Abstract
Background
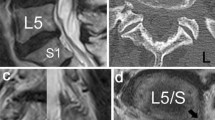
The diagnosis of lumbar intraforaminal and extraforaminal stenosis (lumbar foraminal stenosis) is sometimes difficult. However, sensory nerve action potential (SNAP) decreases in amplitude when the lesion is at or distal to the dorsal root ganglion. Therefore, the amplitude of SNAP with lumbar foraminal stenosis should be decreased. In this cohort study, the usefulness of SNAP for the preoperative diagnosis of L5/S foraminal stenosis was assessed.
Methods
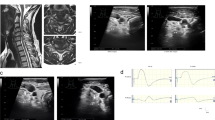
In 63 patients undergoing unilateral L5 radiculopathy, bilateral SNAPs were recorded for the superficial peroneal nerve (L5 origin). The patients were divided into two groups according to the results of imaging examinations. Group A (37 patients) included patients whose lesion was located only at the intraspinal canal. In group B (26 patients), the lesion was located only at the intra- or extraforaminal area. All patients received surgery and the symptoms were diminished. The ratios of the amplitudes of SNAPs on the affected side to that on the unaffected side were compared between groups A and B.
Results
SNAPs could not be elicited bilaterally in four patients. The amplitude ratio for group B (median 0.42, max 1.17, min 0) was significantly lower than that in group A (median 0.85, max 1.43, min 0) (p < 0.001 by Mann–Whitney U test). Using a cut-off value of 0.5 for the amplitude ratio, the sensitivity for the diagnosis of lumbar foraminal stenosis was 91.3 % with a specificity of 85.7 %.
Conclusions
Measurement of SNAP could be useful to diagnose a unilateral L5/S foraminal stenosis.





Similar content being viewed by others
References
Kunogi J, Hasue M (1991) Diagnosis and operative treatment of intraforaminal and extraforaminal nerve root compression. Spine 16:1312–1320
Briggs CA, Chandraraj S (1995) Variations in the lumbosacral ligament and associated changes in the lumbosacral region resulting in compression of the fifth dorsal root ganglion and spinal nerve. Clin Anat 8:339–346
Matsumoto M, Chiba K, Nojiri K et al (2002) Extraforaminal entrapment of the fifth lumbar spinal nerve by osteophytes of the lumbosacral spine—anatomical study and a report of four cases. Spine 27:E169–E173
Muller A, Reulen HJ (1998) A paramedian tangential approach to lumbosacral extraforaminal disc herniations. Neurosurgery 43:854–862
Nathan H, Weizenbluth M, Halperin N (1982) The lumbosacral ligament (LSL) with special emphasis on the “lumbosacral tunnel” and the entrapment of the 5th lumbar nerve. Int Orthop 6:197–202
Olsewski JM, Simmons EH, Kallen FC, Mendel FC (1991) Evidence from cadavers suggestive of entrapment of fifth lumbar spinal nerves by lumbosacral ligaments. Spine 16:336–347
Transfeldt EE, Robertson D, Bradford DS (1993) Ligaments of the lumbosacral spine and their role in possible extraforaminal spinal nerve entrapment and tethering. J Spinal Disord 6:507–512
Wiltse LL, Guyer RD, Spencer CW (1984) Alar transverse process impingement of the L5 spinal nerve: the far-out syndrome. Spine 9:31–41
Macnab I (1971) Negative disc exploration. An analysis of the causes of nerve-root involvement in sixty-eight patients. J Bone Joint Surg 53-A:891–903
Jabre JF (1981) The superficial peroneal sensory nerve revisited. Arch Neurol 38:666–667
Ducker TB (1989) Extreme lateral lumbar disc herniation. J Spinal Disord 2:131–132
Hashimoto M, Watanabe O, Hirano H (1996) Extraforaminal stenosis in the lumbosacral spine. Efficacy of MR imaging in the coronal plane. Acta Radiol 37:610–613
Kunogi J, Hasue M, Hamanaka K (1992) Usefulness of MRI and its limitation in the diagnosis of intra-and extraforaminal nerve root compression. Rinshouseikeigeka 27:503–511 (Japanese)
Hashiguchi T, Taguchi T (1995) Evaluation of lumbar radiculopathy. J West Jpn Res Soc Spine 21:113–117 (Japanese)
Tani T, Yamamoto H, Kida K (1989) Does the sensory nerve action potential remain intact in lumbosacral radiculopathy? Chubu seikeigekasaigaigeka zasshi 32:1379–1381 (Japanese)
Fisher MA (2002) Electrophysiology of radiculopathies. Clin Neurophysiol 113:317–335
Wilbourn AJ, Aminoff MJ (1998) AAEM minimonograph 32: the electrodiagnostic examination in patients with radiculopathies. Muscle Nerve 21:1612–1631
Levin KH (1998) L5 radiculopathy with reduced superficial peroneal sensory responses: intraspinal and extraspinal causes. Muscle Nerve 21:3–7
Hamanishi C, Tanaka S (1993) Dorsal root ganglia in the lumbosacral region observed from the axial views of MRI. Spine 18:1753–1756
Hasue M, Kunogi J, Konno S (1989) Classification by position of dorsal root ganglia in the lumbosacral region. Spine 14:1261–1264
Kikuchi S, Sato K, Konno S (1994) Anatomic and radiographic study of dorsal root ganglia. Spine 19:6–11
Sato K, Kikuchi S (1993) An anatomic study of foraminal nerve lesions in the lumbar spine. Spine 18:2246–2251
Ho YH, Yan SH, Lin YT (2004) Sensory nerve conduction studies of the superficial peroneal nerve in L5 radiculopathy. Acta Neurologica Taiwanica 13:114–119
Conflict of interest
No funds were received in support of this work. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ando, M., Tamaki, T., Kawakami, M. et al. Electrophysiological diagnosis using sensory nerve action potential for the intraforaminal and extraforaminal L5 nerve root entrapment. Eur Spine J 22, 833–839 (2013). https://doi.org/10.1007/s00586-012-2592-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-012-2592-5