Abstract
Purpose
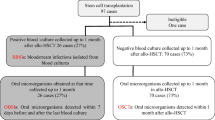
Coagulase-negative staphylococci (CoNS) are frequently isolated from blood cultures of hematopoietic cell transplantation (HCT) patients. Generally, the use of central venous catheters is recognized as a significant risk factor for CoNS infection, while the impact of CoNS infection from oral ulcerative mucositis, which occurs frequently in HCT, may be underestimated. Here, we examined the bacteria on the buccal mucosa after HCT.
Methods
Sixty-one patients were examined for bacteria on the buccal mucosa routinely once a week from 1 week before to 3 weeks after allogeneic HCT. Subjects were divided into groups with short and long periods of antibiotic use, and differences in bacterial substitution were evaluated. The relationships between type of HCT (conventional HCT or RIST) and bacterial substitution were also evaluated.
Results
The changes in detection frequencies of CoNS and α-streptococci from before to 3 weeks after HCT were significant (P < 0.05, χ 2 test): 14.5–53.3% and 92.7–53.1%, respectively. Significant bacterial substitution of CoNS for streptococci was observed in the long-term antibiotic use group (P < 0.05, χ 2 test), but also occurred in cases with short-term or no antibiotic use. No relationships between type of HCT (conventional HCT or RIST) were observed.
Conclusion
Bacterial substitution of CoNS for streptococci occurred frequently on the buccal mucosa after HCT. In addition to antibiotic use, environmental factors may be involved in bacterial substitution. It is important to consider the presence of oral mucositis in CoNS infection after HCT.



Similar content being viewed by others
References
López Dupla M, Martinez JA, Vidal F et al (2005) Clinical characterization of breakthrough bacteraemia: a survey of 392 episodes. J Intern Med 258:172–180
Kloos WE, Bannerman TL (1994) Update on clinical significance of coagulase-negative staphylococci. Clin Microbiol Rev 7:117–140
Weinstein MP, Towns ML, Quartey SM et al (1997) The clinical significance of positive blood cultures in the 1990s: a prospective comprehensive evaluation of the microbiology, epidemiology, and outcome of bacteremia and fungemia in adults. Clin Infect Dis 24:584–602
Herwaldt LA, Magdalena G, Kao C, Pfaller MA (1996) The positive predictive value of isolating coagulase-negative staphylococci from blood cultures. Clin Infect Dis 22:14–20
Khatib R, Riederer KM, Clark JA, Khatib S, Briski LE, Wilson FM (1995) Coagulase-negative staphylococci in multiple blood cultures: strain relatedness and determinants of same-strain bacteremia. J Clin Microbiol 33:816–820
Thylefors JD, Harbarth S, Pittet D (1998) Increasing bacteremia due to coagulase-negative staphylococci: fiction or reality? Infect Control Hosp Epidemiol 19:581–589
Seo SK, Venkataraman L, DeGirolami PC, Samore MH (2000) Molecular typing of coagulase-negative staphylococci from blood cultures does not correlate with clinical criteria for true bacteremia. Am J Med 109:697–704
Heiden G (1996) A comparison of methods to determine whether clinical isolates of Staphylococcus epidermidis from the same patient are related. J Hosp Infect 34:31–42
Tan TQ, Musser JM, Shulman RJ, Mason EO Jr, Mahoney DH Jr, Kaplan SL (1994) Molecular epidemiology of coagulase-negative Staphylococcus blood isolates from neonates with persistent bacteremia and children with central venous catheter infections. J Infect Dis 169:1393–1397
Toldos CM, Yague G, Ortiz G, Segovia M (1997) Assessment of multiple coagulase-negative staphylococci isolated in blood cultures using pulsed-field gel electrophoresis. Eur J Clin Microbiol Infect Dis 16:581–586
Tardieu C, Cowen D, Thirion X, Franquin JC (1996) Quantitative scale of oral mucositis associated with autologous bone marrow transplantation. Eur J Cancer 32:381–387
Takahashi K, Soga Y, Murayama Y et al (2010) Oral mucositis in patients receiving reduced-intensity regimens for allogeneic hematopoietic cell transplantation: comparison with conventional regimen. Support Care Cancer. doi: 10.1007/s00520-009-0637-z
Hughes WT, Armstrong D, Bodey GP et al (2002) Guidelines for the use of antimicrobial agents in neutropenic patients with cancer. Clin Infect Dis 34:730
Sonis ST, Oster G, Fuchs H et al (2001) Oral mucositis and the clinical and economic outcomes of hematopoietic stem-cell transplantation. J Clin Oncol 19:2201–2205
Bellm LA, Epstein JB, Rose-Ped A, Martin P, Fuchs HJ (2000) Patient reports of complications of bone marrow transplantation. Support Care Cancer 8:33–39
Amerongen AV, Veerman EC (2003) Current therapies for xerostomia and salivary gland hypofunction associated with cancer therapies. Support Care Cancer 11:226–231
Jensen SB, Pedersen AM, Reibel J, Nauntofte B (2003) Xerostomia and hypofunction of the salivary glands in cancer therapy. Support Care Cancer 11:207–225
Sugiura Y, Soga Y, Nishide S et al (2008) Evaluation of xerostomia in hematopoietic cell transplantation by a simple capacitance method device. Support Care Cancer 16:1197–1200
Cervera C, Almela M, Martínez-Martínez JA, Moreno A, Miró JM (2009) Risk factors and management of Gram-positive bacteraemia. Int J Antimicrob Agents 34(Suppl 4):S26–S30
Raad I, Kassar R, Ghannam D, Chaftari AM, Hachem R, Jiang Y (2009) Management of the catheter in documented catheter-related coagulase-negative staphylococcal bacteremia: remove or retain? Clin Infect Dis 49:1187–1194
Kennedy HF, Morrison D, Kaufmann ME et al (2000) Origins of Staphylococcus epidermidis and Streptococcus oralis causing bacteraemia in a bone marrow transplant patient. J Med Microbiol 49:367–370
Blijlevens NM, Donnelly JP, de Pauw BE (2001) Empirical therapy of febrile neutropenic patients with mucositis: challenge of risk-based therapy. Clin Microbiol Infect 7(Suppl 4):47–52
Costa SF, Miceli MH, Anaissie EJ (2004) Mucosa or skin as source of coagulase-negative staphylococcal bacteraemia? Lancet Infect Dis 4:278–286
Acknowledgments
This study was partially conducted as the education curriculum, Practice in Dental Sciences, in Okayama University Dental School. We thank Ms. Hitomi Ono and Mr. Hidetaka Ideguchi, students at Okayama University Dental School, for data analysis. This study was supported by a Grant-in-Aid for Young Scientists (Start-up #20890138 and B #22791836), from the Japan Society for the Promotion of Science (JSPS) (YS) and FY 2010 Researcher Exchange Program between JSPS and The Netherlands Organization for Scientific Research.
Conflicts of interest
The authors declare that there were no conflicts of interest in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Soga, Y., Maeda, Y., Ishimaru, F. et al. Bacterial substitution of coagulase-negative staphylococci for streptococci on the oral mucosa after hematopoietic cell transplantation. Support Care Cancer 19, 995–1000 (2011). https://doi.org/10.1007/s00520-010-0923-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-010-0923-9