Abstract
Purpose
The body mass index (BMI) before lung transplantation (LT) is a benchmark of the post-LT survival. The aim of the study is to determine the BMI inadequate for the post-LT survival.
Methods
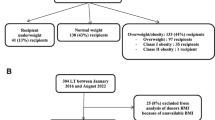
We examined the survival after LT in patients grouped into the following BMI categories: <18.5 kg/m2 (underweight), 18.5–24.9 kg/m2 (normal weight), 25–29.9 kg/m2 (overweight), and ≥30.0 kg/m2 (obese) according to the World Health Organization (WHO) criteria. A more detailed categorization was made for further evaluation of the underweight group: mild (17.0 ≤ BMI < 18.5 kg/m2) and severely underweight (BMI <17.0 kg/m2).
Results
There was no statistically significant difference in the post-LT survival between underweight and normal-weight patients (5-year survival: 78.7 vs. 76.1%). Patients with BMI <17.0 kg/m2 had a worse prognosis than those with 17.0 ≤ BMI < 18.5 kg/m2 (5-year survival: 70.3 vs. 90.0%).
Conclusions
Standard BMI categorization per the WHO criteria is inadequate for determining the post-LT survival, especially in underweight patients. For the nutritional evaluation of underweight pre-LT patients, BMI <17.0 kg/m2 should be used instead of BMI <18.5 kg/m2.


Similar content being viewed by others
References
Unilateral lung transplantation for pulmonary fibrosis. Toronto lung transplant group. N Engl J Med. 1986;314(18):1140–5.
Chen F, Oga T, Yamada T, Sato M, Aoyama A, Chin K, et al. Lung allocation score and health-related quality of life in Japanese candidates for lung transplantation. Interact Cardiovasc Thorac Surg. 2015;21(1):28–33.
Miyoshi R, Chen-Yoshikawa TF, Hijiya K, Motoyama H, Aoyama A, Menju T, et al. Significance of single lung transplantation in the current situation of severe donor shortage in Japan. Gen Thorac Cardiovasc Surg. 2016;64(2):93–7.
Sayegh MH, Carpenter CB. Transplantation 50 years later—progress, challenges, and promises. N Engl J Med. 2004;351(26):2761–6.
Weill D, Benden C, Corris PA, Dark JH, Davis RD, Keshavjee S, et al. A consensus document for the selection of lung transplant candidates: 2014—an update from the pulmonary transplantation council of the international society for heart and lung transplantation. J Heart Lung Transplant. 2015;34(1):1–15.
Allen JG, Arnaoutakis GJ, Weiss ES, Merlo CA, Conte JV, Shah AS. The impact of recipient body mass index on survival after lung transplantation. J Heart Lung Transplant. 2010;29(9):1026–33.
Culver DA, Mazzone PJ, Khandwala F, Blazey HC, Decamp MM, Chapman JT. Discordant utility of ideal body weight and body mass index as predictors of mortality in lung transplant recipients. J Heart Lung Transplant. 2005;24(2):137–44.
de la Torre MM, Delgado M, Paradela M, Gonzalez D, Fernandez R, Garcia JA, et al. Influence of body mass index in the postoperative evolution after lung transplantation. Transplant Proc. 2010;42(8):3026–8.
Madill J, Gutierrez C, Grossman J, Allard J, Chan C, Hutcheon M, et al. Nutritional assessment of the lung transplant patient: Body mass index as a predictor of 90-day mortality following transplantation. J Heart Lung Transplant. 2001;20(3):288–96.
Ruttens D, Verleden SE, Vandermeulen E, Vos R, van Raemdonck DE, Vanaudenaerde BM, et al. Body mass index in lung transplant candidates: a contra-indication to transplant or not? Transplant Proc. 2014;46(5):1506–10.
Souza SM, Nakasato M, Bruno ML, Macedo A. Nutritional profile of lung transplant candidates. Jornal brasileiro de pneumologia : publicacao oficial da Sociedade Brasileira de Pneumologia e Tisilogia. 2009;35(3):242–7.
Obesity: preventing and managing the global epidemic. Report of a who consultation. World Health Organ Tech Rep Ser. 2000;894:i-xii, 1–253.
Christie JD, Bavaria JE, Palevsky HI, Litzky L, Blumenthal NP, Kaiser LR, et al. Primary graft failure following lung transplantation. Chest. 1998;114(1):51–60.
Christie JD, Sager JS, Kimmel SE, Ahya VN, Gaughan C, Blumenthal NP, et al. Impact of primary graft failure on outcomes following lung transplantation. Chest. 2005;127(1):161–5.
Shah RJ, Diamond JM, Cantu E, Flesch J, Lee JC, Lederer DJ, et al. Objective estimates improve risk stratification for primary graft dysfunction after lung transplantation. Am J Transplant. 2015;15(8):2188–96.
Chen F, Date H. Update on ischemia–reperfusion injury in lung transplantation. Curr Opin Organ Transplant. 2015;20(5):515–20.
Mizota T, Miyao M, Yamada T, Sato M, Aoyama A, Chen F, et al. Graft dysfunction immediately after reperfusion predicts short-term outcomes in living-donor lobar lung transplantation but not in cadaveric lung transplantation. Interact Cardiovasc Thorac Surg. 2016;22(3):314–20.
Kuntz CL, Hadjiliadis D, Ahya VN, Kotloff RM, Pochettino A, Lewis J, et al. Risk factors for early primary graft dysfunction after lung transplantation: a registry study. Clin Transplant. 2009;23(6):819–30.
Lederer DJ, Kawut SM, Wickersham N, Winterbottom C, Bhorade S, Palmer SM, et al. Obesity and primary graft dysfunction after lung transplantation: the lung transplant outcomes group obesity study. Am J Respir Crit Care Med. 2011;184(9):1055–61.
Singer JP, Peterson ER, Snyder ME, Katz PP, Golden JA, D’Ovidio F, et al. Body composition and mortality after adult lung transplantation in the united states. Am J Respir Crit Care Med. 2014;190(9):1012–21.
Hoffman SA, Wang L, Shah CV, Ahya VN, Pochettino A, Olthoff K, et al. Plasma cytokines and chemokines in primary graft dysfunction post-lung transplantation. Am J Transplant. 2009;9(2):389–96.
Mathur A, Baz M, Staples ED, Bonnell M, Speckman JM, Hess PJ Jr., et al. Cytokine profile after lung transplantation: correlation with allograft injury. Ann Thorac Surg. 2006;81(5):1844–9 (discussion 1849–1850).
Geurden B, Franck E, Weyler J, Ysebaert D. The risk of malnutrition in community-living elderly on admission to hospital for major surgery. Acta Chir Belg. 2015;115(5):341–7.
Chamogeorgakis T, Mason DP, Murthy SC, Thuita L, Raymond DP, Pettersson GB, et al. Impact of nutritional state on lung transplant outcomes. J Heart Lung Transplant. 2013;32(7):693–700.
Cheng GS, Edelman JD, Madtes DK, Martin PJ, Flowers ME. Outcomes of lung transplantation after allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transpl. 2014;20(8):1169–75.
Ri M, Miyata H, Aikou S, Seto Y, Akazawa K, Takeuchi M, et al. Effects of body mass index (BMI) on surgical outcomes: a nationwide survey using a Japanese web-based database. Surg Today. 2015;45(10):1271–9.
Keevil VL, Romero-Ortuno R. Ageing well: a review of sarcopenia and frailty. Proc Nutr Soc. 2015 74:337–47.
van Stijn MF, Korkic-Halilovic I, Bakker MS, van der Ploeg T, van Leeuwen PA, Houdijk AP. Preoperative nutrition status and postoperative outcome in elderly general surgery patients: a systematic review. JPEN J Parenter Enter Nutr. 2013;37(1):37–43.
Tanaka S, Chen-Yoshikawa TF, Yamada T, Hijiya K, Motoyama H, Aoyama A, et al. Malignancies after living-donor and cadaveric lung transplantations in Japanese patients. Surg Today. 2016;46(12):1415–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has a financial relationship with a commercial entity that has an interest in the subject of the presented manuscript or other conflicts of interest to disclose.
Rights and permissions
About this article
Cite this article
Komatsu, T., Chen-Yoshikawa, T.F., Oshima, A. et al. Severe underweight decreases the survival rate in adult lung transplantation. Surg Today 47, 1243–1248 (2017). https://doi.org/10.1007/s00595-017-1508-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-017-1508-8