Abstract
Purpose
The purpose of this study is to compare clinical patient-reported outcomes and radiographic sagittal parameters between obese and non-obese patients following open posterior lumbar spine fusion (PLSF).
Methods
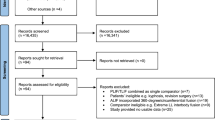
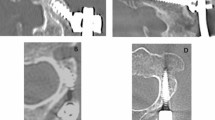
A retrospective cohort study was conducted for patients who underwent open PLSF from 2011 to 2018. Patients were classified as obese as per Center for Disease Control and Prevention guidelines if their body mass index (BMI) ≥ 30 kg/m2. Preoperative and final visual analog scale (VAS) back pain, VAS leg pain, and Oswestry Disability Index (ODI) were obtained for both obese and non-obese groups. Achievement of minimal clinically important difference was evaluated. Preoperative, immediate postoperative, and final lumbar plain radiographs were assessed to measure spinopelvic parameters. Additionally, postoperative complication measures were collected.
Results
A total of 569 patients were included; 290 (50.97%) patients with BMI < 30 (non-obese) and 279 (49.03%) patients with BMI ≥ 30 (obese). Patients classified as obese were more likely to have a diagnosis of diabetes mellitus (p < 0.001), and American Society of Anesthesiologists Physical Status Classification System of ≥ 3 (p < 0.001). Obese patients had significantly longer operative times (p < 0.001) compared to non-obese patients. There was no difference in radiographic measurements, patient-reported outcomes, postoperative complications, or reoperations between groups.
Conclusion
Obese patients had significantly more comorbidities and longer operative time compared to non-obese patients. However, sagittal parameters, patient-reported outcomes, inpatient complications, length of hospital stay, and reoperations were similar between groups. Given these findings, open PLSF can be considered safe and effective in obese patients after thorough consideration of related comorbidities.
Graphic abstract
These slides can be retrieved under Electronic Supplementary Material.

Similar content being viewed by others
References
Sorimachi Y, Neva MH, Vihtonen K, Kyrola K, Iizuka H, Takagishi K, Hakkinen A (2016) Effect of obesity and being overweight on disability and pain after lumbar fusion: an analysis of 805 patients. Spine 41(9):772–777
De la Garza-Ramos R, Bydon M, Abt NB, Sciubba DM, Wolinsky JP, Bydon A, Gokaslan ZL, Rabin B, Witham TF (2015) The impact of obesity on short- and long-term outcomes after lumbar fusion. Spine 40(1):56–61
Shamji MF, Parker S, Cook C, Pietrobon R, Brown C, Isaacs RE (2009) Impact of body habitus on perioperative morbidity associated with fusion of the thoracolumbar and lumbar spine. Neurosurgery 65(3):490–498
Vaidya R, Carp J, Bartol S, Ouellette N, Lee S, Sethi A (2009) Lumbar spine fusion in obese and morbidly obese patients. Spine 34(5):495–500
Kalanithi PA, Arrigo R, Boakye M (2012) Morbid obesity increases cost and complication rates in spinal arthrodesis. Spine 37(11):982–988
Puvanesarajah V, Werner BC, Cancienne JM, Jain A, Pehlivan H, Shimer AL, Singla A, Shen F, Hassanzadeh H (2017) Morbid obesity and lumbar fusion in patients older than 65 years: complications, readmissions, costs, and length of stay. Spine 42(2):122–127
Patel N, Bagan B, Vadera S, Maltenfort MG, Deutsch H, Vaccaro AR, Harrop J, Sharan A, Ratliff JK (2007) Obesity and spine surgery: relation to perioperative complications. J Neurosurg Spine 6(4):291–297
Basques BA, Fu MC, Buerba RA, Bohl DD, Golinvaux NS, Grauer JN (2014) Using the ACS-NSQIP to identify factors affecting hospital length of stay after elective posterior lumbar fusion. Spine 39(6):497–502
Puvanesarajah V, Nourbakhsh A, Hassanzadeh H, Shimer AL, Shen FH, Singla A (2016) Readmission rates, reasons, and risk factors in elderly patients treated with lumbar fusion for degenerative pathology. Spine 41(24):1933–1938
Djurasovic M, Bratcher KR, Glassman SD, Dimar JR, Carreon LY (2008) The effect of obesity on clinical outcomes after lumbar fusion. Spine 33(16):1789–1792
Lingutla KK, Pollock R, Benomran E, Purushothaman B, Kasis A, Bhatia CK, Krishna M, Friesem T (2015) Outcome of lumbar spinal fusion surgery in obese patients: a systematic review and meta-analysis. Bone Joint J 97(10):1395–1404
Lamartina C, Berjano P (2014) Classification of sagittal imbalance based on spinal alignment and compensatory mechanisms. Eur Spine J 23(6):1177–1189
Klineberg E, Schwab F, Smith JS, Gupta MC, Lafage V, Bess S (2013) Sagittal spinal pelvic alignment. Neurosurg Clin N Am 24(2):157–162
Le Huec JC, Faundez A, Dominguez D, Hoffmeyer P, Aunoble S (2015) Evidence showing the relationship between sagittal balance and clinical outcomes in surgical treatment of degenerative spinal diseases: a literature review. Int Orthop 39(1):87–95
Romero-Vargas S, Zarate-Kalfopulos B, Otero-Camara E, Rosales-Olivarez L, Alpizar-Aguirre A, Morales-Hernandez E, Reyes-Sanchez A (2013) The impact of body mass index and central obesity on the spino-pelvic parameters: a correlation study. Eur Spine J 22(4):878–882
Motta MMD, Pratali RR, Coutinho MAC, Hoffman CB, Barsotti CEG, Santos FPED (2015) Oliveira CEASD: correlation between obesity, sagittal balance and clinical outcome in spinal fusion. Coluna/Columna 14(3):186–189
Dripps RD, Sergent WF (1963) New classification of physical status. Anesthesiology 24:111
Parker SL, Adogwa O, Paul AR, Anderson WN, Aaronson O, Cheng JS, McGirt MJ (2011) Utility of minimum clinically important difference in assessing pain, disability, and health state after transforaminal lumbar interbody fusion for degenerative lumbar spondylolisthesis. J Neurosurg Spine 14(5):598–604
Sun X, Zeng R, Li G, Wei B, Hu Z, Lin H, Chen G, Chen S, Sun J (2015) Comparison of effectiveness and change of sagittal spino-pelvic parameters between minimally invasive transforaminal and conventional open posterior lumbar interbody fusions in treatment of low-degree isthmic lumbar spondylolisthesis. Chin J Repar Reconstr Surg 29(12):1504–1509
Park P, Wang MY, Nguyen S, Mundis GM Jr, La Marca F, Uribe JS, Anand N, Okonkwo DO, Kanter AS, Fessler R et al (2016) Comparison of complications and clinical and radiographic outcomes between nonobese and obese patients with adult spinal deformity undergoing minimally invasive surgery. World Neurosurg 87:55–60
Jalai CM, Diebo BG, Cruz DL, Poorman GW, Vira S, Buckland AJ, Lafage R, Bess S, Errico TJ, Lafage V et al (2017) The impact of obesity on compensatory mechanisms in response to progressive sagittal malalignment. Spine J 17(5):681–688
Esposito CI, Miller TT, Kim HJ, Barlow BT, Wright TM, Padgett DE, Jerabek SA, Mayman DJ (2016) Does degenerative lumbar spine disease influence femoroacetabular flexion in patients undergoing total hip arthroplasty? Clin Orthop Relat Res 474(8):1788–1797
Sielatycki JA, Chotai S, Stonko D, Wick J, Kay H, McGirt MJ, Devin CJ (2016) Is obesity associated with worse patient-reported outcomes following lumbar surgery for degenerative conditions? Eur Spine J 25(5):1627–1633
Andreshak TG, An HS, Hall J, Stein B (1997) Lumbar spine surgery in the obese patient. J Spinal Disord 10(5):376–379
Suess O, Kombos T, Bode F (2016) The negligible influence of chronic obesity on hospitalization, clinical status, and complications in elective posterior lumbar interbody fusion. Int J Chronic Dis 2016:2964625
Elgafy H, O’Brien P, Blessinger B, Hassan A (2012) Challenges of spine surgery in obese patients. Am J Ortho 41(3):E46–E50
Rosenfeld HE, Limb R, Chan P, Fitzgerald M, Bradley WP, Rosenfeld JV (2013) Challenges in the surgical management of spine trauma in the morbidly obese patient: a case series. J Neurosurg Spine 19(1):101–109
Funding
No funds were received in support of this work. No benefits in any form have been or will be received from any commercial party related directly or indirectly to the subject of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Jannat M. Khan, Bryce A. Basques, Kyle K. Kunze, Gagan Grewal, Young Soo Hong, Coralie Pardo, Philip K. Louie, and Matthew Colman declare that they have no conflict of interest. Howard S. An reports other from U&I Inc., Zimmer, Articular Engineering LLC, Medyssey Inc., Spinal Kinetics, Bioventis, Stryker, American Journal of Orthopaedics, Spine Journal, with grants from Medyssey Inc., and Spinalcyte Inc., outside the submitted work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Khan, J.M., Basques, B.A., Kunze, K.N. et al. Does obesity impact lumbar sagittal alignment and clinical outcomes after a posterior lumbar spine fusion?. Eur Spine J 29, 340–348 (2020). https://doi.org/10.1007/s00586-019-06094-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-019-06094-y