Abstract
Background
Gallstone disease is a common gastrointestinal disorder in industrialised countries. Although symptoms can be severe, some people can be symptom free for many years after the original attack. Surgery is the current treatment of choice, but evidence suggests that observation is also feasible and safe. We reviewed the evidence on cholecystectomy versus observation for uncomplicated symptomatic gallstones and conducted a cost-effectiveness analysis.
Methods
We searched six electronic databases (last search April 2014). We included randomised controlled trials (RCTs) or non-randomised comparative studies where adults received either cholecystectomy or observation/conservative management for the first episode of symptomatic gallstone disease (biliary pain or cholecystitis) being considered for surgery in secondary care. Meta-analysis was used to combine results. A de novo Markov model was developed to assess the cost effectiveness of the interventions.
Results
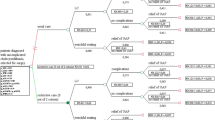
Two RCTs (201 participants) were included. Eighty-eight percent of people randomised to surgery and 45 % of people randomised to observation underwent cholecystectomy during the 14-year follow-up period. Participants randomised to observation were significantly more likely to experience gallstone-related complications (RR = 6.69, 95 % CI = 1.57–28.51, p = 0.01), in particular acute cholecystitis (RR = 9.55, 95 % CI = 1.25–73.27, p = 0.03), and less likely to undergo surgery (RR = 0.50, 95 % CI = 0.34–0.73, p = 0.0004) or experience surgery-related complications (RR = 0.36, 95 % CI = 0.16–0.81, p = 0.01) than those randomised to surgery. Fifty-five percent of people randomised to observation did not require surgery, and 12 % of people randomised to cholecystectomy did not undergo surgery. On average, surgery costs £1,236 more per patient than conservative management, but was more effective.
Conclusions
Cholecystectomy is the preferred treatment for symptomatic gallstones. However, approximately half the observation group did not require surgery or suffer complications indicating that it may be a valid alternative to surgery. A multicentre trial is needed to establish the effects, safety and cost effectiveness of observation/conservative management relative to cholecystectomy.


Similar content being viewed by others
References
Guidelines for the treatment of gallstones (1993) American college of physicians. Ann Int Med 119:620–622
Aerts R, Penninckx F (2003) The burden of gallstone disease in Europe. Aliment Pharmacol Ther 18(Suppl. 3):49–53
Kang JY, Ellis C, Majeed A, Hoare J, Tinto A, Williamsons RCN et al (2003) Gallstones—An increasing problem: a study of hospital admissions in England between 1989/1990 and 1999/2000. Aliment Pharmacol Ther 17:561–569
Sandler RS, Everhart JE, Donowitz M, Adams E, Cronin K, Goodman C et al (2002) The burden of selected digestive diseases in the United States. Gastroenterology 122:1500–1511
Gallstones and laparoscopic cholecystectomy, NIH Consensus Statement [document on the Internet] (1992) National Institutes of Health available from: URL: http://consensus.nih.gov/1992/1992gallstoneslaparoscopy090html.htm
Halldestam I, Enell EL, Kullman E, Borch K (2004) Development of symptoms and complications in individuals with asymptomatic gallstones. Br J Surg 91:734–738
Portincasa P, Moschetta A, Palasciano G (2006) Cholesterol gallstone disease. Lancet 368:230–239
Shaffer EA (2006) Epidemiology of gallbladder stone disease. Best Pract Res Clin Gastroenterol 20:981–996
Stinton LM, Myers RP, Shaffer EA (2010) Epidemiology of gallstones. Gastroenterol Clin N Am 39:157–169
Portincasa P, Di Ciaula A, Wang HH, Moschetta A, Wang DQH (2009) Medicinal treatments of cholesterol gallstones: old, current and new perspectives. Curr Med Chem 16:1531–1542
Attili AF, De Santis A, Capri R, Repice AM, Maselli S, Capocaccia L et al (1995) The natural history of gallstones: the GREPCO experience. Hepatology 21:656–660
Schmidt M, Hausken T, Glambek I, Schleer C, Eide GE, Sondenaa K (2011) A 24-year controlled follow-up of patients with silent gallstones showed no long-term risk of symptoms or adverse events leading to cholecystectomy. Scand J Gastroenterol 46:949–954
McSherry CK, Ferstenberg H, Calhoun WF, Lahman E, Virshup M (1985) The natural history of diagnosed gallstone disease in symptomatic and asymptomatic patients. Ann Surg 202:59–63
Festi D, Reggiani MLB, Attili AF, Loria P, Pazzi P, Scaioli E et al (2010) Natural history of gallstone disease: expectant management or active treatment? Results from a population-based cohort study. J Gastroenterol Hepatol 25:719–724
Friedman GD, Raviola CA, Fireman B (1989) Prognosis of gallstones with mild or no symptoms: 25 years of follow-up in a health maintenance organization. J Clin Epidemiol 42:1989
Sondenaa K, Nesvik I, Solhaug JH, Soreide O (1997) Randomization to surgery or observation in patients with symptomatic gallbladder stone disease: the problem of evidence-based medicine in clinical practice. Scand J Gastroenterol 32:611–616
Schmidt M, Dumot JA, Soreide O, Sondenaa K (2012) Diagnosis and management of gallbladder calculus disease. Scand J Gastroenterol 47:1257–1265
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol 62:e1–e34
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA G (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA Statement. Open Med 3:e123–e130
Higgins JP, Green S (2011) Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [document on the Internet]. The Cochrane Collaboration available from: URL: http://www.cochrane-handbook.org/
Schmidt M, Sondenaa K, Vetrhus M, Berhane T, Eide GE (2011) A randomized controlled study of uncomplicated gallstone disease with a 14-year follow-up showed that operation was the preferred treatment. Dig Surg 28:270–276
Schmidt M, Sondenaa K, Vetrhus M, Berhane T, Eide GE (2011) Long-term follow-up of a randomized controlled trial of observation versus surgery for acute cholecystitis: non-operative management is an option in some patients. Scand J Gastroenterol 46:1257–1262
Vetrhus M, Soreide O, Eide GE, Solhaug JH, Nesvik I, Sondenaa K (2004) Pain and quality of life in patients with symptomatic, non-complicated gallbladder stones: results of a randomized controlled trial. Scand J Gastroenterol 39:270–276
Vetrhus M, Soreide O, Solhaug JH, Nesvik I, Sondenaa K (2002) Symptomatic, non-complicated gallbladder stone disease. Operation or observation? A randomized clinical study. Scand J Gastroenterol 37:834–839
Vetrhus M, Soreide O, Nesvik I, Sondenaa K (2003) Acute cholecystitis: delayed surgery or observation. A randomized clinical trial. Scand J Gastroenterol 38:985–990
Vetrhus M, Soreide O, Eide GE, Nesvik I, Sondenaa K (2005) Quality of life and pain in patients with acute cholecystitis. Results of a randomized clinical trial. Scand J Surg 94:34–39
Bass EB, Steinberg EP, Pitt HA, Griffiths RI, Lillemoe KD, Saba GP et al (1994) Comparison of the rating scale and the standard gamble in measuring patient preferences for outcomes of gallstone disease. Med Decis Mak 14:307–314
Ransohoff DF, Gracie WA (1993) Treatment of gallstones. Ann Int Med 119:606–619
Larsen TK, Qvist N (2007) The influence of gallbladder function on the symptomatology in gallstone patients, and the outcome after cholecystectomy or expectancy. Dig Dis Sci 52:760–763
Lamberts MP, Lugtenberg M, Rovers MM, Roukema AJ, Drenth JPH, Westert GP et al (2013) Persistent and de novo symptoms after cholecystectomy: a systematic review of cholecystectomy effectiveness. Surg Endosc 27:709–718
Bates T, Ebbs SR, Harrison M, A’Hern RP (1991) Influence of cholecystectomy on symptoms. Br J Surg 78:964–967
Borly L, Anderson IB, Bardram L, Christensen E, Sehested A, Kehlet H et al (1999) Preoperative prediction model of outcome after cholecystectomy for symptomatic gallstones. Scand J Gastroenterol 34:1144–1152
Gui GP, Cheruvu CV, West N, Sivaniah K, Fiennes AG (1998) Is cholecystectomy effective treatment for symptomatic gallstones? Clinical outcome after long-term follow-up. Ann R Coll Surg Engl 80:25–32
Middelfart HV, Kristensen JU, Laursen CN, Qvist N, Hojgaard L, Funch-Jensen P et al (1998) Pain and dyspepsia after elective and acute cholecystectomy. Scand J Gastroenterol 33:10–14
Ure BM, Troidl H, Spangenberger W, Lefering R, Dietrich A, Eypasch EP et al (1995) Long-term results after laparoscopic cholecystectomy. Br J Surg 82:267–270
Ahmed R, Freeman JV, Ross B, Kohler B, Nicholl JP, Johnson AG (2000) Long term response to gallstone treatment—problems and surprises. Eur J Surg 166:447–454
Jorgensen T, Stubbe Teglbjerg J, Wille-Jorgensen P, Bille T, Thorvaldsen P (1991) Persisting pain after cholecystectomy. A prospective investigation. Scand J Gastroenterol 26:124–128
McSherry CK (1989) Cholecystectomy: the gold standard. Am J Surg 158:174–178
Keus F, de Jong J, Gooszen HG, Laarhoven CJHM (2006) Small-incision versus open cholecystectomy for patients with symptomatic cholecystolithiasis. Cochrane Database Syst Rev Issue 4:Art. No.: CD004788
Keus F, De Jong JAF, Gooszen HG, van Laarhoven CJHM (2006) Laparoscopic versus open cholecystectomy for patients with symptomatic cholecystolithiasis. Cochrane Database Syst Rev Issue 4:Art. no. CD006231
Keus F, de Jong JA, Gooszen HG, van Laarhoven CJ (2006) Laparoscopic versus small-incision cholecystectomy for patients with symptomatic cholecystolithiasis. Cochrane Database Syst Rev Issue 4:Art. no. CD006229
Hospital episode statistics, Admitted patient care, England—2012–13: procedures and interventions [speadsheet on the Internet] (2012) Health & Social Care Information Centre available from: URL: http://www.hscic.gov.uk/searchcatalogue?productid=13264&q=title%3a%22Hospital+Episode+Statistics%3a+Admitted+patient+care%22&sort=Relevance&size=10&page=1#top
Goldacre MJ, Abisgold JD, Seagroatt V, Yeates D (2005) Cancer after cholecystectomy: record-linkage cohort study. Br J Cancer 92:1307–1309
Shao T, Yang YX (2005) Cholecystectomy and the risk of colorectal cancer. Am J Gastroenterol 100:1813–1820
Acknowledgments
This review was commissioned by the UK NIHR HTA Programme (project number 12/16)
Disclosures
The authors Drs. Brazzelli, Cruickshank, Ahmed & Avenell; Profs McNamee & Ramsay; Ms Kilonzo; Ms Stewart; MsFraser; and Mr Elders have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Appendices
Appendix 1: Sample search strategy
Ovid multifile search URL: http://shibboleth.ovid.com/.
-
1.
cholecystitis/.
-
2.
cholecystitis, acute/.
-
3.
cholecystolithiasis/.
-
4.
Gallstones/.
-
5.
Cholelithiasis/.
-
6.
Biliary colic/.
-
7.
(gall?bladder adj3 (empyema or inflam$)).tw.
-
8.
(biliary colic or gall?stone$ or cholecystitis or cholecystolithiasis).tw.
-
9.
((pain or biliary symptom$) adj5 (cholecystitis or cholecystolithiasis or gall?bladder)).tw.
-
10.
Or/1-9.
-
11.
Exp Cholecystectomy/.
-
12.
Cholecystectom$.tw.
-
13.
((excis$ or remov$) adj4 gall?bladder).tw.
-
14.
((surgery or surgical) adj5 (cholecystitis or cholecystolithiasis or gall?bladder)).tw.
-
15.
Or/11-14.
-
16.
Exp clinical trial/.
-
17.
Randomized controlled trial.pt.
-
18.
Controlled clinical trial.pt.
-
19.
Randomi?ed.ab.
-
20.
Randomly.ab.
-
21.
Trial.ab.
-
22.
Placebo.ab.
-
23.
Drug therapy.fs.
-
24.
Groups.ab.
-
25.
Comparative study/use prmz.
-
26.
(prospective$ or retrospective$).tw.
-
27.
(compare$ or compara$).ti,ab.
-
28.
Or/16-27.
-
29.
10 and 15 and 28.
-
30.
(review or editorial or case report$ or letter).pt.
-
31.
Exp animals/not humans/.
-
32.
29 not (30 or 31).
-
33.
Limit 32 to yr = “1980 -Current”.
-
34.
Limit 33 to yr = “2000-Current”.
-
35.
Limit 33 to yr = “1980-1999”.
-
36.
Remove duplicates from 34.
-
37.
Remove duplicates from 35.
-
38.
36 or 37.
Appendix 2: Risk of bias summary figure for clinical effectiveness review

Rights and permissions
About this article
Cite this article
Brazzelli, M., Cruickshank, M., Kilonzo, M. et al. Systematic review of the clinical and cost effectiveness of cholecystectomy versus observation/conservative management for uncomplicated symptomatic gallstones or cholecystitis. Surg Endosc 29, 637–647 (2015). https://doi.org/10.1007/s00464-014-3712-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3712-6