversion recovery MRI with 87.5 % vs. 87.1 %, but the positive predictive value was higher in susceptibility-weighted 3-T MRI (86.0 %) than in the other MRI sequences.
Conclusions
The susceptibility-weighted 3-T MRI-based subthalamic nucleus localization shows the best accuracy compared with T2-weighted and fluid-attenuated inversion recovery 3-T MRI. Therefore, the susceptibility-weighted 3-T MRI should be preferred for surgical planning when the operation procedure is performed under general anesthesia without microelectrode recordings.




Similar content being viewed by others
References
Saint-Cyr JA, Hoque T, Pereira LC, Dostrovsky JO, Hutchison WD, Mikulis DJ, Abosch A, Sime E, Lang AE, Lozano AM (2002) Localization of clinically effective stimulating electrodes in the human subthalamic nucleus on magnetic resonance imaging. J Neurosurg 97:1152–1166
Starr PA, Christine CW, Theodosopoulos PV, Lindsey N, Byrd D, Mosley A, Marks WJ (2002) Implantation of deep brain stimulators into the sub thalamic nucleus: technical ap- proach and magnetic resonance imaging-verified lead localization. J Neurosurg 97:370–387
Voges J, Volkmann J, Allert N, Lehrke R, Koulousakis A, Freund HJ, Sturm V (2002) Bilateral high-frequency stimulation in the subthalamic nucleus for the treatment of Parkinson disease: correlation of therapeutic effect with anatomical electrode position. J Neurosurg 96:269–279
Hutchison WD, Allan RJ, Opitz H, Levy R, Dostrovsky JO, Lang AE, Lozano AM (1998) Neurophysiological identification of the subthalamic nucleus in surgery for Parkinson’s disease. Ann Neurol 44:622–628
Sterio D, Zonenshayn M, Moligner AY, Rezai AR, Kiprovski K, Kelly PJ, Beric A (2002) Neurophysiological refinement of the subthalamic nucleus targeting. Neurosurg 50:58–67
Carlson JD, Neumiller JJ, Swain LDW, Mark J, McLeod P, Hirschauer J (2014) Postoperative delirium in Parkinson’s disease pateints following deep brain stimulation surgery. J Clin Neurosci 21:1192–1195
Reck C, Maarouf M, Wojtecki L, Groiss SJ, Florin E, Sturm V, Fink GR, Schnitzler A, Timmermann L (2012) Clinical outcome of subthalamic stimulation in Parkinson’s disease is improved by intraoperative multiple trajectories microelectrode recording. J Neurol Surg A Cent Eur Neurosurg 73:377–386
Binder DK, Rau G, Starr PA (2005) Risk factors for hemorrhage during microelectrode-guided deep brain stimulator implantation for movement disorders. Neurosurg 56:722–732
Kerl HU, Gerigk L, Penchlivanis I, Al-Zghloul M, Groden C, Noelte I (2012) The subthalamic nucleus at 3.0 Tesla: choice of optimal sequence and orientation for deep brain stimulation using a standard installation protocol: clinical article. J Neurosurg 117:1155–1165
Nakajima T, Zrinzo L, Foltynie T, Olmos IA, Taylor C, Hariz MI, Limousin P (2011) MRI-guided subthalamic nucleus deep brain stimulation without microelectrode recording: can we dispense with surgery under local anaesthesia? Stereotact Funct Neurosurg 89:318–325
Schlaier JR, Habermeyer C, Janzen A, Felnner C, Hochreiter A, Proescholdt M, Brawanski A, Lange M (2013) The influence of intraoperative microelectrode recordings and clinical testing on the location of final stimulation sites in deep brain stimulation for Parkinson’s disease. Acta Neurochir 155:357–366
Zeiler FA, Wilkinson M, Krcek JP (2013) Subthalamic nucleus deep brain stimulation: an invaluable role of MER. Can J Neurol Sci 40:572–575
Schlaier JR, Habermeyer C, Warnat J, Lange M, Janzen A, Hochreiter A, Proescholdt M, Brawanski A, Fellner C (2011) Discrepancies between the MRI- and the electrophysiologically defined subthalamic nucleus. Acta Neurochir 12:2307–2318
Harries AM, Kausar J, Robterts SA, Mocroft AP, Hodson JA, Pall HS, Mitchell RD (2012) Deep brain stimulation of the subthalamic nucleus for advanced Parkinson disease using general anesthesia: long-term results. J Neurosurg 116:107–113
Conflicts of interest
None.
Full Financial Disclosures of All Authors for the Past Year
Klaus D. Martin, Kay Engellandt, Rüdiger von Kummer, Lisa Klingelhoefer, Alexander Storch, Mareike Fauser, Stephan B. Sobottka and Gabriele Schackert have no financial disclosures. Witold H. Polanski have received a travel grant (10/2013-04/2014) and a poster price (08/2013) from Medtronic.
Contributorship statement
All authors contributed to the conception and design, acquisition of the data or analysis and interpretation of the data; drafting of the article or revising it critically for important intellectual content; and final approval of the version to be published.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
Table (suppl). MRI parameters of the used T2 3-T MRI, fluid-attenuated inversion recovery 3-T MRI and susceptibility-weighted 3-T MRI (DOC 28 kb)
Rights and permissions
About this article
Cite this article
Polanski, W.H., Martin, K.D., Engellandt, K. et al. Accuracy of subthalamic nucleus targeting by T2, FLAIR and SWI-3-Tesla MRI confirmed by microelectrode recordings. Acta Neurochir 157, 479–486 (2015). https://doi.org/10.1007/s00701-014-2328-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-014-2328-x