Abstract
Background
Tranexamic acid (TXA) is well established as a versatile intraarticular and intravenous (IV) antifibrinolytic agent that has been successfully used to control bleeding after total knee arthroplasty (TKA). The present meta-analysis aimed at assessing the effectiveness and safety of TXA in reducing blood loss and transfusion in TKA.
Methods
We searched the PubMed, Medline, Embase, Cochrane Central Register of Controlled Trials, and Google Scholar databases from 1966 to December 2013. Only randomized controlled trials (RCTs) were included in the present study. Two independent reviewers identified the eligible studies, assessed their methodological quality, and extracted data. The data were using fixed-effects or random-effects models with standard mean differences and risk ratios for continuous and dichotomous variables, respectively. Subgroup analysis was performed according to the IV or intraarticular administration of TXA.
Results
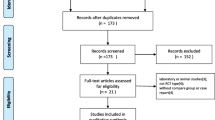
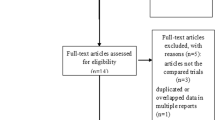
Thirty-four RCTs encompassing 2,594 patients met the inclusion criteria for our meta-analysis. Our meta-analysis indicated that when compared with the control group, the IV or intraarticular use of TXA significantly reduced total blood loss, postoperative blood loss, Hb loss, and transfusion rate as well as blood units transfused per patient after primary TKA, but did not reduce intraoperative blood loss. No significant difference in deep vein thrombosis (DVT), pulmonary embolism, or other adverse events among the study groups.
Conclusions
IV or intraarticular use of TXA for patients undergoing TKA is effective and safe for the reduction blood loss and blood transfusion requirements, yet does not increase the risk of postoperative DVT.
Level of evidence
Level II.








Similar content being viewed by others
References
Park JH, Rasouli MR, Mortazavi SM, Tokarski AT, Maltenfort MG, Parvizi J (2013) Predictors of perioperative blood loss in total joint arthroplasty. J Bone Joint Surg Am 95(19):1777–1783
Banerjee S, Kapadia BH, Issa K, McElroy MJ, Khanuja HS, Harwin SF, Mont MA (2013) Postoperative blood loss prevention in total knee arthroplasty. J Knee Surg 26(6):395–400
Vielpeau C (2012) Perioperative bleeding and early mortality in hip and knee surgery. Orthop Traumatol Surg Res 98(5):475–476
Alshryda S, Mason J, Vaghela M, Sarda P, Nargol A, Maheswaran S, Tulloch C, Anand S, Logishetty R, Stothart B, Hungin AP (2013) Topical (intra-articular) tranexamic acid reduces blood loss and transfusion rates following total knee replacement: a randomized controlled trial (TRANX-K). J Bone Joint Surg Am 95(21):1961–1968
Schreiber GB, Busch MP, Kleinman SH, Korelitz JJ (1996) The risk of transfusion transmitted viral infections: the retrovirus epidemiology donor study. N Engl J Med 334(26):1685–1690
Muñoz M, Cobos A, Campos A (2014) Low vacuum re-infusion drains after total knee arthroplasty: is there a real benefit? Blood Transfus 12(Suppl 1):s173–s175
Horstmann W, Kuipers B, Ohanis D, Slappendel R, Kollen B, Verheyen C (2014) Autologous re-transfusion drain compared with no drain in total knee arthroplasty: a randomised controlled trial. Blood Transfus 12(Suppl 1):s176–s181
Perazzo P, Viganò M, De Girolamo L, Verde F, Vinci A, Banfi G, Romagnoli S (2013) Blood management and transfusion strategies in 600 patients undergoing total joint arthroplasty: an analysis of pre-operative autologous blood donation. Blood Transfus 11(3):370–376
Hardy JF, Desroches J (1992) Natural and synthetic antifibrino-lytics in cardiac surgery. Can J Anaesth 39(4):353–365
Abrishami A, Chung F, Wong J (2009) Topical application of antifibrinolytic drugs for on-pump cardiac surgery: a systematic review and meta-analysis. Can J Anaesth 56(3):202–212
Ker K, Edwards P, Perel P, Shakur H, Roberts I (2012) Effect of tranexamic acid on surgical bleeding: systematic review and cumulative meta-analysis. BMJ 344:e3054
Zhang H, Chen J, Chen F, Que W (2012) The effect of tranexamic acid on blood loss and use of blood products in total knee arthroplasty: a meta-analysis. Knee Surg Sports Traumatol Arthrosc 20(9):1742–1752
Aguilera X, Martinez-Zapata MJ, Bosch A, Urrútia G, González JC, Jordan M, Gich I, Maymó RM, Martínez N, Monllau JC, Celaya F, Fernández JA (2013) Efficacy and safety of fibrin glue and tranexamic Acid to prevent postoperative blood loss in total knee arthroplasty: a randomized controlled clinical trial. J Bone Joint Surg Am 95(22):2001–2007
Chareancholvanich K, Siriwattanasakul P, Narkbunnam R, Pornrattanamaneewong C (2012) Temporary clamping of drain combined with tranexamic acid reduce blood loss after total knee arthroplasty: a prospective randomized controlled trial. BMC Musculoskelet Disord 13:124
Georgiadis AG, Muh SJ, Silverton CD, Weir RM, Laker MW (2013) A prospective double-blind placebo controlled trial of topical tranexamic acid in total knee arthroplasty. J Arthroplasty 28(8 Suppl):78–82
Kim TK, Chang CB, Kang YG, Seo ES, Lee JH, Yun JH, Lee SH (2014) Clinical value of tranexamic acid in unilateral and simultaneous bilateral TKAs under a contemporary blood-saving protocol: a randomized controlled trial. Knee Surg Sports Traumatol Arthrosc 22(8):1870–1878
Lee SH, Cho KY, Khurana S, Kim KI (2013) Less blood loss under concomitant administration of tranexamic acid and indirect factor Xa inhibitor following total knee arthroplasty: a prospective randomized controlled trial. Knee Surg Sports Traumatol Arthrosc 21(11):2611–2617
Martin JG, Cassatt KB, Kincaid-Cinnamon KA, Westendorf DS, Garton AS, Lemke JH (2014) Topical administration of tranexamic acid in primary total hip and total knee arthroplasty. J Arthroplasty 29(5):889–894
Pachauri A, Acharya KK, Tiwari AK (2013) The effect of tranexamic acid on hemoglobin levels during total knee arthroplasty. Am J Ther 21(5):366–370
Roy SP, Tanki UF, Dutta A, Jain SK, Nagi ON (2012) Efficacy of intra-articular tranexamic acid in blood loss reduction following primary unilateral total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 20(12):2494–2501
Seo JG, Moon YW, Park SH, Kim SM, Ko KR (2013) The comparative efficacies of intra-articular and IV tranexamic acid for reducing blood loss during total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 21(8):1869–1874
Abrishami A (2010) Timing and volume of topical tranexamic acid administration for postoperative blood loss in total knee arthroplasty. Can J Anesth 51:S142–S143
Alvarez JC, Santiveri FX, Ramos I, Vela E, Puig L, Escolano F (2008) Tranexamic acid reduces blood transfusion in total knee arthroplasty even when a blood conservation program is applied. Transfusion 48(3):519–525
Benoni G, Fredin H (1996) Fibrinolytic inhibition with tranexamic acid reduces blood loss and blood transfusion after knee arthroplasty: a prospective, randomised, double-blind study of 86 patients. J Bone Joint Surg Br 78(3):434–440
Camarasa MA, Ollé G, Serra-Prat M, Martín A, Sánchez M, Ricós P, Pérez A, Opisso L (2006) Efficacy of aminocaproic, tranexamic acids in the control of bleeding during total knee replacement: a randomized clinical trial. Br J Anaesth 96(5):576–582
Charoencholvanich K, Siriwattanasakul P (2011) Tranexamic acid reduces blood loss and blood transfusion after TKA: a prospective randomized controlled trial. Clin Orthop Relat Res 469(10):2874–2880
Ellis MH, Fredman B, Zohar E, Ifrach N, Jedeikin R (2001) The effect of tourniquet application, tranexamic acid, and desmopressin on the procoagulant and fibrinolytic systems during total knee replacement. J Clin Anesth 13(7):509–513
Engel JM, Hohaus T, Ruwoldt R, Menges T, Jürgensen I, Hempelmann G (2001) Regional hemostatic status and blood requirements after total knee arthroplasty with and without tranexamic acid or aprotinin. Anesth Analg 92(3):775–780
Gautam PL, Katyal S, Yamin M, Singh A (2011) Effect of tranexamic acid on blood loss and transfusion requirement in total knee replacement in the Indian population: a case series. Indian J Anaesth 55(6):590–593
Good L, Peterson E, Lisander B (2003) Tranexamic acid decreases external blood loss but not hidden blood loss in total knee replacement. Br J Anaesth 90(5):596–599
Hiippala ST, Strid LJ, Wennerstrand MI, Arvela JV, Niemelä HM, Mäntylä SK, Kuisma RP, Ylinen JE (1997) Tranexamic acid radically decreases blood loss and transfusions associated with total knee arthroplasty. Anesth Analg 84(4):839–844
Hiippala S, Strid L, Wennerstrand M, Arvela V, Mäntylä S, Ylinen J, Niemelä H (1995) Tranexamic acid (Cyklokapron) reduces perioperative blood loss associated with total knee arthroplasty. Br J Anaesth 74(5):534–537
Ishida K, Tsumura N, Kitagawa A, Hamamura S, Fukuda K, Dogaki Y, Kubo S, Matsumoto T, Matsushita T, Chin T, Iguchi T, Kurosaka M, Kuroda R (2011) Intra-articular injection of tranexamic acid reduces not only blood loss but also knee joint swelling after total knee arthroplasty. Int Orthop 35(11):1639–1645
Jansen AJ, Andreica S, Claeys M, D’Haese J, Camu F, Jochmans K (1999) Use of tranexamic acid for an effective blood conservation strategy after total knee arthroplasty. Br J Anaesth 83(4):596–601
Kakar PN, Gupta N, Govil P, Shah V (2009) Efficacy and safety of tranexamic acid in control of bleeding following TKR: a randomized clinical trial. Indian J Anaesth 53(6):667–671
Maniar RN, Kumar G, Singhi T, Nayak RM, Maniar PR (2012) Most effective regimen of tranexamic acid in knee arthroplasty: a prospective randomized controlled study in 240 patients. Clin Orthop Relat Res 470(9):2605–2612
McConnell JS, Shewale S, Munro NA, Shah K, Deakin AH, Kinninmonth AW (2012) Reducing blood loss in primary knee arthroplasty: a prospective randomised controlled trial of tranexamic acid and fibrin spray. Knee 19(4):295–298
Molloy DO, Archbold HA, Ogonda L, McConway J, Wilson RK, Beverland DE (2007) Comparison of topical fibrin spray and tranexamic acid on blood loss after total knee replacement: a prospective, randomised controlled trial. J Bone Joint Surg Br 89(3):306–309
Onodera T, Majima T, Sawaguchi N, Kasahara Y, Ishigaki T, Minami A (2012) Risk of deep venous thrombosis in drain clamping with tranexamic acid and carbazochrome sodium sulfonate hydrate in total knee arthroplasty. J Arthroplasty 27(1):105–108
Orpen NM, Little C, Walker G, Crawfurd EJ (2006) Tranexamic acid reduces early post-operative blood loss after total knee arthroplasty: a prospective randomised controlled trial of 29 patients. Knee 13(2):106–110
Tanaka N, Sakahashi H, Sato E, Hirose K, Ishima T, Ishii S (2001) Timing of the administration of tranexamic acid for maximum reduction in blood loss in arthroplasty of the knee. J Bone Joint Surg Br 83(5):702–705
Veien M, Sørensen JV, Madsen F, Juelsgaard P (2002) Tranexamic acid given intraoperatively reduces blood loss after total knee replacement: a randomized, controlled study. Acta Anaesthesiol Scand 46(10):1206–1211
Wong J, Abrishami A, El Beheiry H, Mahomed NN, Roderick Davey J, Gandhi R, Syed KA, Muhammad Ovais Hasan S, De Silva Y, Chung F (2010) Topical application of tranexamic acid reduces postoperative blood loss in total knee arthroplasty: a randomized, controlled trial. J Bone Joint Surg Am 92(15):2503–2513
Zhang F, Gao Z, Yu J (2007) Clinical comparative studies on effect of tranexamic acid on blood loss associated with total knee arthroplasty. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi 21(12):1302–1304
Zohar E, Ellis M, Ifrach N, Stern A, Sapir O, Fredman B (2004) The postoperative blood-sparing efficacy of oral versus intravenous tranexamic acid after total knee replacement. Anesth Analg 99(6):1679–1683
Tan J, Chen H, Liu Q, Chen C, Huang W (2013) A meta-analysis of the effectiveness and safety of using tranexamic acid in primary unilateral total knee arthroplasty. J Surg Res 184(2):880–887
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wu, Q., Zhang, HA., Liu, SL. et al. Is tranexamic acid clinically effective and safe to prevent blood loss in total knee arthroplasty? A meta-analysis of 34 randomized controlled trials. Eur J Orthop Surg Traumatol 25, 525–541 (2015). https://doi.org/10.1007/s00590-014-1568-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-014-1568-z