Abstract
Purpose
We hypothesized that different patterns of biomarkers of brain injury and inflammation exist in aged patients with postoperative cognitive dysfunction (POCD) after total hip-replacement with spinal anesthesia.
Methods
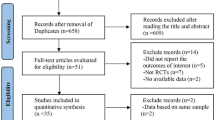
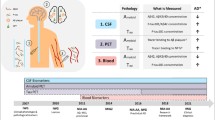
Eighty-three patients older than 65 years undergoing elective total hip-replacement surgery were enrolled in this prospective observational study. The CSF levels of Tau, phosphorylated-tau (pTau), amyloidβ1–42 (Aβ1–42), Tau/Aβ1–42, pTau/Aβ1–42, BDNF, IL-6, and IL-1β were measured preoperatively. Perioperative plasma levels of IL-1β, IL-6, brain-derived neurotrophic factor (BDNF), C-reactive protein (CRP), and malonaldehyde (MDA) as well as neurocognitive tests were determined preoperatively and seven days postoperatively.
Results
Sixty-one patients completed both the CSF and blood samples collection and the neurocognitive tests. POCD occurred in 24.6 % of patients at seven days after surgery. Patients with POCD had significantly higher IL-1β, Tau/Aβ1–42, pTau/Aβ1–42, and a lower level of Aβ1–42 in CSF when compared with the Non-POCD group (P < 0.05). Furthermore, POCD patients displayed significantly higher plasma levels of MDA when compared with Non-POCD patients at seven days after surgery (P < 0.05). There was no difference in preoperative CSF levels of Tau, IL-6, and pTau as well as plasma levels of IL-1β, IL-6, BDNF and CRP between POCD and Non-POCD groups (P > 0.05).
Conclusion
The POCD patients were associated with higher postoperative plasma levels of MDA, and higher IL-1β and lower Aβ1–42 levels in preoperative CSF that might predispose the development of POCD in aged patients following total hip-replacement surgery with spinal anesthesia.


Similar content being viewed by others
References
Steinmetz J, Christensen KB, Lund T, Lohse N, Rasmussen LS. Long-term consequences of postoperative cognitive dysfunction. Anesthesiology. 2009;110(3):548–55.
Cibelli M, Fidalgo AR, Terrando N, Ma D, Monaco C, Feldmann M, Takata M, Lever IJ, Nanchahal J, Fanselow MS, Maze M. Role of interleukin-1beta in postoperative cognitive dysfunction. Ann Neurol. 2010;68(3):360–8.
Sauër AM, Kalkman C, van Dijk D. Postoperative cognitive decline. J Anesth. 2009;23(2):256–9.
Monk TG, Weldon BC, Garvan CW, Dede DE, van der Aa MT, Gravenstein JS. Predictors of cognitive dysfunction after major noncardiac surgery. Anesthesiology. 2008;108(1):18–30.
Moller JT, Cluitmans P, Rasmussen LS, Houx P, Rasmussen H, Canet J, Rabbitt P, Jolles J, Larsen K, Hanning CD, Langeron O, Johnson T, Lauven PM, Kristensen PA, Biedler A, van Beem H, Fraidakis O, Silverstein JH, Beneken JE, Gravenstein JS. Long-term postoperative cognitive dysfunction in the elderly: ISPOCD1 study. Lancet. 1998;351(9106):6857–61.
McDonagh DL, Mathew JP, White WD, Phillips-Bute B, Laskowitz DT, Podgoreanu MV, Newman MF, Neurologic Outcome Research Group. Cognitive function after major noncardiac surgery, apolipoprotein E4 genotype, and biomarkers of brain injury. Anesthesiology. 2010;112(4):852–9.
Li YC, Xi CH, An YF, Dong WH, Zhou M. Perioperative inflammatory response and protein S-100β concentrations—relationship with post-operative cognitive dysfunction in elderly patients. Acta Anaesthesiol Scand. 2012;56(5):595–600.
Fodale V, Santamaria LB, Schifilliti D, Mandal PK. Anaesthetics and postoperative cognitive dysfunction: a pathological mechanism mimicking Alzheimer’s disease. Anaesthesia. 2010;65(4):388–95.
Seidenberg M, O’Leary DS, Berent S, Boll T. Changes in seizure frequency and test-retest scores on the Wechsler Adult Intelligence Scale. Epilepsia. 1981;22:75–83.
Brickenkamp R. Test d2: Aufmerksamkeits-Belastungs-test manual. Gottingen: Hogrefe; 1994.
Oswald WD, Roth E. Der Zahlen-Verbindungs-Test (ZVT). Gottingen: Hogrefe; 1997.
Krenk L, Rasmussen LS, Kehlet H. New insights into the pathophysiology of postoperative cognitive dysfunction. Acta Anaesthesiol Scand. 2010;54(8):951–6.
Johnson T, Monk T, Rasmussen LS, Abildstrom H, Houx P, Korttila K, Kuipers HM, Hanning CD, Siersma VD, Kristensen D, Canet J, Ibañaz MT, Moller JT, ISPOCD2 Investigators. Postoperative cognitive dysfunction in middle-aged patients. Anesthesiology. 2002;96(6):1351–7.
Tang JX, Baranov D, Hammond M, Shaw LM, Eckenhoff MF, Eckenhoff RG. Human Alzheimer and inflammation biomarkers after anesthesia and surgery. Anesthesiology. 2011;115(4):727–32.
Humpel C. Identifying and validating biomarkers for Alzheimer’s disease. Trends Biotechnol. 2011;29(1):26–32.
Mulder C, Verwey NA, van der Flier WM, Bouwman FH, Kok A, van Elk EJ, Scheltens P, Blankenstein MA. Amyloid-beta(1–42), total tau, and phosphorylated tau as cerebrospinal fluid biomarkers for the diagnosis of Alzheimer disease. Clin Chem. 2010;56(2):248–53.
Hudetz JA, Gandhi SD, Iqbal Z, Patterson KM, Pagel PS. Elevated postoperative inflammatory biomarkers are associated with short- and medium-term cognitive dysfunction after coronary artery surgery. J Anesth. 2011;25(1):1–9.
Terrando N, Monaco C, Ma D, Foxwell BM, Feldmann M, Maze M. Tumor necrosis factor-alpha triggers a cytokine cascade yielding postoperative cognitive decline. Proc Natl Acad Sci USA. 2010;107(47):20518–22.
Rudolph JL, Ramlawi B, Kuchel GA, McElhaney JE, Xie D, Sellke FW, Khabbaz K, Levkoff SE, Marcantonio ER. Chemokines are associated with delirium after cardiac surgery. J Gerontol A Biol Sci Med Sci. 2008;63(2):184–9.
Torres LL, Quaglio NB, de Souza GT, Bouwman FH, Kok A, van Elk EJ, Scheltens P, Blankenstein MA. Peripheral oxidative stress biomarkers in mild cognitive impairment and Alzheimer’s disease. J Alzheimers Dis. 2011;26(1):59–68.
Nagahara AH, Merrill DA, Coppola G, Tsukada S, Schroeder BE, Shaked GM, Wang L, Blesch A, Kim A, Conner JM, Rockenstein E, Chao MV, Koo EH, Geschwind D, Masliah E, Chiba AA, Tuszynski MH. Neuroprotective effects of brain-derived neurotrophic factor in rodent and primate models of Alzheimer’s disease. Nat Med. 2009;15(3):331–7.
Gunstad J, Benitez A, Smith J, Glickman E, Spitznagel MB, Alexander T, Juvancic-Heltzel J, Murray L. Serum brain-derived neurotrophic factor is associated with cognitive function in healthy older adults. J Geriatr Psychiatry Neurol. 2008;21(3):166–70.
Wang Y, Sands LP, Vaurio L, Mullen EA, Leung JM. The effects of postoperative pain and its management on postoperative cognitive dysfunction. Am J Geriatr Psychiatry. 2007;15(1):50–9.
Acknowledgments
This work was supported by the Jiangsu Province’s Key Provincial Talents Program (No. RC2011136) and the Natural Science Foundation of Jiangsu Province (No. BK2012778) and attributed to Department of Anesthesiology, Jinling Hospital, School of Medicine, Nanjing University, Nanjing, China.
Conflict of interest
The authors have no potential conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
M.-H. Ji and H.-M. Yuan contributed equally to this work.
About this article
Cite this article
Ji, MH., Yuan, HM., Zhang, GF. et al. Changes in plasma and cerebrospinal fluid biomarkers in aged patients with early postoperative cognitive dysfunction following total hip-replacement surgery. J Anesth 27, 236–242 (2013). https://doi.org/10.1007/s00540-012-1506-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-012-1506-3