Summary
Background
The Pneumocystis pneumonia is an increasing problem in transplanted patients: up to 25 % suffer from Pneumocystis pneumonia, occurring during the first 6 months after transplantation.
Methods
From 2001 to 2009, we investigated 21 patients with pneumonia after renal transplantation for the presence of Pneumocystis jirovecii. The laboratory diagnosis was established by Grocott and Giemsa staining methods and Pneumocystis-specific mitochondrial transcribed large subunit nested polymerase chain reaction (PCR). The PCR was also used for the differentiation of Pneumocystis pneumonia from Pneumocystis carriage.
Results
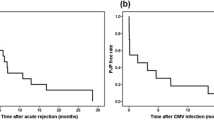
Of 21 patients, 7 had a Pneumocystis pneumonia, 6 were Pneumocystis carriers and 8 patients were negative. Four out of seven Pneumocystis pneumonia patients and two out of six patients with Pneumocystis carriage had a delayed graft function. An acute cytomegalovirus infection after transplantation was not detectable in the patients with Pneumocystis pneumonia, but in three patients with Pneumocystis carriage.
Conclusions
Pneumocystis pneumonia was present in 33.3 % of transplanted patients with suspected pneumonia. An association between acute rejection or co-infections and Pneumocystis pneumonia or carriage in patients after renal transplantation cannot be excluded. In three out of seven Pneumocystis pneumonia patients, an overlapping of hospitalisation times and an onset of Pneumocystis pneumonia 6 months after transplantation was found. Thus, person-to-person transmission seems probable in these cases.
Zusammenfassung
Hintergrund
Die Pneumocystis Pneumonie stellt in zunehmendem Maße ein Problem bei Patienten nach Transplantationen dar: bis zu 25 % der Patienten erkranken an einer Pneumocystis Pneumonie, die innerhalb der ersten sechs Monate nach Transplantation auftritt.
Methodik
Von 2001 bis 2009 wurde bei 21 Patienten nach Nierentransplantation eine Pneumonie durch Pneumocystis jirovecii vermutet. Die Labordiagnostik erfolgte mittels Grocott- und Giemsa-Färbungen sowie Pneumocystis-spezifischer „mitochondrial transcribed large subunit“ nested PCR. Diese PCR wurde zusätzlich zur Differenzierung zwischen einer Pneumocystis Pneumonie und einer Pneumocystis Besiedelung genutzt.
Ergebnisse
Bei 7/21 Patienten wurde eine Pneumocystis Pneumonie nachgewiesen, 6 waren mit Pneumocystis besiedelt und 8 Patienten waren negativ. 4/7 Pneumocystis Pneumonie Patienten sowie 2/6 Patienten mit Pneumocystis Besiedlung hatten eine verzögerte Transplantat-Funktion. Eine akute Cytomegalie-Virus-Infektion nach Transplantation trat bei keinem der Pneumocystis Pneumonie-Fälle und bei drei Patienten mit Pneumocystis Besiedelung auf.
Schlussfolgerungen
Eine Pneumocystis Pneumonie konnte bei 33,3 % der Patienten nach Nierentransplantation und Verdacht auf Pneumonie nachgewiesen werden. Eine Assoziation zwischen akuter Rejektion oder Koinfektionen und dem Auftreten einer PCP bzw. Besiedelung war nicht auszuschließen. Bei 3/7 Pneumocystis Pneumonie Patienten wurde eine Überschneidung der Hospitalisierungs-Zeiträume mit gleichzeitigem Beginn der Pneumocystis Pneumonie sechs Monate nach Transplantation festgestellt. Eine Übertragung von Person zu Person scheint in diesen Fällen sehr wahrscheinlich.
Similar content being viewed by others
References
Morris A, Lundgren JD, Masur H, Walzer PD, Hanson DL, Frederick T, et al. Current epidemiology of Pneumocystis pneumonia. Emerg Infect Dis. 2004;10:1713–20.
Torres HA, Chemaly RF, Storey R, Aguilera EA, Nogueras GM, Safdar A, et al. Influence of type of cancer and hematopoietic stem cell transplantation on clinical presentation of Pneumocystis jiroveci pneumonia in cancer patients. Eur J Clin Microbiol Infect Dis. 2006;25:382–8.
Coyle PV, McCaughey C, Nager A, McKenna J, O’Neill H, Feeney SA, et al. Rising incidence of Pneumocystis jirovecii pneumonia suggests iatrogenic exposure of immune-compromised patients may be becoming a significant problem. J Med Microbiol. 2012;61:1009–15.
Goto N, Oka S. Pneumocystis jirovecii pneumonia in kidney transplantation. Transpl Infect Dis. 2011;13:551–8.
Durand-Joly I, Chabe M, Soula F, Delhaes L, Camus D, Dei-Cas E. Molecular diagnosis of Pneumocystis pneumonia. FEMS Immunol Med Microbiol. 2005;45:405–10.
Morris A, Wei K, Afshar K, Huang L. Epidemiology and clinical significance of Pneumocystis colonization. J Infect Dis. 2008;197:10–7.
Branten AJ, Beckers PJ, Tiggeler RG, Hoitsma AJ. Pneumocystis carinii pneumonia in renal transplant recipients. Nephrol Dial Transplant. 1995;10:1194–7.
Mori S, Cho I, Sugimoto M. A followup study of asymptomatic carriers of Pneumocystis jiroveci during immunosuppressive therapy for rheumatoid arthritis. J Rheumatol. 2009;36:1600–5.
Davis JL, Welsh DA, Beard CB, Jones JL, Lawrence GG, Fox MR, et al. Pneumocystis colonisation is common among hospitalised HIV infected patients with non-Pneumocystis pneumonia. Thorax. 2008;63:329–34.
Fritzsche C, Riebold D, Fuehrer A, Mitzner A, Klammt S, Mueller-Hilke B, et al. Pneumocystis jirovecii colonization among renal transplant recipients. Nephrology. 2013;18:382–7.
Fritzsche C, Riebold D, Munk-Hartig A, Klammt S, Neeck G, Reisinger E. High prevalence of Pneumocystis jirovecii colonization among patients with autoimmune inflammatory diseases and corticosteroid therapy. Scand J Rheumatol. 2012;41:208–13.
Vernadakis S, Sotiropoulos GC, Brokalaki EI, Esser S, Kaiser GM, Cicinnati VR, et al. Long-term outcomes of liver transplant patients with human immunodeficiency virus infection and end-stage-liver-disease: single center experience. Eur J Med Res. 2011;16:342–8.
Le Gal S, Damiani C, Rouille A, Grall A, Treguer L, Virmaux M, et al. A cluster of Pneumocystis infections among renal transplant recipients: molecular evidence of colonized patients as potential infectious sources of Pneumocystis jiroveci. Clin Infect Dis. 2012;54:62–71.
Chandola P, Lall M, Sen S, Bharadwaj R. Outbreak of Pneumocystis jirovecii pneumonia in renal transplant recipients on prophylaxis: our observation and experience. Indian J Med Microbiol. 2014;32:333–6.
Riebold D, Löbermann M, Reisinger EC. Diagnostic features and resistance testing for Pneumocystis jirovecii. J Lab Med. 2008;32:35–9.
Procop GW, Haddad S, Quinn J, Wilson ML, Henshaw NG, Reller LB, et al. Detection of Pneumocystis jiroveci in respiratory specimens by four staining methods. J Clin Microbiol. 2004;42:3333–5.
Sowden E, Carmichael AJ. Autoimmune inflammatory disorders, systemic corticosteroids and Pneumocystis pneumonia: a strategy for prevention. BMC Infect Dis. 2004;4:42.
Rabodonirina M, Vanhems P, Couray-Targe S, Gillibert RP, Ganne C, Nizard N, et al. Molecular evidence of interhuman transmission of Pneumocystis pneumonia among renal transplant recipients hospitalized with HIV-infected patients. Emerg Infect Dis. 2004;10:1766–73.
Hocker B, Wendt C, Nahimana A, Tonshoff B, Hauser PM. Molecular evidence of Pneumocystis transmission in pediatric transplant unit. Emerg Infect Dis. 2005;11:330–2.
de Boer MG, Bruijnesteijn van Coppenraet LE, Gaasbeek A, Berger SP, Gelinck LB, van Houwelingen HC, et al. An outbreak of Pneumocystis jiroveci pneumonia with 1 predominant genotype among renal transplant recipients: interhuman transmission or a common environmental source? Clin Infect Dis. 2007;44:1143–9.
Schmoldt S, Schuhegger R, Wendler T, Huber I, Sollner H, Hogardt M, et al. Molecular evidence of nosocomial Pneumocystis jirovecii transmission among 16 patients after kidney transplantation. J Clin Microbiol. 2008;46:966–71.
Eitner F, Hauser IA, Rettkowski O, Rath T, Lopau K, Pliquett RU, et al. Risk factors for Pneumocystis jiroveci pneumonia (PcP) in renal transplant recipients. Nephrol Dial Transplant. 2011;26:2013–7.
Borstnar S, Lindic J, Tomazic J, Kandus A, Pikelj A, Prah J, et al. Pneumocystis jirovecii pneumonia in renal transplant recipients: a national center experience. Transplant Proc. 2013;45:1614–7.
Gordon SM, LaRosa SP, Kalmadi S, Arroliga AC, Avery RK, Truesdell-LaRosa L, et al. Should prophylaxis for Pneumocystis carinii pneumonia in solid organ transplant recipients ever be discontinued? Clin Infect Dis. 1999;28:240–6.
Mitsides N, Greenan K, Green D, Middleton R, Lamerton E, Allen J, et al. Complications and outcomes of trimethoprim-sulphamethoxazole as chemoprophylaxis for Pneumocystis pneumonia in renal transplant recipients. Nephrology (Carlton). 2014;19:157–63.
Arend SM, Kroon FP, van’t Wout JW. Pneumocystis carinii pneumonia in patients without AIDS, 1980 through 1993. An analysis of 78 cases. Arch Intern Med. 1995;155:2436–41.
Li JY, Yong TY, Grove DI, Coates PT. Late-onset and atypical presentation of Pneumocystis carinii pneumonia in a renal transplant recipient. Clin Exp Nephrol. 2009;13:92–5.
Haidinger M, Hecking M, Memarsadeghi M, Weichhart T, Werzowa J, Horl WH, et al. Late onset Pneumocystis pneumonia in renal transplantation after long-term immunosuppression with belatacept. Transpl Infect Dis. 2009;11:171–4.
Rezavand B, Hosseini MJ, Izadi M, Mahmoodzadeh Poornaki A, Sadraei J, Einollahi B, et al. Lethal Pneumocystis jiroveci pneumonia 24 years after kidney transplantation. Nephrourol Mon. 2014;6:e13605.
EBPG Expert Group on Renal Transplantation. European best practice guidelines for renal transplantation. Section IV: long-term management of the transplant recipient. IV.7.1 Late infections. Pneumocystis carinii pneumonia. Nephrol Dial Transplant. 2002;17(Suppl. 4):36–9.
McCaughan JA, Courtney AE. Pneumocystis jiroveci pneumonia in renal transplantation: time to review our practice? Nephrol Dial Transplant. 2012;27:13–5.
Arend SM, Westendorp RG, Kroon FP, van’t Wout JW, Vandenbroucke JP, van Es LA, et al. Rejection treatment and cytomegalovirus infection as risk factors for Pneumocystis carinii pneumonia in renal transplant recipients. Clin Infect Dis. 1996;22:920–5.
Radisic M, Lattes R, Chapman JF, del Carmen Rial M, Guardia O, Seu F, et al. Risk factors for Pneumocystis carinii pneumonia in kidney transplant recipients: a case-control study. Transpl Infect Dis. 2003;5:84–93.
de Boer MG, Kroon FP, le Cessie S, de Fijter JW, van Dissel JT. Risk factors for Pneumocystis jirovecii pneumonia in kidney transplant recipients and appraisal of strategies for selective use of chemoprophylaxis. Transpl Infect Dis. 2011;13:559–69.
Arichi N, Kishikawa H, Mitsui Y, Kato T, Nishimura K, Tachikawa R, et al. Cluster outbreak of Pneumocystis pneumonia among kidney transplant patients within a single center. Transplant Proc. 2009;41:170–2.
Adlakha A, Pavlou M, Walker DA, Copas AJ, Dufty N, Batson S, et al. Survival of HIV-infected patients admitted to the intensive care unit in the era of highly active antiretroviral therapy. Int J STD AIDS. 2011;22:498–504.
Chabe M, Dei-Cas E, Creusy C, Fleurisse L, Respaldiza N, Camus D, et al. Immunocompetent hosts as a reservoir of Pneumocystis organisms: histological and rt-PCR data demonstrate active replication. Eur J Clin Microbiol Infect Dis. 2004;23:89–97.
Medrano FJ, Montes-Cano M, Conde M, de la Horra C, Respaldiza N, Gasch A, et al. Pneumocystis jirovecii in general population. Emerg Infect Dis. 2005;11:245–50.
de Boer MG, Kroon FP, le Cessie S, de Fijter JW, van Dissel JT. Risk factors for Pneumocystis jirovecii pneumonia in kidney transplant recipients and appraisal of strategies for selective use of chemoprophylaxis. Transpl Infect Dis. 2011;13(6):559–69.
Debourgogne A, Favreau S, Ladriere M, Bourry S, Machouart M. Characteristics of Pneumocystis pneumonia in Nancy from January 2007 to April 2011 and focus on an outbreak in nephrology. J Mycol Med. 2014;24:19–24.
Damiani C, Choukri F, Le Gal S, Menotti J, Sarfati C, Nevez G, et al. Possible nosocomial transmission of Pneumocystis jirovecii. Emerg Infect Dis. 2012;18:877–8.
Brunot V, Pernin V, Chartier C, Garrigue V, Vetromile F, Szwarc I, et al. An epidemic of Pneumocystis jiroveci pneumonia in a renal transplantation center: role of T-cell lymphopenia. Transplant Proc. 2012;44:2818–20.
Conflict of interest
There are no commercial relationships or conflicts of interests. The authors declare that they did not receive any funding or grants.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maruschke, M., Riebold, D., Holtfreter, M. et al. Pneumocystis pneumonia (PCP) and Pneumocystis jirovecii carriage in renal transplantation patients: a single-centre experience. Wien Klin Wochenschr 126, 762–766 (2014). https://doi.org/10.1007/s00508-014-0608-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-014-0608-3