Abstract
Background
Intestinal Behçet’s disease (BD) is very rare, and epidemiologic data regarding BD are scarce. Moreover, there have been no population-based studies focusing on intestinal BD. We conducted a nationwide population-based study to examine the incidence and clinical course of Korean patients with intestinal BD.
Methods
We collected data on 365 patients diagnosed with intestinal BD from 2011 to 2014 using the Health Insurance Review and Assessment Services claims database. We analyzed the incidence and clinical outcomes, including cumulative rates of bowel resection, hospitalization, and medication use.
Results
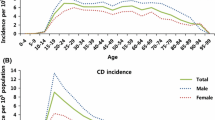
During the study period, the average annual incidence for intestinal BD was 0.18 per 105 population, and the proportion of cases with intestinal involvement was 3.9%. At 1 and 4 years after diagnosis, the cumulative rates of surgery were 5.0 and 10.9%, respectively, whereas those of hospitalization were 27.8 and 32.4%, respectively. The 1- and 4-year cumulative rates of requirements for medications were 39.8 and 49.1% for moderate- to high-dose corticosteroids, 33.6 and 42.1% for immunomodulators, and 3.5 and 6.8% for biologics, respectively. The cumulative probability of corticosteroid and immunomodulator use was higher in male than in female patients and in younger (<40 years) than in older (≥40 years) patients. However, there were no significant differences in the cumulative probabilities of surgery, hospitalization, and biologics use according to sex and age group.
Conclusions
The incidence of intestinal BD in Korea is quite low and has been stable in recent years.



Similar content being viewed by others
References
Dalvi SR, Yildirim R, Yazici Y. Behcet’s syndrome. Drugs. 2012;72:2223–41.
Cheon JH, Kim WH. An update on the diagnosis, treatment, and prognosis of intestinal Behçet’s disease. Curr Opin Rheumatol. 2015;27:24–31.
Suzuki Kurokawa M, Suzuki N. Behcet’s disease. Clin Exp Med. 2004;4:10–20.
Cheon JH, Kim ES, Shin SJ, et al. Development and validation of novel diagnostic criteria for intestinal Behçet’s disease in Korean patients with ileocolonic ulcers. Am J Gastroenterol. 2009;104:2492–9.
Chang HK, Kim JW. The clinical features of Behcet’s disease in Yongdong districts: analysis of a cohort followed from 1997 to 2001. J Korean Med Sci. 2002;17:784–9.
Yazici Y, Yurdakul S, Yazici H. Behçet’s syndrome. Curr Rheumatol Rep. 2010;12:429–35.
Jung YS, Cheon JH, Park SJ, et al. Clinical course of intestinal Behcet’s disease during the first five years. Dig Dis Sci. 2013;58:496–503.
Jung YS, Yoon JY, Lee JH, et al. Prognostic factors and long-term clinical outcomes for surgical patients with intestinal Behcet’s disease. Inflamm Bowel Dis. 2011;17:1594–602.
Ketch LL, Buerk CA, Liechty D. Surgical implications of Behcet’s disease. Arch Surg. 1980;115:759–60.
Iida M, Kobayashi H, Matsumoto T, et al. Postoperative recurrence in patients with intestinal Behcet’s disease. Dis Colon Rectum. 1994;37:16–21.
Jung YS, Hong SP, Kim TI, et al. Long-term clinical outcomes and factors predictive of relapse after 5-aminosalicylate or sulfasalazine therapy in patients with intestinal Behcet disease. J Clin Gastroenterol. 2012;46:e38–45.
Jung YS, Cheon JH, Hong SP, et al. Clinical outcomes and prognostic factors for thiopurine maintenance therapy in patients with intestinal Behcet’s disease. Inflamm Bowel Dis. 2012;18:750–7.
Jung YS, Hong SP, Kim TI, et al. Early versus late surgery in patients with intestinal Behçet disease. Dis Colon Rectum. 2012;55:65–71.
Molodecky NA, Soon IS, Rabi DM, et al. Increasing incidence and prevalence of the inflammatory bowel diseases with time, based on systematic review. Gastroenterology. 2012;142:46–54 (quiz e30).
Shimizu T, Ehrlich GE, Inaba G, et al. Behcet disease (Behcet syndrome). Semin Arthritis Rheum. 1979;8:223–60.
Jankowski J, Crombie I, Jankowski R. Behcet’s syndrome in Scotland. Postgrad Med J. 1992;68:566–70.
Kim HJ, Hann HJ, Hong SN, et al. Incidence and natural course of inflammatory bowel disease in Korea, 2006–2012: a nationwide population-based study. Inflamm Bowel Dis. 2015;21:623–30.
Alpsoy E. Behçet’s disease: a comprehensive review with a focus on epidemiology, etiology and clinical features, and management of mucocutaneous lesions. J Dermatol. 2016;43:620–32.
Cho SB, Bang D. New insights in the clinical understanding of Behçet’s disease. Yonsei Med J. 2012;53:35–42.
Ng WK, Wong SH, Ng SC. Changing epidemiological trends of inflammatory bowel disease in Asia. Intest Res. 2016;14:111–9.
Loftus EV, Sandborn WJ. Epidemiology of inflammatory bowel disease. Gastroenterol Clin North Am. 2002;31:1–20.
Ugurlu N, Bozkurt S, Bacanli A, et al. The natural course and factors affecting severity of Behçet’s disease: a single-center cohort of 368 patients. Rheumatol Int. 2015;35:2103–7.
Ideguchi H, Suda A, Takeno M, et al. Behçet disease: evolution of clinical manifestations. Medicine. 2011;90:125–32.
Ng SC, Tang W, Ching JY, et al. Incidence and phenotype of inflammatory bowel disease based on results from the Asia-Pacific Crohn’s and Colitis Epidemiology Study. Gastroenterology. 2013;145(158–165):e152.
Jung YS, Cheon JH, Park SJ, et al. Long-term clinical outcomes of Crohn’s disease and intestinal Behcet’s disease. Inflamm Bowel Dis. 2013;19:99–105.
Jung YS, Yoon JY, Hong SP, et al. Influence of age at diagnosis and sex on clinical course and long-term prognosis of intestinal Behcet’s disease. Inflamm Bowel Dis. 2012;18:1064–71.
Frolkis AD, Dykeman J, Negrón ME, et al. Risk of surgery for inflammatory bowel diseases has decreased over time: a systematic review and meta-analysis of population-based studies. Gastroenterology. 2013;145:996–1006.
Schnitzler F, Fidder H, Ferrante M, et al. Mucosal healing predicts long-term outcome of maintenance therapy with infliximab in Crohn’s disease. Inflamm Bowel Dis. 2009;15:1295–301.
Burger D, Travis S. Conventional medical management of inflammatory bowel disease. Gastroenterology. 2011;140(1827–1837):e1822.
Colombel JF, Rutgeerts P, Reinisch W, et al. Early mucosal healing with infliximab is associated with improved long-term clinical outcomes in ulcerative colitis. Gastroenterology. 2011;141:1194–201.
Lakatos PL, Golovics PA, David G, et al. Has there been a change in the natural history of Crohn’s disease? Surgical rates and medical management in a population-based inception cohort from Western Hungary between 1977–2009. Am J Gastroenterol. 2012;107:579–88.
Ramadas AV, Gunesh S, Thomas GA, et al. Natural history of Crohn’s disease in a population-based cohort from Cardiff (1986–2003): a study of changes in medical treatment and surgical resection rates. Gut. 2010;59:1200–6.
Rungoe C, Langholz E, Andersson M, et al. Changes in medical treatment and surgery rates in inflammatory bowel disease: a nationwide cohort study 1979–2011. Gut. 2014;63:1607–16.
Chhaya V, Saxena S, Cecil E, et al. Steroid dependency and trends in prescribing for inflammatory bowel disease—a 20-year national population-based study. Aliment Pharmacol Ther. 2016;44:482–94.
Yazici H, Tüzün Y, Pazarli H, et al. Influence of age of onset and patient’s sex on the prevalence and severity of manifestations of Behçet’s syndrome. Ann Rheum Dis. 1984;43:783–9.
Alpsoy E, Donmez L, Onder M, et al. Clinical features and natural course of Behçet’s disease in 661 cases: a multicentre study. Br J Dermatol. 2007;157:901–6.
Bardak Y. Effects of age and sex on Behçet’s disease. J Rheumatol. 1999;26:1008–9.
Kural Seyahi E, Fresko I, Seyahi N, et al. The long-term mortality and morbidity of Behçet syndrome: a 2-decade outcome survey of 387 patients followed at a dedicated center. Medicine. 2003;82:60–76.
Yazici H, Basaran G, Hamuryudan V, et al. The ten-year mortality in Behcet’s syndrome. Br J Rheumatol. 1996;35:139–41.
Miheller P, Kiss LS, Juhasz M, et al. Recommendations for identifying Crohn’s disease patients with poor prognosis. Expert Rev Clin Immunol. 2013;9:65–75 (quiz 76).
Moon CM, Cheon JH, Shin JK, et al. Prediction of free bowel perforation in patients with intestinal Behçet’s disease using clinical and colonoscopic findings. Dig Dis Sci. 2010;55:2904–11.
Park JJ, Kim WH, Cheon JH. Outcome predictors for intestinal Behçet’s disease. Yonsei Med J. 2013;54:1084–90.
Kobayashi K, Ueno F, Bito S, et al. Development of consensus statements for the diagnosis and management of intestinal Behcet’s disease using a modified Delphi approach. J Gastroenterol. 2007;42:737–45.
Acknowledgements
This research was supported by two grants (A120176 and HI13C1345) from the Korean Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), which is funded by the Ministry of Health and Welfare, Republic of Korea; two grants (NRF-2013R1A2A2A01067123 and NRF-2014R1A1A1008096) from the Basic Science Research Program through the National Research Foundation of Korea, which is funded by the Ministry of Science, ICT and Future Planning; and a faculty research grant (2012-31-0477) from the Department of Internal Medicine, Yonsei University, College of Medicine.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Additional information
M. Han and Y. S. Jung contributed equally to this study.
Rights and permissions
About this article
Cite this article
Han, M., Jung, Y.S., Kim, W.H. et al. Incidence and clinical outcomes of intestinal Behçet’s disease in Korea, 2011–2014: a nationwide population-based study. J Gastroenterol 52, 920–928 (2017). https://doi.org/10.1007/s00535-016-1300-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-016-1300-3