Abstract
Background
A number of studies have investigated several aspects of feasibility and validity of performance assessments with virtual reality surgical simulators. However, the validity of performance assessments is limited by the reliability of such measurements, and some issues of reliability still need to be addressed. This study aimed to evaluate the hypothesis that test subjects show logarithmic performance curves on repetitive trials for a component task of laparoscopic cholecystectomy on a virtual reality simulator, and that interindividual differences in performance after considerable training are significant. According to kinesiologic theory, logarithmic performance curves are expected and an individual’s learning capacity for a specific task can be extrapolated, allowing quantification of a person’s innate ability to develop task-specific skills.
Methods
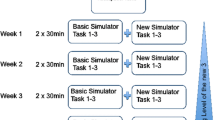
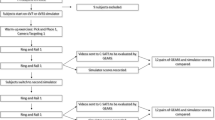
In this study, 20 medical students at the University of Basel Medical School performed five trials of a standardized task on the LS 500 virtual reality simulator for laparoscopic surgery. Task completion time, number of errors, economy of instrument movements, and maximum speed of instrument movements were measured.
Results
The hypothesis was confirmed by the fact that the performance curves for some of the simulator measurements were very close to logarithmic curves, and there were significant interindividual differences in performance at the end of the repetitive trials.
Conclusions
Assessment of perceptual motor skills and the innate ability of an individual with no prior experience in laparoscopic surgery to develop such skills using the LS 500 VR surgical simulator is feasible and reliable.



Similar content being viewed by others
References
Haluck RS, Krummel TM (2000) Computers and virtual reality for surgical education in the 21st century. Arch Surg 135: 786–792
Marescaux J, Leroy J, Gagner M, Rubino F, Mutter D, Vix M, Butner SE, Smith MK (2001) Transatlantic robot-assisted telesurgery. Nature 413: 379–380
Marescaux J, Clement JM, Tassetti V, Koehl C, Cotin S, Russier Y, Mutter D, Delingette H, Ayache N (1998) Virtual reality applied to hepatic surgery simulation: the next revolution. Ann Surg 228: 627–634
Gorman PJ, Meier AH, Krummel TM (1999) Simulation and virtual reality in surgical education: real or unreal? Arch Surg 134: 1203–1208
Bridges M, Diamond DL (1999) The financial impact of teaching surgical residents in the operating room. Am J Surg 177: 28–32
Tendick F, Downes M, Cavusoglu M, Gantert W, Way LW (1998) Development of virtual environments for training skills and reducing errors in laparoscopic surgery. SPIE Conference 3262 on Surgical-Assist Systems, San Jose, CA pp 36–44
Cao C, MacKenzie CL, Ibbotson JA, Turner LJ, Blair NP, Nagy AG (1999) Hierarchical decomposition of laparoscopic procedures. Stud Health Technol Inform 62: 83–89
Gallagher AG, McClure N, McGuigan J, Crothers I, Browning J (1999) Virtual reality training in laparoscopic surgery: a preliminary assessment of minimally invasive surgical traininer virtual reality (MIST-VR). Endoscopy 31: 310–313
Szekely G, Satava RM (1999) Virtual reality in medicine. BMJ 319:1305
O’Toole RV, Playter RR, Krummel TM, Blank WC, Cornelius NH, Roberts WR, Bell WJ, Raibert M (1999) Measuring and developing suturing technique with a virtual reality surgical simulator. J Am Coll Surg 189: 114–127
Chaudhry A, Sutton C, Wood J, Stone R, McCloy R (1999) Learning rate for laparoscopic skills on MIST-VR, a virtual simulator: quality of human–computer interface. Ann R Coll Surg Engl 81: 281–286
Taffinder NJ, McManus IC, Gul Y, Russell RCG, Darzi A (1998) Effect of sleep deprivation on surgeons’ dexterity on laparoscopy simulator. Lancet 352: 1191
Darzi A, Smith S, Taffinder N (1999) Assessing operative skill: needs to become more objective. BMJ 318: 887–888
Devitt JH, Kurrek MM, Cohen MM, Cleave-Hogg D (2001) The validity of performance assessments using simulation. Anesthesiology 95: 36–42
Jordan JA, Gallagher AG, McGuigan J, McGlade K, McClure N (2000) A comparison between randomly alternative imaging, normal laparoscopic imaging, and virtual reality training in laparoscopic psychomotor skill acquisition. Am J Surg 180: 208–211
Schijven MP, Jakimowicz J (2004) The learning curve on the Xitact LS 500 laparoscopy simulator: profiles of performance. Surg Endosc 18: 121–127
Schijven MP, Jakimowicz J (2002) Face, expert, and a referent validity of the Xitact LS 500 laparoscopy simulator. Surg Endosc 16: 1764–1770
Schijven MP, Jakimowicz J (2003) Construct validity: experts and residents performing on the Xitact LS500 laparoscopy simulator. Surg Endosc 17: 803–810
Grantcharov TP, Kristiansen VB, Bendix J, Bardram L, Rosenberg J, Funch-Jensen P (2004) Randomized clinical trial of virtual reality simulation for laparoscopic skills training. Br J Surg 91: 146–150
Risucci DA, Tortolani AJ (1990) A methodological framework for the design of research on the evaluation of residents. Acad Med 65: 36–41
Schmidt RA (1982) Motor control and learning: a behavioral emphasis. Human Kinetics Publishers, Champaign, IL
Ivry R (1996) Representational issues in motor learning: phenomena and theory. In: Handbook of perception and action. Academic Press, San Diego, CA
Hanna GB, Drew T, Clinch P, Shimi S, Dunkley P, Hau C, Cuschieri A (1997) Psychomotor skills for endoscopic manipulations: differing abilities between right- and left-handed individuals. Ann Surg 225: 333–338
Reznick R (1993) Teaching and testing technical skills. Am J Surg 165: 358–361
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rosenthal, R., Gantert, W.A., Scheidegger, D. et al. Can skills assessment on a virtual reality trainer predict a surgical trainee’s talent in laparoscopic surgery?. Surg Endosc 20, 1286–1290 (2006). https://doi.org/10.1007/s00464-005-0635-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-005-0635-2