Abstract
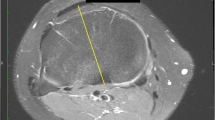
Commonly used total knee arthroplasty (TKA) systems utilising measured resection techniques default to 5°–7° valgus for the distal cut relative to the anatomical axis and 3° external rotation of the femoral component relative to posterior condylar axis (PCA). Rotational errors of the femoral component are associated with pain, patella maltracking and a poorer outcome. We analysed MRI scans from patients undergoing TKA using patient-specific instrumentation to assess coronal and rotational alignment from landmarks identified on the scans. One hundred and eight scans in 59 males and 49 females were studied with age range 35–93 years (mean 67.9 years). We found 91 % of patients had a femoral valgus angle between 5° and 7° (mean angles 5.9°), while only 24 % had an external rotation angle between 2.5° and 3.5° relative to PCA. There was no statistical significance in rotation between males and females although outliers tended to be female. Mean Whiteside’s angle was 92.9° (87.8–98). This study highlights the variations in external rotation between patients undergoing TKA using the PCA as a reference for rotation. This may be a contributing factor in implant malalignment and patient dissatisfaction.


Similar content being viewed by others
References
The National Joint Registry for England and Wales: 11th annual report (2014). http://www.njrreports.ork.uk. Accessed 3 May 2015
Green GV et al (2002) The effects of varus tibial alignment on proximal tibial surface strain in total knee arthroplasty: the posteromedial hotspot. J Arthroplasty 17:1033–1039
Algietti P, Sensi L, Cuomo P, Ciardullo A (2008) Rotational position of femoral and tibial components in TKA using the femoral transepicondylar axis. Clin Orthop Relat Res 466:2751–2755
Victor J (2009) Rotational alignment of the distal femur: a literature review. Orthop Traumatol Surg Res 95:365–372
Jerosch J, Peuker E, Philipps B, Filler T (2002) Interindividual reproducibility in perioperative rotational alignment of femoral components in knee prosthetic surgery using the transepicondylar axis. Knee Surg Sports Traumatol Arthrosc 10(3):194–197
Barrack R et al (2001) Component rotation and anterior knee pain after total knee arthroplasty. Clin Orthop Relat Res 392:46–55
Berger RA, Rubash HE, Sell MJ et al (1993) Determining the rotational alignment of the femoral component in total knee arthroplasty using the epicondylar axis. Clin Orthop Relat Res 286:40–47
Akagi M, Yamashita E et al (2001) Relationship between frontal knee alignment and reference axes in the distal femur. Clin Orthop Relat Res 388:147–156
Olcott C, Scott R (1999) Femoral component rotation during total knee arthroplasty. Clin Orthop Relat Res 367:39–42
Stoeckl B et al (2006) Reliability of the transepicondylar axis as an anatomical landmark in total knee arthroplasty. J Arthroplasty 21(6):878–882
Bédard M, Vince KG, Redfern J, Collen SR (2011) Internal rotation of the tibial component is frequent in stiff total knee arthroplasty. Clin Orthop Relat Res 469:2346–2355
Matsuda S, Kawahara S, Okazaki K, Tashiro Y, Iwamoto Y (2013) Postoperative alignment and ROM affect patient satisfaction after TKA. Clin Orthop 471(1):127–133
Matsuda S et al (2001) Effect of femoral and tibial component position on patellar tracking following total knee arthroplasty: 10-year follow-up of Miller–Galante I knees. Am J Knee Surg 14:152–156
Berger RA et al (1998) Malrotation causing patellofemoral complications after total knee arthroplasty. Clin Orthop Relat Res 356:144–153
Dossett H et al (2012) Kinematically versus mechanically aligned total knee arthroplasty. Orthopedics 35(2):e160–e169
Chareancholvanich K, Narkhunnam R, Pornrattanamaneewong C (2013) A prospective randomised controlled trial of patient specific cutting guides compared with conventional instrumentation in total knee replacement. Bone Joint J 95-B:354–359
Barrack R et al (2012) Patient specific cutting blocks are currently of no proven value. J Bone Joint Surg 94-B(Supple A):95–99
Boonen B et al (2013) Intra-operative results and radiological outcome of conventional and patient specific surgery in total knee arthroplasty: multicentre, randomized control trial. Knee Surg Sports Traumatol Athrosc 21(10):2206–2212
Chen JY et al (2014) The radiological outcomes of patient-specific instrumentation versus conventional total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 22(3):630–635
Koch PP et al (2013) Radiographic accuracy in TKA with a CT-based patient specific cutting block technique versus imageless, computer assisted surgery system in total knee arthroplasty. Knee 20(4):263–267
Daniilidis K et al (2013) Frontal plane alignment after total knee arthroplasty using patient-specific instruments. Int Orthop 37(1):45–50
Heyse T et al (2012) MRI analysis for rotation of total knee replacements. Knee 19(5):571–575
Chotanaphuti T et al (2014) The accuracy of component alignment in custom cutting blocks compared with conventional total knee arthroplasty instrumentation: prospective control trial. Knee 21(1):185–188
Frye B, Najim A, Adams J, Berend K, Lombardi A (2015) MRI is more accurate than CT for patient-specific total knee arthroplasty. Knee. doi:10.1016/j.knee.2015.02.014
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical standard
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Jones, C., Nawaz, Z., Hassan, A. et al. The variability in the external rotation axis of the distal femur: an MRI-based anatomical study. Eur J Orthop Surg Traumatol 26, 199–203 (2016). https://doi.org/10.1007/s00590-015-1719-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-015-1719-x