Abstract
Purpose
To analyze the neurological and mechanical outcomes in 44 consecutive patients treated for a hematological malignancy with epidural localization to assess the place of surgery in the treatment of this pathology.
Methods
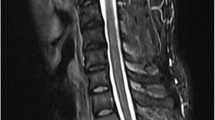
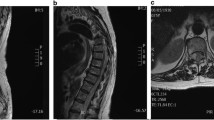
Clinical records, CT and MRI scans of 44 patients with epidural localizations of multiple myeloma or lymphoma treated between 1990 and 2005 were analyzed retrospectively. Neurological status, epiduritis and osteolysis volumes, vertebral collapse, and spinal canal compromise were assessed. The neurological outcome was graded according to Frankel and the mechanical outcome was evaluated on the rate of vertebral collapse.
Results
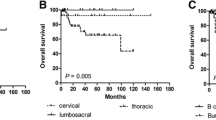
Surgery was performed in 11 patients (25 %) for neurological (n = 9) or mechanical (n = 2) reasons. In five cases, a concomitant biopsy was performed because the etiology of the epiduritis was unknown. Fifteen patients (34.1 %) presented with a neurological deficit secondary to an acute vertebral collapse (n = 4), an epiduritis (n = 7), or both (n = 4). Whatever the treatment (surgical or not), a complete recovery (Frankel E) occurred in 14/15 (93.3 %) after a mean delay of 12 weeks (range 2–24 weeks). During the follow-up, seven collapses occurred. We estimated that a threshold of 30 % of osteolysis was associated with a significant risk of vertebral collapse (P = 0.005).
Conclusions
Hematological malignancies with epidural localization must be treated first medically, even in patients with neurological symptoms. Surgery should be considered only in the cases of acute vertebral collapse, medical treatment failure, or to prevent acute collapse in patients with vertebral osteolysis of more than 30 %.




Similar content being viewed by others
References
Callander NS, Roodman GD (2001) Myeloma bone disease. Semin Hematol 38:276–285 (pii S0037196301000841)
Benson WJ, Scarffe JH, Todd ID, Palmer M, Crowther D (1979) Spinal-cord compression in myeloma. Br Med J 1:1541–1544
Blade J, Rosinol L (2007) Complications of multiple myeloma. Hematol Oncol Clin North Am 21:1231–1246. doi:10.1016/j.hoc.2007.08.006 xi
Nau KC, Lewis WD (2008) Multiple myeloma: diagnosis and treatment. Am Fam Physician 78:853–859
Blade J, Cibeira MT, Fernandez de Larrea C, Rosinol L (2010) Multiple myeloma. Ann Oncol 21:vii313–vii319. doi:10.1093/annonc/mdq363
Barron KD, Hirano A, Araki S, Terry RD (1959) Experiences with metastatic neoplasms involving the spinal cord. Neurology 9:91–106
Wise JJ, Fischgrund JS, Herkowitz HN, Montgomery D, Kurz LT (1999) Complication, survival rates, and risk factors of surgery for metastatic disease of the spine. Spine (Phila Pa 1976) 24:1943–1951
Smith ML, Newland AC (1999) Treatment of myeloma. QJM 92:11–14
Palumbo A, Anderson K (2011) Multiple myeloma. N Engl J Med 364:1046–1060. doi:10.1056/NEJMra1011442
Leigh BR, Kurtts TA, Mack CF, Matzner MB, Shimm DS (1993) Radiation therapy for the palliation of multiple myeloma. Int J Radiat Oncol Biol Phys 25:801–804
Chataigner H, Onimus M, Polette A (1998) Surgical treatment of myeloma localized in the spine. Rev Chir Orthop Reparatrice Appar Mot 84:311–318 (Pii MDOI-RCO-07-1998-84-4-0035-1040-101019-ART71)
Brenner B, Carter A, Tatarsky I, Gruszkiewicz J, Peyser E (1982) Incidence, prognostic significance and therapeutic modalities of central nervous system involvement in multiple myeloma. Acta Haematol 68:77–83
Tancioni F, Navarria P, Pessina F, Attuati L, Mancosu P, Alloisio M, Scorsetti M, Santoro A, Baena R (2012) Assessment of prognostic factors in patients with metastatic epidural spinal cord compression (MESCC) from solid tumor after surgery plus radiotherapy: a single institution experience. Eur Spine J 21:146–148
Sundaresan N, Digiacinto GV, Hughes JE, Cafferty M, Vallejo A (1991) Treatment of neoplastic spinal cord compression: results of a prospective study. Neurosurgery 29:645–650
Hammerberg KW (1992) Surgical treatment of metastatic spine disease. Spine (Phila Pa 1976) 17:1148–1153
Bickels J, Dadia S, Lidar Z (2009) Surgical management of metastatic bone disease. J Bone Joint Surg Am 91:1503–1516. doi:10.2106/JBJS.H.00175
Akeyson EW, McCutcheon IE (1996) Single-stage posterior vertebrectomy and replacement combined with posterior instrumentation for spinal metastasis. J Neurosurg 85:211–220. doi:10.3171/jns.1996.85.2.0211
Akhaddar A, Albouzidi A, Elmostarchid B, Gazzaz M, Boucetta M (2008) Sudden onset of paraplegia caused by hemorrhagic spinal epidural angiolipoma. A case report. Eur Spine J 17:S296–S298
Bauer HC (1997) Posterior decompression and stabilization for spinal metastases. Analysis of sixty-seven consecutive patients. J Bone Joint Surg Am 79:514–522
Rompe JD, Eysel P, Hopf C, Heine J (1993) Decompression/stabilization of the metastatic spine. Cotrel-Dubousset-Instrumentation in 50 patients. Acta Orthop Scand 64:3–8
Barlogie B, Shaughnessy J, Munshi N, Epstein J (2010) Plasma cell myeloma. In: Beutler E, Lichtman MA, Coller BS, Kipps T, Seligsohn U (eds) Williams Hematology, 8th edn. McGraw-Hill, New York
Frankel HL, Hancock DO, Hyslop G, Melzak J, Michaelis LS, Ungar GH, Vernon JD, Walsh JJ (1969) The value of postural reduction in the initial management of closed injuries of the spine with paraplegia and tetraplegia. Paraplegia 7:179–192
Bacci G, Savini R, Calderoni P, Gnudi S, Minutillo A, Picci P (1982) Solitary plasmacytoma of the vertebral column. A report of 15 cases. Tumori 68:271–275
Feldmann JL, Guedri M, Ohana N, Menkes CJ, Amor B (1984) Solitary spinal plasmacytoma. Ann Med Interne (Paris) 135:259–264
Quraishi NA, Gokaslan ZL, Boriani S (2010) The surgical management of metastatic epidural compression of the spinal cord. J Bone Joint Surg Br 92:1054–1060. doi:10.1302/0301-620X.92B8.22296
Husband DJ (1998) Malignant spinal cord compression: prospective study of delays in referral and treatment. BMJ 317:18–21
Sinoff CL, Blumsohn A (1989) Spinal cord compression in myelomatosis: response to chemotherapy alone. Eur J Cancer Clin Oncol 25:197–200
Fidler MW (1986) Anterior decompression and stabilisation of metastatic spinal fractures. J Bone Joint Surg Br 68:83–90
Harrington KD (1988) Anterior decompression and stabilization of the spine as a treatment for vertebral collapse and spinal cord compression from metastatic malignancy. Clin Orthop Relat Res 233:177–197
Manabe S, Tateishi A, Abe M, Ohno T (1989) Surgical treatment of metastatic tumors of the spine. Spine (Phila Pa 1976) 14:41–47
McLain RF (2001) Spinal cord decompression: an endoscopically assisted approach for metastatic tumors. Spinal Cord 39:482–487. doi:10.1038/sj.sc.3101194
Conflict of interest
No conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Flouzat-Lachaniette, CH., Allain, J., Roudot-Thoraval, F. et al. Treatment of spinal epidural compression due to hematological malignancies: a single institution’s retrospective experience. Eur Spine J 22, 548–555 (2013). https://doi.org/10.1007/s00586-012-2562-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-012-2562-y